Infection Timeline - The Risky Calendar
-
<1 Month (Immediate): Hospital-acquired infections dominate. Think bacterial sources from the surgical wound, IV lines (catheter-related), or ventilator-associated pneumonia. Candida infections are also frequent.
-
1-6 Months (Delayed): Corresponds to peak immunosuppressive therapy. This is the prime window for opportunistic pathogens normally controlled by T-cells (e.g., Pneumocystis jirovecii, Aspergillus).
-
>6 Months (Late): As immunosuppression is reduced, the risk profile shifts. Patients are more susceptible to common community-acquired pathogens and reactivation of chronic viruses like BK virus (nephropathy).
⭐ Cytomegalovirus (CMV) is the quintessential opportunistic infection of the 1-6 month period. It can manifest as pneumonitis, colitis, retinitis, or a mono-like syndrome.
Opportunistic Bugs - The Usual Suspects
- CMV (Cytomegalovirus): The most significant pathogen in the 1-6 month window.
- Presents as pneumonitis, esophagitis/colitis, hepatitis, or retinitis.
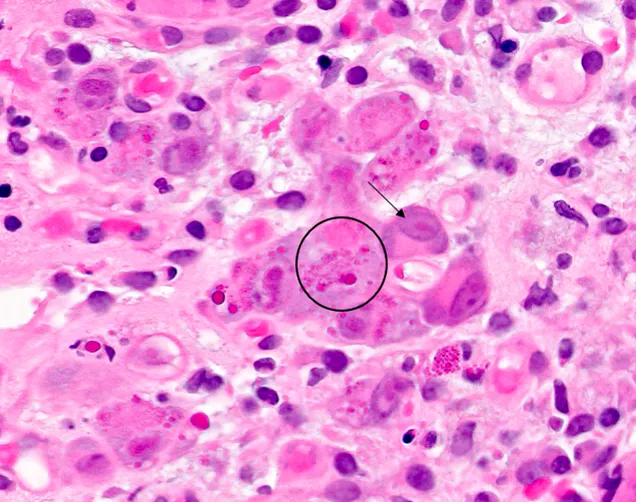
- Biopsy reveals characteristic "owl's eye" intranuclear inclusions.
- Pneumocystis jirovecii (PJP):
- Causes diffuse interstitial pneumonia; diagnosed via bronchoalveolar lavage (BAL).
⭐ Prophylaxis is crucial, typically with Trimethoprim-Sulfamethoxazole (TMP-SMX) for the first 6-12 months post-transplant.
- Other Key Pathogens:
- Fungi: Aspergillus fumigatus (invasive disease, "halo sign" on chest CT), Candida species.
- Bacteria: Nocardia (cavitary lung lesions, brain abscesses), Listeria monocytogenes (meningitis).
- Viruses: EBV (risk of Post-Transplant Lymphoproliferative Disorder - PTLD), VZV.
Prophylaxis & Tx - The Protective Shield
-
Universal Prophylaxis (First 6-12 months):
- PJP/PCP: Lifelong TMP-SMX. Alternatives: atovaquone, dapsone.
- CMV: Valganciclovir for high-risk (D+/R-). Others monitored with PCR (pre-emptive therapy).
- Fungal (Candida): Fluconazole or nystatin, especially with high steroid use.
- HSV/VZV: Acyclovir or valacyclovir if seropositive.
-
Treatment Approach:
- Guided by pathogen identification (culture, PCR, biopsy).
- Crucial first step: Reduce immunosuppression if feasible, balancing rejection risk.
⭐ For febrile neutropenia post-transplant, initial treatment requires broad-spectrum coverage against Pseudomonas, like cefepime or piperacillin-tazobactam.
High‑Yield Points - ⚡ Biggest Takeaways
- Infection timing is the most crucial diagnostic clue.
- <1 month post-transplant: Think nosocomial bacterial infections from the surgical site, catheters, or aspiration.
- 1-6 months: This is the classic window for opportunistic infections (e.g., CMV, PJP, Aspergillus) due to peak immunosuppression.
- >6 months: The risk profile shifts towards community-acquired pathogens and chronic viral infections like BK virus nephropathy.
- Universal prophylaxis with TMP-SMX (for PJP) is standard.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

