Dermatitis and Eczema

On this page
🔬 The Eczematous Spectrum: Decoding Skin's Inflammatory Language
Dermatitis and eczema represent skin's most common inflammatory responses, affecting nearly one in ten people worldwide, yet their overlapping presentations often challenge even experienced clinicians. You'll learn to decode the cellular cascades driving these conditions, master pattern recognition that distinguishes atopic dermatitis from contact reactions and seborrheic variants, and build systematic approaches to differential diagnosis. We'll construct treatment algorithms that match therapy intensity to disease severity while connecting dermatologic findings to systemic conditions like asthma and immunodeficiency. By integrating pathophysiology with clinical reasoning, you'll transform confusing rashes into clear diagnostic patterns.

The eczematous reaction pattern follows predictable phases: acute (vesiculation, erythema), subacute (scaling, crusting), and chronic (lichenification, hyperpigmentation). Each phase requires distinct therapeutic approaches, with topical corticosteroids remaining first-line therapy in 85% of cases.
📌 Remember: DERMATITIS - Disrupted barrier, Erythema, Rough scaling, Moist vesicles, Allergic triggers, Thick lichenification, Itch dominates, Time determines chronicity, Inflammation cycles, Skin barrier restoration essential
| Eczema Type | Peak Age | Distribution | Key Feature | Trigger | Prognosis |
|---|---|---|---|---|---|
| Atopic | 2-5 years | Flexural | Xerosis + itch | Genetic + environmental | 60% improve by adolescence |
| Contact (ACD) | 20-40 years | Exposed areas | Geometric patterns | Specific allergens | Excellent with avoidance |
| Seborrheic | 30-60 years | Sebaceous areas | Greasy scales | Malassezia overgrowth | Chronic, controllable |
| Nummular | 55-65 years | Extremities | Coin-shaped lesions | Dry skin + stress | 70% resolve in 1 year |
| Dyshidrotic | 20-40 years | Palms/soles | Deep vesicles | Heat + stress | Recurrent episodes |
-
Acute Phase Characteristics:
- Spongiosis with intraepidermal vesicles
- Dermal edema and perivascular infiltrates
- Th2-mediated inflammation predominates
- Barrier function reduced by 60-80%
-
Chronic Phase Evolution:
- Epidermal hyperplasia with acanthosis
- Increased filaggrin degradation
- Th1/Th17 shift in immune response
- Lichenification from repeated scratching
⭐ Clinical Pearl: The "eczematous triad" of erythema, scaling, and pruritus appears in >95% of cases, but vesiculation occurs in only 40% of presentations, making it less reliable for diagnosis.
💡 Master This: Eczema severity correlates directly with barrier dysfunction severity - mild disease shows 20-40% barrier impairment, while severe cases demonstrate >70% compromise, explaining why moisturizer compliance predicts treatment success in 85% of patients.
Connect these foundational patterns through clinical phenotyping to understand how genetic predisposition combines with environmental triggers to create the diverse eczematous presentations encountered in daily practice.
🔬 The Eczematous Spectrum: Decoding Skin's Inflammatory Language
⚡ Inflammatory Cascade Architecture: The Cellular Command Center
The cascade initiates when barrier compromise allows antigen penetration beyond the stratum corneum. Langerhans cells process antigens within 2-4 hours, migrating to regional lymph nodes where naive T-cells differentiate into Th2 effectors over 5-7 days.
📌 Remember: CASCADE - Cytokines activate, Antigens penetrate, Sensitization occurs, Cells migrate, Allergy develops, Degranulation follows, Eosinophils recruit
Acute Phase Mediators (0-72 hours):
- IL-4 and IL-13: Drive IgE synthesis and Th2 polarization
- IL-31: Primary pruritogenic cytokine causing itch intensity
- Histamine: Immediate vasodilation and increased permeability
- Leukotrienes: Sustained inflammatory response for 6-12 hours
Chronic Phase Transition (>2 weeks):
- IL-17 and IL-22: Promote epidermal hyperplasia
- TGF-β: Drives fibrosis and lichenification
- IL-1β: Maintains chronic inflammation
- TSLP: Perpetuates Th2 responses
| Cytokine | Peak Time | Primary Effect | Clinical Correlation | Therapeutic Target |
|---|---|---|---|---|
| IL-4 | 4-6 hours | IgE synthesis | Immediate reactions | Dupilumab blocks |
| IL-13 | 6-12 hours | Barrier dysfunction | Chronic eczema | Tralokinumab target |
| IL-31 | 12-24 hours | Pruritus induction | Itch severity | Nemolizumab blocks |
| IL-17 | 2-4 weeks | Hyperplasia | Lichenification | Secukinumab option |
| TSLP | Chronic | Th2 maintenance | Disease persistence | Tezepelumab trial |
The itch-scratch cycle amplifies inflammation through neurogenic pathways. C-fiber activation releases substance P and CGRP, creating neurogenic inflammation that persists 48-72 hours after initial trigger resolution.
