Social and Behavioral Sciences

On this page
🧠 Health Psychology Basics - Mind Matters Medically
Understanding why patients struggle to quit smoking, how chronic stress triggers disease, and what makes one conversation build trust while another destroys it-these are the clinical skills that transform good doctors into healers. This lesson equips you with frameworks from health psychology and behavioral science to decode the human factors shaping illness and recovery, from the biology of stress responses to evidence-based strategies for motivating lasting change. You'll learn to recognize the psychological forces at play in every patient encounter and apply communication techniques that improve adherence, outcomes, and the therapeutic relationship itself.

The biopsychosocial model serves as health psychology's foundational framework, recognizing that optimal health emerges from the dynamic interaction of biological vulnerabilities, psychological resources, and social support systems. Research demonstrates that psychological factors account for 30-40% of variance in treatment outcomes across major medical conditions, while chronic stress increases cardiovascular disease risk by 27% and depression doubles the likelihood of developing diabetes.
📌 Remember: BIOPSYCHOSOCIAL - Biological predisposition + Individual psychology + Operational behaviors + Psychological resources + Social environment + Yearning for health + Cognitive patterns + Health outcomes + Optimal interventions + Support systems + Organizational factors + Cultural context + Integrated care + Adaptive responses + Lifestyle modifications
Core Psychological Determinants of Health
-
Cognitive Factors
- Health beliefs and risk perceptions (accuracy varies 40-85% across populations)
- Self-efficacy beliefs (correlate r=0.52 with treatment adherence)
- Specific self-efficacy: confidence in particular health behaviors
- General self-efficacy: overall belief in personal capability
- Collective efficacy: community-level confidence in health outcomes
- Health locus of control (internal locus associated with 23% better outcomes)
-
Emotional Regulation Patterns
- Stress response systems (cortisol elevation >15 μg/dL predicts immune suppression)
- Emotional expression styles (emotional suppression increases inflammation markers by 18%)
- Adaptive emotional processing: healthy expression and regulation
- Maladaptive suppression: chronic emotional inhibition
- Emotional intelligence: ability to recognize and manage emotions effectively
-
Behavioral Health Patterns
- Health-promoting behaviors (exercise >150 minutes/week reduces mortality by 31%)
- Risk behavior clusters (smoking + alcohol + poor diet increases disease risk multiplicatively by 3.2x)
- Protective behaviors: regular exercise, balanced nutrition, adequate sleep
- Risk behaviors: substance use, sedentary lifestyle, poor stress management
- Behavior change readiness: motivation and capability for health modifications
| Psychological Factor | Health Impact | Measurement Tool | Clinical Threshold | Intervention Success Rate |
|---|---|---|---|---|
| Chronic Stress | CVD risk ↑27% | Perceived Stress Scale | Score >20 | 68% with CBT |
| Depression | Diabetes risk ↑2x | PHQ-9 | Score ≥10 | 72% with integrated care |
| Self-Efficacy | Adherence ↑52% | General Self-Efficacy Scale | Score <25 | 81% with skills training |
| Social Support | Mortality ↓50% | Multidimensional Scale | Score <60 | 64% with group interventions |
| Health Anxiety | Healthcare utilization ↑3x | Health Anxiety Inventory | Score >18 | 76% with exposure therapy |
💡 Master This: The stress-illness pathway operates through three primary mechanisms: direct physiological effects (cortisol-mediated immune suppression), indirect behavioral effects (poor health choices during stress), and healthcare utilization patterns (delayed seeking or excessive utilization).
Understanding these psychological foundations reveals how mental processes translate into measurable health outcomes, setting the stage for examining specific stress and coping mechanisms that determine individual resilience and vulnerability patterns.
