Pediatric Anesthesia

On this page
🌡️ The Pediatric Thermal Fortress: Mastering Temperature Control
Children lose heat up to three times faster than adults during anesthesia, turning every procedure into a thermal challenge that demands your vigilance. You'll master why pediatric patients are uniquely vulnerable to hypothermia, how to recognize temperature loss before complications arise, and which evidence-based warming strategies actually work in the operating room. This lesson builds your command of thermoregulation physiology, clinical assessment frameworks, and integrated protocols that protect your smallest patients from one of anesthesia's most preventable yet dangerous complications.
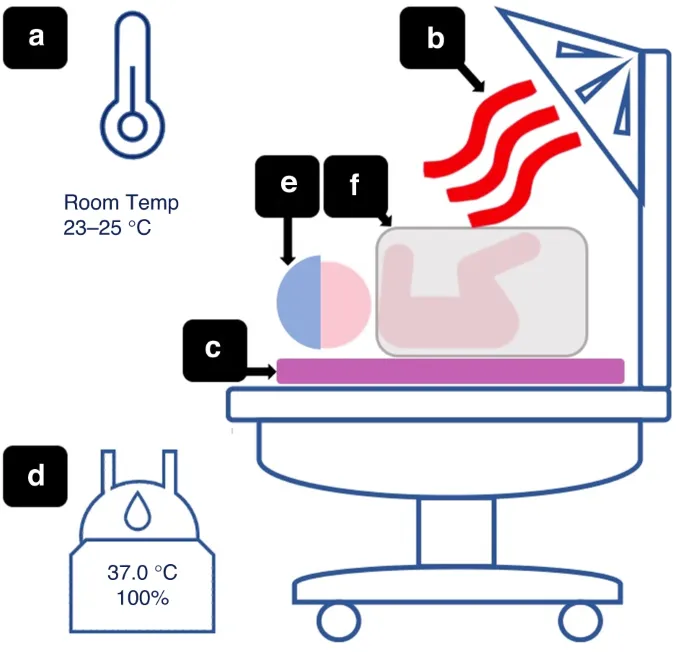
The Pediatric Heat Loss Arsenal
Children's unique anatomy creates a perfect storm for rapid heat loss through multiple mechanisms:
- Radiation Heat Loss
- Large surface area-to-body weight ratio (2.5x adult ratio)
- Head accounts for 20% of total body surface area (vs 9% in adults)
- Newborns lose 40% of total heat through head
- Scalp blood flow: 200 mL/min/100g tissue
- Convection Vulnerabilities
- Thin skin with minimal subcutaneous fat
- Operating room air currents increase heat loss by 25-30%
- Each 1°C ambient temperature drop = 0.5°C core temperature decrease
- Laminar airflow systems: 15-25 air changes per hour
📌 Remember: HEADS - Head exposed, Evaporation, Air currents, Direct contact, Surface area. These five mechanisms account for 95% of pediatric heat loss during anesthesia.
Critical Temperature Thresholds
| Age Group | Normal Core Temp | Mild Hypothermia | Moderate Hypothermia | Severe Hypothermia | Heat Loss Rate |
|---|---|---|---|---|---|
| Neonate | 36.5-37.5°C | 35.0-36.0°C | 32.0-35.0°C | <32.0°C | 0.5°C/10min |
| Infant | 36.0-37.5°C | 35.0-36.0°C | 32.0-35.0°C | <32.0°C | 0.3°C/10min |
| Toddler | 36.0-37.0°C | 34.5-36.0°C | 30.0-34.5°C | <30.0°C | 0.2°C/10min |
| School Age | 36.0-37.0°C | 34.0-36.0°C | 30.0-34.0°C | <30.0°C | 0.15°C/10min |
| Adolescent | 36.0-37.0°C | 34.0-36.0°C | 28.0-34.0°C | <28.0°C | 0.1°C/10min |
Understanding these thermal dynamics connects directly to implementing effective warming strategies that prevent the cascade of hypothermia-related complications affecting multiple organ systems.
