Blistering Diseases

On this page
🔬 The Autoimmune Blister Blueprint: Decoding Skin's Cellular Rebellion
Blistering diseases represent a fascinating intersection where the immune system turns against the very architecture holding skin together, transforming microscopic protein failures into dramatic clinical presentations. You'll master the pathophysiology driving pemphigus and pemphigoid, learn to distinguish these life-threatening conditions through pattern recognition and targeted diagnostics, and command the immunosuppressive strategies that can mean the difference between remission and catastrophe. By connecting autoantibody specificity to blister location, integrating histology with immunofluorescence, and recognizing systemic associations, you'll build the diagnostic precision and therapeutic confidence essential for managing these complex autoimmune emergencies.
The autoimmune blistering disease spectrum encompasses 5 major categories affecting distinct anatomical planes. Pemphigus attacks intraepidermal desmosomes at depths of 0.1-0.5mm, while pemphigoid targets the dermal-epidermal junction at basement membrane level. Linear IgA disease creates subepidermal splits, dermatitis herpetiformis produces papillary dermal microabscesses, and epidermolysis bullosa represents inherited structural protein defects.
📌 Remember: PEMPHIGUS - Painful Erosions, Mucosal Predominance, Histology Intraepidermal, Grave Untreated Sequelae. Pemphigus vulgaris affects oral mucosa in 90% of cases, with mortality rates reaching 75% without treatment.
| Disease Category | Target Antigen | Split Level | Age Peak | Mucosal Involvement | Mortality Risk |
|---|---|---|---|---|---|
| Pemphigus Vulgaris | Dsg3/Dsg1 | Intraepidermal | 40-60 years | 90% | High |
| Bullous Pemphigoid | BP180/BP230 | Subepidermal | 70-80 years | 20% | Moderate |
| Cicatricial Pemphigoid | Multiple BMZ | Subepidermal | 60-70 years | 100% | Low |
| Linear IgA Disease | LAD-1/BP180 | Subepidermal | Bimodal | 70% | Low |
| Dermatitis Herpetiformis | Tissue TG | Subepidermal | 30-50 years | Rare | Minimal |
⭐ Clinical Pearl: Nikolsky sign positivity indicates active acantholysis - gentle lateral pressure creates epidermal separation in 85% of active pemphigus cases but only 15% of pemphigoid cases.
💡 Master This: Desmoglein compensation theory explains clinical patterns - Dsg1 predominates in superficial epidermis, Dsg3 in deep epidermis and mucosa. Dsg3 antibodies alone cause mucosal-only disease, while Dsg1+Dsg3 antibodies create mucocutaneous presentations.
Diagnostic precision requires tissue biopsy from perilesional skin within 24-48 hours of blister formation. Direct immunofluorescence reveals characteristic patterns - intercellular staining in pemphigus, linear basement membrane deposition in pemphigoid. Indirect immunofluorescence titers correlate with disease activity in 70-80% of cases.
The clinical spectrum ranges from localized presentations affecting <5% body surface area to generalized disease involving >30% skin surface. Mortality rates vary dramatically: untreated pemphigus vulgaris carries 75% mortality, while bullous pemphigoid shows 10-15% mortality primarily from complications rather than disease progression.
Understanding this autoimmune blueprint enables rapid pattern recognition and guides targeted therapeutic interventions that can transform patient outcomes from devastating to manageable.
🔬 The Autoimmune Blister Blueprint: Decoding Skin's Cellular Rebellion
⚔️ Pemphigus Pathogenesis: The Desmoglein Wars

Desmoglein compensation theory provides the mechanistic framework for understanding clinical presentations. Desmoglein 3 (Dsg3) predominates in basal and suprabasal layers plus mucous membranes, while Desmoglein 1 (Dsg1) concentrates in superficial epidermal layers. Antibody specificity determines anatomical distribution of disease manifestations.
📌 Remember: DSG WARS - Dsg3 Suprabasal Grip, Weak Adhesion Releases Superficial layers. Dsg3 antibodies alone cause mucosal-only disease in 60% of early pemphigus vulgaris cases.