🧠 Health Psychology Basics — Mind Matters Medically
⚡ Stress & Coping - Pressure Cooker Physiology
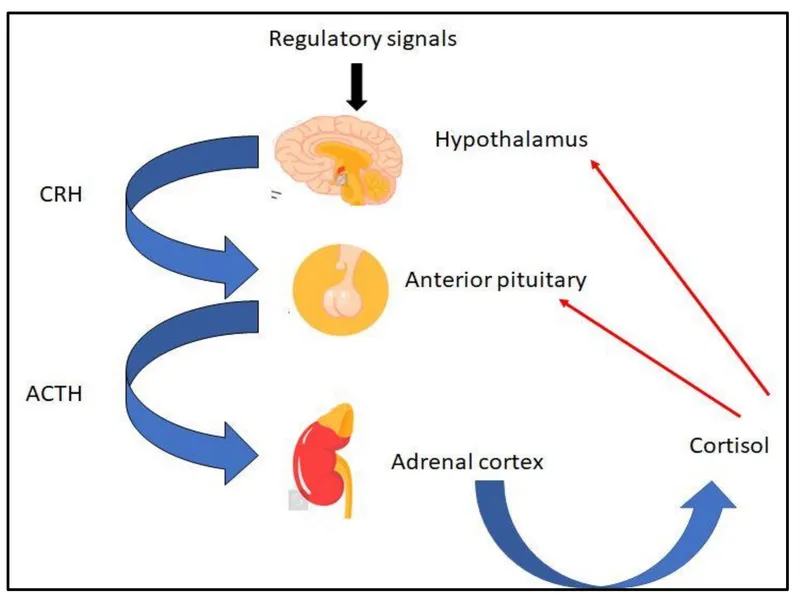
The hypothalamic-pituitary-adrenal (HPA) axis serves as the primary stress response system, with cortisol levels peaking within 20-30 minutes of stressor onset and returning to baseline within 60-90 minutes under normal circumstances. Chronic stress dysregulates this system, leading to sustained cortisol elevation >15 μg/dL that suppresses immune function, disrupts glucose metabolism, and accelerates cardiovascular disease progression.
📌 Remember: STRESS CASCADE - Stimulus triggers + Thalamic activation + Release of CRH + Endocrine response + Sympathetic activation + Systemic effects + Cortisol elevation + Adaptive responses + Suppressed immunity + Cardiovascular strain + Allostatic load + Disease vulnerability + Exhaustion phase
Physiological Stress Response Mechanisms
-
Acute Stress Response (Fight-or-Flight)
- Sympathetic nervous system activation within 2-3 seconds
- Epinephrine and norepinephrine release (peak levels at 5-10 minutes)
- Heart rate increases 20-40 beats per minute
- Blood pressure elevation 15-25 mmHg systolic
- Glucose mobilization increases blood sugar by 20-30%
- Enhanced cognitive performance and physical readiness
- Natural recovery within 30-60 minutes post-stressor
-
Chronic Stress Pathophysiology
- Sustained HPA axis activation (cortisol >12 μg/dL for >6 months)
- Allostatic load accumulation (wear-and-tear on multiple systems)
- Immune suppression: 30% reduction in lymphocyte function
- Metabolic dysfunction: insulin resistance increases by 40%
- Cardiovascular strain: hypertension risk increases 2.3-fold
- Neurological changes: hippocampal volume reduction of 8-12%
Coping Mechanisms and Health Outcomes
| Coping Strategy | Effectiveness Rating | Health Impact | Stress Reduction | Long-term Outcomes |
|---|---|---|---|---|
| Problem-Focused | 85% effective | Positive | 60-70% reduction | Improved resilience |
| Emotion-Focused | 70% effective | Mixed | 40-50% reduction | Variable outcomes |
| Avoidance | 25% effective | Negative | 10-20% reduction | Increased pathology |
| Social Support | 80% effective | Positive | 55-65% reduction | Enhanced well-being |
| Mindfulness | 75% effective | Positive | 45-55% reduction | Neuroplasticity benefits |
-
Adaptive Coping Strategies
- Problem-focused coping: direct action to modify stressor
- Emotion-focused coping: managing emotional responses when change isn't possible
- Cognitive reappraisal: reframing stressor interpretation
- Acceptance strategies: acknowledging unchangeable circumstances
- Meaning-making: finding purpose in difficult experiences
- Social support utilization (reduces cortisol by 23% and improves immune markers)
-
Maladaptive Coping Patterns
- Avoidance behaviors (increase anxiety by 35% and prolong stress exposure)
- Substance use as coping (alcohol increases cortisol by 18% and disrupts sleep quality)
- Behavioral avoidance: avoiding stress-related situations
- Cognitive avoidance: suppressing stress-related thoughts
- Emotional numbing: disconnecting from emotional experiences
- Rumination patterns (extend stress response by 200-300% beyond stressor duration)
💡 Master This: Allostatic load represents the cumulative physiological wear-and-tear from chronic stress exposure, measurable through 10 biomarkers including cortisol, blood pressure, cholesterol, and inflammatory markers, with scores >3 predicting 2.5-fold increased mortality risk.
