🩸 Anatomy - Plumbing for Purity
-
Access Types & Preference:
- Arteriovenous Fistula (AVF): Direct artery-to-vein anastomosis. Best patency, lowest infection rate.
- Arteriovenous Graft (AVG): Synthetic tube connecting artery and vein.
- Central Venous Catheter (CVC): Tunneled catheter (e.g., Permacath). Highest infection risk; used for immediate/temporary access.
-
Common AVF Sites (Distal to Proximal):
- Radiocephalic (Brescia-Cimino): Radial artery & cephalic vein.
- Brachiocephalic: Brachial artery & cephalic vein.
⭐ Rule of 6s for AVF Maturation: A usable fistula should be:
- Flow > 600 mL/min
- Diameter > 6 mm
- Depth < 6 mm from skin
- Matures in ~6 weeks
📌 Mnemonic: "Fistula First" - the preferred primary access.
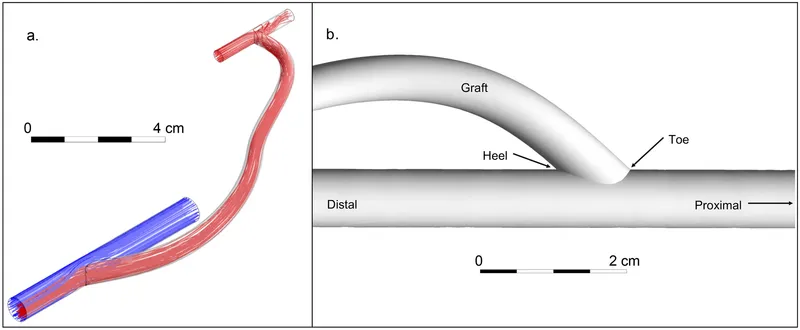
💉 Clinical - The Access Trinity
📌 Fistula > Graft > Catheter. Choice depends on urgency and vessel quality.
- AV Fistula (AVF): Gold standard; direct artery-vein connection (e.g., radiocephalic).
- Pros: Best long-term patency, lowest infection/thrombosis risk.
- Cons: Requires ~2-3 months to mature; potential for steal syndrome.
- AV Graft (AVG): Synthetic (PTFE) tube connects artery to vein.
- Pros: Usable sooner (2-4 weeks); for patients with inadequate veins.
- Cons: Higher thrombosis, stenosis, and infection risk than AVF.
- CVC: Tunneled catheter for temporary/bridge access.
- Pros: Immediate use.
- Cons: ⚠️ Highest infection risk (S. aureus bacteremia), central venous stenosis.
⭐ The most common cause of AVF/AVG failure is thrombosis, typically due to stenosis at the venous anastomosis. Loss of a palpable thrill or audible bruit is a key sign.
💔 Complications - When Lifelines Fail
- Thrombosis: Most common cause of access failure.
- Sx: Sudden loss of thrill/bruit.
- Tx: Pharmacomechanical thrombectomy or surgical thrombectomy.
- Stenosis: Typically at the venous anastomosis.
- Sx: ↑ venous pressures during dialysis, prolonged bleeding post-cannulation, limb swelling.
- Dx: Duplex US; fistulogram is gold standard.
- Tx: Balloon angioplasty ± stenting.
- Infection: Risk: Catheter > Graft (AVG) > Fistula (AVF).
- Pathogen: S. aureus is most common.
- Tx: IV antibiotics; may require graft excision for AVG infection.
- Dialysis Access Steal Syndrome (DASS):
- Patho: Ischemia distal to access due to shunting of arterial blood.
- Sx: Pain (especially with exertion/dialysis), pallor, paresthesias, cool digits.
- Aneurysm/Pseudoaneurysm:
- Cause: High flow, repeated needle sticks weaken the wall.
- Tx: Surgical repair if symptomatic, rapidly expanding, or skin erosion.
⭐ New-onset hand pain, numbness, and coolness after AV fistula creation is classic for Dialysis Access Steal Syndrome (DASS).
🔧 Management - Salvage Operations
- Goal: Preserve existing access & avoid new access creation.
- Primary Interventions: Endovascular approaches are first-line.
- Thrombectomy: For clotted access. Can be percutaneous (pharmacomechanical) or open surgical.
- Angioplasty (PTA): Balloon dilation for stenosis. Stents used for elastic recoil or recurrent lesions.
- Surgical Revisions:
- Anastomotic revision/Interposition graft: For complex stenosis or aneurysmal changes.
- Banding/DRIL: For dialysis-associated steal syndrome to ↓ flow.
⭐ The most common site of stenosis in an AV fistula is the venous outflow tract, just distal to the anastomosis.
⚡ Biggest Takeaways
- AV fistula (AVF) is the preferred access: best patency, lowest infection/thrombosis rates.
- AVFs require ~6-8 weeks to mature ("Rule of 6s"); grafts are usable in ~2-3 weeks.
- Stenosis and thrombosis are the most common complications of AVF/AVG, often at the venous anastomosis.
- Central venous catheters have the highest risk of infection (S. aureus) and central vein stenosis.
- Dialysis steal syndrome causes distal limb ischemia (pain, pallor) after access creation.
- High-output heart failure is a rare complication from excessive shunting through large, proximal access.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