The molecular cascade begins with autoantibody binding to extracellular domains of desmoglein proteins. Steric hindrance prevents trans-interaction between opposing cell surfaces, while complement activation amplifies tissue damage. Plasminogen activator upregulation creates proteolytic microenvironment that accelerates desmosome dissolution.
| Pemphigus Type | Primary Target | Secondary Target | Split Level | Mucosal Risk | Mortality |
|---|---|---|---|---|---|
| Vulgaris | Dsg3 | Dsg1 | Suprabasal | 90% | High |
| Foliaceus | Dsg1 | None | Subcorneal | <5% | Low |
| Vegetans | Dsg3 | Dsg1 | Suprabasal | 95% | Moderate |
| Erythematosus | Dsg1 | Nuclear | Subcorneal | Rare | Minimal |
| Paraneoplastic | Multiple | Plakins | Variable | 100% | Very High |
⭐ Clinical Pearl: Antibody titers correlate with disease activity in 70% of pemphigus vulgaris cases. Dsg3 ELISA values >20 units indicate active disease, while <10 units suggest clinical remission.
Genetic susceptibility involves HLA associations - HLA-DRB1*04:02 and HLA-DQB1*05:03 increase pemphigus vulgaris risk by 14-fold in Ashkenazi Jewish populations. Environmental triggers include medications (penicillamine, captopril), infections (herpes viruses), and physical trauma (burns, UV exposure).
💡 Master This: Pemphigus antibodies demonstrate pathogenic potential - passive transfer of patient serum to neonatal mice reproduces acantholysis within 24-48 hours, proving direct causation rather than epiphenomenon.
Complement-independent mechanisms contribute significantly to pathogenesis. Direct antibody binding triggers intracellular signaling through p38 MAPK and c-Myc pathways, leading to keratinocyte apoptosis and cytoskeletal reorganization. Plasminogen activator upregulation creates proteolytic environment that accelerates desmosome breakdown.
The threshold effect explains clinical variability - subclinical acantholysis occurs when antibody levels exceed baseline compensation, but visible blistering requires overwhelming the repair mechanisms. Stress factors (infection, surgery, pregnancy) can precipitate clinical disease in subclinical cases.
Therapeutic implications emerge from understanding molecular targets - rituximab depletes B-cell clones producing pathogenic antibodies, while plasmapheresis provides rapid antibody removal. Desmoglein peptide therapy represents emerging treatment targeting specific epitopes without broad immunosuppression.
This molecular understanding transforms pemphigus from mysterious blistering to predictable autoimmune process, enabling targeted interventions that address root pathogenic mechanisms.
⚔️ Pemphigus Pathogenesis: The Desmoglein Wars
🎯 Clinical Pattern Recognition: The Blister Detective Framework
Blister morphology serves as the primary discriminator. Pemphigus creates flaccid, easily ruptured vesicles that collapse within hours, leaving shallow erosions with peripheral scale. Pemphigoid produces tense, thick-walled bullae that persist for days and heal with minimal scarring.
📌 Remember: TENSE vs FLACCID - Thick-walled Epidermal Normal Subepidermal Elevation (pemphigoid) versus Fragile Loose Acantholytic Cells Create Intraepidermal Defects (pemphigus).
Anatomical distribution patterns provide crucial diagnostic information:
- Pemphigus Vulgaris: Oral mucosa (90%), scalp, face, trunk - mucosal-predominant early disease
- Bullous Pemphigoid: Flexural areas, abdomen, thighs - skin-predominant with urticarial phase
- Cicatricial Pemphigoid: Mucous membranes (100%) - conjunctiva, oral, genital with scarring
- Linear IgA Disease: Perioral, anogenital, extensor surfaces - "string of pearls" configuration
- Dermatitis Herpetiformis: Elbows, knees, buttocks, scalp - symmetric and intensely pruritic
| Clinical Feature | Pemphigus | Bullous Pemphigoid | Cicatricial Pemphigoid | Linear IgA | Dermatitis Herpetiformis |
|---|---|---|---|---|---|
| Blister Type | Flaccid | Tense | Tense | Tense | Vesicles |
| Nikolsky Sign | Positive | Negative | Negative | Negative | Negative |
| Mucosal Risk | 90% | 20% | 100% | 70% | <5% |
| Pruritus | Mild | Severe | Moderate | Moderate | Intense |
| Scarring | Minimal | Rare | Universal | Rare | None |
⭐ Clinical Pearl: Nikolsky sign demonstrates >85% sensitivity for active pemphigus but <15% for pemphigoid. Gentle lateral pressure on perilesional skin creates epidermal separation only when active acantholysis is present.
