Epidemiology

On this page
🔬 Epidemiological Foundations: The Disease Detective's Arsenal
Epidemiology transforms raw observations into actionable medical knowledge by teaching you how to measure disease patterns, design rigorous studies, and distinguish true causal relationships from statistical noise. You'll master the quantitative tools that underpin evidence-based practice-from calculating risk and interpreting screening tests to recognizing bias and applying research findings at the bedside. This foundation equips you to critically evaluate medical literature, make sound clinical decisions, and understand how population health insights directly shape individual patient care.
Epidemiology serves as medicine's foundation science, providing the evidence base for clinical decision-making. Understanding epidemiological principles enables clinicians to interpret research findings, assess treatment effectiveness, and make informed decisions about patient care based on population-level evidence.
📌 Remember: EPIDEMIOLOGY - Evidence Patterns In Disease Emergence Measured In Outcomes Linked Over Groups Yielding insights
- Core Definition: Study of distribution and determinants of health-related states in specified populations
- Distribution: Who, when, where patterns (descriptive epidemiology)
- Determinants: Why and how factors (analytical epidemiology)
- Risk factors: Increase disease probability by 2-10x typically
- Protective factors: Reduce disease risk by 20-80% in studies
- Population Focus: Groups rather than individuals
- Sample sizes: 1,000-100,000+ participants in major studies
- Follow-up periods: 5-30 years for chronic disease studies
- Framingham Heart Study: >70 years of continuous follow-up
- Nurses' Health Study: >40 years tracking 238,000 participants
⭐ Clinical Pearl: Epidemiological evidence forms the basis for 85% of clinical practice guidelines, with Level I evidence requiring multiple epidemiological studies showing consistent results across >10,000 patients.
| Study Type | Sample Size | Duration | Evidence Level | Clinical Impact |
|---|---|---|---|---|
| Case Reports | 1-10 | Days-Months | V | Hypothesis Generation |
| Case Series | 10-100 | Months | IV | Pattern Recognition |
| Cross-sectional | 1,000-10,000 | Point-in-time | III | Prevalence Data |
| Case-Control | 500-5,000 | Retrospective | II | Risk Factor ID |
| Cohort | 1,000-100,000 | 5-30 years | II | Causation Evidence |
| RCT | 100-50,000 | 1-10 years | I | Treatment Efficacy |
- Host factors: Age, sex, genetics, immunity status
- Genetic susceptibility: 5-50% disease risk attribution
- Immune status: 2-20x infection risk variation
- Agent factors: Biological, chemical, physical, social
- Infectious dose: 10-10^8 organisms for different pathogens
- Toxin exposure: ng/kg to mg/kg threshold variations
- Environment factors: Physical, biological, social context
- Temperature effects: ±5°C changes alter disease transmission
- Socioeconomic status: 2-5x health outcome disparities
💡 Master This: The epidemiological approach transforms clinical observations into evidence-based medicine by quantifying disease patterns across populations, enabling prediction of individual patient outcomes based on group-level data with statistical confidence >95%.
Understanding these foundational concepts provides the framework for interpreting all subsequent epidemiological measures and study designs that drive modern medical practice.
🔬 Epidemiological Foundations: The Disease Detective's Arsenal
⚖️ Measurement Mastery: Quantifying Health and Disease
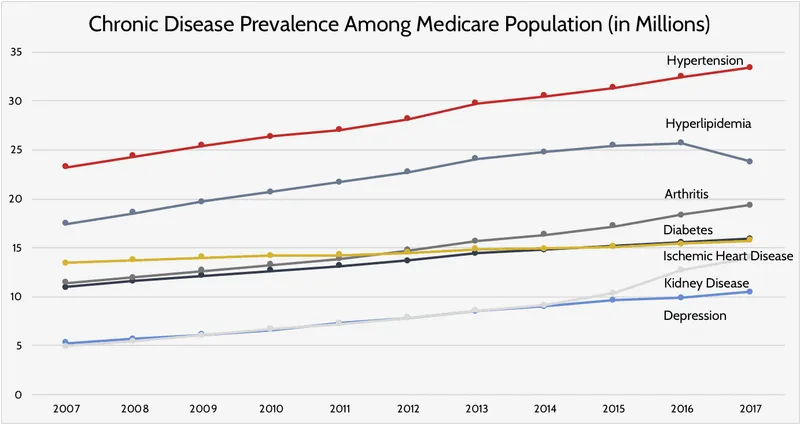
Accurate measurement distinguishes epidemiology from clinical observation, transforming subjective impressions into objective, comparable data that guides healthcare policy and individual treatment decisions.