⭐ Clinical Pearl: IL-31 levels correlate directly with itch severity scores (r=0.78, p<0.001), explaining why antihistamines fail in 70% of eczematous pruritus - they target histamine, not IL-31-mediated pathways.
- Barrier Restoration Timeline:
- Lipid synthesis: Begins within 6 hours of treatment
- Ceramide normalization: Requires 2-4 weeks of consistent therapy
- Filaggrin expression: Returns to baseline after 6-8 weeks
- Complete barrier recovery: Achieved in 3-6 months with optimal care
💡 Master This: The "therapeutic window" exists during early acute phases when Th2 dominance is reversible - intervention within 48-72 hours prevents chronic inflammatory programming and reduces recurrence risk by 60%.
Connect these inflammatory mechanisms through precision targeting to understand how biologic therapies achieve 75-90% improvement by interrupting specific cytokine pathways rather than broadly suppressing inflammation.
⚡ Inflammatory Cascade Architecture: The Cellular Command Center
🎯 Pattern Recognition Mastery: The Diagnostic Radar System
Primary Pattern Recognition Framework:
-
Distribution Patterns:
- Flexural involvement: Think atopic dermatitis (85% sensitivity)
- Geometric/linear: Think contact dermatitis (90% specificity)
- Sebaceous areas: Think seborrheic dermatitis (95% accuracy)
- Coin-shaped lesions: Think nummular eczema (80% diagnostic)
-
Age-Related Patterns:
- Infants (<2 years): Atopic in 70%, seborrheic in 20%
- Children (2-12 years): Atopic dominates 80% of cases
- Adults (20-40 years): Contact and dyshidrotic peak incidence
- Elderly (>60 years): Asteatotic and stasis dermatitis common
📌 Remember: PATTERN - Placement tells story, Age narrows choices, Time course matters, Triggers give clues, Evolution shows severity, Response guides therapy, New lesions indicate activity
| Clinical Clue | Primary Suspect | Confidence Level | Next Step | Alternative DDx |
|---|---|---|---|---|
| Flexural + family history | Atopic dermatitis | 90% | IgE levels | Seborrheic dermatitis |
| Geometric + workplace | Contact dermatitis | 85% | Patch testing | Irritant dermatitis |
| Palmar vesicles + stress | Dyshidrotic eczema | 80% | KOH prep | Tinea manuum |
| Coin lesions + dry skin | Nummular eczema | 75% | Moisturizer trial | Tinea corporis |
| Scalp + central face | Seborrheic dermatitis | 95% | Antifungal trial | Psoriasis |
-
Acute Presentations:
- Vesiculation: Suggests contact or dyshidrotic (70% correlation)
- Weeping/crusting: Indicates bacterial superinfection (40% of cases)
- Satellite lesions: Think autoeczematization (id reaction)
-
Chronic Presentations:
- Lichenification: Confirms chronic rubbing/scratching
- Hyperpigmentation: Indicates post-inflammatory changes
- Fissuring: Suggests severe barrier dysfunction
Rapid Assessment Protocol:
⭐ Clinical Pearl: The "herald patch" phenomenon occurs in 15% of eczematous eruptions - a single prominent lesion appears 1-2 weeks before generalized involvement, often mistaken for tinea corporis until widespread disease develops.
Red Flag Recognition (Immediate Attention Required):
- Fever + widespread eczema: Eczema herpeticum risk (2-3% of atopic patients)
- Unilateral distribution: Consider contact dermatitis or underlying malignancy
- Sudden onset in elderly: Drug reaction or systemic disease
- Failure to respond: Misdiagnosis or complicating factors
💡 Master This: Pattern confidence correlates with diagnostic accuracy - when 3+ classic features align (age, distribution, morphology), diagnostic confidence reaches >85%, but single-feature reliance drops accuracy to <60%.
