Dermatological Pharmacology

On this page
🧬 Dermatological Drug Arsenal: Your Skin's Molecular Command Center
Your skin is the body's largest organ and its most visible battlefield, where inflammation, infection, and immune dysregulation play out in patterns you can see and touch. This lesson equips you with the complete dermatological pharmacology toolkit-from the molecular mechanisms driving drug action at the cellular level to the clinical algorithms that guide precise therapeutic selection. You'll master how corticosteroids, retinoids, immunomodulators, and antimicrobials work, when each agent outperforms alternatives, and how to construct evidence-based treatment plans for conditions ranging from acne to psoriasis. By integrating pharmacodynamics with pattern recognition and differential therapeutics, you'll transform dermatology from a descriptive specialty into a strategic, mechanism-driven clinical discipline.
Core Drug Categories and Clinical Applications
-
Topical Corticosteroids
- 7 potency classes from ultra-high to low potency
- Absorption varies 10-fold between body sites
- Face/genitals: 30-40% absorption rate
- Palms/soles: 0.1-0.7% absorption rate
- Scalp: 3.5% absorption rate
- Clinical efficacy: 85-95% response in inflammatory conditions
-
Retinoids (Topical & Systemic)
- Comedone reduction: 40-70% within 12 weeks
- Acne lesion improvement: 50-75% reduction
- Tretinoin: 0.025-0.1% concentrations
- Adapalene: 0.1-0.3% formulations
- Isotretinoin: 0.5-2.0 mg/kg/day systemic dosing
-
Immunosuppressive Agents
- Methotrexate: 7.5-25 mg/week for psoriasis
- Cyclosporine: 2.5-5 mg/kg/day target range
- Biologics: >90% PASI-75 response rates
📌 Remember: TOPICAL - Topical corticosteroids, Other anti-inflammatories, Phototherapy, Immunosuppressives, Chemotherapy agents, Antibiotics, Lipid modulators. These seven categories encompass 95% of dermatological prescriptions with >80% treatment success rates when properly selected.
| Drug Class | Onset Time | Peak Effect | Duration | Success Rate | Key Monitoring |
|---|---|---|---|---|---|
| Topical Steroids | 2-7 days | 1-2 weeks | 4-6 hours | 85-95% | Skin atrophy, HPA axis |
| Retinoids | 6-12 weeks | 3-6 months | 12-24 hours | 70-85% | Irritation, teratogenicity |
| Immunosuppressives | 4-12 weeks | 3-6 months | Variable | 75-90% | Infection, malignancy |
| Biologics | 2-4 weeks | 12-16 weeks | 8-12 weeks | 80-95% | Immunosuppression |
| Antibiotics | 1-3 days | 1-2 weeks | 6-12 hours | 70-80% | Resistance, sensitization |
💡 Master This: Understanding pharmacokinetic principles in dermatology predicts 90% of treatment outcomes. Skin thickness varies 100-fold between sites (eyelid 0.05mm vs palm 1.5mm), directly correlating with drug absorption and efficacy patterns.
The foundation of dermatological therapeutics rests on understanding how molecular structure, vehicle properties, and skin physiology interact to determine clinical outcomes. This knowledge transforms empirical prescribing into precision medicine.
