🧠 Pathophysiology - Brain Fluid Fiasco
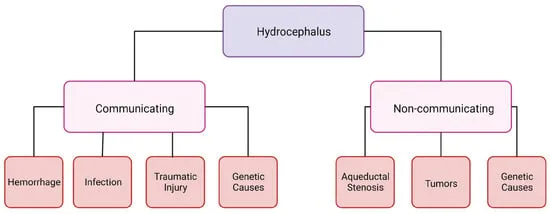
- Non-communicating (Obstructive): Blockage within the ventricular system prevents CSF from reaching the subarachnoid space.
- Causes: Aqueductal stenosis, tumors, intraventricular hemorrhage.
- Communicating: Impaired CSF reabsorption by arachnoid granulations; ventricles are in communication with the subarachnoid space.
- Causes: Post-meningitis scarring, subarachnoid hemorrhage (SAH) debris.
⭐ Acute hydrocephalus after SAH is often obstructive (blood clots), while chronic is communicating (impaired absorption).
🧠 Head Full of Trouble
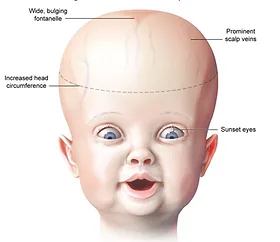
- Presentation varies dramatically by age, primarily due to skull suture fusion status. ↑ ICP drives symptoms.
| Feature | Infants (Open Sutures) | Children & Adults (Fused Sutures) |
|---|---|---|
| Head/ICP | Macrocephaly, bulging fontanelles | Headache (worse AM), papilledema |
| Eyes | "Sunsetting" eyes (tonic downward gaze) | 6th nerve palsy (lateral gaze deficit) |
| Function | Irritability, poor feeding, developmental delay | Gait instability, cognitive decline, lethargy |
- 📌 **Hakim's Triad: "Wet, Wobbly, Wacky"**
- Urinary incontinence, magnetic gait, dementia.
⭐ In NPH, gait disturbance is typically the first symptom to appear and the most likely to improve with CSF shunting.
🧠 Diagnosis - Spotting the Swell
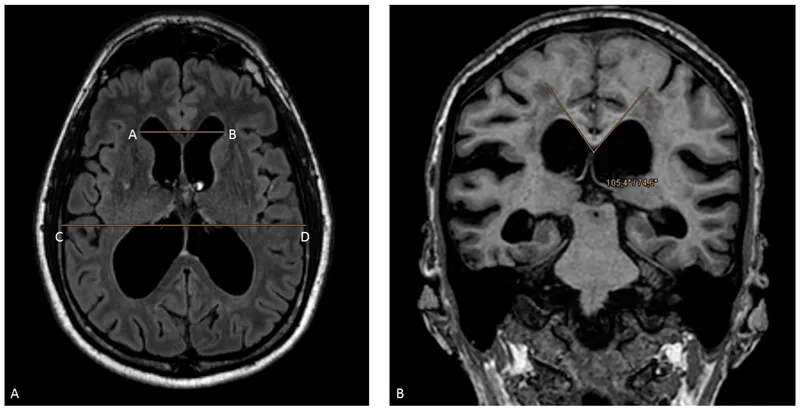
- Imaging (CT/MRI): First-line test shows ventriculomegaly.
- For Normal Pressure Hydrocephalus (NPH), calculate the Evan's Index.
- Evan's Index > 0.3 is diagnostic for NPH.
- $Evan's\ Index = \frac{Maximal\ Frontal\ Horn\ Width}{Maximal\ Internal\ Skull\ Diameter}$
- NPH Confirmation:
- 💡 High-Volume Lumbar Puncture (LP Tap Test): Remove 30-50 mL CSF.
- Transient improvement in gait/cognition predicts positive shunt response.
⭐ In NPH, ventriculomegaly is disproportionately large compared to sulcal effacement, distinguishing it from hydrocephalus ex vacuo (brain atrophy).