📌 Remember: COPING TOOLKIT - Cognitive reappraisal + Optimal problem-solving + Physical exercise + Interpersonal support + Neuroplasticity training + Grounded mindfulness + Time management + Optimism cultivation + Organized planning + Lifestyle balance + Kindness practices + Inner resilience + Thought monitoring
The stress-coping relationship directly influences behavior change capacity, as chronic stress impairs the cognitive resources necessary for adopting and maintaining new health behaviors, connecting to the behavioral models that guide health psychology interventions.
⚡ Stress & Coping — Pressure Cooker Physiology
🔄 Behavior Change Models - Nudging New Habits

The Transtheoretical Model (TTM) conceptualizes behavior change as a process occurring through six distinct stages, with individuals spending average durations of 6 months in precontemplation, 6 months in contemplation, and requiring 3-6 attempts before achieving sustained behavior change. Research demonstrates that stage-matched interventions improve success rates by 40-60% compared to generic approaches.
📌 Remember: TTM STAGES - Precontemplation (unaware) + Recognition dawning + Evaluation phase + Commitment building + Organized action + New habits + Termination achieved + Ending old patterns + Maintenance mastery + Permanent change + Lifelong integration + Automatic behaviors + Transformation complete + Identity shift + Optimal health + New normal
Transtheoretical Model Framework
-
Stage-Specific Characteristics and Interventions
- Precontemplation (40% of population for any given behavior)
- No intention to change within next 6 months
- Intervention focus: consciousness-raising, dramatic relief
- Success strategy: increase awareness without pressure
- Contemplation (40% of population considering change)
- Intending to change within next 6 months
- Intervention focus: self-reevaluation, environmental reevaluation
- Success strategy: explore ambivalence, weigh pros/cons
- Preparation (20% of population ready for action)
- Planning to change within next 30 days
- Intervention focus: commitment, goal-setting, skill development
- Success strategy: concrete planning, barrier identification
- Precontemplation (40% of population for any given behavior)
-
Action and Maintenance Dynamics
- Action Stage (active behavior modification for <6 months)
- High relapse risk: 50-80% return to previous stages
- Intervention focus: stimulus control, contingency management
- Success factors: social support, self-monitoring, reward systems
- Maintenance Stage (sustained change for >6 months)
- Relapse risk decreases to 20-30% after 12 months
- Intervention focus: relapse prevention, lifestyle integration
- Success factors: habit formation, identity change, environmental modification
- Action Stage (active behavior modification for <6 months)

Health Belief Model Applications
| HBM Component | Clinical Application | Measurement Scale | Predictive Power | Intervention Target |
|---|---|---|---|---|
| Perceived Susceptibility | Disease risk awareness | 1-5 Likert scale | r=0.35 with behavior | Risk communication |
| Perceived Severity | Consequence understanding | 1-5 Likert scale | r=0.28 with behavior | Severity education |
| Perceived Benefits | Outcome expectations | 1-5 Likert scale | r=0.42 with behavior | Benefit highlighting |
| Perceived Barriers | Obstacle identification | 1-5 Likert scale | r=-0.38 with behavior | Barrier reduction |
| Self-Efficacy | Confidence in ability | 1-10 confidence scale | r=0.51 with behavior | Skills training |
- Perceived Threat (susceptibility × severity)
- Personal vulnerability assessment (accuracy varies 30-70% across conditions)
- Consequence severity evaluation (often underestimated by 40-50%)
- Threat perception threshold for action (moderate levels most motivating)
- Perceived Benefits vs. Barriers
- Outcome expectancies (benefits must outweigh barriers by 2:1 ratio)
- Barrier identification and problem-solving (reduces dropout by 35%)
- Cost-benefit analysis (both tangible and intangible factors)
- Social Cognitive Theory Elements
- Self-Efficacy (confidence in performing behavior)
- Specific self-efficacy: strongest predictor of behavior change (r=0.51)
- Sources: mastery experiences, vicarious learning, verbal persuasion, physiological states
- Enhancement strategies: graduated exposure, modeling, skills training
- Outcome Expectations (anticipated consequences)
- Physical outcomes: health improvements, symptom reduction
- Social outcomes: approval, support, relationship changes
- Self-evaluative outcomes: pride, satisfaction, identity alignment
- Self-Efficacy (confidence in performing behavior)
⭐ Clinical Pearl: Self-efficacy serves as the strongest predictor of behavior change success across all health behaviors, with specific self-efficacy (confidence in particular situations) showing correlation coefficients of 0.45-0.65 with actual behavior performance.