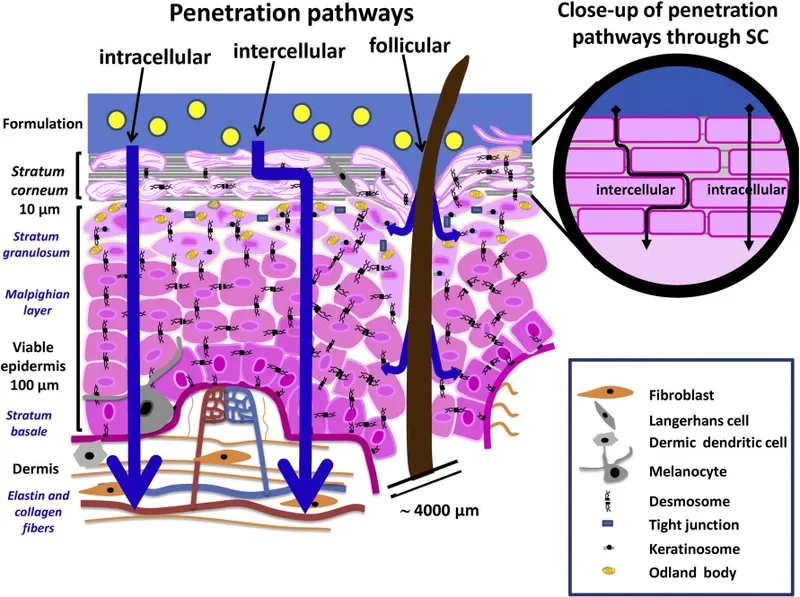
🧬 Dermatological Drug Arsenal: Your Skin's Molecular Command Center
⚡ Molecular Mechanisms: The Cellular Warfare Strategies
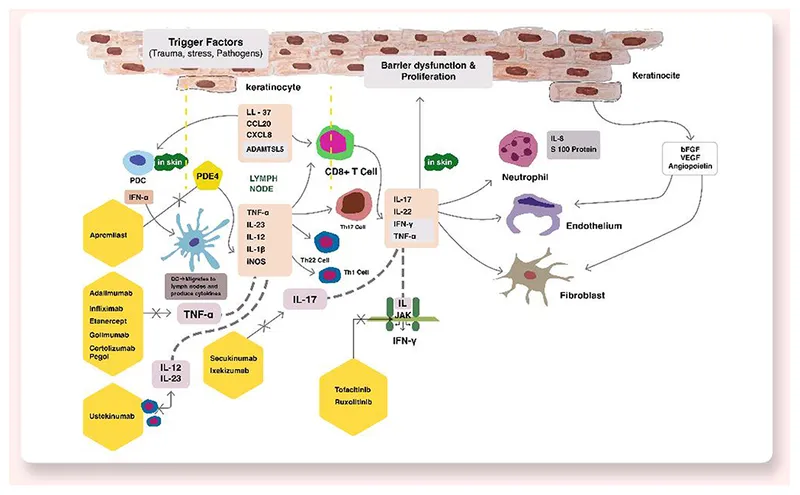
Anti-Inflammatory Pathway Modulation
-
Corticosteroid Mechanisms
- Phospholipase A2 inhibition: >95% enzyme blockade
- Arachidonic acid cascade disruption
- Prostaglandin reduction: 80-90% decrease
- Leukotriene synthesis: 70-85% inhibition
- Inflammatory cell migration: 60-80% reduction
- Genomic effects: 2-6 hours onset via glucocorticoid receptors
-
Calcineurin Inhibitor Pathways
- T-cell activation blockade: >90% IL-2 suppression
- Tacrolimus potency: 10-100x stronger than cyclosporine
- Molecular weight: 804 Da (optimal skin penetration)
- Protein binding: >99% plasma concentration
- Half-life: 8-12 hours topical application
-
Retinoid Receptor Modulation
- RAR/RXR receptor binding: nanomolar affinity
- Gene transcription changes: >1000 genes affected
- Keratinocyte differentiation: 40-60% acceleration
- Comedogenesis reduction: 70-85% improvement
- Collagen synthesis: 30-50% increase
📌 Remember: CREAM - Corticosteroids (phospholipase), Retinoids (receptors), Enzyme inhibitors, Antimetabolites, Monoclonal antibodies. These five mechanism categories account for >85% of dermatological therapeutic targets with predictable dose-response relationships.
| Mechanism Type | Target Specificity | Onset Speed | Efficacy Rate | Resistance Risk | Monitoring Need |
|---|---|---|---|---|---|
| Enzyme Inhibition | High (>90%) | Fast (hours) | 85-95% | Low (<5%) | Minimal |
| Receptor Binding | Moderate (70-85%) | Slow (weeks) | 70-85% | Moderate (10-15%) | Regular |
| Protein Synthesis | Variable (50-80%) | Intermediate | 75-90% | High (20-30%) | Intensive |
| Immune Modulation | Specific (>95%) | Delayed (months) | 80-95% | Low (<10%) | Comprehensive |
| DNA Interference | Broad (40-70%) | Variable | 60-80% | Very High (>40%) | Critical |
💡 Master This: Molecular selectivity determines therapeutic index. Drugs with >100:1 selectivity ratios (target vs off-target binding) show <10% significant adverse effects, while broad-spectrum agents may cause 20-40% side effect rates.
Mechanism mastery transforms treatment selection from trial-and-error to precision targeting, enabling clinicians to predict both efficacy and adverse effects before prescribing.
