Back
Dual Coding for Medical Students: How to Combine Text and Diagrams for Better Recall
Learn how dual coding theory helps medical students combine text and diagrams for stronger recall. Practical framework for converting dense notes into visual schemas that work under exam pressure.

Dual Coding for Medical Students: How to Combine Text and Diagrams for Better Recall
You probably have 3,000 pages of medical textbooks staring at you right now. Dense paragraphs explaining pathophysiology, endless lists of drug interactions, and complex anatomical relationships that somehow need to stick in your brain for the next 40 years.
Heres the problem: most medical students study like theyre cramming for a literature exam. Pure text. Highlighting everything. Reading the same paragraph five times hoping it finally clicks.
But medical knowledge isnt just words on a page. Its spatial relationships, cascading pathways, and interconnected systems. When you study cardiology by memorizing paragraphs about "decreased preload leading to reduced stroke volume," you miss the visual logic that makes it obvious.
The solution? Dual coding. Not the productivity hack version you see on study blogs, but the specific technique that works for medical concepts where understanding the mechanism matters more than memorizing facts.
This is how you pair text with diagrams to build recall pathways that actually work under exam pressure.
What Dual Coding Means for Medical Students
Dual coding theory says your brain processes information through two connected channels: verbal (words, definitions, lists) and visual (diagrams, spatial relationships, mental images). When you encode the same concept in both channels, you create multiple retrieval pathways.
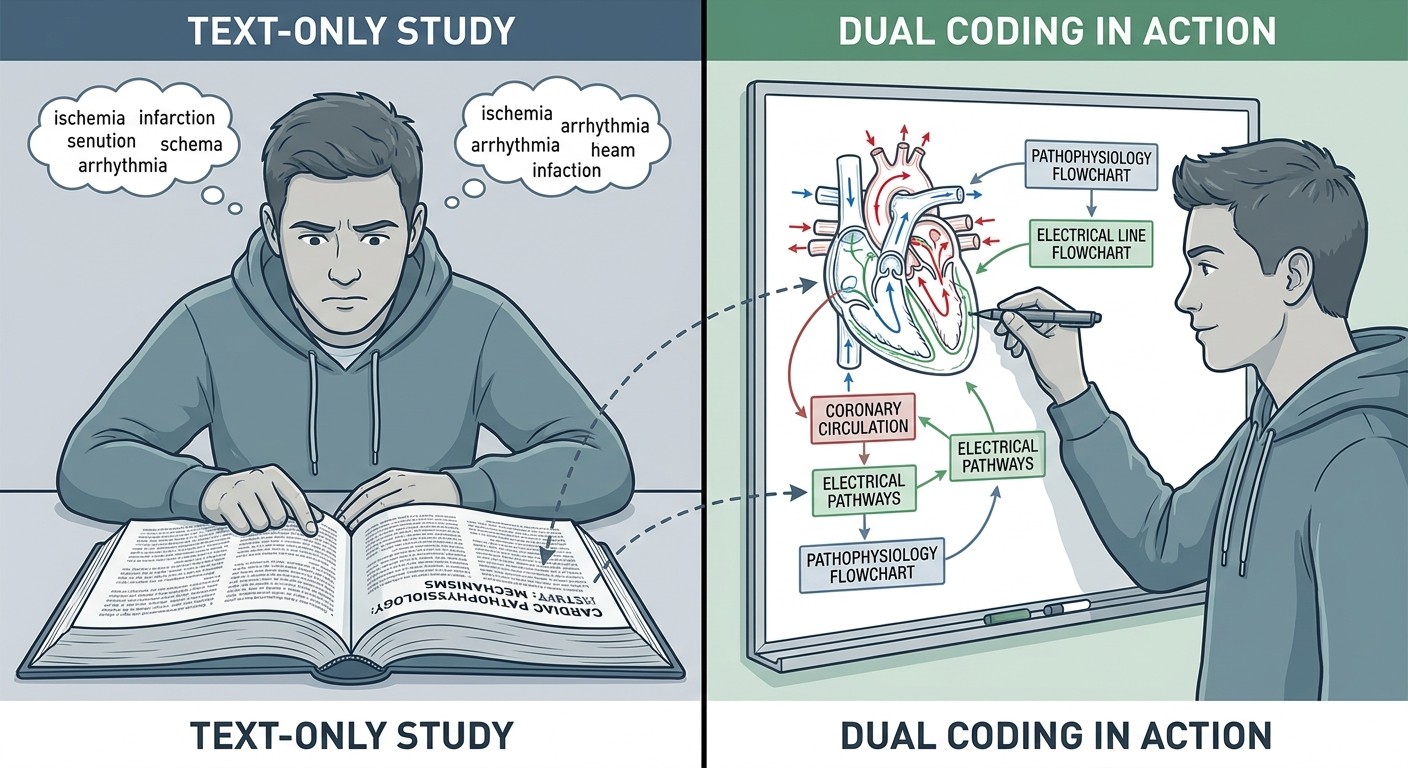
Think about learning the cardiac cycle. Reading "isovolumetric contraction occurs when ventricular pressure exceeds atrial pressure but remains below aortic pressure" gives you one retrieval path. Drawing the pressure-volume loop with labeled phases gives you another. Learning both creates cross-connections that strengthen recall.