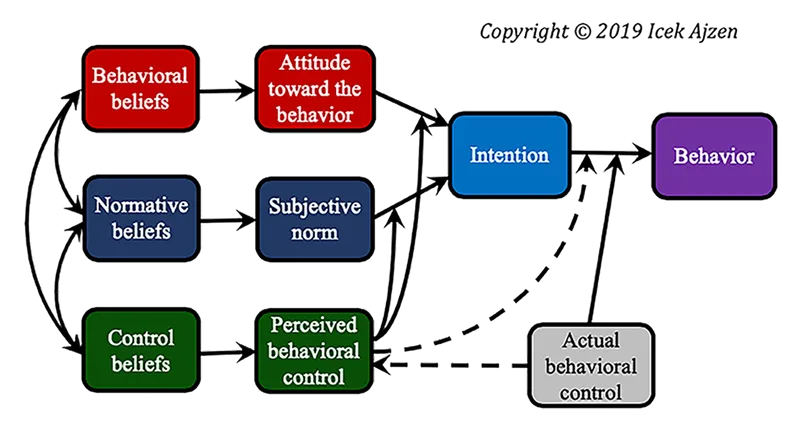
Advanced Behavior Change Integration
- Theory of Planned Behavior (TPB)
- Behavioral Intention (immediate predictor of behavior)
- Intention-behavior correlation: r=0.47 across health behaviors
- Implementation intentions: "if-then" planning increases success by 30%
- Intention stability: stronger intentions show less decay over time
- Attitude-Behavior Consistency
- Explicit attitudes: conscious evaluations (r=0.38 with behavior)
- Implicit attitudes: automatic associations (r=0.27 with behavior)
- Attitude accessibility: easily retrieved attitudes predict behavior better
- Behavioral Intention (immediate predictor of behavior)
💡 Master This: Implementation intentions ("if-then" planning) bridge the intention-action gap by creating automatic behavioral responses to environmental cues, increasing behavior change success rates by 25-30% across diverse health behaviors through pre-commitment to specific action plans.
📌 Remember: BEHAVIOR CHANGE SUCCESS - Belief in capability + Environmental support + Habit formation + Action planning + Value alignment + Intention strength + Outcome expectations + Relapse prevention + Cue management + Health motivation + Accountability systems + New identity + Goal specificity + Emotional regulation
These behavior change frameworks provide the foundation for effective patient communication strategies, as successful health behavior modification requires skillful therapeutic relationships that motivate and sustain change efforts.
🔄 Behavior Change Models — Nudging New Habits
💬 Patient Communication & Care - Healing Conversations
Patient communication represents the therapeutic foundation upon which all medical interventions rest, transforming clinical encounters from mere information exchange into healing relationships that promote adherence, reduce anxiety, and improve health outcomes. Effective communication operates as both diagnostic tool and therapeutic intervention, with research demonstrating that communication quality accounts for 15-20% of variance in patient satisfaction and 12-18% of variance in treatment adherence.

The patient-centered communication model emphasizes collaborative partnership rather than paternalistic information delivery, with studies showing that patient-centered approaches increase satisfaction by 25-35%, improve adherence by 19-28%, and reduce malpractice risk by 40-50%. This model recognizes patients as active participants in their healthcare journey, requiring clinicians to balance medical expertise with patient autonomy and preferences.
