PACU Admission - The First Five
Immediate assessment upon patient arrival from the OR. A structured handoff (e.g., SBAR) is crucial, followed by the primary survey.
📌 ABCDE Approach:
- Airway: Ensure patency; note any artificial airway.
- Breathing: Check respiratory rate, effort, and SpO₂ (goal >92%). Auscultate lungs.
- Circulation: Monitor BP, HR, and ECG. Assess peripheral pulses and temperature.
- Disability: Evaluate level of consciousness (e.g., GCS) and motor/sensory function.
- Exposure: Inspect surgical site for bleeding/hematoma. Check all drains, catheters, and IV lines.
⭐ The Aldrete Score is used to assess recovery after anesthesia. A score of ≥9 is typically required for discharge from PACU.
PACU Complications - Recovery Roadblocks
-
Airway & Breathing
- Hypoxemia ($SpO_2$ < 92%): Most common cause is atelectasis (tongue obstruction, laryngospasm).
- Management: Jaw thrust/chin lift, ↑ FiO2, positive pressure ventilation. Consider naloxone for opioid reversal.
- Hypoventilation (↑ $pCO_2$): Residual effects of anesthetics/opioids.
- Management: Stimulate patient, support ventilation, reverse agents.
- Hypoxemia ($SpO_2$ < 92%): Most common cause is atelectasis (tongue obstruction, laryngospasm).
-
Cardiovascular
- Hypotension (↓ SBP < 90 mmHg): Suspect hemorrhage first, then vasodilation.
- Management: IV fluid bolus, vasopressors (phenylephrine).
- Hypertension (↑ SBP > 180 mmHg): Pain, anxiety, bladder distension.
- Management: Treat cause (analgesia), IV labetalol or hydralazine.
- Hypotension (↓ SBP < 90 mmHg): Suspect hemorrhage first, then vasodilation.
-
Neurologic & Other
- Emergence Delirium: Common in kids & elderly. Rule out hypoxia.
- PONV (Post-Op Nausea/Vomiting): Treat with ondansetron.
- Hypothermia (< 36°C): Causes shivering, ↑ O2 demand. Use forced-air warmers.
⭐ High-Yield: In an unconscious PACU patient, the most common cause of airway obstruction is the tongue falling back and occluding the pharynx.
PACU Discharge - The Green Light
Discharge from the Post-Anesthesia Care Unit (PACU) hinges on physiologic stability. The Aldrete score is the primary tool used.
-
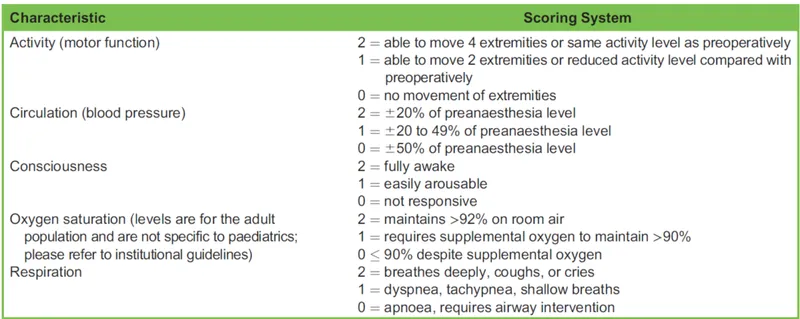
Aldrete Score Criteria: Assesses five key areas to determine recovery.
- Activity: Able to move 4 extremities voluntarily or on command.
- Respiration: Able to breathe deeply and cough freely.
- Circulation: Blood pressure ± 20% of pre-anesthetic level.
- Consciousness: Fully awake.
- O₂ Saturation: SpO₂ >92% on room air.
-
Discharge Threshold: A score of $ \ge 9 $ is typically required.
⭐ Patients must void within 6-8 hours post-op to rule out urinary retention, especially after spinal anesthesia.

High‑Yield Points - ⚡ Biggest Takeaways
- Airway patency is paramount; watch for laryngospasm and hypoventilation from residual anesthesia.
- Assess hemodynamic stability; hypotension may signal hemorrhage or anesthetic-induced vasodilation.
- Postoperative nausea and vomiting (PONV) is common; treat with antiemetics like ondansetron.
- Shivering and hypothermia are frequent; manage with forced-air warmers.
- Suspect malignant hyperthermia with unexplained tachycardia, hyperthermia, and muscle rigidity.
- The Aldrete score determines PACU discharge readiness, assessing key physiological parameters.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