Associated symptoms refine differential diagnosis. Intense pruritus suggests bullous pemphigoid or dermatitis herpetiformis, while painful erosions indicate pemphigus. Ocular symptoms (conjunctival scarring, symblepharon) point toward cicatricial pemphigoid.
Prodromal phases provide early diagnostic opportunities. Bullous pemphigoid often begins with urticarial lesions weeks to months before blistering. Pemphigus may present with isolated oral erosions for months before cutaneous involvement.
💡 Master This: "String of pearls" configuration - linear arrangement of small tense vesicles along inflammatory borders - pathognomonic for linear IgA bullous dermatosis and distinguishes it from other subepidermal blistering diseases.
Drug-induced patterns require specific recognition. Penicillamine causes pemphigus-like disease, vancomycin triggers linear IgA disease, while furosemide can precipitate bullous pemphigoid. Drug history within 6 months of onset suggests medication-induced disease.
Rapid assessment tools enable emergency department triage:
- Flaccid blisters + mucosal erosions = Pemphigus (urgent dermatology)
- Tense blisters + elderly + pruritus = Bullous pemphigoid (moderate urgency)
- Conjunctival involvement + scarring = Cicatricial pemphigoid (ophthalmology referral)
- Grouped vesicles + intense itch + gluten sensitivity = Dermatitis herpetiformis
Complications assessment guides immediate management. Extensive pemphigus (>30% body surface) requires hospitalization for fluid management and infection prevention. Ocular cicatricial pemphigoid needs urgent ophthalmology evaluation to prevent blindness.
This systematic pattern recognition framework transforms complex blistering presentations into manageable diagnostic algorithms, enabling rapid identification and appropriate urgent referrals.
🎯 Clinical Pattern Recognition: The Blister Detective Framework
🔬 Diagnostic Precision: Laboratory Confirmation Arsenal

Biopsy technique determines diagnostic success. Perilesional skin within 2-4mm of active blisters provides optimal DIF results, while intact early blisters yield best histopathology. Biopsy timing within 24-48 hours of blister formation maximizes diagnostic yield.
Histopathological patterns provide immediate diagnostic direction:
- Pemphigus: Intraepidermal split with acantholytic cells ("tombstoning" of basal layer)
- Bullous Pemphigoid: Subepidermal split with eosinophilic infiltrate
- Cicatricial Pemphigoid: Subepidermal split with neutrophilic infiltrate and fibrosis
- Linear IgA Disease: Subepidermal split with neutrophilic microabscesses
- Dermatitis Herpetiformis: Papillary dermal neutrophilic microabscesses
📌 Remember: SPLIT LEVELS - Intraepidermal Acantholysis (pemphigus), Subepidermal Eosinophils (bullous pemphigoid), Subepidermal Neutrophils (cicatricial pemphigoid/linear IgA), Papillary Neutrophils (dermatitis herpetiformis).
Direct Immunofluorescence (DIF) patterns provide pathognomonic findings:
| Disease | DIF Pattern | Primary Antibody | Secondary Pattern | Sensitivity |
|---|---|---|---|---|
| Pemphigus Vulgaris | Intercellular IgG | IgG4 | C3 intercellular | 90-95% |
| Bullous Pemphigoid | Linear BMZ IgG | IgG1 | C3 linear | 85-90% |
| Cicatricial Pemphigoid | Linear BMZ IgG | IgG1/IgA | Fibrin BMZ | 75-85% |
| Linear IgA Disease | Linear BMZ IgA | IgA | Minimal C3 | 90-95% |
| Dermatitis Herpetiformis | Granular IgA | IgA | Papillary tips | 85-90% |
⭐ Clinical Pearl: Salt-split skin IIF differentiates bullous pemphigoid (epidermal binding) from epidermolysis bullosa acquisita (dermal binding) with >95% accuracy. Dermal binding indicates worse prognosis and treatment resistance.