But heres what makes medical dual coding different from generic visual learning: the diagrams arent decorations. Theyre functional representations of mechanisms you need to understand, not just remember.
When you see a patient with chest pain, you dont recall a paragraph about "typical angina presentation." You reconstruct the coronary circulation diagram, identify the likely vessel, and predict the EKG changes. The visual pathway guides clinical reasoning.
The Medical Student's Dual Coding Framework
Not every medical concept needs a diagram. Some information works better as pure text. Heres when to use each approach:
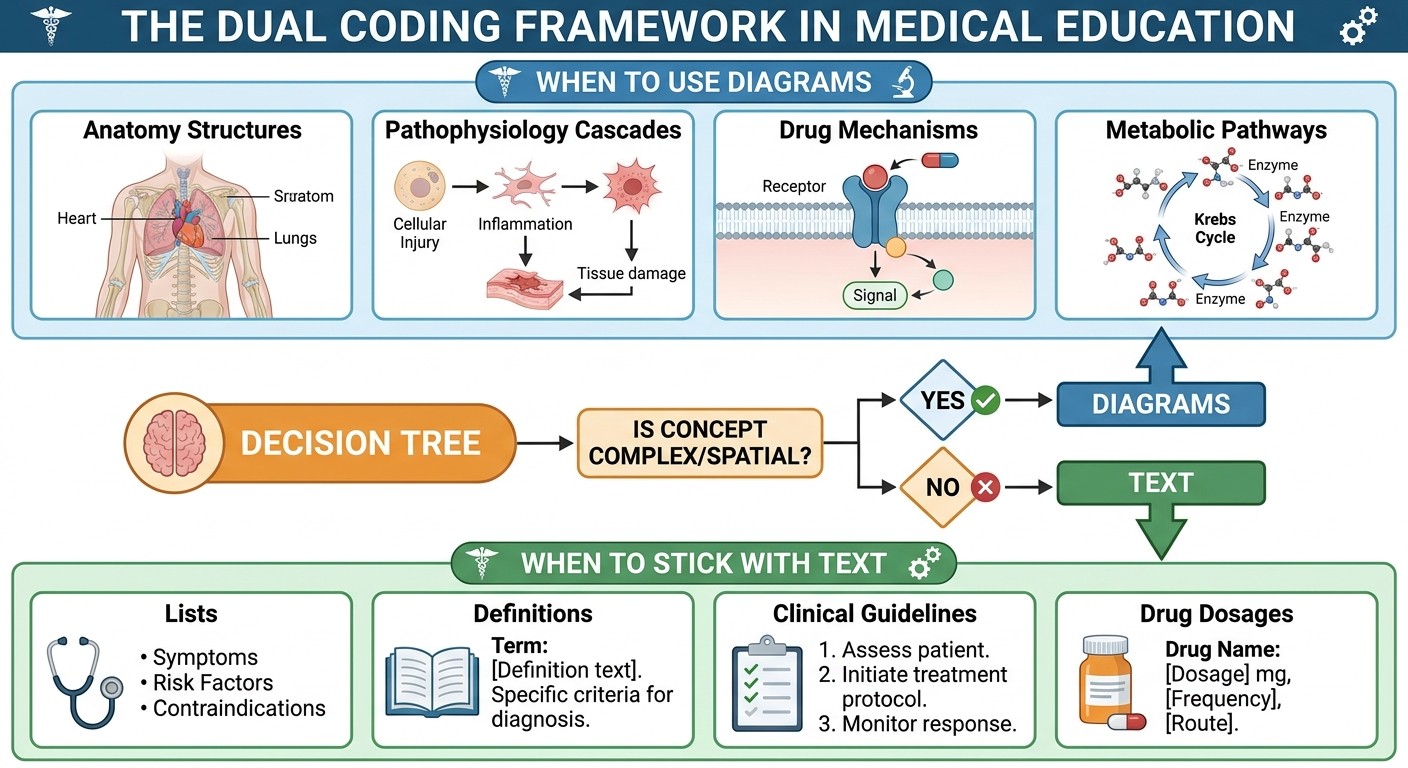
Use dual coding for:
Anatomical structures and their relationships
Pathophysiology cascades and feedback loops
Drug mechanisms and metabolic pathways
Disease progression and complications
Diagnostic algorithms and treatment protocols
Stick with text for:
Drug dosages and contraindications
Clinical guidelines and criteria
Statistical data and epidemiology
Historical facts and classifications
Symptom lists and mnemonics
The key question: does understanding the spatial or sequential relationship help you apply the knowledge? If yes, add a visual component.