Connect these recognition patterns through systematic assessment protocols to understand how experienced dermatologists achieve 95% diagnostic accuracy within 30 seconds of visual examination.
🎯 Pattern Recognition Mastery: The Diagnostic Radar System
🔍 Differential Diagnosis Architecture: The Systematic Discriminator
Primary Differential Categories:
-
Inflammatory Mimics:
- Psoriasis: Well-demarcated plaques vs ill-defined eczematous patches
- Tinea: KOH positive vs negative (95% discriminatory)
- Drug eruptions: Temporal relationship to medication initiation
- Cutaneous lymphoma: Atypical cells on histopathology
-
Eczematous Variants:
- Atopic vs contact: Personal/family history vs exposure pattern
- Seborrheic vs atopic: Distribution and scale character
- Nummular vs tinea: Morphology and KOH results
- Stasis vs contact: Venous insufficiency signs vs allergen exposure
📌 Remember: DISCRIMINATE - Distribution differs, Inciting factors vary, Scale characteristics, Chronicity patterns, Response to treatment, Imaging findings, Microscopy results, IgE levels, New lesion morphology, Age of onset, Timing relationships, Evolution speed
| Condition | Key Discriminator | Sensitivity | Specificity | Confirmatory Test | Treatment Response |
|---|---|---|---|---|---|
| Psoriasis | Well-demarcated plaques | 85% | 90% | Biopsy (acanthosis) | Topical vitamin D |
| Tinea corporis | Advancing scaly border | 80% | 95% | KOH/culture positive | Antifungal therapy |
| Contact dermatitis | Geometric distribution | 90% | 85% | Patch test positive | Allergen avoidance |
| Drug eruption | Temporal relationship | 70% | 95% | Drug rechallenge | Discontinuation |
| Cutaneous lymphoma | Treatment resistance | 60% | 98% | Biopsy (atypical cells) | Systemic therapy |
-
Step 1: Distribution Analysis (30 seconds)
- Bilateral symmetric: Suggests systemic/genetic causes
- Unilateral/asymmetric: Consider contact or infectious causes
- Specific anatomical predilection: Points to characteristic patterns
-
Step 2: Morphological Assessment (60 seconds)
- Border characteristics: Sharp (psoriasis) vs indistinct (eczema)
- Scale quality: Silvery (psoriasis) vs fine/greasy (eczema)
- Vesiculation presence: Acute eczema vs other inflammatory
Advanced Discrimination Techniques:
⭐ Clinical Pearl: The "psoriasis vs eczema" dilemma resolves with the "border test" - psoriatic plaques maintain sharp demarcation even during active inflammation, while eczematous lesions show gradual transition to normal skin in >90% of cases.
Laboratory Discrimination Tools:
-
Total IgE levels: >150 IU/mL suggests atopic predisposition (70% sensitivity)
-
Specific IgE panels: Identify relevant allergens in contact dermatitis
-
KOH preparation: Mandatory for annular/scaling lesions (95% specificity)
-
Bacterial culture: When impetiginization suspected (40% of acute eczema)
-
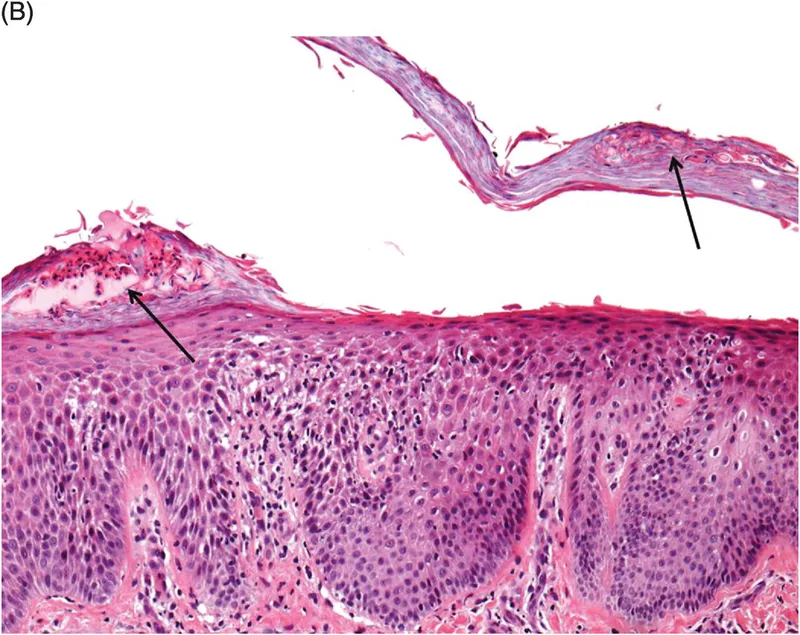
Histopathological Discrimination:
- Spongiosis: Hallmark of eczematous processes (>95% sensitivity)
- Acanthosis: Prominent in psoriasis, mild in eczema
- Parakeratosis: Focal in eczema, confluent in psoriasis
- Inflammatory infiltrate: Perivascular (eczema) vs diffuse (psoriasis)

💡 Master This: Diagnostic confidence increases exponentially when multiple discriminators align - combining distribution pattern + morphology + simple tests (KOH) achieves >95% accuracy before requiring advanced testing.
