Virchow's Triad - The Clotting Trinity
Three core factors that predispose to thrombosis. 📌 Mnemonic: SHE
- Stasis of Blood Flow
- Immobilization (post-op), prolonged travel
- Heart failure, atrial fibrillation, venous obstruction
- Hypercoagulability
- Malignancy (e.g., pancreatic, lung)
- Pregnancy, estrogen therapy
- Inherited thrombophilias (e.g., Factor V Leiden)
- Endothelial Injury
- Surgery, trauma, catheter placement
- Atherosclerosis, vasculitis
⭐ High-Yield: Factor V Leiden is the most common inherited cause of hypercoagulability in Caucasian populations, leading to resistance to activated protein C.
DVT Risk Factors - Spotting the Danger
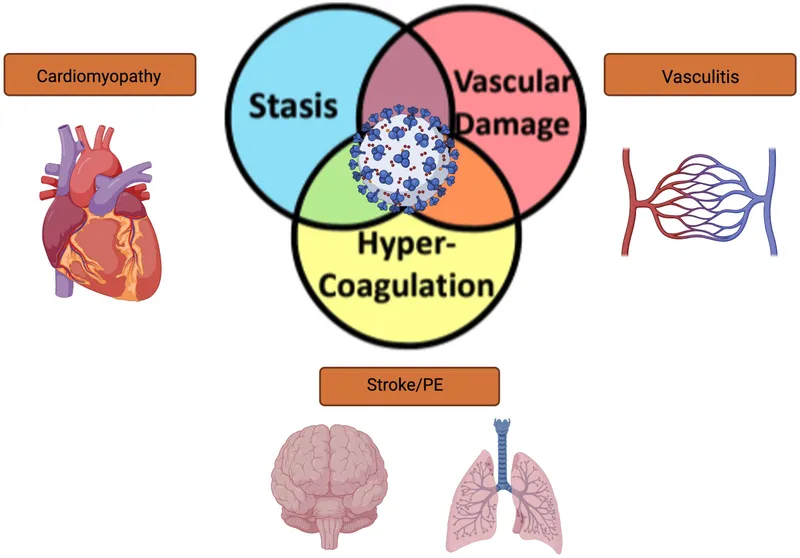
Risk is classically stratified by Virchow's Triad:
-
Venous Stasis
- Immobilization (post-op, paralysis, prolonged travel >4 hrs)
- Obesity (BMI >30)
- Heart failure (decompensated)
- Advanced age
-
Hypercoagulability
- Malignancy (especially pancreatic, lung, hematologic)
- Pregnancy & postpartum period (up to 6 weeks)
- Estrogen therapy (OCPs, HRT)
- Inherited thrombophilias (e.g., Factor V Leiden)
- Sepsis & inflammatory states
-
Endothelial Injury
- Surgery (highest risk: orthopedic, pelvic, major abdominal)
- Trauma (fractures, direct vessel injury)
- Central venous catheters
- Smoking
⭐ High-Yield: The single strongest predictor for developing a VTE is a personal history of a prior DVT or pulmonary embolism.
Caprini Score - Quantifying the Risk
A cumulative risk assessment model to estimate postoperative VTE risk and guide prophylaxis. Points are assigned for individual risk factors.
- 1 Point Factors
- Age 41-60 yrs, BMI >25, minor surgery, varicose veins, pregnancy/postpartum, OCP/HRT
- 2 Point Factors
- Age 61-74 yrs, major open surgery (>45 min), laparoscopic surgery (>45 min), bed rest >72 hrs
- 3 Point Factors
- Age ≥75 yrs, personal or family hx of VTE, Factor V Leiden, Prothrombin 20210A
- 5 Point Factors
- Elective major lower extremity arthroplasty, hip/pelvis/leg fracture, stroke (<1 mo), multiple trauma

| Score | Risk Level | Recommended Prophylaxis |
|---|---|---|
| 0-1 | Low | Early ambulation |
| 2 | Moderate | Mechanical (SCDs) |
| 3-4 | High | LMWH/LDUH ± Mechanical |
| ≥5 | Highest | LMWH/LDUH + Mechanical |
Risk-Based Prophylaxis - The Prevention Playbook
- Goal: Match prophylaxis intensity to patient's thrombotic risk using a validated model.
- Tool: Caprini Score for VTE Risk Assessment is a common standard.
⭐ Withhold LMWH for ≥12-24 hours before neuraxial anesthesia (e.g., epidural) and for >4 hours after catheter removal to minimize spinal hematoma risk.
- Pharmacologic Options:
- LMWH: Enoxaparin 40 mg SC daily.
- UFH: 5000 units SC q8-12h.
- Mechanical Options: Intermittent pneumatic compression (IPC) devices are superior to graduated compression stockings (GCS).
High-Yield Points - ⚡ Biggest Takeaways
- The Wells score is the key clinical tool to estimate pre-test probability of DVT.
- Major risk factors include prior VTE, active cancer, recent surgery or prolonged immobilization, and inherited thrombophilias.
- A negative D-dimer is highly effective at ruling out DVT in patients with a low Wells score.
- Compression ultrasonography is the first-line imaging test for confirming a DVT diagnosis.
- Pharmacologic prophylaxis (e.g., LMWH) is crucial in high-risk surgical patients.
- The Caprini score specifically tailors VTE prophylaxis recommendations for surgical patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