Converting Dense Notes Into Visual Schemas
Your biochemistry textbook explains glycolysis in 847 words. Heres how to convert that into a dual-coded study tool that actually works:
Step 1: Extract the core pathway
Start with the linear sequence. Glucose → Glucose-6-phosphate → Fructose-6-phosphate → Pyruvate. Draw boxes connected by arrows.
Step 2: Add the regulatory layers
Mark the irreversible steps (hexokinase, phosphofructokinase, pyruvate kinase). Use different colors for rate-limiting enzymes. Add feedback inhibition arrows.
Step 3: Include the clinical connections
Label where genetic defects cause disease. Mark the steps affected by diabetes. Connect to lactate production in hypoxia.
Step 4: Test the reconstruction
Cover the diagram. Can you redraw the pathway from memory? Can you explain why phosphofructokinase deficiency causes exercise intolerance?
The text provides the detailed mechanisms. The diagram provides the spatial logic. Together, they create a complete mental model you can access under pressure.
For complex topics, Oncourse AI's Smart Lens feature helps bridge this gap - when you create a flashcard from a pathway diagram, Smart Lens adds explanatory layers that connect visual relationships to underlying mechanisms, letting you inspect the logic behind each connection without losing the big picture.
Using Labels and Arrows for Mechanism Mapping
Medical diagrams arent art projects. Every label and arrow serves a functional purpose. Heres how to make them work for recall:
Arrow conventions that matter:
Solid arrows: direct causation or flow
Dashed arrows: regulatory influence
Blocked arrows (⊥): inhibition
Bidirectional arrows: equilibrium or feedback
Curved arrows: electron movement in reactions
Label strategically:
Use standard abbreviations your exam will use (ACE, not angiotensin-converting enzyme)
Include numerical values where relevant (normal BP: 120/80)
Mark time scales (seconds for action potentials, hours for hormone responses)
Add clinical correlations in smaller text
Example: Renin-Angiotensin-Aldosterone System
Draw the kidney releasing renin. Arrow to angiotensinogen conversion. Label ACE at the lungs. Show aldosterone effects at the collecting duct. Add feedback inhibition from increased blood pressure back to renin release.
Each arrow represents a step you might need to explain in a viva. Each label connects to potential MCQ options.
The goal isnt creating perfect diagrams. Its building visual frameworks that support rapid retrieval and clinical application.
Self-Testing From Blank Diagrams
This is where dual coding proves its worth. You cant fake understanding when youre reconstructing a pathway from scratch.
The blank diagram method:
1. Draw the basic framework (boxes for organs, circles for hormones, rectangles for processes)
2. Fill in the labels from memory
3. Add the arrows and connections
4. Include regulatory mechanisms and clinical correlations
5. Check against your reference
Start with high-yield topics:
Cardiac conduction system
Nephron function and regulation
Coagulation cascade
Steroid hormone synthesis
Complement pathway
When studying with Oncourse's flashcard system, you can create dual-coded cards with text cues on one side and diagram reconstruction on the other. This lets you self-test both verbal recall and visual reconstruction, distinguishing whether you forgot the label, the relationship, or the mechanism. Pro tip: Time your reconstructions. In exams, you need rapid access to these pathways, not perfect artistic renditions.
Common Dual Coding Mistakes That Kill Recall
Most medical students get dual coding wrong. They treat diagrams as decoration instead of functional tools.
Mistake 1: Decorating instead of testing
Making beautiful, color-coded notes that you never test from memory. The act of creating pretty diagrams feels productive, but it doesnt build recall pathways.