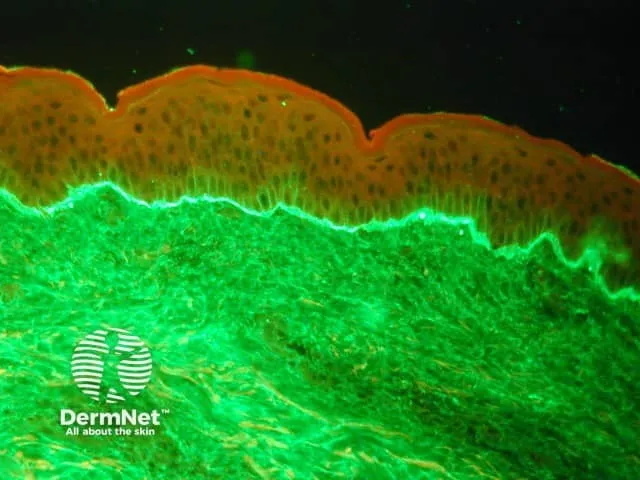
ELISA testing provides quantitative antibody measurement for disease monitoring. Desmoglein 1 and Desmoglein 3 ELISA correlate with pemphigus activity in 70-80% of cases. BP180 and BP230 ELISA predict bullous pemphigoid severity and treatment response.
Antigen-specific patterns guide targeted therapy:
- Dsg3-only antibodies: Mucosal-predominant pemphigus, better prognosis
- Dsg1+Dsg3 antibodies: Mucocutaneous disease, aggressive course
- BP180 antibodies: Inflammatory bullous pemphigoid, steroid-responsive
- BP230 antibodies: Non-inflammatory disease, milder course
💡 Master This: Epitope mapping reveals disease severity - N-terminal BP180 antibodies correlate with severe bullous pemphigoid, while C-terminal antibodies indicate localized disease with better prognosis.
Advanced testing includes immunoblotting for complex cases. Envoplakin and periplakin antibodies suggest paraneoplastic pemphigus, while laminin-332 antibodies indicate anti-epiligrin cicatricial pemphigoid with malignancy risk.
Quality control measures ensure diagnostic accuracy:
- Fresh-frozen tissue for DIF (not formalin-fixed)
- Transport medium for >24-hour delays
- Positive controls for each antibody
- Correlation with clinical presentation
Diagnostic algorithms integrate multiple parameters:
- Clinical pattern recognition (70% accuracy)
- Histopathology confirmation (85% accuracy)
- DIF pattern identification (90% accuracy)
- Antigen-specific testing (95% accuracy)
False-negative results occur in 5-15% of cases due to technical factors, early disease, or treatment effects. Repeat testing from new sites may be necessary in high clinical suspicion cases.
This comprehensive diagnostic arsenal transforms uncertain blistering presentations into precise molecular diagnoses, enabling targeted therapeutic interventions and accurate prognostic counseling.
🔬 Diagnostic Precision: Laboratory Confirmation Arsenal
⚖️ Treatment Algorithms: Evidence-Based Therapeutic Mastery
Severity stratification guides initial treatment intensity. Mild disease (<5% body surface area) receives topical therapy, moderate disease (5-30% BSA) requires systemic immunosuppression, while severe disease (>30% BSA) demands hospitalization and aggressive intervention.
Pemphigus treatment protocols prioritize rapid disease control due to high mortality risk:
First-line pemphigus therapy employs prednisolone at 1-1.5mg/kg/day (maximum 80-100mg daily) for disease control. Response rates reach 85-90% within 2-4 weeks, with new blister cessation as the primary endpoint.