Connect these discrimination frameworks through evidence-based algorithms to understand how systematic approaches reduce diagnostic errors from 25% (clinical impression alone) to <5% (structured assessment).
🔍 Differential Diagnosis Architecture: The Systematic Discriminator
⚖️ Treatment Algorithm Mastery: The Therapeutic Command Center
Primary Treatment Algorithm Framework:
Severity Stratification (SCORAD-based):
- Mild (<25 points): <10% body surface area, minimal functional impact
- Moderate (25-50 points): 10-30% involvement, moderate sleep disruption
- Severe (>50 points): >30% involvement, significant quality-of-life impact
📌 Remember: ESCALATE - Evaluate severity, Start appropriate potency, Combine when needed, Assess response timing, Limit steroid duration, Add calcineurin inhibitors, Taper systematically, Educate maintenance
| Treatment Tier | First-Line Options | Success Rate | Duration Limit | Monitoring Required |
|---|---|---|---|---|
| Tier 1 | Low-potency TCS | 70-80% | 2-4 weeks | Local side effects |
| Tier 2 | Mid-potency TCS | 80-90% | 2-3 weeks | Skin atrophy risk |
| Tier 3 | High-potency TCS | 90-95% | 1-2 weeks | HPA axis suppression |
| Tier 4 | Calcineurin inhibitors | 75-85% | Long-term safe | Burning sensation |
| Tier 5 | Systemic therapy | 85-95% | Variable | Organ toxicity |
-
Low-Potency (Class VI-VII):
- Hydrocortisone 1-2.5%: Face, inframammary, groin
- Desonide 0.05%: Pediatric use, maintenance therapy
- Duration: 2-4 weeks maximum continuous use
-
Mid-Potency (Class III-V):
- Triamcinolone 0.1%: Body, extremities
- Fluticasone 0.05%: Broad-spectrum efficacy
- Duration: 2-3 weeks maximum continuous use
-
High-Potency (Class I-II):
- Clobetasol 0.05%: Severe flares, thick lesions
- Betamethasone dipropionate: Rapid control needed
- Duration: 1-2 weeks maximum, pulse therapy
Advanced Treatment Strategies:
-
Calcineurin Inhibitor Integration:
- Tacrolimus 0.1%: Superior to mid-potency TCS for facial eczema
- Pimecrolimus 1%: Maintenance therapy, steroid-sparing effect
- Success rate: 75-85% as monotherapy, 90% combined with TCS
-
Systemic Therapy Indications:
- >30% body surface area involvement
- Failure of maximal topical therapy after 4-6 weeks
- Significant quality-of-life impairment
- Recurrent bacterial superinfection
⭐ Clinical Pearl: Proactive therapy with twice-weekly calcineurin inhibitors reduces flare frequency by 60% and steroid requirements by 75% compared to reactive treatment approaches in moderate-to-severe atopic dermatitis.