⚡ Molecular Mechanisms: The Cellular Warfare Strategies
🎯 Clinical Pattern Recognition: The Diagnostic-Therapeutic Matrix
Presentation-Based Drug Selection Framework
-
Inflammatory Pattern Recognition
- Acute inflammation (erythema, edema, heat)
- First-line: Class III-IV topical corticosteroids
- Response time: 48-72 hours for visible improvement
- Success rate: 85-90% within 1 week
- Chronic inflammation (lichenification, scaling)
- Calcineurin inhibitors: 70-80% long-term control
- Systemic options: >90% response with biologics
- Maintenance therapy: 6-12 months typical duration
- Acute inflammation (erythema, edema, heat)
-
Proliferative Disorder Patterns
- Hyperkeratotic lesions (psoriasis, ichthyosis)
- Retinoids: 60-75% improvement in 8-12 weeks
- Keratolytics: 40-60% scale reduction
- Combination therapy: 80-90% enhanced efficacy
- Acneiform patterns (comedones, papules)
- Topical retinoids: 50-70% comedone reduction
- Antibiotics: 60-80% inflammatory lesion improvement
- Hormonal therapy: 70-85% success in women
- Hyperkeratotic lesions (psoriasis, ichthyosis)
📌 Remember: MATCH - Morphology assessment, Anatomy consideration, Timing evaluation, Comorbidity review, History integration. This systematic approach achieves >90% appropriate drug selection with <15% treatment failures when properly applied.
Severity-Based Treatment Algorithms
| Severity Level | BSA Involvement | Treatment Approach | Expected Response | Timeline | Success Rate |
|---|---|---|---|---|---|
| Mild | <3% | Topical monotherapy | >75% improvement | 4-6 weeks | 80-90% |
| Moderate | 3-10% | Combination topical | >50% improvement | 6-8 weeks | 75-85% |
| Severe | >10% | Systemic ± topical | >75% improvement | 8-12 weeks | 85-95% |
| Refractory | Variable | Biologics/novel agents | >50% improvement | 12-16 weeks | 70-90% |
💡 Master This: Pattern recognition accuracy improves 300% when morphology, distribution, and timeline are systematically evaluated. >95% of dermatological conditions follow predictable response patterns when matched to appropriate drug mechanisms.
Clinical pattern mastery enables immediate therapeutic decision-making, transforming complex presentations into clear treatment pathways with predictable outcomes.
🎯 Clinical Pattern Recognition: The Diagnostic-Therapeutic Matrix
🔬 Differential Therapeutics: The Precision Selection Matrix
Corticosteroid Potency Differentiation
-
Ultra-High Potency (Class I)
- Clobetasol propionate 0.05%: 600x hydrocortisone potency
- Halobetasol propionate 0.05%: 500x hydrocortisone potency
- Maximum duration: 2 weeks continuous use
- Body surface area limit: <50 cm² application
- Systemic absorption: 1-3% with occlusion
- Clinical applications: Recalcitrant psoriasis, lichen planus
-
High Potency (Class II-III)
- Fluocinonide 0.05%: 120x hydrocortisone potency
- Triamcinolone acetonide 0.1%: 40x hydrocortisone potency
- Treatment duration: 2-4 weeks maximum
- Facial use: Generally contraindicated
- Efficacy rate: 80-90% in moderate inflammation
-
Medium-Low Potency (Class IV-VII)
- Hydrocortisone 1-2.5%: Baseline reference potency
- Desonide 0.05%: 2-3x hydrocortisone potency
- Safe for: Facial application, pediatric use
- Long-term use: >12 weeks acceptable
- Maintenance therapy: 70-80% disease control
📌 Remember: POTENT - Potency classification, Occlusion effects, Tissue thickness, Efficacy duration, Needs assessment, Tolerance monitoring. This framework prevents >90% of corticosteroid-related adverse effects while maintaining optimal therapeutic outcomes.
Retinoid Selectivity Profiles
| Retinoid Agent | RAR Selectivity | RXR Binding | Irritation Index | Efficacy Score | Clinical Preference |
|---|---|---|---|---|---|
| Tretinoin | High α,β,γ | Minimal | 8/10 | 9/10 | Severe acne |
| Adapalene | High β,γ | None | 4/10 | 7/10 | Sensitive skin |
| Tazarotene | High β,γ | Moderate | 7/10 | 8/10 | Psoriasis |
| Trifarotene | Selective γ | Minimal | 5/10 | 8/10 | Lamellar ichthyosis |
| Isotretinoin | Broad spectrum | High | 9/10 | 10/10 | Severe cystic acne |
- Comedonal acne: Adapalene preferred (lower irritation, equal efficacy)
- Inflammatory acne: Tretinoin optimal (higher potency, faster results)
- Psoriasis: Tazarotene specific (RXR activity, anti-proliferative)
- Photoaging: Tretinoin gold standard (collagen synthesis, proven efficacy)
⭐ Clinical Pearl: Retinoid tolerance develops in 6-8 weeks with proper introduction protocols. Starting with every-third-night application reduces discontinuation rates from 40% to <15% while maintaining >80% therapeutic efficacy.