📌 Remember: THERAPEUTIC COMMUNICATION - Trust building + Honest information + Empathetic responses + Respectful interaction + Active listening + Patient autonomy + Emotional support + Understanding verification + Tailored messaging + Inclusive approach + Clear explanations + Collaborative planning + Open dialogue + Mutual respect + Meaningful connection
Core Communication Skills and Techniques
-
Active Listening Mastery
- Nonverbal attention (55% of communication impact)
- Eye contact: 60-70% of conversation time for optimal engagement
- Body positioning: open posture increases patient disclosure by 23%
- Facial expressions: congruent emotions build trust and rapport
- Verbal reflection techniques
- Paraphrasing: "What I hear you saying is..." increases understanding by 35%
- Emotional labeling: "You seem worried about..." validates patient experience
- Summarizing: periodic synthesis ensures mutual understanding
- Nonverbal attention (55% of communication impact)
-
Empathetic Response Patterns
- Cognitive empathy (understanding patient perspective)
- Perspective-taking: "Help me understand what this means to you"
- Validation: "Your concerns make complete sense"
- Normalization: "Many patients feel this way"
- Affective empathy (emotional resonance)
- Emotional matching: appropriate emotional tone for patient state
- Compassionate presence: "I can see this is really difficult"
- Support offering: "We'll work through this together"
- Cognitive empathy (understanding patient perspective)
Shared Decision-Making Framework
| Communication Element | Patient Impact | Adherence Improvement | Satisfaction Increase | Malpractice Risk Reduction |
|---|---|---|---|---|
| Active Listening | Trust ↑40% | 19% better adherence | 28% higher satisfaction | 35% risk reduction |
| Empathetic Responses | Anxiety ↓30% | 23% better adherence | 32% higher satisfaction | 42% risk reduction |
| Clear Explanations | Understanding ↑50% | 31% better adherence | 25% higher satisfaction | 28% risk reduction |
| Shared Decision-Making | Autonomy ↑45% | 27% better adherence | 38% higher satisfaction | 48% risk reduction |
| Cultural Sensitivity | Engagement ↑35% | 22% better adherence | 29% higher satisfaction | 31% risk reduction |
- Chunk and Check Method
- Deliver information in 2-3 concept chunks
- Check understanding: "What questions do you have about this?"
- Adjust complexity based on patient health literacy level
- Visual and Verbal Integration
- Written materials: improve recall by 40% when combined with verbal explanation
- Diagrams and models: increase understanding by 35% for complex conditions
- Teach-back method: "In your own words, tell me..." ensures comprehension
⭐ Clinical Pearl: The teach-back method ("In your own words, can you tell me how you'll take this medication?") improves patient understanding by 40-60% and reduces medication errors by 30%, making it the gold standard for verifying patient comprehension.
- Difficult Conversation Navigation
- Breaking Bad News Protocol (SPIKES)
- Setting: private, uninterrupted environment
- Perception: assess patient's current understanding
- Invitation: ask permission to share information
- Knowledge: deliver information clearly and compassionately
- Emotions: respond to emotional reactions empathetically
- Strategy: develop collaborative next steps
- Conflict Resolution Strategies
- Acknowledge emotions: "I can see you're frustrated"
- Find common ground: "We both want what's best for your health"
- Explore underlying concerns: "Help me understand your main worry"
- Breaking Bad News Protocol (SPIKES)
Cultural Competence and Health Equity
-
Cultural Communication Adaptations
- Language considerations (20% of US population speaks language other than English at home)
- Professional interpreters: improve outcomes by 25% compared to family interpreters
- Cultural brokers: bridge cultural gaps in health beliefs and practices
- Health literacy adaptation: adjust communication to educational and cultural background
- Cultural Health Beliefs Integration
- Traditional healing practices: respectful inquiry about complementary approaches
- Family involvement: cultural variations in decision-making authority
- Religious considerations: spiritual needs in health and illness
- Language considerations (20% of US population speaks language other than English at home)
-
Health Equity Communication
- Bias recognition and mitigation
- Implicit bias: affects clinical decisions in measurable ways
- Stereotype threat: patient awareness of potential bias affects communication
- Microaggression awareness: subtle discriminatory communications harm therapeutic relationships
- Inclusive communication practices
- Gender-inclusive language: respectful terminology for all patients
- Socioeconomic sensitivity: avoid assumptions about resources and capabilities
- Disability accommodation: communication adaptations for diverse abilities
- Bias recognition and mitigation
💡 Master This: Cultural humility involves recognizing the limits of one's cultural knowledge, maintaining openness to learning from patients about their cultural perspectives, and acknowledging power imbalances in healthcare relationships, leading to 30% better patient engagement in diverse populations.