📌 Remember: PEMPHIGUS PROTOCOL - Prednisolone 1mg/kg, Evaluate 2 weeks, Methylprednisolone Pulse if severe, Hospitalize >30% BSA, Immunoglobulin Gamma if resistant, Use Rituximab early, Steroid-sparing agents.
| Treatment Phase | Duration | Primary Agent | Dose | Success Rate | Key Monitoring |
|---|---|---|---|---|---|
| Induction | 2-8 weeks | Prednisolone | 1-1.5mg/kg | 85-90% | New blisters |
| Consolidation | 2-6 months | Steroid taper | 10mg/month | 70-80% | Antibody titers |
| Maintenance | 12-24 months | Steroid-sparing | Variable | 60-70% | Relapse prevention |
| Remission | >24 months | Monitoring | None | 40-50% | Clinical vigilance |
Bullous pemphigoid protocols emphasize symptom control and quality of life:
- Localized disease: Topical clobetasol 0.05% twice daily
- Generalized disease: Prednisolone 0.5-0.75mg/kg/day
- Elderly patients: Doxycycline 200mg daily plus nicotinamide 1.5g daily
⭐ Clinical Pearl: Doxycycline-nicotinamide combination achieves 70% response rates in elderly bullous pemphigoid patients with significantly lower adverse effects compared to systemic steroids (mortality reduction from 15% to 5%).
Cicatricial pemphigoid requires aggressive early intervention to prevent irreversible scarring:
- Ocular involvement: Systemic immunosuppression mandatory
- Oral disease: Topical steroids plus systemic therapy
- Genital involvement: Combination therapy to prevent strictures
Steroid-sparing agents reduce long-term complications:
- Azathioprine: 2-3mg/kg/day, onset 6-12 weeks
- Mycophenolate mofetil: 2-3g/day, onset 4-8 weeks
- Methotrexate: 15-25mg/week, onset 8-12 weeks
- Cyclophosphamide: 1-2mg/kg/day, severe cases only
💡 Master This: TPMT testing before azathioprine prevents life-threatening myelosuppression - 1:300 patients have deficient enzyme activity requiring dose reduction to <1mg/kg/day or alternative agents.
Adjuvant therapies enhance treatment efficacy:
- Plasmapheresis: Rapid antibody removal, bridge to immunosuppression
- IVIG: 2g/kg monthly, steroid-sparing in elderly patients
- Omalizumab: Anti-IgE therapy for refractory bullous pemphigoid
- Dupilumab: IL-4/IL-13 inhibition for pruritus control
Monitoring protocols ensure treatment safety:
- Complete blood count: Weekly during induction, monthly during maintenance
- Liver function tests: Monthly for methotrexate, azathioprine
- Bone density: Baseline and annual for chronic steroid use
- Infection screening: Hepatitis B/C, tuberculosis before rituximab
Treatment resistance occurs in 15-20% of cases, requiring combination therapy or experimental approaches:
- Rituximab plus IVIG
- Bortezomib (proteasome inhibitor)
- Alemtuzumab (anti-CD52)
- Chimeric antigen receptor T-cells (investigational)
Pregnancy considerations limit therapeutic options - topical steroids and prednisolone remain first-line, while azathioprine is relatively safe. Rituximab and methotrexate are contraindicated.
This evidence-based treatment framework transforms autoimmune blistering diseases from historically fatal conditions to manageable chronic diseases with excellent long-term prognoses.
⚖️ Treatment Algorithms: Evidence-Based Therapeutic Mastery
🌐 Multi-System Integration: The Autoimmune Constellation
Endocrine associations demonstrate shared autoimmune susceptibility. Dermatitis herpetiformis shows 90% association with celiac disease, while 15-20% of patients develop type 1 diabetes or thyroid disease. HLA-DQ2/DQ8 haplotypes predispose to multiple autoimmune conditions through molecular mimicry mechanisms.
Gastrointestinal connections extend beyond celiac disease. Pemphigus vulgaris patients show increased inflammatory bowel disease risk (3-fold elevation), while bullous pemphigoid associates with neurological conditions including dementia (2-fold risk) and Parkinson's disease (1.5-fold risk).
📌 Remember: AUTOIMMUNE CLUSTERS - Associated Understanding Thyroid Organ Involvement Multiple Manifestations Unify Neurologic Endocrine connections. Dermatitis herpetiformis patients require lifelong gluten-free diet and screening for diabetes (annual HbA1c) and thyroid dysfunction (annual TSH).
