Ileus & SBO - The Great Gut Slowdown
- Ileus: Functional, non-mechanical obstruction. Uniformly dilated bowel loops. Common causes: post-op state, opioids, hypokalemia, sepsis.
- Small Bowel Obstruction (SBO): True mechanical blockage. Key finding: transition point with dilated proximal bowel and collapsed distal bowel. Common causes: Adhesions (>75%), hernias, tumors.
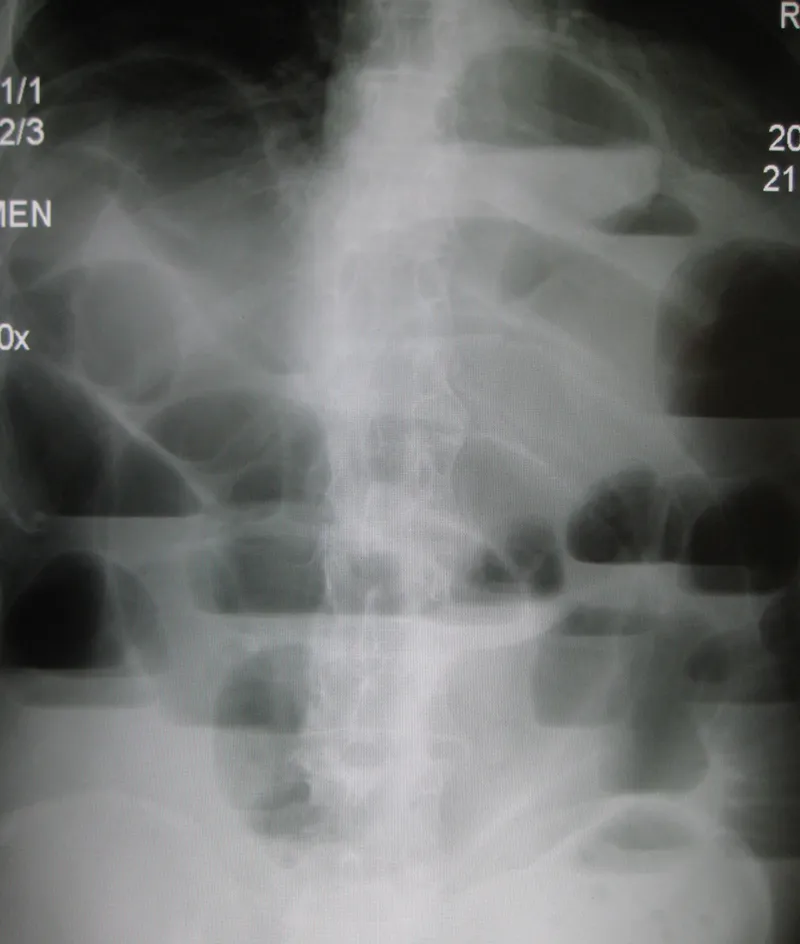
⭐ The most common cause of SBO is post-surgical adhesions. In a "virgin" abdomen (no prior surgery), incarcerated hernias are a primary suspect.
Pathophysiology - Guts on Strike
Post-surgical gut paralysis (ileus) results from a coordinated inflammatory and neurogenic response.
- Neurogenic Phase (Immediate):
- Surgical stress activates splanchnic nerves, leading to a surge in sympathetic tone (norepinephrine).
- Inhibits parasympathetic (vagal) activity, silencing pro-kinetic pathways.
- Inflammatory Phase (Delayed):
- Gut handling triggers resident macrophage activation in the muscularis externa.
- Release of inflammatory mediators (e.g., IL-1α, IL-6, TNF-α) recruits more leukocytes.
- This inflammatory soup suppresses smooth muscle contractility.

⭐ Ileus is physiologic for 2-3 days post-op. If it persists beyond 3-5 days (prolonged ileus), it must be distinguished from mechanical obstruction, often requiring CT imaging.
Diagnosis & Workup - Deciphering the Silence
-
Clinical Evaluation:
- History: Recent surgery, medications (opioids), electrolyte imbalance.
- Physical Exam: Abdominal distension, minimal tenderness, absent/hypoactive bowel sounds.
-
Imaging Studies:
- Abdominal X-ray (AXR): First-line test. Shows generalized, uniform dilation of both small and large bowel; no transition point.
- CT Scan: More specific. Confirms ileus, rules out mechanical obstruction, and can identify underlying causes (e.g., abscess).

⭐ On imaging, paralytic ileus is distinguished from SBO by gas and dilation throughout both the small and large bowel, whereas SBO typically shows a clear transition point with distal bowel collapse.
Management - Getting Things Moving
- Conservative First: NPO/clears, IV fluids, correct electrolytes (K⁺, Mg²⁺), early & frequent ambulation.
- Decompression: Nasogastric (NG) tube if significant vomiting or distention.
- Remove Obstacles: Minimize opioids (use multimodal analgesia), treat underlying causes.
- Pharmacologic Aids:
- Alvimopan: Peripherally-acting µ-opioid antagonist for postoperative ileus after bowel resection.
- Chewing gum can act as "sham feeding" to stimulate the vagus nerve.
⭐ Alvimopan is for short-term, inpatient use only (max 7 days or 15 doses) due to an increased risk of myocardial infarction with long-term use.

High‑Yield Points - ⚡ Biggest Takeaways
- Postoperative ileus is a functional, non-mechanical bowel obstruction from inflammatory mediators and ↑ sympathetic tone.
- Presents with absent bowel sounds, nausea, vomiting, and failure to pass flatus or stool.
- Physiologic ileus typically resolves within 72 hours; a longer duration is considered prolonged ileus.
- Opioid use is the most significant risk factor; also check for hypokalemia.
- Management is supportive: NPO, IV fluids, and minimizing opioids.
- Differentiate from SBO via X-ray: ileus shows diffusely dilated bowel loops, while SBO has a clear transition point.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