Fix: Create rough, functional diagrams. Test reconstruction weekly. Mistake 2: Over-diagramming everything
Turning simple lists into complex flowcharts. Not every piece of medical knowledge needs visualization.
Fix: Use the framework above. If spatial relationships dont matter, stick with text. Mistake 3: Passive review of completed diagrams
Looking at finished concept maps without active retrieval. This creates false confidence.
Fix: Always test from blank versions. Cover labels and reconstruct from memory. Mistake 4: Ignoring clinical connections
Creating isolated academic diagrams that dont connect to patient presentations.
Fix: Add clinical correlations to every diagram. What does this pathway look like in disease? Mistake 5: Inconsistent symbols and conventions
Using different arrow styles and labeling systems across topics, creating confusion during recall.
Fix: Establish consistent visual vocabulary early and stick to it.
Subject-Specific Applications
Different medical subjects require different dual coding approaches:
Anatomy: Use cross-sectional views paired with surface landmarks. Label origin, insertion, innervation, and blood supply for muscles. Create layered diagrams showing deep to superficial structures. Physiology: Focus on feedback loops and regulatory mechanisms. Use graphs for dose-response relationships. Create timeline diagrams for processes that unfold over time. Pathology: Map normal structure to pathological changes. Use side-by-side comparisons. Include gross and microscopic correlations with clinical presentations. Pharmacology: Diagram drug targets within physiological pathways. Show receptor subtypes and their tissue distribution. Map side effects back to mechanism of action. Clinical subjects: Create diagnostic algorithms with branch points. Map symptom clusters to differential diagnoses. Show treatment protocols as decision trees.
After mastering pathway diagrams, using rapid recall games like Probe forces retrieval from multiple cues rather than single memorized sentences. This strengthens flexible recall thats useful when exams present the same concept through different angles - vignettes, lab values, imaging, or mechanisms.
Building Your Dual Coding Study System
Implementing dual coding requires systematic practice, not random diagram creation:
Week 1-2: Establish your visual vocabulary
Create a personal symbol library. Decide on arrow types, color coding, and labeling conventions. Use these consistently across all subjects.
Week 3-4: Convert existing notes
Take dense text-heavy topics and create visual schemas. Start with high-yield pathways youll see repeatedly.
Week 5+: Active reconstruction practice
Weekly testing sessions using blank diagrams. Time yourself. Identify gaps in understanding vs. gaps in recall.
Integration with your existing study routine:
Morning review: reconstruct 2-3 key diagrams from memory
Post-lecture: convert new material into visual format within 24 hours
Before exams: test blank diagram reconstruction under time pressure
After mistakes: create or revise diagrams for concepts you got wrong
The key is treating dual coding as a study method, not a note-taking style. The value comes from active reconstruction, not passive review of beautiful diagrams.
Frequently Asked Questions
How long should it take to create a good medical diagram?
15-30 minutes for initial creation, 5 minutes for reconstruction once you know the pathway. If youre spending hours perfecting diagrams, youre prioritizing aesthetics over function.
Should I memorize every detail in complex pathways?
No. Focus on rate-limiting steps, regulatory points, and clinical correlations. You need the logical framework, not every intermediate compound.
Can I use digital tools or should I draw by hand?
Both work. Hand drawing forces active processing during creation. Digital tools allow easy revision and consistent formatting. Use whatever you'll actually practice with regularly.
How do I know if dual coding is working for my recall?
Test yourself: can you explain the pathway to someone else using only your reconstructed diagram? Can you predict what happens when each step is blocked? If yes, its working.
What if I'm better at memorizing text than creating diagrams?
Start small. Convert one text-heavy topic per week into visual format. The goal isnt becoming an artist - its building additional retrieval pathways for complex material.
How many diagrams should I create for each subject?
Focus on high-yield topics that appear repeatedly in questions. Anatomy: 10-15 key systems. Physiology: 8-10 major regulatory pathways. Pathology: 5-7 core disease mechanisms per system.
---
Medical school throws massive amounts of interconnected information at you. Pure text-based studying treats everything as isolated facts to memorize. Dual coding helps you see the underlying logic and relationships that make medical knowledge predictable instead of random.
The goal isnt perfect diagrams. Its building visual frameworks that support rapid retrieval and clinical reasoning under pressure. When you can reconstruct pathways from memory and predict what happens when they go wrong, youve moved from memorization to understanding.
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for medical exams. Download free on Android and iOS.