Malignancy associations require systematic screening protocols. Paraneoplastic pemphigus shows 90% association with hematologic malignancies (non-Hodgkin lymphoma, chronic lymphocytic leukemia, Castleman disease). Anti-epiligrin cicatricial pemphigoid carries 25% solid tumor risk, particularly adenocarcinomas.
| Blistering Disease | Associated Condition | Prevalence | Screening Protocol | Monitoring Frequency |
|---|---|---|---|---|
| Dermatitis Herpetiformis | Celiac Disease | 90% | Endoscopy + Serology | Annual |
| Paraneoplastic Pemphigus | Hematologic Malignancy | 90% | CT + Flow Cytometry | 6 months |
| Anti-epiligrin CP | Solid Tumors | 25% | Age-appropriate Screen | Annual |
| Bullous Pemphigoid | Neurological Disease | 15% | Cognitive Assessment | Annual |
| Linear IgA Disease | Drug Associations | 50% | Medication Review | Each visit |
Pharmacological interactions complicate multi-system management. Methotrexate requires folate supplementation and hepatotoxicity monitoring, while azathioprine interactions with allopurinol can cause life-threatening myelosuppression. Rituximab increases infection risk, particularly hepatitis B reactivation.
⭐ Clinical Pearl: Hepatitis B screening is mandatory before rituximab therapy - HBsAg-negative/anti-HBc-positive patients have 10-15% reactivation risk requiring prophylactic antiviral therapy with entecavir or tenofovir.
Genetic counseling becomes relevant for inherited forms. Epidermolysis bullosa shows Mendelian inheritance patterns requiring family screening and reproductive counseling. Genetic testing identifies specific mutations affecting prognosis and treatment selection.
Pregnancy implications affect multiple systems. Pemphigoid gestationis increases fetal growth restriction risk (15-20%) and preterm delivery (25-30%). Maternal antibodies can cause transient neonatal blistering in 5-10% of cases.
Nutritional considerations extend beyond gluten restriction. Chronic steroid therapy requires calcium (1200-1500mg daily) and vitamin D (800-1000 IU daily) supplementation. Malabsorption in dermatitis herpetiformis may necessitate B-vitamin, iron, and fat-soluble vitamin replacement.
💡 Master This: Bone health monitoring in chronic immunosuppression requires DEXA scanning at baseline, 1 year, and every 2 years thereafter. Bisphosphonate therapy reduces fracture risk by 40-50% in high-risk patients.
Quality of life assessment incorporates multi-system impact. Dermatology Life Quality Index (DLQI) scores >10 indicate severe impairment, while pain scales and functional assessments guide comprehensive management approaches.
Emerging therapeutic targets address multi-system pathways. JAK inhibitors show promise for multiple autoimmune conditions, while complement inhibitors target shared inflammatory cascades. Precision medicine approaches use genetic profiling to predict treatment responses.
Long-term monitoring protocols integrate multi-system surveillance:
- Annual comprehensive metabolic panel
- Thyroid function and autoantibody screening
- Cancer surveillance based on disease associations
- Bone density and cardiovascular risk assessment
- Infection screening for opportunistic pathogens
This multi-system integration framework transforms isolated skin disease management into comprehensive autoimmune care, optimizing outcomes across all affected organ systems while minimizing treatment-related complications.
🌐 Multi-System Integration: The Autoimmune Constellation
🎯 Clinical Mastery Arsenal: Rapid-Fire Diagnostic Tools
The 60-Second Blister Assessment Protocol:
- Age + Distribution (15 seconds): Elderly + flexural = bullous pemphigoid
- Blister morphology (15 seconds): Flaccid + erosions = pemphigus
- Mucosal involvement (15 seconds): Oral erosions = pemphigus/cicatricial
- Nikolsky sign (15 seconds): Positive = active pemphigus
📌 Remember: RAPID BLISTER - Recognize Age Pattern, Identify Distribution, Blister Look, Involvement Sites, Test Epidermis Rub. Elderly + tense blisters + flexural = bullous pemphigoid (moderate urgency). Any age + flaccid blisters + mucosal = pemphigus (high urgency).