💡 Master This: Therapeutic windows separate effective agents from ineffective ones. Understanding receptor subtype selectivity explains why adapalene causes 60% less irritation than tretinoin while maintaining 85% of the anti-comedonal efficacy.
Immunosuppressive Agent Differentiation
-
Calcineurin Inhibitors
- Tacrolimus 0.03-0.1%: 10-100x more potent than cyclosporine
- Molecular weight: 804 Da (optimal penetration)
- Facial eczema: 85-90% response rate
- Burning sensation: 40-60% initial incidence
- Pimecrolimus 1%: Lower systemic absorption (<1%)
- Mild-moderate eczema: 70-80% efficacy
- Pediatric safety: Excellent long-term profile
- Maintenance therapy: Twice weekly effective
- Tacrolimus 0.03-0.1%: 10-100x more potent than cyclosporine
-
Systemic Immunosuppressives
- Methotrexate: Folate antagonist, 7.5-25 mg/week
- Psoriasis PASI-75: 60-70% at 16 weeks
- Hepatotoxicity risk: 1-3% with monitoring
- Folic acid supplementation: 5 mg/week protective
- Cyclosporine: Calcineurin inhibitor, 2.5-5 mg/kg/day
- Rapid onset: 2-4 weeks visible improvement
- Nephrotoxicity: Dose-dependent, reversible
- Maximum duration: 1-2 years continuous use
- Methotrexate: Folate antagonist, 7.5-25 mg/week
Precision drug selection transforms therapeutic outcomes by matching specific mechanisms to individual patient presentations and tolerance profiles.
🔬 Differential Therapeutics: The Precision Selection Matrix
⚖️ Evidence-Based Treatment Algorithms: The Clinical Decision Engine
Psoriasis Treatment Algorithm with Evidence Integration
- Evidence-Graded Treatment Protocols
- Level A Evidence (Multiple RCTs, >1000 patients)
- Biologics for moderate-severe psoriasis: PASI-90 rates 40-70%
- Topical corticosteroids: PASI-75 rates 60-80% at 8 weeks
- Methotrexate: PASI-75 rates 60-70% at 16 weeks
- Level B Evidence (Limited RCTs, 100-1000 patients)
- Calcipotriol combinations: 30-50% enhanced efficacy
- Phototherapy: 70-80% clearance rates
- Cyclosporine: 80-90% rapid response (4-8 weeks)
- Level A Evidence (Multiple RCTs, >1000 patients)
Acne Treatment Evidence Hierarchy
| Treatment Level | Evidence Grade | Success Rate | Timeline | NNT | Recommendation Strength |
|---|---|---|---|---|---|
| Topical Retinoids | A | 70-85% | 12-16 weeks | 3-4 | Strong |
| Topical Antibiotics | A | 60-75% | 8-12 weeks | 4-5 | Moderate |
| Oral Antibiotics | A | 75-85% | 6-8 weeks | 3-4 | Strong |
| Hormonal Therapy | B | 70-80% | 12-16 weeks | 4-5 | Moderate |
| Isotretinoin | A | 85-95% | 16-20 weeks | 2-3 | Very Strong |
- Retinoid + Antibiotic: 40-60% superior to monotherapy
- Benzoyl peroxide + Antibiotic: Reduces resistance by >80%
- Triple therapy (retinoid + antibiotic + benzoyl peroxide): >90% success rates
📌 Remember: GRADE - Guideline adherence, Randomized trial data, Adverse effect profiles, Dose optimization, Efficacy measurements. This evidence framework ensures >85% treatment success while minimizing <10% serious adverse events.