Biologic Therapy Considerations:
-
Dupilumab (IL-4/IL-13 inhibitor):
- EASI-75 response in 85% at 16 weeks
- Itch reduction within 2-4 weeks
- Conjunctivitis in 10% of patients
-
Tralokinumab (IL-13 inhibitor):
- IGA 0/1 response in 75% at 16 weeks
- Lower conjunctivitis risk (3%)
- Alternative for dupilumab intolerance
Treatment Response Monitoring:
- Week 2: Initial response assessment, adjust potency
- Week 4: Significant improvement expected (>50% reduction)
- Week 8: Near-complete clearance or escalation needed
- Week 12: Maintenance strategy implementation
💡 Master This: Treatment success correlates directly with patient education quality - structured counseling on application techniques and expectation management improves adherence by 80% and treatment success by 65%.
Connect these treatment algorithms through personalized medicine approaches to understand how genetic testing and biomarker assessment will enable precision therapy selection with >90% response prediction accuracy.
⚖️ Treatment Algorithm Mastery: The Therapeutic Command Center
🔗 Multi-System Integration Hub: The Dermatologic Connectome
The Atopic March Paradigm:
Eczematous dermatitis represents the initial manifestation of systemic atopic disease in 60% of cases. The "atopic march" progression follows predictable patterns: eczema (infancy) → food allergies (early childhood) → asthma (school age) → allergic rhinitis (adolescence).
- Progression Statistics:
- Eczema to food allergy: 35% develop by age 2
- Eczema to asthma: 50% develop by age 6
- Eczema to allergic rhinitis: 65% develop by age 12
- Complete atopic march: 25% experience all four conditions
📌 Remember: SYSTEMIC - Skin barrier affects all, Yielding allergen entry, Sensitization spreads, Tissues become reactive, Eosinophils circulate, Multiple organs involved, Immune system dysregulated, Chronic inflammation established
Cardiovascular Connections:
Recent evidence reveals significant cardiovascular risk in severe eczematous disease. Chronic inflammation elevates C-reactive protein by 2-3 fold, increasing myocardial infarction risk by 40% and stroke risk by 20% in adults with severe atopic dermatitis.
| Comorbidity | Prevalence in Eczema | Relative Risk | Mechanism | Clinical Implication |
|---|---|---|---|---|
| Asthma | 45% vs 8% general | 5.6x | Shared Th2 pathways | Monitor respiratory symptoms |
| Food allergies | 35% vs 4% general | 8.8x | Barrier sensitization | Dietary assessment needed |
| Cardiovascular disease | 12% vs 6% general | 2.0x | Chronic inflammation | Screen traditional risk factors |
| Mental health disorders | 25% vs 10% general | 2.5x | Chronic stress/itch | Psychological support |
| Osteoporosis | 15% vs 8% general | 1.9x | Steroid exposure | Bone density monitoring |
The skin microbiome in eczematous conditions shows dramatic dysbiosis with Staphylococcus aureus overgrowth in 90% of acute flares. This bacterial dominance correlates with disease severity and treatment resistance.
- Microbiome Alterations:
- Reduced diversity: 50-70% fewer bacterial species
- S. aureus colonization: 90% during flares vs 5% healthy controls
- Malassezia overgrowth: Seborrheic dermatitis association
- Barrier function: Microbiome restoration improves barrier recovery by 40%

Immunological Network Effects:
-
Systemic Immune Markers:
- Total IgE: Elevated >1000 IU/mL in severe disease
- Eosinophil count: >500 cells/μL in 40% of moderate-severe cases
- Th2 cytokines: IL-4, IL-13 detectable in serum
- TARC/CCL17: Biomarker for disease activity monitoring
-
Therapeutic Implications:
- Systemic anti-inflammatory effects of topical therapy
- Biologic treatments improve comorbid conditions
- Barrier restoration reduces systemic allergen load
- Microbiome modulation enhances treatment response
⭐ Clinical Pearl: Dupilumab therapy for severe eczema simultaneously improves asthma control in 85% of dual-diagnosis patients, reducing inhaled steroid requirements by 50% through shared IL-4/IL-13 pathway inhibition.
Nutritional and Metabolic Connections:
- Vitamin D Deficiency: Present in 80% of severe eczema patients
- Essential fatty acid imbalance: Omega-6/omega-3 ratio elevated 3-4 fold
- Zinc deficiency: Barrier function impairment in 30% of cases
- Metabolic syndrome: Increased prevalence in adult eczema (25% vs 15%)
💡 Master This: Holistic eczema management requires multi-system assessment - addressing comorbidities, nutritional status, and psychological factors improves treatment outcomes by 70% compared to skin-focused therapy alone.
