💎 Stone Cold Science
Nephrolithiasis results from urine supersaturation with stone-forming solutes, leading to crystal precipitation and growth. Key factors include low urine volume, abnormal pH, and metabolic disturbances.
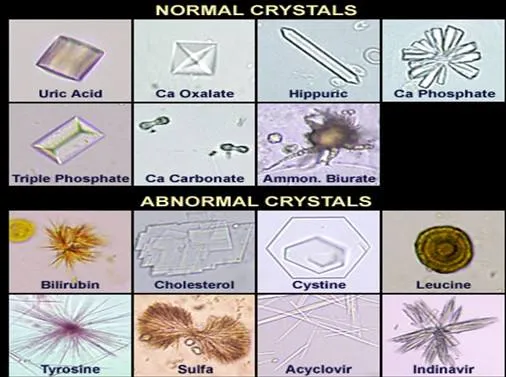
| Stone Type | Composition | Cause/Risk Factors | Urine pH | X-ray | Treatment |
|---|---|---|---|---|---|
| Ca Oxalate | $CaC_2O_4$ | Most common. Hypercalciuria, hyperoxaluria (Crohn's) | ↓ or neutral | Opaque | Thiazides, citrate |
| Ca Phosphate | $Ca_3(PO_4)_2$ | Hypercalciuria, Renal Tubular Acidosis (Type 1) | ↑ (Alkaline) | Opaque | Treat RTA |
| Struvite | $MgNH_4PO_4$ | Urease+ UTI (Proteus, Klebsiella); staghorn calculi | ↑ (Alkaline) | Opaque | Abx, stone removal |
| Uric Acid | Uric Acid | Gout, ↑cell turnover (leukemia), dehydration | ↓ (Acidic) | Lucent | Allopurinol, alkalinize |
| Cystine | Cystine | Genetic defect (cystinuria), hexagonal crystals | ↓ (Acidic) | Faintly opaque | Alkalinize, penicillamine |
😫 Clinical Manifestations - The Agony of the Stone
- Renal Colic: Acute, severe, colicky flank pain. Patients are often writhing, unable to find a comfortable position.
- Pain Radiation: Follows the stone's path.
- Upper Ureter: Flank/CVA pain.
- Mid Ureter: Radiates anteriorly to groin, testes, or labia.
- Distal Ureter (UVJ): Lower quadrant pain, mimics UTI with urgency/frequency.
- Associated Symptoms:
- Hematuria (gross or microscopic).
- Nausea & vomiting (shared autonomic innervation).
- Physical Exam:
- Costovertebral angle (CVA) tenderness.
⭐ The inability to find a comfortable position is a classic sign, distinguishing it from peritonitis where patients lie still.
🕵️♂️ Diagnosis - Finding the Culprit
-
Initial Workup:
- Urinalysis (UA): Essential first step. Look for hematuria (microscopic/gross).
- Urine pH: Suggests stone type.
- pH < 5.5: Uric acid, Cystine stones.
- pH > 7.2: Struvite (infection) stones.
- Basic Metabolic Panel (BMP): Assess renal function (BUN/Cr).
-
Imaging Modalities:
- Non-contrast CT (Abdomen/Pelvis): Gold standard. High sensitivity & specificity.
- Ultrasound (US): Preferred in pregnant patients & children to avoid radiation.
- KUB X-ray: Monitors radiopaque stones (e.g., Calcium).
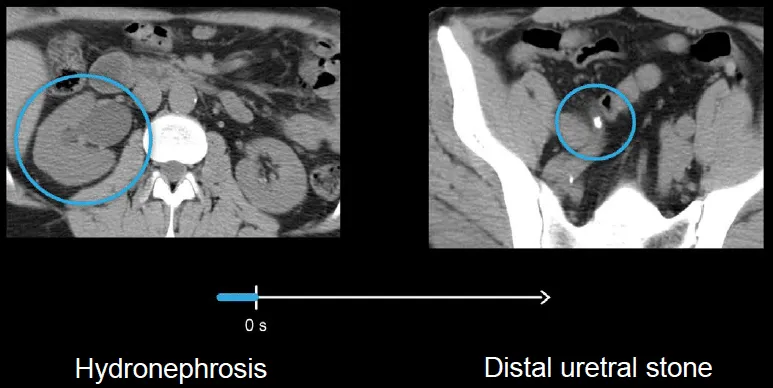
⭐ Non-contrast helical CT is the single best test for diagnosing acute flank pain suspicious for nephrolithiasis in non-pregnant adults. It identifies stone size, location, and degree of obstruction.
💎 Management - Crush, Grab, Blast
- Medical Expulsive Therapy (MET): For uncomplicated stones <10 mm.
- Hydration, analgesia (NSAIDs), and alpha-blockers (e.g., Tamsulosin).
- Extracorporeal Shock Wave Lithotripsy (ESWL): "Blast"
- Non-invasive acoustic pulses. Best for stones <2 cm in the renal pelvis/upper ureter.
- ⚠️ Contraindicated in pregnancy, bleeding diathesis.
- Ureteroscopy (URS): "Grab"
- Endoscopic approach; laser fragments stone, basket retrieves.
- Primary for mid-to-distal ureteral stones.
- Percutaneous Nephrolithotomy (PCNL): "Crush"
- Invasive access through the flank. For large stones (>2 cm) or staghorn calculi.
⭐ High-Yield: For stones 1-2 cm, the choice between ESWL and ureteroscopy depends on location. ESWL is preferred for renal pelvis/upper ureter stones, while ureteroscopy is better for mid/distal ureteral stones and offers a higher stone-free rate.
⚡ Biggest Takeaways
- Non-contrast CT is the gold standard for diagnosis; use ultrasound in pregnant patients or children.
- Stones < 5 mm typically pass spontaneously; manage with hydration, pain control, and medical expulsive therapy (tamsulosin).
- Stones > 10 mm rarely pass and usually require intervention.
- ESWL is for smaller stones (< 2 cm) in the renal pelvis or upper ureter.
- Ureteroscopy is preferred for mid-to-distal ureteral stones.
- PCNL is reserved for large stones (> 2 cm) or staghorn calculi.
- Urosepsis, AKI, or anuria require urgent decompression via stent or nephrostomy tube.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