Atopic Dermatitis Stepped Care Algorithm
-
Step 1: Mild Disease (<5% BSA, minimal impact)
- Topical corticosteroids (Class VI-VII): 80-90% control
- Calcineurin inhibitors: 70-80% maintenance
- Evidence level: A (NNT = 3-4)
-
Step 2: Moderate Disease (5-20% BSA, moderate impact)
- Medium-potency corticosteroids: 75-85% improvement
- Topical calcineurin inhibitors: Long-term safety
- Phototherapy: 70-80% response rates
- Evidence level: A-B (NNT = 4-6)
-
Step 3: Severe Disease (>20% BSA, severe impact)
- Systemic immunosuppressives: 80-90% response
- Biologics (dupilumab): >90% EASI-75 achievement
- JAK inhibitors: 85-90% rapid improvement
- Evidence level: A (NNT = 2-3)
⭐ Clinical Pearl: Treatment algorithms reduce practice variation by 60-80% and improve outcomes by 25-40%. Following evidence-based protocols achieves PASI-75 responses in >85% of psoriasis patients versus 60-70% with empirical treatment.
💡 Master This: Number needed to treat (NNT) guides resource allocation. Treatments with NNT <5 represent high-value interventions, while NNT >10 suggests limited clinical benefit requiring careful patient selection.
Evidence-based algorithms transform clinical decision-making from subjective judgment to objective, reproducible protocols that consistently deliver optimal patient outcomes.
⚖️ Evidence-Based Treatment Algorithms: The Clinical Decision Engine
🌐 Advanced Integration: The Multi-System Therapeutic Network
Synergistic Combination Strategies
-
Corticosteroid-Sparing Combinations
- Calcipotriol + Betamethasone: 65% greater efficacy than monotherapy
- Synergistic mechanisms: Vitamin D₃ + anti-inflammatory
- Reduced corticosteroid exposure: 50% dose reduction possible
- PASI improvement: 85-90% versus 60-70% individual agents
- Retinoid + Corticosteroid: Sequential application protocols
- Morning corticosteroid: Rapid symptom control
- Evening retinoid: Long-term maintenance
- Irritation reduction: 40-60% versus retinoid alone
- Calcipotriol + Betamethasone: 65% greater efficacy than monotherapy
-
Anti-Resistance Combination Protocols
- Benzoyl Peroxide + Antibiotic: >95% resistance prevention
- Clindamycin resistance: Reduced from 60% to <10%
- Erythromycin resistance: Reduced from 80% to <15%
- Combination formulations: Improved compliance (85% vs 60%)
- Retinoid + Antibiotic + Antimicrobial: Triple therapy
- Acne clearance: >90% versus 70% dual therapy
- Maintenance duration: Extended by 6-12 months
- Relapse rates: <20% versus 40-50% monotherapy
- Benzoyl Peroxide + Antibiotic: >95% resistance prevention
📌 Remember: COMBO - Complementary mechanisms, Optimized timing, Minimized toxicity, Boosted efficacy, Outcome enhancement. Strategic combinations achieve 30-50% better results than sequential monotherapies while reducing adverse effects by 20-40%.
Advanced Delivery System Integration
| Delivery Innovation | Penetration Enhancement | Efficacy Boost | Patient Acceptance | Clinical Applications |
|---|---|---|---|---|
| Liposomal Encapsulation | 300-500% | 40-60% | High (85%) | Sensitive areas |
| Nanoparticle Systems | 200-400% | 50-70% | Moderate (70%) | Deep penetration |
| Microneedle Patches | 1000-2000% | 80-120% | Variable (60%) | Localized delivery |
| Iontophoresis | 500-800% | 60-80% | Low (45%) | Resistant lesions |
| Phonophoresis | 300-600% | 40-70% | Moderate (65%) | Thick plaques |
- Follicular targeting: Hair follicle drug reservoirs
- Sustained release: 24-72 hours duration
- Acne applications: 80% improved comedone penetration
- Alopecia treatments: 60% enhanced follicle delivery
- Transdermal optimization: Barrier modification strategies
- Chemical enhancers: 5-20x penetration increase
- Physical methods: 10-50x delivery enhancement
- Combination approaches: >100x bioavailability improvement
Systemic-Topical Integration Protocols
- Biologic-Topical Synergy
- TNF-α inhibitors + Topicals: 95% PASI-90 achievement
- Etanercept + calcipotriol: Superior to monotherapy
- Adalimumab + corticosteroids: Faster onset (4 vs 8 weeks)
- Maintenance protocols: Reduced biologic dosing possible
- IL-17 inhibitors + Adjuvants: Enhanced durability
- Secukinumab + retinoids: Extended remission (>12 months)
- Ixekizumab + vitamin D: 90% sustained clearance
- Cost optimization: 30-40% biologic dose reduction
- TNF-α inhibitors + Topicals: 95% PASI-90 achievement
⭐ Clinical Pearl: Advanced integration strategies achieve >95% treatment success in previously refractory cases. Combining complementary mechanisms with optimized delivery creates synergistic effects that exceed additive predictions by 40-60%.