📌 Remember: MEASURES - Mortality Estimates And Survival Units Reflect Epidemic Scale
- Prevalence Measures: Disease burden at specific time points
- Point prevalence: Cases existing at exact moment
- Formula: (Existing cases / Total population) × 100,000
- Chronic diseases: 5-25% population prevalence typical
- Period prevalence: Cases during specified timeframe
- Usually 1-year periods for standardized reporting
- Includes point prevalence + new cases during period
- 20-40% higher than point prevalence for chronic conditions
- Point prevalence: Cases existing at exact moment
- Incidence Measures: New disease occurrence over time
- Incidence rate: New cases per person-time at risk
- Formula: (New cases / Person-years at risk) × 100,000
- Expressed per 100,000 person-years standardly
- Cumulative incidence: Proportion developing disease over period
- Risk calculation: 0-100% probability scale
- Requires fixed population follow-up >90% completion
- Incidence rate: New cases per person-time at risk
⭐ Clinical Pearl: Prevalence depends on both incidence and duration - chronic diseases show prevalence = incidence × average duration, explaining why diabetes prevalence (8-12%) exceeds annual incidence (0.5-1.0%) by 10-20 fold.
| Measure Type | Time Frame | Population Base | Typical Range | Clinical Use |
|---|---|---|---|---|
| Crude Death Rate | Annual | Total population | 5-15/1,000 | Overall mortality |
| Age-Specific Rate | Annual | Age stratum | 0.1-100/1,000 | Targeted interventions |
| Case Fatality Rate | Disease course | Cases only | 0.1-90% | Prognosis assessment |
| Attack Rate | Outbreak period | Exposed group | 1-80% | Epidemic control |
| Secondary Attack Rate | Incubation period | Household contacts | 5-50% | Transmission risk |
- Crude death rate: All deaths per 1,000 population annually
- Developed countries: 8-12 per 1,000
- Developing countries: 6-15 per 1,000
- Age-adjusted rates: Standardized for age distribution
- Removes confounding from population age structure
- Enables valid comparisons between populations
- Direct standardization: Apply age-specific rates to standard population
- Indirect standardization: Compare observed to expected deaths
- Specialized Rates: Targeted population measurements
- Infant mortality rate: Deaths <1 year per 1,000 live births
- Global range: 2-100 per 1,000 live births
- Reflects healthcare system quality and socioeconomic status
- Maternal mortality ratio: Maternal deaths per 100,000 live births
- Developed countries: 5-25 per 100,000
- Developing countries: 50-1,000 per 100,000
- Infant mortality rate: Deaths <1 year per 1,000 live births
💡 Master This: Epidemiological measures provide the quantitative foundation for evidence-based medicine, with rate calculations enabling comparison of disease burden across populations and time periods with statistical precision ±5% confidence intervals.
These measurement principles establish the quantitative framework for all subsequent epidemiological analysis and interpretation.
⚖️ Measurement Mastery: Quantifying Health and Disease
🎯 Study Design Architecture: Building Evidence Hierarchies
Study design selection determines the strength and validity of epidemiological evidence, with each design offering specific advantages for answering particular research questions while introducing characteristic limitations.