Essential Numbers Arsenal:
- Pemphigus mortality: 75% untreated, <10% with treatment
- Bullous pemphigoid elderly mortality: 15% (complications)
- Nikolsky sensitivity: 85% pemphigus, 15% pemphigoid
- Mucosal involvement: 90% pemphigus, 20% bullous pemphigoid
- Treatment response: 85% pemphigus responds to prednisolone 1mg/kg
| Rapid Recognition Matrix | Age Peak | Blister Type | Key Site | Urgency Level | First Action |
|---|---|---|---|---|---|
| Pemphigus Vulgaris | 40-60 | Flaccid | Oral | HIGH | Dermatology STAT |
| Bullous Pemphigoid | 70-80 | Tense | Flexural | MODERATE | Dermatology 24h |
| Cicatricial Pemphigoid | 60-70 | Tense | Conjunctiva | HIGH | Ophthalmology STAT |
| Linear IgA Disease | Bimodal | Tense | Perioral | LOW | Dermatology 1 week |
| Dermatitis Herpetiformis | 30-50 | Vesicles | Elbows | LOW | GI evaluation |
- >30% BSA involvement = Hospitalization required
- Conjunctival scarring = Urgent ophthalmology (prevent blindness)
- Respiratory symptoms + pemphigus = Paraneoplastic (oncology)
- Pregnancy + blisters = Pemphigoid gestationis (high-risk obstetrics)
Treatment Quick-Start Protocols:
Pemphigus Emergency Protocol:
- Prednisolone: 1mg/kg/day (max 80mg)
- Infection prophylaxis: Consider if >20% BSA
- Fluid management: Monitor electrolytes
- Pain control: Avoid NSAIDs (bleeding risk)
Bullous Pemphigoid Elderly Protocol:
- Localized: Clobetasol 0.05% twice daily
- Generalized: Doxycycline 200mg + nicotinamide 1.5g
- Severe: Prednisolone 0.5mg/kg (lower dose than pemphigus)
⭐ Clinical Pearl: Doxycycline-nicotinamide combination in elderly bullous pemphigoid reduces mortality from 15% to 5% compared to systemic steroids, with 70% response rates and minimal side effects.
Red Flag Indicators requiring immediate escalation:
- Nikolsky positive + >20% BSA = Severe pemphigus
- Conjunctival symblepharon = Cicatricial pemphigoid (blindness risk)
- Respiratory/laryngeal involvement = Paraneoplastic pemphigus
- Pregnancy + new blisters = Pemphigoid gestationis
Monitoring Essentials:
- New blister formation = Primary endpoint for treatment response
- Antibody titers = Disease activity in 70% of cases
- Infection signs = Leading cause of morbidity/mortality
- Steroid complications = Monitor glucose, blood pressure, bone health
💡 Master This: Treatment response timeline - Pemphigus should show new blister cessation within 2-4 weeks of adequate therapy. Continued new blisters after 2 weeks of prednisolone 1mg/kg indicates treatment failure requiring rituximab or pulse steroids.
Consultation Triggers:
- Dermatology STAT: Pemphigus, cicatricial pemphigoid
- Ophthalmology STAT: Any conjunctival involvement
- Oncology: Paraneoplastic pemphigus suspicion
- High-risk obstetrics: Pregnancy-associated blistering
- Gastroenterology: Dermatitis herpetiformis (celiac evaluation)
Patient Education Priorities:
- Infection prevention: Gentle skin care, avoid trauma
- Medication compliance: Steroid tapering importance
- Warning signs: New blisters, fever, vision changes
- Follow-up scheduling: Close monitoring during induction phase
This clinical mastery arsenal transforms complex autoimmune blistering diseases into manageable diagnostic and therapeutic challenges, enabling rapid, accurate, and life-saving clinical decisions.
🎯 Clinical Mastery Arsenal: Rapid-Fire Diagnostic Tools
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























