Pathophysiology & Risk Factors - Under Pressure
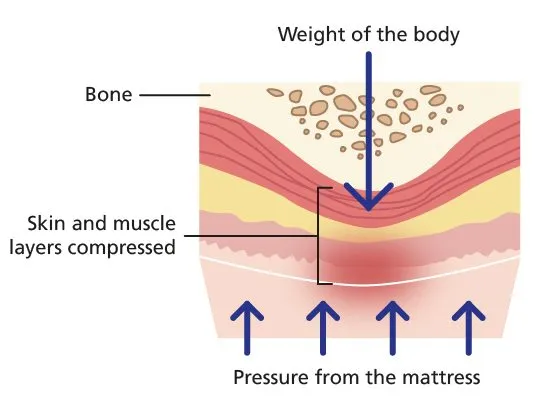
- Primary Injury: Sustained pressure on soft tissue, typically over a bony prominence, exceeds capillary filling pressure (>32 mmHg).
- Ischemic Cascade:
- Obstructed blood flow → ↓ tissue perfusion (ischemia) & lymphatic drainage.
- Waste product accumulation → inflammation, endothelial damage, thrombosis.
- Leads to irreversible tissue necrosis.
- Key Risk Factors:
- Immobility: sedation, paralysis, fractures.
- Sensory Loss: spinal cord injury, neuropathy.
- Extrinsic Factors: ↑ moisture (incontinence), friction, shear forces.
- Systemic Factors: poor nutrition (↓ albumin), anemia, altered mental status.
⭐ Shear forces, which stretch and distort tissue and vessels parallel to the skin, are more damaging than direct vertical pressure.
Pressure Ulcer Staging - Setting the Stage
| Stage | Depth of Tissue Loss | Clinical Presentation |
|---|---|---|
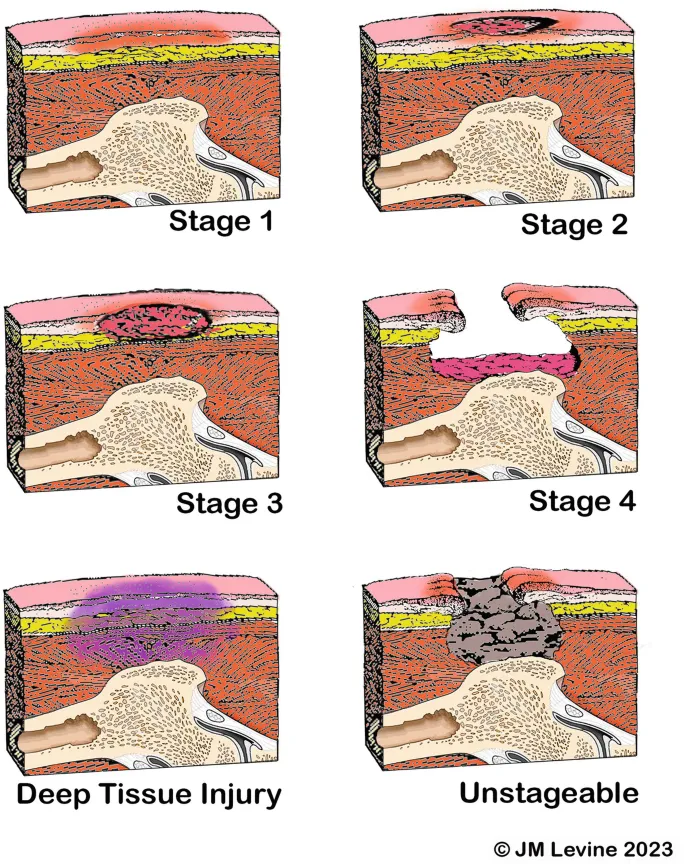
| Stage 1 | - | Intact skin with non-blanchable erythema. |
| Stage 2 | Partial-thickness | Shallow open ulcer with a red-pink wound bed, without slough. May also present as an intact or ruptured serum-filled blister. > ⭐ Exam favorite: Often mistaken for simple abrasion or tape burn. |
| Stage 3 | Full-thickness skin loss | Subcutaneous fat may be visible, but bone, tendon, or muscle are NOT exposed. Slough may be present. |
| Stage 4 | Full-thickness tissue loss | Exposed bone, tendon, or muscle. Slough or eschar may be present. Often includes undermining and tunneling. |
| Unstageable | Full-thickness tissue loss | Base of the ulcer is completely obscured by slough (yellow, tan, gray, green, or brown) and/or eschar (tan, brown, or black). |
| Deep Tissue Injury (DTI) | - | Purple or maroon localized area of discolored intact skin or blood-filled blister. |
Management by Stage - Healing the Hurt
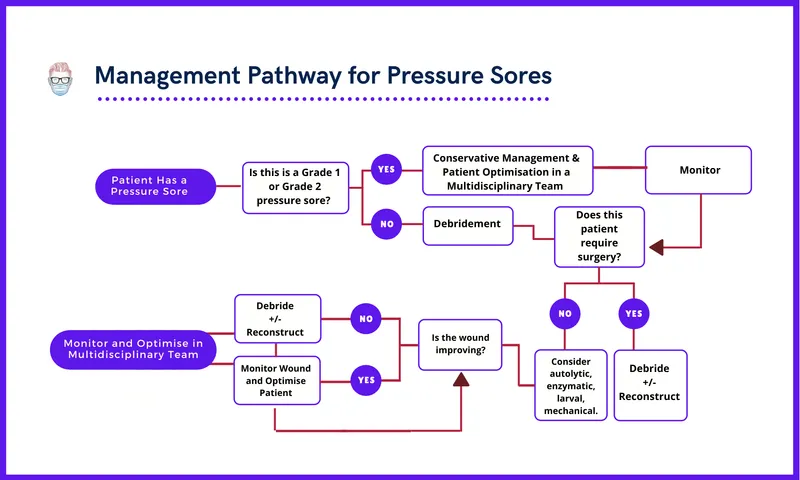
- Core Principles: Offload pressure, optimize nutrition (protein, vitamins), manage incontinence, and maintain a moist wound environment.