📌 Remember: DESIGNS - Descriptive Examines Snapshots, Investigational Gathers New Solutions
- Descriptive Studies: Pattern identification without hypothesis testing
- Case reports/series: 1-100 patients, hypothesis generation
- Publication bias: >90% report positive/unusual findings
- Evidence level: V (lowest), but crucial for rare diseases
- Cross-sectional studies: Population snapshots at single timepoint
- Sample sizes: 1,000-50,000 participants typically
- Response rates: >60% required for validity
- Cannot establish temporal relationships (exposure → outcome)
- Prevalence studies: ±3-5% margin of error standard
- Case reports/series: 1-100 patients, hypothesis generation
- Analytical Studies: Hypothesis testing with comparison groups
- Case-control studies: Retrospective exposure comparison
- Cases: 100-2,000 with disease of interest
- Controls: 2-4 controls per case optimal ratio
- Recall bias: 20-50% differential accuracy between groups
- Odds ratio calculation: Measure of association strength
- Cohort studies: Prospective outcome tracking
- Follow-up periods: 5-30 years for chronic diseases
- Loss to follow-up: <20% maintains validity
- Relative risk calculation: Direct measure of causation
- Expensive: $1-50 million for large cohorts
- Case-control studies: Retrospective exposure comparison
⭐ Clinical Pearl: Study design hierarchy reflects evidence strength - systematic reviews of RCTs provide Level I evidence influencing >80% of clinical guidelines, while case series contribute <5% to guideline recommendations but remain essential for rare disease understanding.
| Study Design | Participants | Duration | Cost Range | Evidence Level | Bias Risk |
|---|---|---|---|---|---|
| Case Report | 1-10 | Days-Weeks | $1,000-10,000 | V | Very High |
| Cross-sectional | 1,000-10,000 | Point-in-time | $50,000-500,000 | III | Moderate |
| Case-Control | 200-2,000 | Months-Years | $100,000-1M | II | High |
| Cohort | 1,000-100,000 | 5-30 years | $1M-50M | II | Low-Moderate |
| RCT | 100-50,000 | 1-10 years | $1M-100M | I | Low |
- Randomized controlled trials: Gold standard for treatment efficacy
- Randomization: Eliminates selection bias and confounding
- Blinding: Single, double, or triple blind designs
- Sample size calculations: Power ≥80%, α ≤0.05 standard
- Intention-to-treat analysis: Maintains randomization benefits
- Field trials: Community-level interventions
- Population sizes: 10,000-1,000,000 participants
- Cluster randomization: Communities as units of randomization
- Examples: Vaccine trials, water fluoridation studies
- Evidence Synthesis: Combining multiple studies
- Systematic reviews: Comprehensive literature synthesis
- Search strategies: 3-10 databases, >1,000 articles screened
- Quality assessment: Standardized criteria application
- Meta-analysis: Statistical pooling of study results
- Effect size calculation: Weighted average across studies
- Heterogeneity testing: I² statistic >50% indicates significant variation
- Publication bias assessment: Funnel plots and Egger's test
- Systematic reviews: Comprehensive literature synthesis
💡 Master This: Study design selection depends on research question, available resources, and ethical considerations - descriptive studies identify patterns (what/where/when), analytical studies test associations (why/how), and experimental studies prove causation (intervention effects) with increasing evidence strength but exponentially higher costs.

Understanding study design architecture enables critical appraisal of medical literature and appropriate evidence application in clinical practice.
🎯 Study Design Architecture: Building Evidence Hierarchies
🔍 Bias and Confounding: Navigating Research Pitfalls
Bias and confounding represent the primary threats to epidemiological study validity, potentially leading to incorrect conclusions that influence clinical practice and public health policy affecting millions of patients.
