Risk Factors - The Usual Suspects
Key predictors for postoperative pulmonary complications (PPCs) divide into patient-specific and procedure-specific categories.
| Patient-Related Factors | Procedure-Related Factors |
|---|---|
| * Age >60 years | * Surgical Site (greatest risk) |
| * COPD / Asthma | - Aortic > Thoracic > Abdominal |
| * Active Smoking (w/in 2 mo) | * Anesthesia > 3 hours |
| * Obstructive Sleep Apnea (OSA) | * General Anesthesia |
| * Congestive Heart Failure (CHF) | * Emergency Surgery |
| * Functional Dependence | * NG tube placement |
| * Serum Albumin <3.5 g/dL | |
| * BUN >21 mg/dL |
⭐ The single most important predictor of postoperative pulmonary risk is the surgical site. Aortic and thoracic surgeries carry the highest risk.
Clinical & PFT Assessment - Sizing Up the Lungs
- Clinical Predictors:
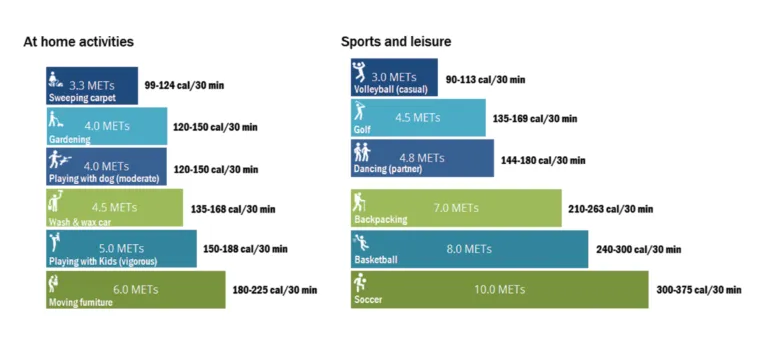
- Functional capacity: Inability to climb 2 flights of stairs (< 4 METs) is a key risk marker.
- Smoking: Advise cessation >8 weeks pre-op.
- Symptoms: Chronic cough, dyspnea, or wheezing.
- Comorbidities: COPD, asthma, obesity (BMI >30), obstructive sleep apnea (OSA).
- Pulmonary Function Tests (PFTs):
- Not routine. Indicated for patients undergoing lung resection or with unexplained dyspnea.
- High-risk markers for non-resection surgery:
- FEV₁ < 1.5 L
- PaCO₂ > 45 mmHg on baseline ABG.
⭐ For lung resection, the predicted postoperative FEV₁ (ppoFEV₁) is the most critical value. A ppoFEV₁ < 40% of predicted signals very high risk.
Risk Reduction Strategies - Pre-Op Power-Ups
- Smoking Cessation:
- The single most important intervention.
- Advise cessation at least 4-8 weeks pre-op to significantly ↓ risk of post-op complications.
- Nicotine replacement therapy can aid success.
- Optimize Underlying Lung Disease:
- Asthma: Ensure symptoms are well-controlled. Consider a pre-op "tune-up" with inhaled corticosteroids or a short course of oral steroids if recently unstable. Administer pre-op SABA.
- COPD: Optimize with bronchodilators (e.g., tiotropium, albuterol). Treat exacerbations with systemic steroids and/or antibiotics.
- Lung Expansion & Secretion Clearance:
- Pre-operative patient education is key for post-op compliance.
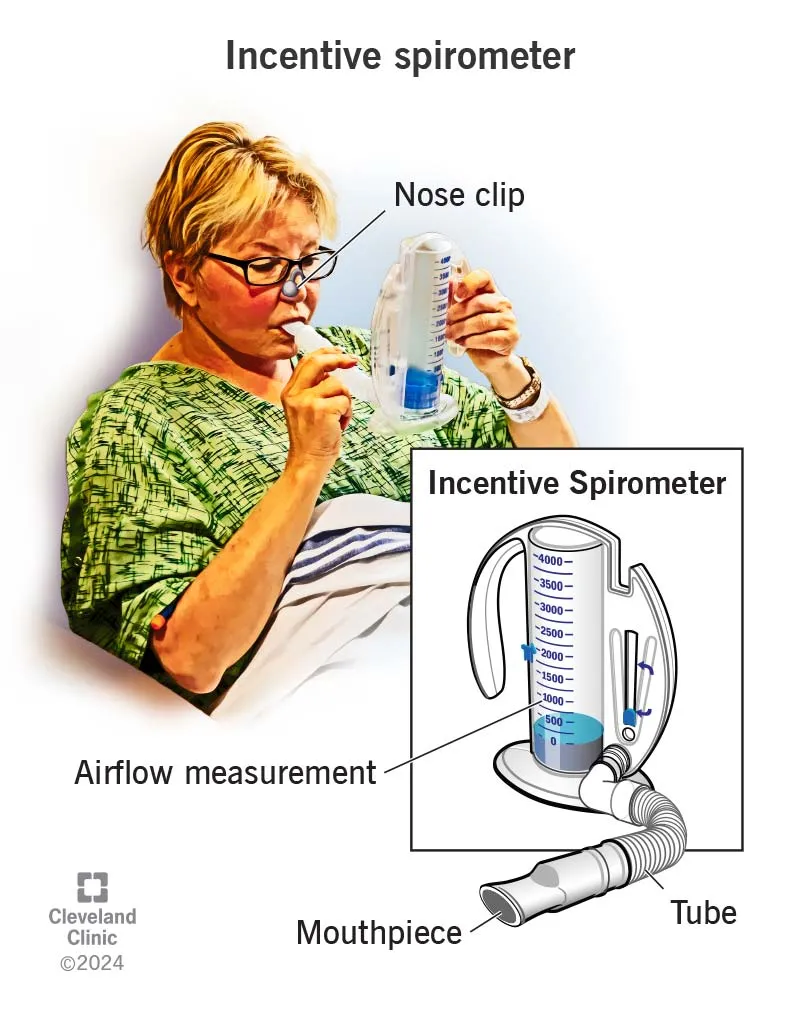
- Techniques: Incentive Spirometry (IS), deep breathing exercises, directed coughing.
- Consider pre-op Inspiratory Muscle Training (IMT) for high-risk patients.
- Infection Control:
- Treat any existing bronchitis or pneumonia with appropriate antibiotics before elective surgery.
⭐ Any period of smoking cessation is beneficial, but stopping <2 weeks before surgery may paradoxically increase postoperative pulmonary complications due to transiently increased sputum production. The ideal window is >4 weeks.
- Surgical site is the most important predictor of postoperative pulmonary complications (PPCs).
- Major risk factors include COPD, smoking, obstructive sleep apnea (OSA), age >60, and ASA class >II.
- Advise smoking cessation at least 4 weeks pre-operatively to reduce risk.
- Routine PFTs are not recommended; consider for unexplained dyspnea or planned lung resection.
- Atelectasis is the most common PPC, usually developing within 48 hours post-op.
- Prevention involves pre-op optimization and post-op lung expansion maneuvers like incentive spirometry.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

