🔭 Core concept - The Inner Tube
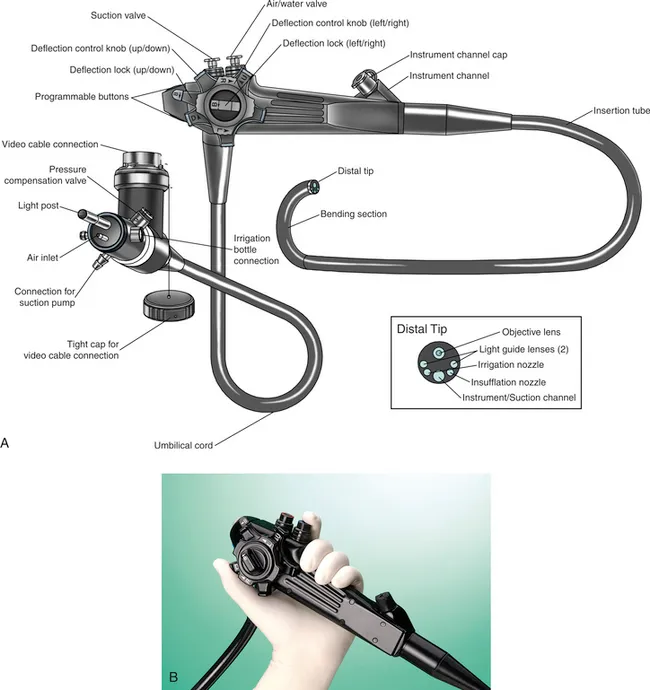
- Endoscopy: Visualizing internal organs using an endoscope, a tube with a light source and camera.
- Purpose: Diagnostic (e.g., biopsy) and therapeutic (e.g., polypectomy, stenting).
- Types:
- Flexible: Navigates tortuous lumens (GI tract, bronchi).
- Rigid: Superior optics, larger working channels for straight-access procedures (laparoscopy, arthroscopy).
- Key Components:
- Light source & camera/lens system.
- Working channel(s) for instruments.
- Insufflation/irrigation channels.
⭐ Perforation is a feared complication of any endoscopic procedure, especially during therapeutic interventions. It often presents with acute pain, fever, and signs of peritonitis.
🩺 Clinical manifestations - Scope on Demand
Endoscopy is performed for both diagnostic evaluation and therapeutic intervention based on clinical presentation. The decision pathway often follows initial assessment of symptoms and risk factors.
⭐ In patients with new-onset dyspepsia, endoscopy is indicated for age >60 or presence of alarm features: unintentional weight loss, persistent vomiting, dysphagia, odynophagia, palpable mass, or iron deficiency anemia.
🔧 Management - Fix-It Flex
- Gastrointestinal (GI) Interventions:
- EGD: Banding esophageal varices, dilating strictures, placing stents for malignancy, percutaneous endoscopic gastrostomy (PEG) for feeding.
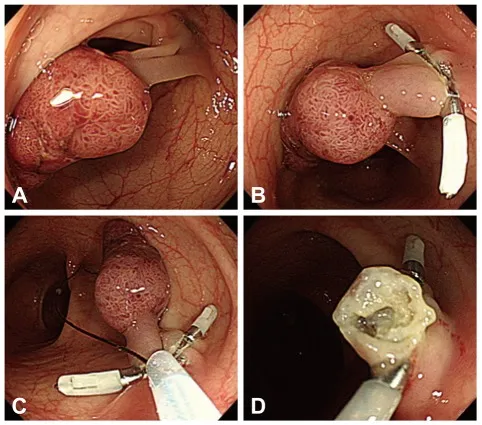
- Colonoscopy: Polypectomy prevents colorectal cancer. Hemostasis via clips, thermal coagulation (e.g., APC), or injection.
- ERCP: Biliary sphincterotomy, stone extraction from CBD, stenting for benign/malignant strictures.
- Other Systems:
- Bronchoscopy: Airway stenting, foreign body removal, tumor ablation.
- Cystoscopy: Ureteral stenting, lithotripsy/stone removal, transurethral resection of bladder tumor (TURBT).
⭐ Post-ERCP pancreatitis is the most common complication. Prophylactic rectal NSAIDs (e.g., indomethacin) can significantly decrease incidence.
🕵️ Diagnosis - The Inside Scoop
- Direct Visualization: Real-time assessment of mucosal surfaces for inflammation, ulcers, polyps, and masses.
- Tissue Sampling (Definitive Dx):
- Biopsy: Forceps obtain tissue for histopathology (e.g., cancer, H. pylori, celiac disease). The gold standard for many conditions.
- Cytology: Brushings collect cells for analysis.
- Advanced Imaging Modalities:
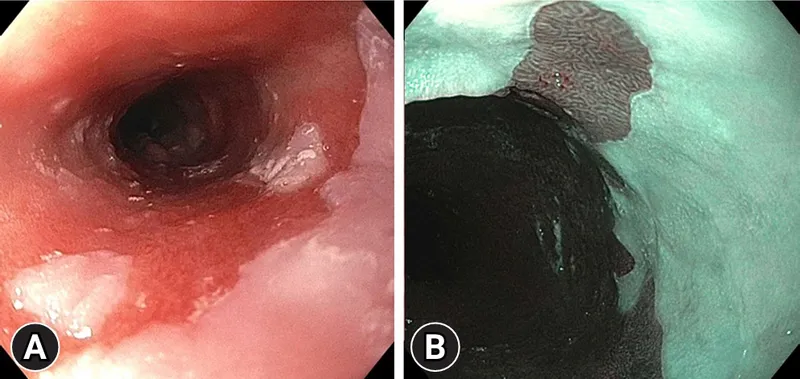
- Narrow-Band Imaging (NBI): Enhances mucosal and vascular patterns to better identify dysplasia.
- Endoscopic Ultrasound (EUS): Assesses depth of tumor invasion and evaluates adjacent lymph nodes.
⭐ EUS is critical for locoregional staging (T & N stages) of esophageal, gastric, and rectal cancers, guiding neoadjuvant therapy.
⚠️ Complications - Perilous Probes
- Perforation: Most feared. Risk ↑ with therapeutic interventions. Presents with acute pain, fever, peritonitis, subcutaneous emphysema.
- Bleeding: Immediate or delayed (up to 2 weeks). Manage with endoscopic clips, cautery, or angiography.
- Infection: Transient bacteremia is common; sepsis is rare. Prophylaxis for high-risk cases.
- Sedation-related: Aspiration, hypotension, hypoxia.
- Post-polypectomy Syndrome: Transmural burn without frank perforation; manage conservatively with bowel rest and antibiotics.
⭐ Perforation of retroperitoneal structures (e.g., duodenum) may cause back/flank pain and retroperitoneal air on CT, lacking classic peritonitis.
⚡ Biggest Takeaways
- Endoscopy has dual roles: diagnostic (visualization, biopsy) and therapeutic (polypectomy, stenting, hemostasis).
- Key procedures: EGD (upper GI), colonoscopy (lower GI), ERCP (biliary/pancreatic), bronchoscopy (airways).
- Major complications are perforation, bleeding, infection, and sedation-related cardiopulmonary events.
- Post-ERCP pancreatitis is a classic, high-yield complication.
- Adequate bowel preparation is critical for a successful colonoscopy.
- Pre-procedure management of anticoagulants is vital to mitigate bleeding risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

