👶 Belly's Big Debut
Two major ventral wall defects from failed embryologic closure. The key difference is the presence or absence of a protective sac covering the herniated viscera.
| Feature | Gastroschisis | Omphalocele |
|---|---|---|
| Location | Right of umbilicus | Midline, through umbilicus |
| Covering | Absent; bowel exposed | Sac (amnion, peritoneum) |
| Cord | Normal abdominal insertion | Inserts onto the sac |
| Etiology | Vascular insult | Failure of gut to return |
| Anomalies | Rare; bowel atresia | Common (>50%); cardiac, trisomies |
👶 Pathology - Why It Pops Out
-
Omphalocele: Failure of lateral body wall folds to fuse.
- Herniation of abdominal contents through the umbilical ring.
- Contents are covered by a sac (peritoneum & amnion).
-
Gastroschisis: Full-thickness defect lateral to the umbilicus (usually right).
- Likely due to a vascular accident (e.g., involution of the right omphalomesenteric artery).
- Bowel herniates with no covering sac, exposed to amniotic fluid.
⭐ Omphalocele is a midline defect often associated with other midline defects (cardiac) and chromosomal abnormalities (Trisomies 13, 18).
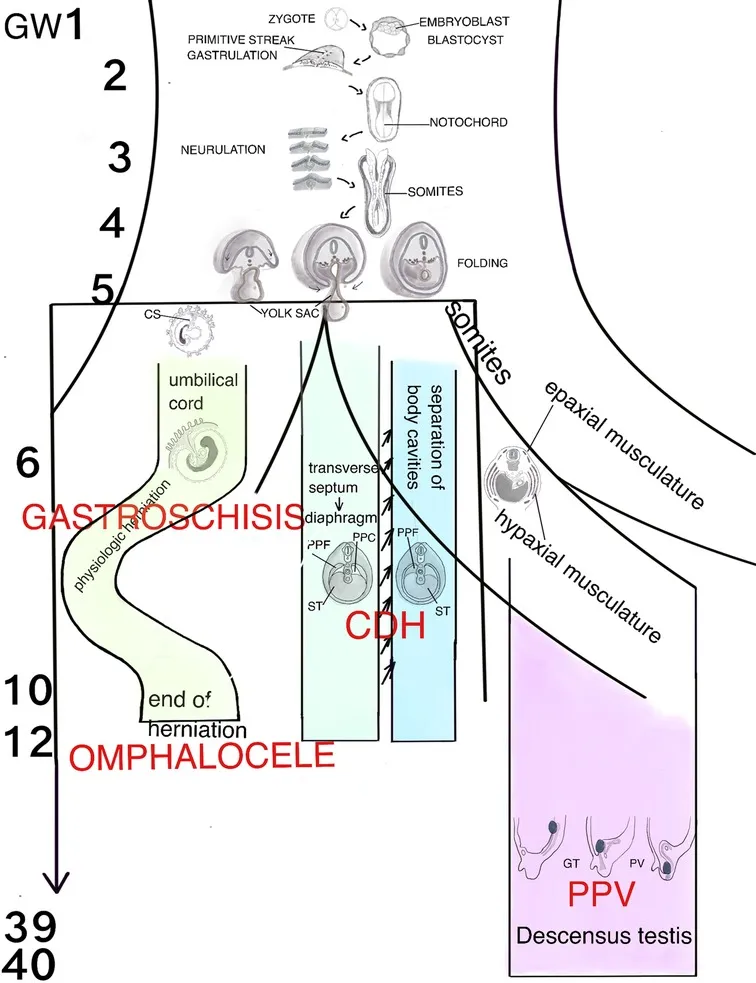
👶 Clinical Manifestations - The Great Divide
| Feature | Omphalocele | Gastroschisis |
|---|---|---|
| Location | Midline, failure of umbilical ring closure. Defect >4 cm. | Paraumbilical (right > left), likely vascular insult. Defect <4 cm. |
| Covering Sac | ✅ Present (amnion, peritoneum), shiny, gray. | ❌ Absent; bowel directly exposed to amniotic fluid. |
| Contents | Bowel, liver, spleen. | Usually only midgut loops, stomach. Liver is rare. |
| Cord Insertion | At the apex of the sac. | Normal, lateral to the defect. |
| Bowel Appearance | Protected, normal. | Inflamed, edematous, matted, thickened ("peel"). |
| Maternal AFP | ↑ | ↑↑ (significantly higher due to exposed bowel). |
| Associated Anomalies | Common (~50-70%); cardiac, trisomies (13, 18). | Rare (~10-15%); intestinal atresia/stenosis. |
🛠️ Management - The Fix-It Plan
Immediate Stabilization (Both):
- Cover defect with sterile, saline-soaked gauze & plastic wrap.
- IV fluids for resuscitation & broad-spectrum antibiotics.
- NG/OG tube for decompression.
- Maintain temperature in a radiant warmer.
Surgical Strategy: Goal is tension-free closure.
- Gastroschisis: Urgent repair. If primary closure isn't feasible, a silo is placed for staged reduction.
- Omphalocele: Repair after full anomaly workup. Staged repair or "paint and wait" technique for giant defects.
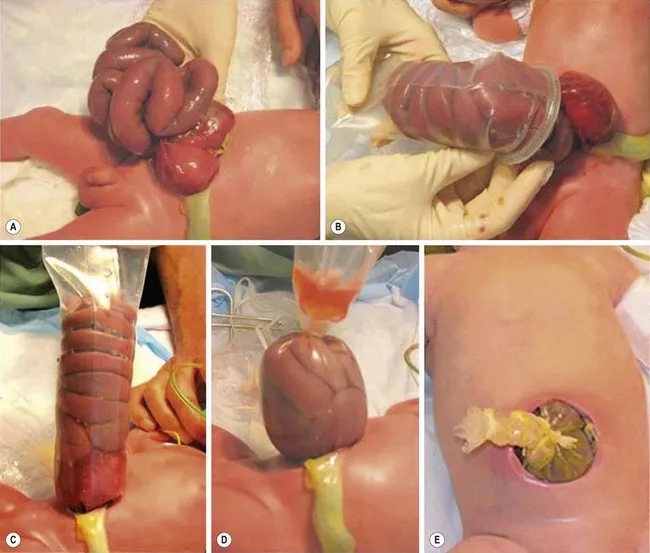
⭐ Gastroschisis is a surgical emergency due to exposed, inflamed bowel. Omphalocele repair is often delayed to evaluate for severe associated anomalies (e.g., cardiac defects, Beckwith-Wiedemann), which dictate overall prognosis.
⚡ Biggest Takeaways
- Gastroschisis is a full-thickness defect right of the umbilicus with no covering sac; bowel is exposed and inflamed.
- Omphalocele is a midline defect where herniated viscera (often including liver) are covered by a sac.
- Omphalocele is highly associated with other anomalies (cardiac, trisomies 13/18, Beckwith-Wiedemann).
- Gastroschisis is typically an isolated defect, resulting from a vascular accident.
- Both present with elevated maternal serum AFP.
- Initial management involves sterile wrapping, fluid resuscitation, and NG tube decompression.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

