💉 Why We Tap
LP is performed for both diagnostic and therapeutic reasons.
-
Diagnostic (CSF Analysis & Pressure)
- Infection: Suspected meningitis or encephalitis.
- Hemorrhage: Suspected subarachnoid hemorrhage (SAH) with a negative head CT.
- Inflammation: Multiple sclerosis (oligoclonal bands), Guillain-Barré syndrome (albuminocytologic dissociation).
- Malignancy: CNS lymphoma, leptomeningeal metastases.
- Pressure: Measure opening pressure (e.g., idiopathic intracranial hypertension [IIH]).
-
Therapeutic
- Relieve ↑ intracranial pressure (e.g., large volume tap in IIH).
- Administer intrathecal medications (e.g., chemotherapy, anesthetics, antibiotics).
⭐ In suspected SAH with a negative non-contrast head CT, an LP is the definitive next step to check for xanthochromia or RBCs.
⚠️ Clinical Correlations - Danger Zones
The primary risk of LP is iatrogenic cerebral herniation. Always assess for contraindications before proceeding.
| Absolute Contraindications | Relative Contraindications |
|---|---|
| • Infection at puncture site | • Coagulopathy (Platelets < 50,000/μL, INR > 1.5) |
| • Signs of ↑ ICP / mass lesion | • Severe spinal deformity |
| • Suspected spinal epidural abscess | • Brain abscess (risk of seeding) |
💉 The Needle's Path
- Positioning: Lateral decubitus (fetal position) or sitting upright, maximally flexed to open interspinous spaces.
- Landmark: A line connecting the superior iliac crests crosses the L4 spinous process.
- Insertion: L3-L4 or L4-L5 interspace. Needle with bevel up (parallel to dural fibers), angled slightly cephalad.
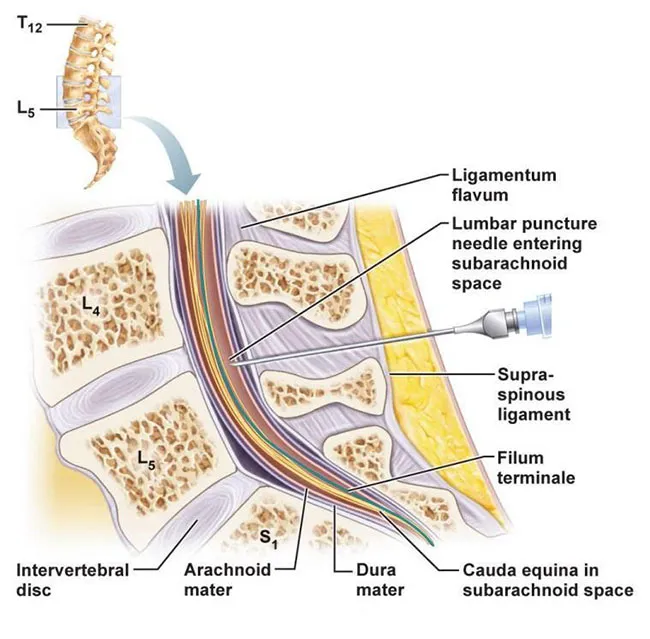
⭐ A distinct "pop" is felt as the needle pierces the ligamentum flavum and a second, finer pop for the dura-arachnoid membrane.
📌 Skinny Suzan Is Always Laying Down Asleep: Skin, Subcutaneous, Supraspinous, Interspinous, Ligamentum flavum, Dura, Arachnoid.
🧪 Diagnosis - Decoding the Fluid
Analyze CSF via 4 tubes: 1) Cell count/differential, 2) Gram stain/culture, 3) Glucose/protein, 4) Special tests (e.g., oligoclonal bands, VDRL). Classic findings differentiate key CNS pathologies.
| Condition | OP (cmH₂O) | WBC/μL (Diff) | Glucose (mg/dL) | Protein (mg/dL) |
|---|---|---|---|---|
| Bacterial | ↑↑ (>25) | ↑↑ (>1000, PMNs) | ↓↓ (<40) | ↑↑ (>200) |
| Viral | N/↑ (<25) | ↑ (<1000, Lymphs) | Normal | N/↑ (<150) |
| Fungal/TB | ↑ | ↑ (<500, Lymphs) | ↓ (<45) | ↑ (>150) |
| SAH | ↑ | ↑↑ RBCs | Normal | ↑ |
🤕 Complications - The Aftermath
- Post-LP Headache: Most common. Orthostatic (worse upright, better supine) from CSF leakage.
- Infection: Iatrogenic meningitis (rare).
- Bleeding: Epidural/subdural hematoma, esp. with coagulopathy.
- ⚠️ Herniation: Fatal risk if ↑ICP with a mass lesion.
⭐ Treat post-LP headache with bed rest, hydration, and caffeine; consider an epidural blood patch for severe, refractory cases.
⚡ Biggest Takeaways
- Insert needle at the L3/L4 or L4/L5 interspace (level of iliac crests); the spinal cord ends at L1-L2 in adults.
- Absolute contraindication: Signs of increased ICP (e.g., papilledema); risk of cerebral herniation. Get a CT head first if suspected.
- Key indications: Suspected meningitis, subarachnoid hemorrhage (SAH), Guillain-Barré syndrome, and multiple sclerosis.
- Needle pierces ligaments (ligamentum flavum gives a "pop"), dura, and arachnoid mater.
- Use the lateral decubitus position to accurately measure opening pressure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