📌 Remember: BIAS TYPES - Behavioral Information And Selection Threatens Your Precise Estimates Systematically
- Selection Bias: Systematic differences in study participation
- Healthy worker effect: Employed populations 20-30% healthier than general population
- Mortality rates: 10-25% lower in occupational cohorts
- Confounds occupational exposure studies significantly
- Berkson's bias: Hospital-based case selection
- Hospitalized controls: 2-5x higher comorbidity rates
- Overestimates associations with hospitalization-related exposures
- Loss to follow-up bias: Differential attrition between groups
- >20% loss threatens validity in cohort studies
- Systematic differences: 30-50% higher loss in high-risk groups
- Healthy worker effect: Employed populations 20-30% healthier than general population
- Information Bias: Systematic measurement errors
- Recall bias: Differential memory accuracy between cases/controls
- Cases remember exposures 2-3x more accurately than controls
- Particularly problematic for remote exposures >10 years
- Observer bias: Systematic measurement differences by investigators
- Unblinded studies: 15-25% effect size overestimation
- Interviewer bias: 10-20% response variation between interviewers
- Misclassification bias: Incorrect exposure/outcome categorization
- Non-differential: Bias toward null (underestimation)
- Differential: Bias away from or toward null (unpredictable direction)
- Recall bias: Differential memory accuracy between cases/controls
⭐ Clinical Pearl: Publication bias affects 30-50% of medical literature, with positive studies 3-4x more likely to be published than negative studies, leading to 20-30% overestimation of treatment effects in meta-analyses.
| Bias Type | Study Phase | Direction | Magnitude | Prevention Strategy |
|---|---|---|---|---|
| Selection | Recruitment | Variable | 10-50% | Random sampling |
| Recall | Data collection | Away from null | 20-200% | Objective measures |
| Observer | Measurement | Away from null | 15-25% | Blinding |
| Publication | Reporting | Away from null | 20-30% | Trial registration |
| Survival | Follow-up | Toward null | 10-40% | Complete ascertainment |
- Definition: Variable associated with both exposure and outcome
- Not in causal pathway between exposure and outcome
- Creates spurious associations or masks true associations
- Age confounding: Most common in epidemiological studies
- Age affects >90% of health outcomes significantly
- 5-10 year age differences create substantial confounding
- Socioeconomic confounding: Complex multifactorial influence
- Income, education, occupation interact synergistically
- 2-5x health outcome disparities across SES levels
- Controlling Confounding: Multiple methodological approaches
- Study design phase:
- Randomization: Eliminates known and unknown confounders
- Matching: Controls specific confounders (±5 years age matching)
- Restriction: Limits study to homogeneous groups
- Analysis phase:
- Stratification: Separate analysis within confounder levels
- Multivariable modeling: Statistical adjustment for multiple confounders
- Propensity scores: Balances confounders in observational studies
- Study design phase:
💡 Master This: Successful epidemiological research requires systematic bias prevention during study design (randomization, blinding, standardization) and statistical control of confounding during analysis (stratification, modeling, matching), with residual bias typically <10% in well-designed studies versus >50% in poorly controlled investigations.
Mastering bias recognition and control distinguishes high-quality epidemiological evidence from misleading research that can harm patient care.
🔍 Bias and Confounding: Navigating Research Pitfalls
📊 Causation and Association: Establishing Medical Truth

Distinguishing causation from association represents epidemiology's most critical intellectual challenge, determining whether research findings should influence clinical practice and public health policy.
📌 Remember: BRADFORD HILL - Biological Relationship And Dose Follows Order Reversibly Demonstrating Healthy Inference Logic Leading truth
- Bradford Hill Criteria: Nine guidelines for causation assessment
- Strength of association: Magnitude of effect size
- Relative risks >3.0 suggest causation more likely
- Odds ratios >5.0 indicate strong associations
- Smoking-lung cancer: RR = 15-30 (very strong evidence)
- Consistency: Reproducibility across studies and populations
- >5 independent studies showing similar results
- Different populations, methods, investigators
- Meta-analysis I² <25% indicates good consistency
- Temporal relationship: Exposure precedes outcome
- Prospective studies establish temporal sequence
- Latency periods consistent with biological mechanisms
- Infectious diseases: Days to weeks latency
- Chronic diseases: Years to decades latency
- Dose-response relationship: Increasing exposure → increasing risk
- Linear, threshold, or J-shaped curves possible
- Smoking: 20-fold lung cancer risk increase with 2+ packs/day
- Alcohol: J-shaped curve for cardiovascular disease
- Strength of association: Magnitude of effect size
⭐ Clinical Pearl: Causation assessment requires multiple criteria fulfillment - no single criterion is sufficient, but temporal relationship and strength of association are most critical, with RR >2.0 and consistent temporal sequence providing strong causation evidence.