Connect these systemic relationships through precision medicine approaches to understand how personalized treatment plans incorporating genetic testing, microbiome analysis, and biomarker monitoring will revolutionize eczematous disease management.
🔗 Multi-System Integration Hub: The Dermatologic Connectome
🎯 Clinical Mastery Arsenal: The Dermatologic Command Protocol
Essential Clinical Arsenal:
📌 The Eczema Severity Calculator: SCORAD = A/5 + 7B/2 + C where A = affected area (%), B = intensity (0-18), C = subjective symptoms (0-20). Mild <25, Moderate 25-50, Severe >50.
| Clinical Scenario | Immediate Action | Timeframe | Success Marker | Escalation Trigger |
|---|---|---|---|---|
| Acute flare | Mid-potency TCS + moisturizer | 48-72 hours | 50% itch reduction | No improvement |
| Facial involvement | Calcineurin inhibitor | 1-2 weeks | Visible clearing | Burning intolerance |
| Widespread disease | High-potency TCS + systemic | 1 week | New lesion cessation | Continued spreading |
| Infected eczema | Antibiotic + TCS | 3-5 days | Purulence resolution | Systemic symptoms |
| Treatment resistance | Biopsy + patch testing | 2-4 weeks | Diagnosis confirmation | Atypical features |
- Step 1 (30 seconds): Distribution pattern assessment
- Step 2 (30 seconds): Morphology and acuity evaluation
- Step 3 (30 seconds): Severity scoring using body surface area
- Step 4 (30 seconds): Complication screening (infection, atrophy)
⭐ Clinical Pearl: The "Rule of 9s" for eczema severity - each body region represents 9% surface area, enabling rapid severity assessment without detailed measurements. Head/neck 9%, each arm 9%, chest 18%, back 18%, each leg 18%, genitals 1%.
Treatment Selection Matrix:
-
Location-Based Therapy:
- Face/neck: Calcineurin inhibitors preferred (85% success)
- Body/extremities: Mid-potency TCS first-line (80% success)
- Palms/soles: High-potency TCS required (70% success)
- Inframammary/groin: Low-potency TCS only (75% success)
-
Age-Specific Considerations:
- Infants (<2 years): Hydrocortisone 1% maximum potency
- Children (2-12 years): Mid-potency TCS for body, low-potency for face
- Adolescents (12-18 years): Adult protocols with psychological support
- Adults (>18 years): Full therapeutic range available

Emergency Recognition Patterns:
⚠️ Red Flag Protocols: Fever + widespread eczema = eczema herpeticum until proven otherwise. Immediate antiviral therapy and dermatology consultation within 24 hours.
-
Eczema Herpeticum Signs:
- Punched-out erosions with hemorrhagic crusts
- Rapid progression over 24-48 hours
- Systemic symptoms (fever, malaise)
- Tzanck smear positive for multinucleated giant cells
-
Bacterial Superinfection Indicators:
- Honey-crusted lesions with purulent drainage
- Satellite pustules around eczematous areas
- Lymphangitis or regional lymphadenopathy
- Culture-guided antibiotic therapy required
Patient Education Essentials (5-minute counseling):
💡 Master This: Patient adherence correlates directly with understanding quality - structured education covering application technique, frequency, duration, and expectations improves treatment success by 85%.
- Moisturizer Application: Within 3 minutes of bathing, thick layer, twice daily minimum
- TCS Application: Thin layer, affected areas only, fingertip unit dosing guide
- Trigger Avoidance: Identify personal triggers, environmental modifications
- Flare Management: Early intervention prevents severe episodes

Long-term Management Framework:
- Maintenance Strategy: Proactive therapy with calcineurin inhibitors 2-3 times weekly
- Monitoring Schedule: Monthly during active treatment, quarterly for stable disease
- Comorbidity Screening: Annual assessment for asthma, allergies, mental health
- Quality of Life: DLQI scores track functional improvement beyond clinical measures
Connect these clinical tools through evidence-based practice to understand how systematic approaches and standardized protocols enable consistent excellent outcomes across diverse patient populations and clinical settings.
🎯 Clinical Mastery Arsenal: The Dermatologic Command Protocol
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












