👶 Tiny Tummies, Big Trouble
📌 VACTERL association: Vertebral, Anal atresia, Cardiac, TracheoEsophageal fistula, Renal, Limb defects.
| Condition | Pathophysiology Pearl | Classic Presentation |
|---|---|---|
| CDH | Herniation (Bochdalek > Morgagni) → pulmonary hypoplasia. | Scaphoid abdomen, respiratory distress, bowel sounds in chest. |
| TEF | Failed foregut separation (Type C most common). | Choking/coughing with feeds, NG tube coils, gastric air bubble. |
| Gastroschisis / Omphalocele | G: Defect lateral to umbilicus, no sac. O: Midline defect, sac, associated anomalies. | Visible bowel (uncovered/covered). |
| Malrotation w/ Volvulus | Abnormal rotation → Ladd's bands, midgut volvulus. | Sudden bilious vomiting in a well-appearing neonate. |
| Duodenal Atresia | Failure of duodenal recanalization. | "Double bubble" sign on X-ray, bilious vomiting. |
| NEC | Ischemia & inflammation in premature infants. | Abdominal distension, bloody stools, pneumatosis intestinalis. |
⭐ ~30% of infants with duodenal atresia have Down syndrome (Trisomy 21). Conversely, ~5% of infants with Down syndrome have duodenal atresia.
🩺 Diagnosis - Peeking Inside Problems
- Initial Workup:
- Abdominal X-ray (AXR): First-line for any neonatal abdominal distress.
- Contrast Studies: Definitive for specific conditions.
- Pathognomonic Findings:
- CDH: Bowel loops in chest on CXR/AXR.
- TEF: Coiled NG tube in esophageal pouch.
- NEC: ⭐ Pneumatosis intestinalis (air in bowel wall).
- Hirschsprung: Transition zone on contrast enema.
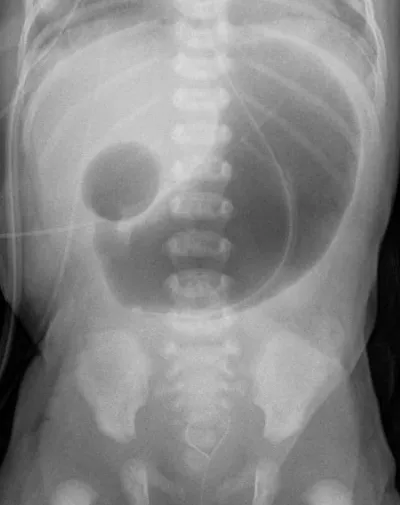
⭐ Bilious emesis in a neonate is malrotation with midgut volvulus until proven otherwise. This is a true surgical emergency requiring immediate evaluation with an upper GI series.
🔪 Management - Scalpels & Support
Initial stabilization is paramount before any surgical intervention.
- Malrotation w/ Volvulus: Emergent laparotomy for Ladd's procedure. Detorse bowel, lyse Ladd's bands, place cecum in LLQ, appendectomy.
- Congenital Diaphragmatic Hernia (CDH): Intubate, NG decompression. Delayed repair after cardiopulmonary stabilization (managing pulmonary hypertension).
- Gastroschisis: Cover bowel with sterile silo/wrap. Aggressive IV fluid resuscitation for massive losses. Staged surgical closure.
⭐ In CDH, avoid bag-mask ventilation. It insufflates the herniated bowel, worsening respiratory compromise by further compressing the hypoplastic lungs.
🚧 Complications - Post-Op Perils
- Short Gut Syndrome: After massive bowel resection (NEC, atresia, volvulus). Leads to malabsorption, TPN dependence, and cholestasis.
- Adhesions → SBO: A universal long-term risk following any neonatal laparotomy. Presents with bilious emesis and abdominal distension.
- GERD: Extremely common post-TEF repair due to esophageal dysmotility. Can cause strictures and recurrent aspiration.
- Neurodevelopmental Delay: Risk in severe cases (e.g., CDH, gastroschisis) from perinatal stress, hypoxia, or prolonged hospitalization.
⭐ Post-TEF repair, GERD is a near-universal complication, often requiring long-term management with PPIs or fundoplication.
⚡ Biggest Takeaways
- Bilious vomiting in a neonate is malrotation with volvulus until proven otherwise; diagnose with an upper GI series.
- Duodenal atresia presents with a "double-bubble" sign on X-ray and is strongly associated with Down syndrome.
- Necrotizing enterocolitis (NEC) in premature infants shows pneumatosis intestinalis (air in bowel wall).
- Congenital diaphragmatic hernia (CDH): Intubate immediately for respiratory distress; avoid bag-mask ventilation.
- Gastroschisis is a defect without a sac; omphalocele is midline and covered by a sac.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