🧠 Management - Draining the Brain
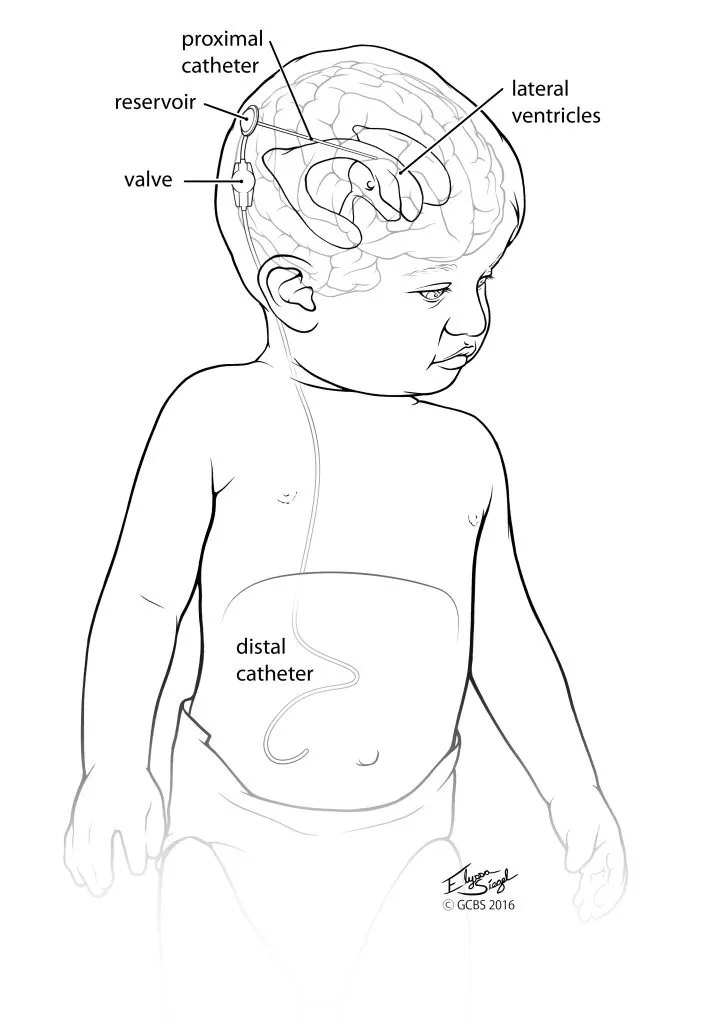
- Ventriculoperitoneal (VP) Shunt: The primary surgical treatment for most hydrocephalus types.
- A catheter drains excess CSF from a lateral ventricle through a one-way valve.
- The distal catheter is tunneled subcutaneously to the peritoneal cavity for CSF absorption.
- Endoscopic Third Ventriculostomy (ETV):
- Alternative for obstructive hydrocephalus (e.g., aqueductal stenosis).
- Creates a bypass by fenestrating the floor of the third ventricle, allowing CSF to flow directly into the interpeduncular cistern.
⭐ Shunt malfunction (obstruction, infection) is the most common complication. Infection risk is highest 1-3 months post-op, typically with Staphylococcus epidermidis.
⚠️ Complications - When Shunts Go South
- Infection: Most common within 6 months post-op.
- Causative organisms: Staphylococcus epidermidis (biofilm), S. aureus.
- Presents with fever, ↑ICP signs, shunt site erythema.
- Malfunction/Obstruction: Most common cause of shunt failure.
- Proximal (ventricular catheter) or distal (peritoneal) blockage.
- Presents with recurrent hydrocephalus symptoms.
- Overdrainage: Excessive CSF removal.
- Leads to slit ventricle syndrome (postural headaches).
- Risk of subdural hematomas from torn bridging veins.
⭐ Shunt infection within the first few months is almost always due to skin flora (S. epidermidis) introduced during surgery.
⚡ Biggest Takeaways
- Normal Pressure Hydrocephalus (NPH) presents with the classic triad: "wet, wobbly, and wacky" (incontinence, ataxia, dementia).
- CT/MRI is the initial diagnostic test, showing ventriculomegaly. NPH diagnosis is supported by improvement after a high-volume LP.
- Ventriculoperitoneal (VP) shunt is the definitive treatment for most forms of hydrocephalus.
- Key shunt complications include infection (S. epidermidis), obstruction, and overdrainage (subdural hematoma).
- In infants, suspect hydrocephalus with a rapidly increasing head circumference, bulging fontanelle, and sunset eyes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

