Imaging Principles - To Scan or Not
- Core Principle: Avoid routine, non-specific preoperative testing. Aligns with the "Choosing Wisely" campaign to reduce unnecessary procedures and costs.
- When to Defer Imaging:
- Routine pre-op chest X-rays (CXRs) are not indicated for asymptomatic patients with an unremarkable history and physical exam.
- Imaging should only be ordered if results are likely to influence management.
- Decision Support:
- Consult the American College of Radiology (ACR) Appropriateness Criteria® to guide evidence-based imaging selection.
⭐ In asymptomatic patients, routine preoperative chest X-rays do not decrease postoperative pulmonary complications.

Imaging Modalities - The Right Tool Kit
Selecting the appropriate imaging is crucial for accurate diagnosis and surgical planning. Key considerations include tissue type, urgency, and patient-specific risks like radiation exposure or contrast allergies.
| Modality | Best For | Key Pre-op Use Cases | Major Risks/Cons |
|---|---|---|---|
| X-ray | Bone, air, metal | Fracture detection, line placement confirmation, bowel obstruction/ileus | Ionizing radiation |
| Ultrasound | Soft tissue, fluid | Gallbladder disease, DVT, abscess localization, vascular access | Operator dependent |
| CT Scan | Bone, soft tissue, vessels | Trauma evaluation, abscess, malignancy staging, pulmonary embolism | High radiation, contrast nephropathy/allergy |
| MRI | Soft tissue detail | Spinal cord/brain injury, soft tissue tumors, ligament/tendon tears, MRCP | Slow, expensive, strong magnetic fields |
- Contrast Considerations:
- Iodinated contrast (CT): Risk of contrast-induced nephropathy (CIN). Screen with creatinine if GFR < 60 or other risk factors exist.
- Gadolinium (MRI): Risk of nephrogenic systemic fibrosis (NSF) in severe renal disease (GFR < 30).
⭐ In suspected appendicitis, ultrasound is the preferred initial imaging in children and pregnant women to avoid radiation; CT is often used in other adults for its high accuracy.
📌 Mnemonic for MRI Contraindications (P.A.C.E.M.A.K.E.R.):
- Pacemakers / ICDs
- Aneurysm clips (ferromagnetic)
- Cochlear implants
- Electronic or Metallic implants
- Artificial heart valves (older types)
- Kidney disease (severe)
- Eye (metal foreign body)
- Rapid tissue expanders
Clinical Algorithms - Surgical Snapshots
- Acute Abdomen Imaging Strategy
- Trauma Imaging: The FAST & Beyond
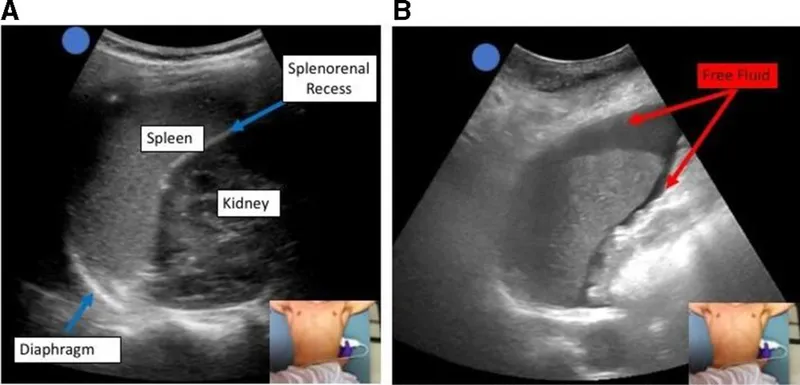
- FAST: Focused Assessment with Sonography for Trauma. Screens for pericardial effusion, intra-abdominal free fluid.
- eFAST: Extended FAST; adds lung views for pneumothorax/hemothorax.
- Pan-Scan CT: For hemodynamically stable patients with significant mechanism of injury.
- Suspected Vascular Obstruction
- Deep Vein Thrombosis (DVT): Doppler US is the first-line diagnostic test.
- Pulmonary Embolism (PE): CT Pulmonary Angiography (CTPA) is the gold standard.
⭐ In a hypotensive trauma patient, a positive FAST exam (free fluid) is a direct indication for an exploratory laparotomy, bypassing further imaging.
- Routine preoperative imaging is not recommended for asymptomatic patients in low-risk surgery.
- A baseline ECG is for patients >50 or with cardiac risk factors (HTN, DM, CAD).
- Chest X-rays are for new or unstable cardiopulmonary signs/symptoms, not routine screening.
- Always get a urine pregnancy test (hCG) in all females of childbearing potential.
- Cardiac stress testing is for high-risk surgery in patients with poor functional capacity (<4 METs).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

