Cardiac Risk Assessment - Sizing Up The Heart
- Goal: Identify patients at risk for Major Adverse Cardiac Events (MACE).
- Functional Capacity: Assessed in Metabolic Equivalents ($METs$).
- Poor: <4 METs (e.g., slow walking, self-care).
- Excellent: >10 METs (e.g., strenuous sports).
- Revised Cardiac Risk Index (RCRI): 1 point per risk factor.
- High-risk surgery (e.g., vascular)
- History of ischemic heart disease
- History of CHF
- History of CVA/TIA
- Pre-op insulin use
- Pre-op creatinine >2.0 mg/dL
⭐ In patients with elevated risk (RCRI ≥1) but good functional capacity (≥4 METs), it is reasonable to proceed with the planned surgery without further cardiac testing.
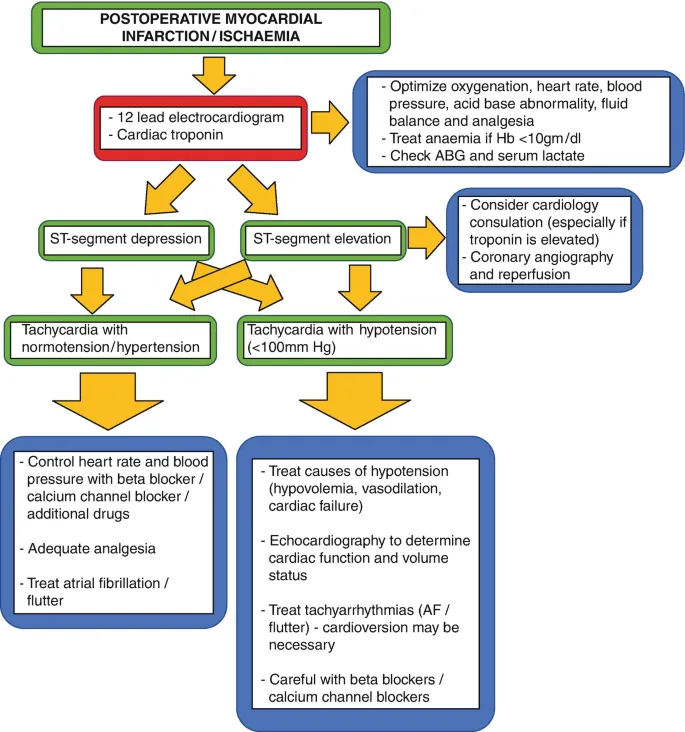
Perioperative MI - The Silent Killer
- Pathophysiology: Surgical stress → catecholamine surge → tachycardia & hypertension → ↑O₂ demand and ↓diastolic filling time → myocardial ischemia.
- Clinical Presentation: Often silent (no chest pain) due to anesthesia/analgesia. May present as hypotension, arrhythmia, delirium, or oliguria.
- Diagnosis:
- ECG: New ST-segment changes, LBBB, or pathologic Q waves.
- Biomarkers: Rise and/or fall of troponins with at least one value >99th percentile.
- Prevention: Preoperative risk stratification (RCRI score), β-blockers in high-risk patients, and statin therapy.
⭐ Most perioperative MIs are NSTEMIs and occur within 48-72 hours post-op, often triggered by physiologic stressors like pain and anemia.
Post-Op Heart Failure - The Pump Sputters
-
Etiology: Often due to fluid overload from IV fluids, stress-induced myocardial ischemia/infarction, or exacerbation of underlying chronic heart failure (especially diastolic dysfunction).
-
Diagnosis: Look for dyspnea, bilateral crackles, JVD, and a new S3 gallop.
- Labs: ↑ BNP (B-type Natriuretic Peptide > 400 pg/mL).
- Imaging: Chest X-ray shows pulmonary edema; echocardiogram is the definitive diagnostic tool.
-
Management:
- 📌 LMNOP: Lasix (furosemide) for diuresis, Morphine for venodilation/anxiolysis, Nitrates for vasodilation, Oxygen for hypoxia, Position (sit upright).
⭐ The most common cause of post-operative heart failure is iatrogenic fluid overload, particularly in elderly patients with unrecognized pre-existing diastolic dysfunction.

Post-Op Arrhythmias - The Heart's Hiccups
-
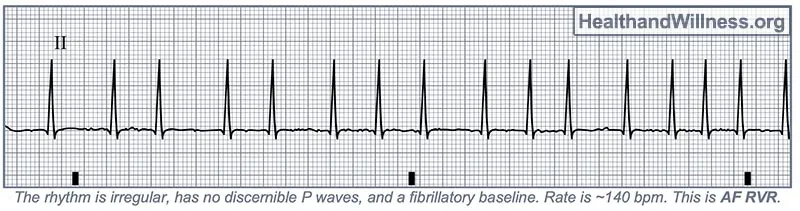
Commonly occurs 2-4 days post-op, with Atrial Fibrillation (AFib) being the most frequent type.
-
Key Triggers:
- Electrolyte imbalance (↓K⁺, ↓Mg²⁺)
- Hypoxemia, anemia, pain
- Volume overload, inflammation
- Underlying cardiac disease
-
Management Steps:
- 1st: ABCs, EKG, check labs (electrolytes, troponins).
- Stable AFib: Rate control is key. Use β-blockers (metoprolol) or CCBs (diltiazem).
- Unstable (hypotension, shock): Immediate synchronized cardioversion.
⭐ High-Yield: New-onset post-op AFib is a major risk factor for future stroke and mortality. Consider prophylactic β-blockers in high-risk patients undergoing major surgery.
High‑Yield Points - ⚡ Biggest Takeaways
- Perioperative MI is the leading cause of death after noncardiac surgery, often presenting silently within 48 hours.
- Use the Revised Cardiac Risk Index (RCRI) to stratify patients; key risks include IHD, CHF, CVA, DM on insulin, and Cr >2.
- Prophylactic beta-blockers and statins are crucial in high-risk patients to reduce cardiac events.
- Postoperative atrial fibrillation is common; prioritize rate control over rhythm control initially.
- New-onset pulmonary edema suggests either fluid overload or underlying cardiac dysfunction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