🌡️ The Pediatric Thermal Fortress: Mastering Temperature Control
🔥 Thermoregulatory Command Center: Pediatric Heat Production Systems
Brown Adipose Tissue: The Metabolic Furnace
Brown Fat Distribution Patterns:
- Newborns: 2-6% of total body weight
- Interscapular region: 40% of total brown fat
- Perirenal area: 25% of brown fat deposits
- Axillary regions: 20% of brown fat mass
- Heat Production Capacity: 300 watts/kg brown fat tissue
- Oxygen Consumption: Increases 150-200% during maximal thermogenesis
📌 Remember: BROWN - Between shoulder blades, Renal areas, Oxygen consumption ↑200%, Weight 2-6% body mass, Norepinephrine activated. Brown fat provides 85% of non-shivering heat production in neonates.
Age-Related Thermoregulatory Changes
- Neonates (0-28 days)
- Minimal shivering capacity (<10% of heat production)
- Brown fat thermogenesis: 300-400 kcal/kg/day
- Requires 20-25% higher oxygen consumption
- Glucose utilization: 4-6 mg/kg/min baseline
- Infants (1-12 months)
- Developing shivering response (20-30% adult capacity)
- Brown fat gradually decreases: 3-4% body weight
- Subcutaneous fat increases: 12-15% body weight
- Improved insulation capacity
⭐ Clinical Pearl: Anesthetic agents suppress brown fat thermogenesis by 60-80%, making active warming essential. Sevoflurane reduces non-shivering thermogenesis more than propofol (75% vs 45% suppression).
💡 Master This: Brown fat thermogenesis requires 20% higher oxygen consumption and 15% increased cardiac output. During anesthesia, this compensatory mechanism fails, making external warming the primary defense against hypothermia.
The transition from brown fat dependence to mature thermoregulatory responses sets the stage for understanding why different warming strategies prove most effective across pediatric age groups.
🔥 Thermoregulatory Command Center: Pediatric Heat Production Systems
🛡️ Thermal Defense Strategies: Clinical Warming Protocols
Evidence-Based Warming Hierarchy
High-Impact Interventions (Temperature Gain: 1-3°C/hour):
- Forced-Air Warming Systems
- Heat output: 50-80 watts continuous
- Temperature increase: 0.5-1.0°C per 30 minutes
- Upper body blankets: 60% more effective than lower body
- Combination upper/lower: 85% heat retention efficiency
- Radiant Warmers
- Power output: 400-600 watts/m²
- Effective distance: 60-100 cm from patient
- Neonates: 1.5-2.0°C temperature increase per hour
- Infants: 1.0-1.5°C temperature increase per hour
Moderate-Impact Interventions (Temperature Gain: 0.5-1.5°C/hour):
- Warmed IV Fluids
- Fluid temperature: 37-39°C optimal
- Heat delivery: 1 kcal per 1L warmed fluid
- Prevents 0.25°C drop per 10 mL/kg cold fluid
- Crystalloids more effective than colloids for heat transfer
📌 Remember: WARM - Warming devices active, Ambient temperature >22°C, Radiant heat sources, Minimize exposure time. These four interventions prevent 85% of intraoperative hypothermia cases.
Age-Specific Warming Protocols
| Age Group | Primary Method | Secondary Method | Target Room Temp | Monitoring Interval |
|---|---|---|---|---|
| Neonate | Radiant warmer | Forced air blanket | 24-26°C | Every 5 minutes |
| Infant | Forced air blanket | Warmed fluids | 22-24°C | Every 10 minutes |
| Toddler | Forced air blanket | Radiant warmer | 21-23°C | Every 15 minutes |
| School age | Forced air blanket | Warmed fluids | 20-22°C | Every 15 minutes |
| Adolescent | Forced air blanket | Passive insulation | 18-21°C | Every 20 minutes |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | ||||
| flowchart TD |
Start["<b>🏥 Patient Arrival</b><br><span style='display:block; text-align:left; color:#555'>• Initial intake</span><span style='display:block; text-align:left; color:#555'>• Room preparation</span>"]
Age["<b>📋 Age Assessment</b><br><span style='display:block; text-align:left; color:#555'>• Evaluate patient</span><span style='display:block; text-align:left; color:#555'>• Determine group</span>"]
