✂️ Clinical - Fertility-Sparing Fibroid Fix
-
Goal: Excise leiomyomas, preserving the uterus for future fertility.
-
Indications: Symptomatic fibroids (abnormal uterine bleeding, bulk symptoms, recurrent pregnancy loss) in women desiring pregnancy.
-
Pre-op: GnRH agonists (e.g., leuprolide) can ↓ fibroid size and correct anemia.
-
Surgical Approach Decision:
-
Key Risks: Hemorrhage, adhesions.
⭐ Counsel on ↑ risk of uterine rupture during future labor. Cesarean delivery is strongly recommended if the uterine cavity was entered.
🗺️ Anatomy - Location, Location, Location!
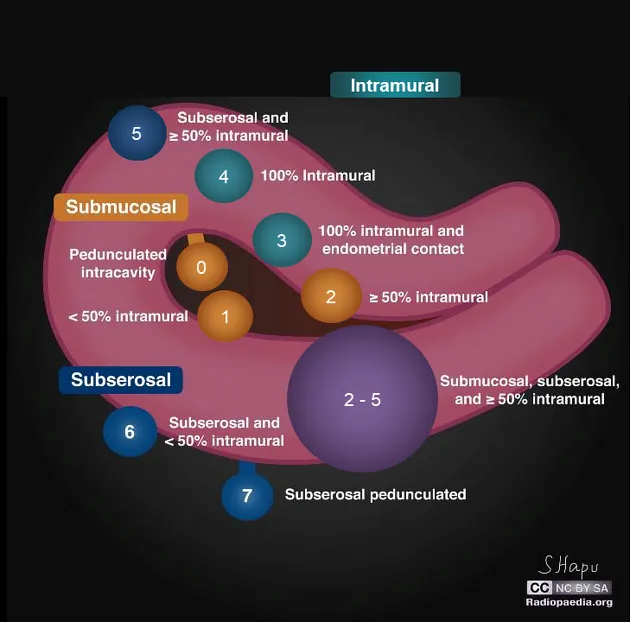
A fibroid's (leiomyoma) location is the key determinant for choosing the surgical approach. The FIGO classification system provides a detailed map.
- Submucosal (FIGO 0-2): Protrude into the uterine cavity. Ideal for hysteroscopic resection.
- Intramural (FIGO 3-5): Contained within the myometrium. Often require laparoscopy or laparotomy.
- Subserosal (FIGO 6-7): Protrude from the external uterine surface. Amenable to laparoscopy or laparotomy.
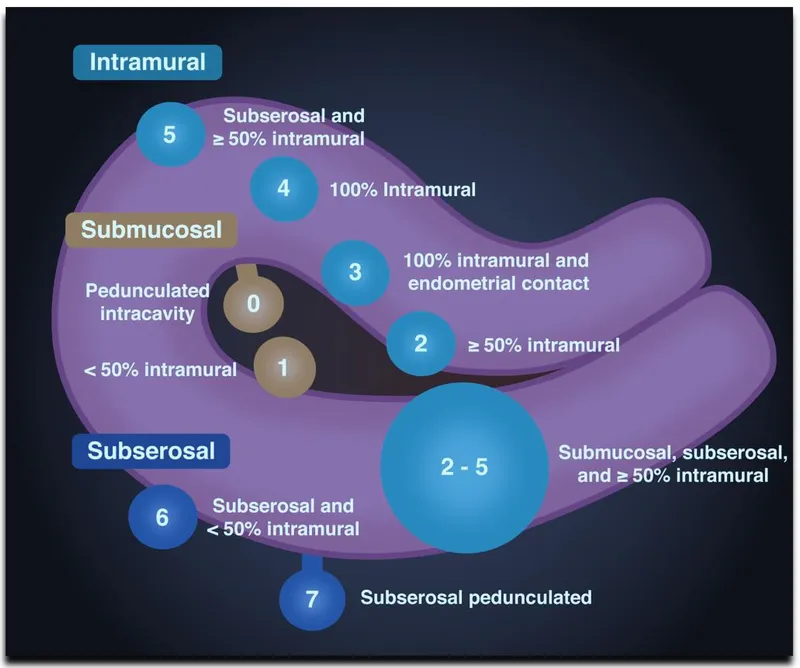
⭐ Submucosal fibroids are most implicated in heavy menstrual bleeding (menorrhagia) and impaired fertility (infertility, recurrent pregnancy loss) due to endometrial cavity distortion.
🔪 Surgical Strategy Selection
- Primary Goal: Symptom relief (e.g., bleeding, bulk symptoms) while preserving the uterus for patients desiring future fertility.
- The surgical approach is tailored based on fibroid size, number, and location (FIGO classification).
- Hysteroscopic: Ideal for intracavitary lesions causing abnormal uterine bleeding. Outpatient, low morbidity.
- Laparoscopic/Robotic: Minimally invasive for subserosal/intramural types. Requires skilled suturing for multi-layer closure to ensure uterine integrity.
- Abdominal (Laparotomy): Gold standard for very large (>10 cm), numerous, or difficult-to-access fibroids. Allows for optimal uterine reconstruction but has higher morbidity (blood loss, adhesions, longer recovery).
⭐ High-Yield: Any myomectomy that breaches the uterine cavity or requires deep myometrial incision (laparoscopic or abdominal) increases the risk of uterine rupture in subsequent pregnancies. This often necessitates a planned Cesarean delivery.
⚠️ Complications - Post-Op Perils
-
Intra-op & Early Post-op:
- Hemorrhage: Most common. Requires meticulous hemostasis (e.g., vasopressin, tourniquets).
- Organ Injury: Bladder, ureter, bowel.
- Hysteroscopy-Specific: Fluid overload (hyponatremia), uterine perforation, gas embolism.
-
Delayed & Long-term:
- Adhesion Formation: Can cause chronic pain, infertility, small bowel obstruction. Risk varies by surgical approach.
- Infection: Endometritis, pelvic cellulitis, abscess.
- Uterine Rupture in Future Pregnancy: Critical risk, especially with deep intramural incisions.
⭐ Counsel patients on planned Cesarean delivery for subsequent pregnancies, typically at 36-37 weeks, to avoid labor and potential rupture.
- Undiagnosed Sarcoma: Risk of morcellating an occult leiomyosarcoma (~1 in 350).
⚡ Biggest Takeaways
- Myomectomy is the uterus-sparing surgery for symptomatic fibroids in women desiring fertility preservation.
- Procedure choice depends on fibroid location: hysteroscopic (submucosal), laparoscopic (intramural/subserosal), or abdominal (large/multiple).
- The most feared long-term complication is uterine rupture during a future pregnancy.
- Patients require counseling on the high likelihood of needing a cesarean section for future deliveries.
- Major risks include intraoperative hemorrhage and postoperative fibroid recurrence.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