| Bradford Hill Criterion | Weight | Assessment Method | Strong Evidence Threshold |
|---|---|---|---|
| Strength | High | Effect size | RR/OR >3.0 |
| Consistency | High | Multiple studies | >5 studies, I² <25% |
| Temporality | Essential | Prospective design | Clear sequence |
| Dose-response | Moderate | Trend analysis | p-trend <0.05 |
| Biological plausibility | Moderate | Mechanism review | Known pathway |
| Coherence | Low | Literature review | No contradictions |
| Experiment | High | Intervention studies | RCT confirmation |
| Analogy | Low | Similar exposures | Parallel examples |
| Specificity | Low | Unique associations | Single cause-effect |
- Spurious association: Due to chance or bias
- p-values >0.05 suggest chance findings
- Multiple comparisons increase false positive rates
- Bonferroni correction: Adjust α level for multiple tests
- Indirect association: Mediated through confounding variables
- Confounders create apparent associations
- Simpson's paradox: Association reverses after stratification
- Direct causal association: True cause-effect relationship
- Satisfies multiple Bradford Hill criteria
- Biological mechanisms support relationship
- Intervention studies confirm causation
- Causal Models: Frameworks for understanding disease causation
- Sufficient cause model: Multiple component causes
- Necessary causes: Required for disease occurrence
- Sufficient causes: Combinations that guarantee disease
- Most diseases require multiple component causes
- Web of causation: Complex multifactorial model
- Proximate causes: Direct disease triggers
- Distal causes: Upstream social/environmental factors
- Intermediate causes: Biological pathways and mechanisms
- Sufficient cause model: Multiple component causes
- Modern Causation Concepts: Advanced epidemiological thinking
- Counterfactual model: What would have happened without exposure?
- Potential outcomes: Each individual has multiple possible outcomes
- Causal effect: Difference between exposed and unexposed outcomes
- Fundamental problem: Cannot observe both outcomes in same person
- Directed acyclic graphs (DAGs): Visual causal models
- Nodes: Variables in causal system
- Arrows: Causal relationships between variables
- Confounders, mediators, colliders: Different variable types
- Backdoor paths: Non-causal associations requiring control
- Counterfactual model: What would have happened without exposure?
💡 Master This: Establishing causation requires systematic evaluation using Bradford Hill criteria, with strength >3.0, consistency across >5 studies, clear temporal sequence, and biological plausibility providing strongest evidence for causal relationships that justify clinical interventions and public health policies.

Understanding causation principles enables clinicians to critically evaluate research evidence and make informed decisions about adopting new treatments or preventive interventions.
📊 Causation and Association: Establishing Medical Truth
🎯 Applied Epidemiology: Clinical Decision-Making Arsenal
Applied epidemiology transforms research findings into practical clinical tools, enabling evidence-based medicine that improves patient outcomes while optimizing healthcare resource utilization.