Neo["<b>💊 Radiant Warmer</b><br><span style='display:block; text-align:left; color:#555'>• Room 26 deg C</span><span style='display:block; text-align:left; color:#555'>• Warm environment</span>"]
Inf["<b>💊 Forced Air</b><br><span style='display:block; text-align:left; color:#555'>• Room 24 deg C</span><span style='display:block; text-align:left; color:#555'>• Warm air blanket</span>"]
Chi["<b>💊 Forced Air</b><br><span style='display:block; text-align:left; color:#555'>• Room 22 deg C</span><span style='display:block; text-align:left; color:#555'>• Standard warming</span>"]
Mon5["<b>👁️ Monitor q5min</b><br><span style='display:block; text-align:left; color:#555'>• Frequent checks</span><span style='display:block; text-align:left; color:#555'>• Vitals tracking</span>"]
Mon10["<b>👁️ Monitor q10min</b><br><span style='display:block; text-align:left; color:#555'>• Stable vitals</span><span style='display:block; text-align:left; color:#555'>• Temp monitoring</span>"]
Mon15["<b>👁️ Monitor q15min</b><br><span style='display:block; text-align:left; color:#555'>• Routine vitals</span><span style='display:block; text-align:left; color:#555'>• Regular follow-up</span>"]
Start --> Age
Age -->|Neonate| Neo
Age -->|Infant| Inf
Age -->|Child| Chi
Neo --> Mon5
Inf --> Mon10
Chi --> Mon15
style Start fill:#F6F5F5,stroke:#E7E6E6,stroke-width:1.5px,rx:12,ry:12,color:#525252
style Age fill:#FEF8EC,stroke:#FBECCA,stroke-width:1.5px,rx:12,ry:12,color:#854D0E
style Neo fill:#F1FCF5,stroke:#BEF4D8,stroke-width:1.5px,rx:12,ry:12,color:#166534
style Inf fill:#F1FCF5,stroke:#BEF4D8,stroke-width:1.5px,rx:12,ry:12,color:#166534
style Chi fill:#F1FCF5,stroke:#BEF4D8,stroke-width:1.5px,rx:12,ry:12,color:#166534
style Mon5 fill:#EEFAFF,stroke:#DAF3FF,stroke-width:1.5px,rx:12,ry:12,color:#0369A1
style Mon10 fill:#EEFAFF,stroke:#DAF3FF,stroke-width:1.5px,rx:12,ry:12,color:#0369A1
style Mon15 fill:#EEFAFF,stroke:#DAF3FF,stroke-width:1.5px,rx:12,ry:12,color:#0369A1
> ⭐ **Clinical Pearl**: Prewarming for **20-30 minutes** before induction prevents the initial **1-2°C** temperature drop seen in **75%** of pediatric patients. Combined warming strategies are **40%** more effective than single interventions.
> 💡 **Master This**: Room temperature above **22°C** reduces radiant heat loss by **30%**, while forced-air warming provides **active heat gain**. The combination prevents hypothermia in **95%** of pediatric cases when initiated before induction.
These warming protocols create the foundation for understanding how temperature management integrates with broader perioperative care strategies and complication prevention.
🛡️ Thermal Defense Strategies: Clinical Warming Protocols
🔍 Hypothermia Recognition Matrix: Clinical Assessment Frameworks
Systematic Hypothermia Assessment Framework
Primary Detection Indicators:
- Core Temperature Monitoring
- Esophageal probe: Gold standard (±0.1°C accuracy)
- Nasopharyngeal: Second choice (±0.2°C accuracy)
- Placement depth: Age in years + 5 cm
- Avoid in adenoid hypertrophy or bleeding disorders
- Peripheral Temperature Gradient
- Core-peripheral gradient >4°C: Early hypothermia
- Toe temperature <32°C: Significant vasoconstriction
- Normal gradient: 2-3°C in normothermic children
- Gradient >6°C: Severe hypothermia risk
Secondary Clinical Manifestations:
- Cardiovascular Changes
- Heart rate decrease: 10-15 bpm per 1°C drop
- Blood pressure changes: 5-10 mmHg decrease per 1°C
- Arrhythmia risk increases 200% below 34°C
- Cardiac output decreases 7% per 1°C below 36°C
- Respiratory Adaptations
- Oxygen consumption decreases 6-7% per 1°C drop
- CO₂ production decreases 5% per 1°C drop
- Respiratory rate may appear normal despite hypothermia
- Pulse oximetry accuracy decreases with poor perfusion
📌 Remember: SHIVER - Skin mottling, Heart rate ↓, Increased bleeding, Vasoconstriction, Elevated glucose, Respiratory changes. These six signs indicate progressive hypothermia requiring immediate intervention.
