🧠 Clinical - Why Open the Box?
Craniotomy is indicated for accessing intracranial structures to treat pathology.
- Tumor Resection:
- Primary (glioma) or metastatic brain tumors.
- Benign tumors (meningioma) causing mass effect.
- Traumatic Brain Injury (TBI):
- Evacuation of space-occupying hematomas (epidural, subdural).
- Decompressive craniectomy for refractory intracranial pressure (↑ICP).
- Vascular Lesions:
- Clipping of cerebral aneurysms.
- Resection of arteriovenous malformations (AVMs).
- Infection:
- Drainage of brain abscesses or subdural empyema.
⭐ An epidural hematoma (EDH) with neurological decline, pupillary changes, or volume >30 cm³ requires emergent craniotomy and evacuation, especially following a "lucid interval."
🗺️ Anatomy - Skull's Surgical Atlas
Key Surgical Landmarks (Craniometric Points):
- Pterion: "H"-shaped junction of frontal, parietal, temporal, & sphenoid bones; weakest point of the skull.
- Bregma: Junction of coronal & sagittal sutures; site of anterior fontanelle.
- Lambda: Junction of sagittal & lambdoid sutures; site of posterior fontanelle.
- Asterion: Junction of lambdoid, occipitomastoid, & parietomastoid sutures; key for retrosigmoid approach.
- Stephanion: Junction of coronal suture & superior temporal line.
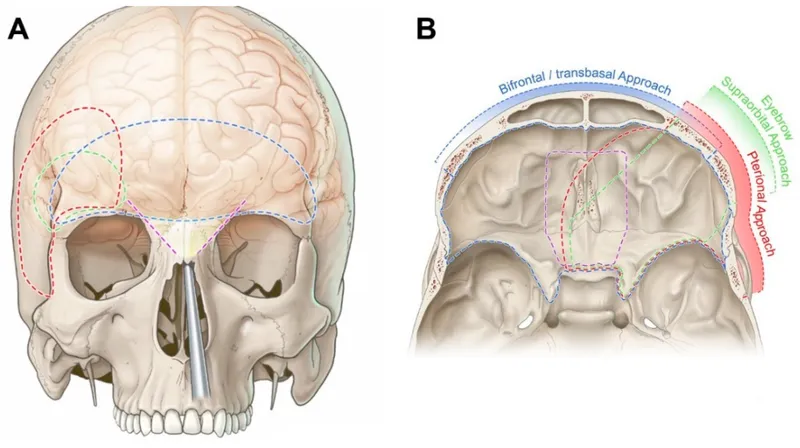
Common Surgical Approaches & Targets:
- Pterional: "Workhorse" approach for Circle of Willis aneurysms, suprasellar tumors.
- Retrosigmoid/Suboccipital: Cerebellopontine Angle (CPA) tumors (e.g., acoustic neuroma).
- Bifrontal: Anterior skull base tumors (e.g., olfactory groove meningioma).
- Transsphenoidal: Pituitary adenomas (via nasal cavity).
⭐ Pterion fracture is a neurosurgical emergency. It can lacerate the underlying anterior division of the middle meningeal artery, leading to a life-threatening epidural hematoma.
🛠️ Clinical - The Neurosurgeon's Toolkit
A craniotomy is a surgical procedure where a bone flap is temporarily removed from the skull to access the brain.
- Positioning: Patient's head is immobilized using a Mayfield clamp (3-pin skull fixation).

- Access:
- An incision is made, and a scalp flap is reflected.
- Burr holes are drilled into the skull.
- A craniotome (foot-plated drill) connects the burr holes to create the bone flap.
- Exposure & Closure:
- The dura mater is opened (C-shaped flap) and later closed (watertight).
- The bone flap is replaced using titanium plates and screws.
⭐ Pearl: The base of the C-shaped dural flap is typically oriented towards major venous sinuses (e.g., superior sagittal sinus) to preserve venous drainage and reduce bleeding risk.
⚠️ Complications - Post-Op Pitfalls
-
Immediate (Hours-Days)
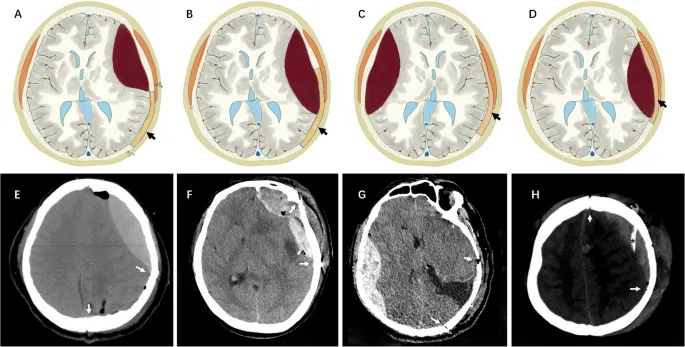
- Hemorrhage (EDH, SDH, IPH): Presents with new focal deficits or ↓LOC. Requires urgent CT scan.
- Cerebral Edema: Worsening neuro status. Manage with steroids, osmotherapy.
- Ischemic Stroke: From direct vessel injury or vasospasm.
-
Early (Days-Weeks)
- CSF Leak: Clear rhinorrhea/otorrhea (test for β-2 transferrin), postural headache.
- Meningitis: Fever, nuchal rigidity, altered mental status.
- Seizures: Prophylaxis is common (e.g., levetiracetam).
- VTE (DVT/PE): High risk due to immobility.
-
Late (Weeks-Months)
- Hydrocephalus: Impaired CSF absorption/flow.
- Syndrome of the Trephined: Sunken flap with neuro decline; cranioplasty is curative.
⭐ Post-op fever workup: Rule out non-neuro causes first (wind, water, wound, walking, wonder drugs). If negative, consider meningitis/ventriculitis; obtain CSF if safe.
⚡ Biggest Takeaways
- Craniotomy involves removing and replacing a bone flap for definitive treatment of tumors, hematomas, or vascular lesions.
- Craniectomy is removal of the bone flap without immediate replacement, primarily for decompression in severe TBI or malignant stroke.
- The pterional approach is a workhorse for anterior circulation aneurysms (e.g., ACoA, PCoA) and suprasellar tumors.
- The suboccipital approach provides access to the posterior fossa (cerebellum, brainstem).
- Major risks include post-operative hematoma, infection, seizures, and new neurological deficits.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