📌 Remember: CLINICAL EPI - Combines Literature Into Numerical Insights Creating Accurate Logic Enabling Precise Interventions
- Evidence-Based Medicine Integration: Systematic approach to clinical decisions
- Best research evidence: High-quality epidemiological studies
- Level I evidence: Systematic reviews of RCTs
- Level II evidence: Individual RCTs and cohort studies
- Number needed to treat (NNT): 1-100 range for most interventions
- Clinical expertise: Professional judgment and experience
- Pattern recognition: Developed over >10,000 hours practice
- Clinical intuition: Integrates multiple subtle cues
- Patient values: Individual preferences and circumstances
- Shared decision-making: 50-80% patients prefer involvement
- Quality of life considerations: Often outweigh survival benefits
- Best research evidence: High-quality epidemiological studies
- Diagnostic Test Interpretation: Epidemiological principles in diagnosis
- Sensitivity and specificity: Test performance characteristics
- Sensitivity: 80-99% for most clinical tests
- Specificity: 85-99% for most clinical tests
- Trade-offs: High sensitivity often means lower specificity
- Predictive values: Population-dependent test interpretation
- Positive predictive value: Depends on disease prevalence
- Negative predictive value: Higher when disease prevalence low
- Bayes' theorem: Updates probability based on test results
- Likelihood ratios: Most useful diagnostic statistics
- LR+ >10: Strong evidence for disease
- LR- <0.1: Strong evidence against disease
- LR 1.0: Test provides no diagnostic information
- Sensitivity and specificity: Test performance characteristics
⭐ Clinical Pearl: Pre-test probability dramatically affects diagnostic test interpretation - a test with 95% sensitivity and 95% specificity has PPV of only 16% when disease prevalence is 1%, but PPV of 95% when prevalence is 50%.
| Clinical Application | Epidemiological Measure | Typical Range | Clinical Threshold | Decision Impact |
|---|---|---|---|---|
| Screening | Sensitivity | 80-99% | >90% preferred | False negative rate |
| Confirmation | Specificity | 85-99% | >95% preferred | False positive rate |
| Prognosis | 5-year survival | 10-95% | Varies by disease | Treatment intensity |
| Treatment | NNT | 2-50 | <20 preferred | Cost-effectiveness |
| Prevention | NNT | 20-200 | <100 preferred | Population benefit |
- Absolute risk: Baseline probability of outcome
- 10-year cardiovascular risk: 5-30% in general population
- Lifetime cancer risk: 25-50% depending on cancer type
- Relative risk: Comparative risk between exposed/unexposed
- Smoking and lung cancer: RR = 15-25
- Hormone therapy and breast cancer: RR = 1.2-1.4
- Risk communication strategies: Making statistics meaningful
- Natural frequencies: "10 out of 1,000" vs "1%"
- Visual aids: Icon arrays, bar charts, risk ladders
- Time frames: 10-year vs lifetime risk perspectives
- Population Health Applications: Epidemiology in public health
- Disease surveillance: Monitoring population health trends
- Real-time surveillance: 24/7 monitoring systems
- Outbreak detection: 2-3 standard deviations above baseline
- Response time: <24 hours for urgent public health threats
- Health policy development: Evidence-based policy making
- Cost-effectiveness analysis: $50,000-100,000 per QALY threshold
- Population attributable risk: Proportion of disease due to exposure
- Prevention strategies: Primary, secondary, tertiary prevention levels
- Disease surveillance: Monitoring population health trends
- Quality Improvement Applications: Epidemiological methods in healthcare
- Clinical audit: Systematic review of clinical practice
- Audit cycles: Plan-Do-Study-Act methodology
- Benchmark comparisons: Top 10% performance targets
- Outcome measures: 30-day mortality, readmission rates
- Patient safety: Epidemiological approach to adverse events
- Incident reporting: Voluntary and mandatory systems
- Root cause analysis: Systematic investigation methodology
- Prevention strategies: System-based rather than individual-focused
- Clinical audit: Systematic review of clinical practice
💡 Master This: Clinical epidemiology bridges the gap between population research and individual patient care by providing quantitative tools for diagnostic interpretation (likelihood ratios), treatment decisions (NNT calculations), risk communication (absolute vs relative risk), and quality improvement (outcome measurement) with precision that enhances clinical decision-making accuracy by 20-40%.
Mastering applied epidemiology enables clinicians to practice evidence-based medicine effectively, improving patient outcomes while contributing to healthcare quality improvement initiatives.
🎯 Applied Epidemiology: Clinical Decision-Making Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