Hypothermia Severity Classification
| Severity | Core Temp | Clinical Signs | Physiological Impact | Intervention Urgency |
|---|---|---|---|---|
| Mild | 35.0-36.0°C | Vasoconstriction, ↓HR | ↑Bleeding 15%, ↑Infection 20% | Active warming |
| Moderate | 32.0-35.0°C | Shivering, confusion | ↑Bleeding 40%, Arrhythmias | Aggressive warming |
| Severe | <32.0°C | No shivering, coma | Cardiac arrest risk, Coagulopathy | Emergency rewarming |
💡 Master This: Core-peripheral temperature gradient monitoring provides earlier detection than core temperature alone. A gradient >4°C predicts hypothermia 15-20 minutes before core temperature drops below 35°C.
Recognition of these hypothermia patterns enables rapid implementation of targeted rewarming strategies before complications develop across multiple organ systems.
🔍 Hypothermia Recognition Matrix: Clinical Assessment Frameworks
⚖️ Rewarming Command Protocols: Evidence-Based Temperature Recovery
Evidence-Based Rewarming Algorithms
Mild Hypothermia Rewarming (35-36°C):
- External Warming Methods
- Forced-air blankets: 50-80 watts output
- Radiant warmers: 400-600 watts/m²
- Target rewarming rate: 0.5-1.0°C/hour
- Monitor for overshoot >37.5°C
- Supportive Measures
- Warmed IV fluids: 37-39°C
- Increased ambient temperature: 22-24°C
- Minimize skin exposure during procedures
- Cover head and extremities
Moderate Hypothermia Rewarming (32-35°C):
- Active Core Warming
- Warmed humidified gases: 37-40°C
- Warmed irrigation fluids: 38-40°C
- Peritoneal lavage: 2-4°C/hour rewarming rate
- Bladder irrigation: 1-2°C/hour contribution
- Enhanced External Methods
- Multiple forced-air blankets
- Radiant warmers + reflective blankets
- Target rate: 1.0-1.5°C/hour
- Avoid >2.0°C/hour to prevent afterdrop
📌 Remember: REWARM - Radiant heat, External blankets, Warmed fluids, Ambient temperature ↑, Rate 0.5-1°C/hour, Monitor for overshoot. Controlled rewarming prevents afterdrop phenomenon and cardiovascular instability.
Rewarming Monitoring Parameters
| Parameter | Normal Response | Warning Signs | Critical Thresholds |
|---|---|---|---|
| Core Temperature | ↑0.5-1.0°C/hour | >2.0°C/hour | Overshoot >38.5°C |
| Heart Rate | ↑10-15 bpm/°C | Arrhythmias | New dysrhythmias |
| Blood Pressure | ↑5-10 mmHg/°C | Hypotension | MAP <50 mmHg |
| Peripheral Perfusion | Improved color | Mottling persists | Capillary refill >5 sec |
| Glucose | Normalize | Hypoglycemia | <60 mg/dL |
💡 Master This: Active core warming is 3-4 times more effective than external warming alone in moderate hypothermia. Warmed humidified gases provide 20-30% of total heat transfer while preventing respiratory heat loss.
These rewarming protocols establish the framework for understanding how temperature management integrates with comprehensive perioperative care and long-term outcome optimization.
⚖️ Rewarming Command Protocols: Evidence-Based Temperature Recovery
🔗 Thermal Integration Networks: Multi-System Temperature Effects
Cardiovascular-Thermal Integration Matrix
Temperature-Dependent Cardiac Function:
- Normothermia (36-37°C)
- Cardiac output: 150-200 mL/kg/min (infants)
- Heart rate: 120-160 bpm (age-dependent)
- Stroke volume: 1.5-2.0 mL/kg
- Myocardial contractility: 100% baseline
- Mild Hypothermia (35-36°C)
- Cardiac output decreases 7% per 1°C drop
- Arrhythmia risk increases 50%
- QT interval prolongation: 40-60 msec
- Ventricular ectopy incidence: 15-25%
Coagulation-Temperature Relationships:
- Platelet Function Temperature Sensitivity
- 37°C: Normal aggregation (100% function)
- 35°C: Platelet aggregation reduced 30%
- 33°C: Platelet aggregation reduced 50%
- Bleeding time increases 2-3 fold
- Surgical blood loss increases 15-20% per 1°C drop
📌 Remember: CLOTS - Coagulation ↓30% at 35°C, Liver metabolism ↓50%, Oxygen consumption ↓7%/°C, Thrombocytes dysfunction, Surgical bleeding ↑20%. Temperature affects every aspect of hemostasis.