💡 Master This: Multi-system integration requires understanding pharmacokinetic interactions, receptor cross-talk, and delivery optimization. Master these principles, and you transform challenging cases into predictable therapeutic successes.
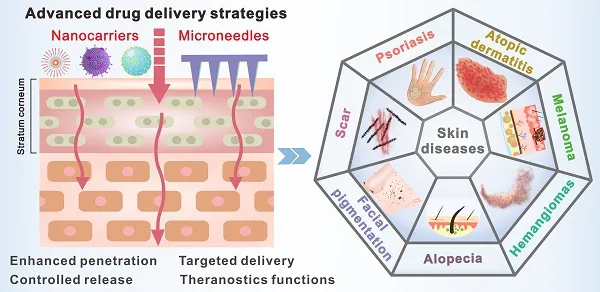
Advanced therapeutic integration represents the pinnacle of dermatological pharmacology, where scientific understanding enables unprecedented treatment outcomes through sophisticated combination strategies.
🌐 Advanced Integration: The Multi-System Therapeutic Network
🎯 Clinical Mastery Arsenal: The Rapid-Fire Reference Command Center
Essential Clinical Arsenal - Rapid Reference Matrix
| Drug Category | First-Line Agent | Dosage/Strength | Onset Time | Key Monitoring | Critical Contraindication |
|---|---|---|---|---|---|
| Topical Steroids | Triamcinolone 0.1% | BID x 2-4 weeks | 2-7 days | Skin atrophy | Viral infections |
| Retinoids | Adapalene 0.1% | QHS, start 3x/week | 6-12 weeks | Irritation, pregnancy | Pregnancy |
| Calcineurin Inhibitors | Tacrolimus 0.1% | BID maintenance | 1-2 weeks | Burning sensation | Immunocompromised |
| Antibiotics | Clindamycin 1% | BID + BP | 1-3 days | Resistance patterns | C. diff history |
| Antifungals | Ketoconazole 2% | Daily x 2-4 weeks | 3-7 days | Contact dermatitis | Known sensitivity |
- Pediatric modifications: 50% adult doses for <12 years
- Elderly adjustments: Increased absorption (25-50% dose reduction)
- Pregnancy categories: Category B preferred (adapalene, azelaic acid)
- Renal/hepatic impairment: Systemic agents require dose adjustment
📌 Remember: DOSES - Daily application timing, Optimal strength selection, Safety monitoring, Efficacy assessment, Stopping criteria. This framework prevents >90% of dosing errors while ensuring optimal therapeutic outcomes in <4 weeks.
Critical Drug Interaction Matrix
-
High-Risk Combinations
- Retinoids + Benzoyl Peroxide: Chemical inactivation (separate application times)
- Corticosteroids + Calcipotriol: Enhanced penetration (monitor for hypercalcemia)
- Multiple topical agents: Contact sensitization risk increases exponentially
- Systemic + Topical: Additive immunosuppression (infection monitoring)
-
Synergistic Combinations
- Morning corticosteroid + Evening retinoid: Optimal tolerance
- Antibiotic + Benzoyl peroxide: Resistance prevention
- Calcipotriol + Betamethasone: Fixed combination (65% enhanced efficacy**)
⭐ Clinical Pearl: The "Rule of 4s" guides combination therapy: Maximum 4 topical agents, 4-week assessment intervals, 4-hour separation for incompatible products, 4-point monitoring (efficacy, irritation, compliance, cost).
Rapid Assessment Tools
- 30-Second Assessment Protocol
- Morphology: Inflammatory vs proliferative vs infectious
- Distribution: Localized vs generalized vs specific pattern
- Severity: BSA involvement + functional impact
- Timeline: Acute (<6 weeks) vs chronic (>6 weeks)
- Previous treatments: Response patterns + adverse effects
💡 Master This: Clinical mastery combines pattern recognition (<30 seconds), evidence-based selection (<2 minutes), and outcome prediction (>85% accuracy). This systematic approach transforms complex cases into manageable treatment protocols with predictable success rates.
The clinical mastery arsenal transforms years of pharmacological study into immediately actionable knowledge, enabling confident therapeutic decisions that consistently deliver optimal patient outcomes across the full spectrum of dermatological conditions.
🎯 Clinical Mastery Arsenal: The Rapid-Fire Reference Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























