HBOT Physiology - The Pressure Cooker
- Core Principle: Utilizes Henry's Law ($P = k_H \cdot C$), which states that ↑ ambient pressure ↑ the amount of gas dissolved in a liquid. HBOT involves breathing 100% O₂ at pressures >1.4 atmospheres absolute (ATA).
- Primary Effect: Dramatically ↑ dissolved oxygen in plasma (from 0.3 mL/dL to ~6 mL/dL at 3 ATA), independent of hemoglobin saturation.
- Mechanism: Creates a massive oxygen partial pressure gradient between plasma and ischemic tissues, driving O₂ deep into poorly perfused areas.
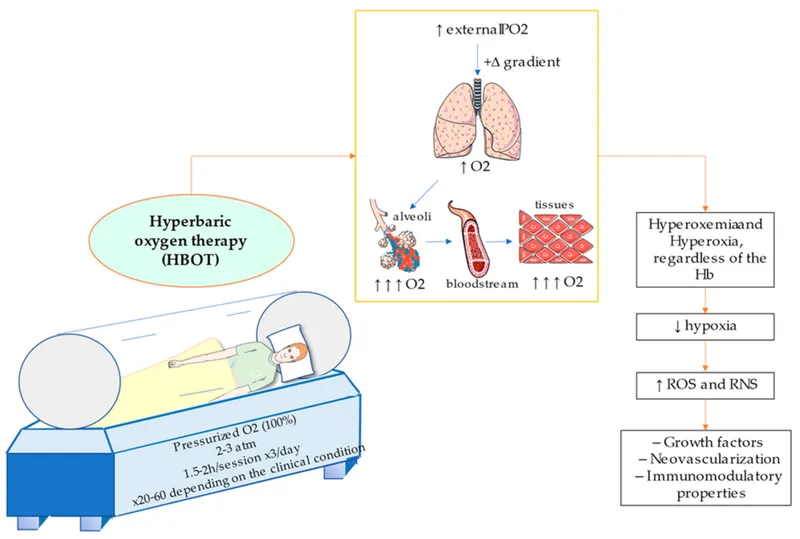
⭐ At 3 ATA, dissolved plasma oxygen alone can meet resting metabolic demands, a state where life is theoretically sustainable without red blood cells.
HBOT Indications - Green Light Conditions
Key approved uses for Hyperbaric Oxygen Therapy. Remember the mnemonic 📌 "CAN'T HEAL".
- Carbon Monoxide & Cyanide Poisoning
- Reduces carboxyhemoglobin half-life from ~300 min (room air) to ~20 min.
- Air or Gas Embolism
- Reduces bubble size and improves oxygenation to ischemic tissues.
- Necrotizing Soft Tissue Infections
- Halts toxin production (e.g., Clostridium perfringens alpha-toxin).
- Traumatic Ischemias & Crush Injuries
- Reduces edema and supports marginal tissue viability.
- Healing-Impaired Wounds
- e.g., Diabetic foot ulcers (Wagner grade ≥3), refractory osteomyelitis.
- Enhanced Radiation Recovery
- Treats osteoradionecrosis and soft tissue radiation necrosis.
- Acute Thermal Burns
- For deep partial-thickness or full-thickness burns, often >20% TBSA.
- Late Radiation Injury
⭐ In CO poisoning, HBOT is critical because it displaces CO from mitochondrial cytochrome c oxidase, restoring aerobic metabolism-a mechanism beyond just clearing carboxyhemoglobin.
HBOT Risks - Red Flags & Dangers
- Absolute Contraindication:
- Untreated pneumothorax → risk of tension pneumothorax.
⭐ Exam Favorite: The only absolute contraindication to HBOT is an untreated pneumothorax. Air trapped in the pleural space will expand upon decompression, leading to a life-threatening tension pneumothorax.
- Major Risks & Complications:
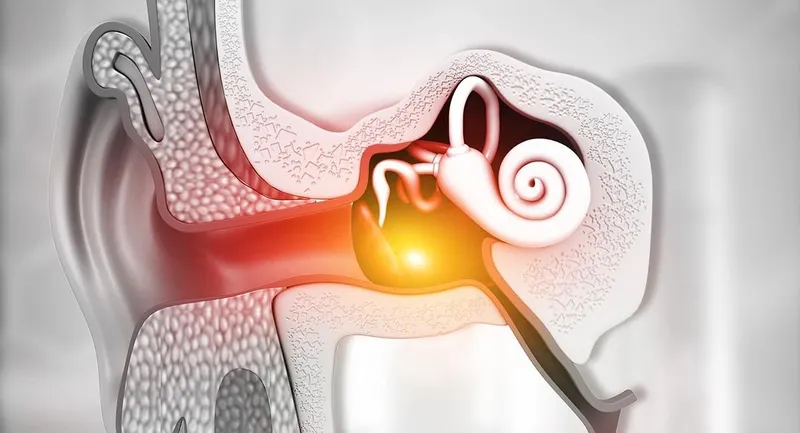
- ⚠️ Barotrauma: Most common side effect. Affects ears (tympanic membrane rupture), sinuses, and lungs.
- Oxygen Toxicity:
- CNS: Seizures (grand mal), visual changes, tinnitus. Risk ↑ with seizures history.
- Pulmonary: Substernal chest pain, cough, progressing to ARDS-like picture.
- Ocular Effects: Reversible myopia is common after multiple sessions.
- Relative Contraindications:
- COPD/Asthma
- Claustrophobia
- Recent fever or seizure
- Chemotherapy agents (e.g., Bleomycin, Doxorubicin)
High‑Yield Points - ⚡ Biggest Takeaways
- Mechanism: Involves breathing 100% oxygen at pressures >1 atmosphere absolute (ATA), significantly increasing dissolved plasma O2.
- Wound Healing: Promotes collagen synthesis, angiogenesis, and fibroblast proliferation, particularly in hypoxic or ischemic wounds.
- Key Indications: Crucial for diabetic foot ulcers, chronic refractory osteomyelitis, radiation injuries, and gas gangrene.
- Antimicrobial Effects: Directly inhibits anaerobic bacteria (like Clostridium perfringens) and enhances leukocyte killing.
- Major Side Effect: The most common adverse effect is barotrauma to the ears, sinuses, and lungs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