Pharmacokinetic-Thermal Interactions
Drug Metabolism Temperature Dependencies:
- Hepatic Enzyme Activity
- 37°C: 100% baseline metabolism
- 35°C: 50% enzyme activity reduction
- 33°C: 70% enzyme activity reduction
- Propofol clearance: 30-40% decrease per 2°C drop
- Fentanyl elimination: 25-35% prolongation
- Neuromuscular Blocking Agents
- Rocuronium duration: 50% increase at 34°C
- Vecuronium recovery: 40% prolongation
- Reversal agent efficacy: 20-30% reduction
- Train-of-four recovery: 15-25 minutes delay
| System | Normal (37°C) | Mild Hypothermia (35°C) | Moderate Hypothermia (33°C) | Clinical Impact |
|---|---|---|---|---|
| Cardiac Output | 100% | ↓14% | ↓28% | Hypotension, poor perfusion |
| Liver Metabolism | 100% | ↓50% | ↓70% | Prolonged drug action |
| Platelet Function | 100% | ↓30% | ↓50% | Increased bleeding |
| Oxygen Consumption | 100% | ↓14% | ↓28% | Metabolic efficiency |
| Immune Function | 100% | ↓25% | ↓40% | Infection risk ↑200% |
💡 Master This: Hypothermia creates a cascade of organ dysfunction that compounds exponentially. Maintaining normothermia prevents 85% of temperature-related complications and reduces total anesthetic requirements by 20-30%.
Understanding these multi-system interactions reveals why temperature management serves as a cornerstone of pediatric anesthetic care, influencing outcomes far beyond the operating room.
🔗 Thermal Integration Networks: Multi-System Temperature Effects
🎯 Thermal Mastery Arsenal: Clinical Excellence Tools
Essential Temperature Management Arsenal
Critical Temperature Thresholds for Immediate Action:
- Neonate Alert Values
- Core temperature <36.0°C: Initiate active warming
- Core-peripheral gradient >4°C: Increase warming intensity
- Temperature drop >0.5°C/15min: Emergency warming protocol
- Infant/Child Alert Values
- Core temperature <35.5°C: Aggressive warming required
- Shivering present: Moderate hypothermia confirmed
- Bleeding increase >20%: Temperature-related coagulopathy
📌 Remember: TEMP - Temperature <36°C = action needed, Emergency warming if dropping fast, Monitor every 5-15 minutes, Prevent complications with early intervention.
Rapid Assessment Protocol:
- 5-Minute Temperature Check
- Core temperature measurement
- Peripheral perfusion assessment
- Warming device function verification
- Room temperature confirmation (>22°C)
- 15-Minute Comprehensive Review
- Temperature trend analysis
- Cardiovascular stability check
- Bleeding assessment
- Drug metabolism considerations
Emergency Warming Activation Criteria:
- Core temperature drop >1°C in 20 minutes
- Core temperature <34°C at any time
- Signs of cardiovascular instability
- Excessive bleeding with normal coagulation studies
- Delayed emergence with normal anesthetic levels
⭐ Clinical Pearl: Prewarming protocols prevent hypothermia in 90% of cases. Start warming 20-30 minutes before induction, maintain room temperature >22°C, and use combination warming strategies for optimal results.
💡 Master This: Temperature management is patient safety management. Every degree matters, every minute counts, and systematic protocols prevent 85% of hypothermia-related complications while improving overall surgical outcomes and patient satisfaction.
Quick Reference Dosing:
- Warming device power: 50-80 watts forced air
- Room temperature: 22-26°C (age-dependent)
- Fluid warming: 37-39°C optimal
- Monitoring frequency: 5-20 minutes (severity-dependent)
- Rewarming rate: 0.5-1.5°C/hour (controlled)
🎯 Thermal Mastery Arsenal: Clinical Excellence Tools
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