📌 Remember: HEALING COMMUNICATION - Honest information sharing + Empathetic responses + Active listening + Language accessibility + Inclusive practices + Nonverbal awareness + Genuine concern + Cultural competence + Open dialogue + Mutual respect + Meaningful connection + Understanding verification + Navigate emotions + Involve families + Collaborative decisions + Accessible explanations + Trust building + Individualized care + Optimal outcomes + Nurturing relationships
These communication foundations integrate with broader health psychology principles to create comprehensive approaches for promoting individual and population health through evidence-based behavioral interventions and health promotion strategies.
💬 Patient Communication & Care — Healing Conversations
🎯 High‑Yield Points - ⚡ Biggest Takeaways

The biopsychosocial integration serves as health psychology's central organizing principle, with research demonstrating that psychological interventions reduce healthcare costs by 20-30%, improve treatment adherence by 25-40%, and decrease symptom severity by 15-35% across chronic medical conditions. This integration transforms traditional biomedical approaches into comprehensive care models that address the full spectrum of factors influencing health and illness.
📌 Remember: HEALTH PSYCHOLOGY MASTERY - Holistic assessment + Evidence-based interventions + Adaptive coping + Lifestyle modification + Therapeutic communication + Health behavior change + Psychological resilience + Stress management + Yielding optimal outcomes + Cultural competence + Healing relationships + Optimal integration + Lifelong wellness + Organized care + Genuine empathy + Yearning for health
Essential Clinical Applications
-
Stress-Health Pathway Mastery
- HPA axis dysfunction predicts 2.5-fold increased mortality risk
- Chronic stress (cortisol >15 μg/dL for >6 months) suppresses immune function by 30%
- Allostatic load scores >3 indicate significant physiological wear-and-tear
- Problem-focused coping shows 85% effectiveness in controllable situations
- Social support reduces stress-related mortality by 50%
-
Behavior Change Implementation
- Self-efficacy represents the strongest predictor (r=0.51) of behavior change success
- Stage-matched interventions improve outcomes by 40-60% over generic approaches
- Implementation intentions ("if-then" planning) increase success rates by 25-30%
- Relapse rates decrease from 50-80% in action stage to 20-30% after 12 months maintenance
- Health beliefs account for 30-40% of variance in health behavior adoption
Rapid Assessment Framework
| Assessment Domain | Key Indicators | Clinical Thresholds | Intervention Priorities | Success Metrics |
|---|---|---|---|---|
| Stress Level | Perceived Stress Scale | Score >20 | Stress management training | 30% cortisol reduction |
| Coping Style | Brief COPE Inventory | Avoidance >15 | Adaptive coping skills | 40% improved outcomes |
| Health Beliefs | Health Belief Model | Barriers >Benefits | Belief modification | 25% behavior change |
| Self-Efficacy | General Self-Efficacy | Score <25 | Confidence building | 50% adherence improvement |
| Communication | Patient satisfaction | Score <80% | Communication training | 35% satisfaction increase |
-
Communication Excellence Markers
- Patient-centered communication increases satisfaction by 25-35%
- Active listening improves treatment adherence by 19-28%
- Teach-back method reduces medication errors by 30%
- Empathetic responses decrease malpractice risk by 40-50%
- Cultural competence improves engagement by 30% in diverse populations
-
Integration Success Factors
- Biopsychosocial assessment improves diagnostic accuracy by 20-25%
- Collaborative care models reduce healthcare costs by 20-30%
- Psychological interventions decrease symptom severity by 15-35%
- Health psychology consultation improves treatment outcomes by 25-40%
- Integrated care teams show 60% better chronic disease management
💡 Master This: Health psychology integration transforms medical care from symptom-focused treatment to person-centered healing, addressing the psychological, behavioral, and social factors that account for 40-60% of variance in health outcomes across major medical conditions.
📌 Remember: CLINICAL EXCELLENCE - Comprehensive assessment + Lifestyle integration + Innovative interventions + Nurturing relationships + Individualized care + Cultural competence + Adaptive strategies + Lifelong learning + Evidence-based practice + Xcellent communication + Collaborative care + Empathetic responses + Leading outcomes + Lasting change + Ethical practice + Nurturing wellness + Caring presence + Effective healing
These high-yield principles provide the foundation for applying health psychology concepts across diverse clinical settings, enabling healthcare providers to address the complex interplay of psychological, behavioral, and social factors that influence health outcomes and guide comprehensive patient care approaches.
🎯 High‑Yield Points — ⚡ Biggest Takeaways
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app



