- Stage 1: Intact skin. Focus on aggressive pressure relief and protective dressings.
- Stage 2: Partial-thickness loss.
⭐ Hydrocolloid dressings are often favored as they are impermeable to bacteria, provide a moist environment, and promote autolytic debridement.
- Stage 3 & 4: Full-thickness loss. Requires debridement of necrotic tissue. Surgical consultation for advanced wounds.
- Unstageable: Obscured full-thickness loss. Must be debrided to determine true depth.
Prevention Strategies - Stop the Sore
- Risk Assessment: Regularly use the Braden scale to identify at-risk patients (score <18 indicates high risk).
- Repositioning & Offloading: Key to prevention.
- Turn bed-bound patients at least every 2 hours.
- Shift weight for chair-bound patients every 15-30 minutes.
⭐ Bed-bound patients should be repositioned at least every 2 hours, while chair-bound patients require more frequent shifts, every 15-30 minutes, to effectively offload pressure from ischial tuberosities.
- Support Surfaces: Use pressure-reducing devices.
- Examples: High-specification foam mattresses, alternating pressure air mattresses, or low-air-loss surfaces.
- Skin Care:
- Keep skin clean, dry, and moisturized.
- Apply barrier creams to protect from incontinence.
- Nutrition:
- Optimize protein and calorie intake to maintain tissue health.
High‑Yield Points - ⚡ Biggest Takeaways
- Pressure redistribution (e.g., q2h turning) is the single most important step in prevention and management.
- Stage 1 is intact skin with non-blanchable redness; Stage 2 is partial-thickness loss of dermis.
- Stage 3 is full-thickness loss into subcutaneous fat; Stage 4 involves exposed bone, tendon, or muscle.
- Unstageable ulcers have a bed obscured by slough/eschar and require debridement (except stable heel eschar).
- Deep Tissue Injury is a localized area of purple or maroon discolored intact skin.
- Management requires a moist wound environment, adequate nutrition, and continuous pressure offloading.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

