✂️ Indications - Why We Cut
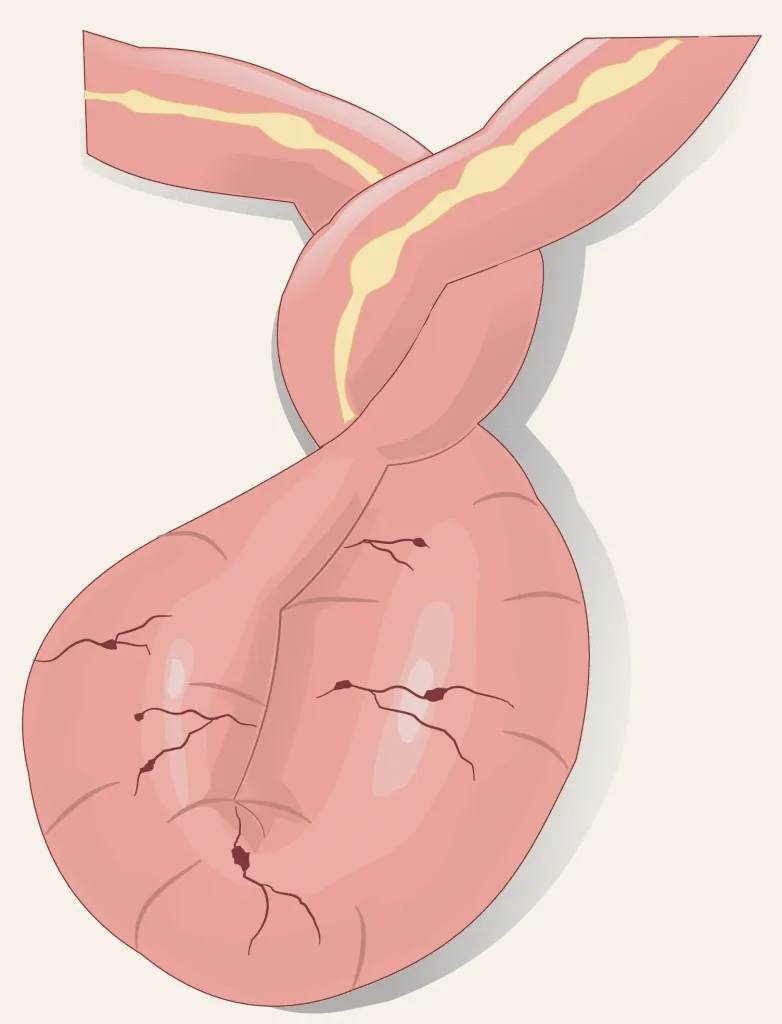
- Obstruction: Irreducible blockage from adhesions, incarcerated hernias, tumors, or volvulus.
- Ischemia/Infarction: Compromised blood supply from mesenteric events (thrombosis/embolism) or strangulation (hernia, volvulus), leading to necrosis.
- Perforation/Fistula: Bowel wall disruption from trauma, foreign bodies, or complicated inflammatory bowel disease (e.g., Crohn's).
- Neoplasm: Resection of malignant (adenocarcinoma, carcinoid) or symptomatic benign tumors.
- Hemorrhage: Uncontrolled bleeding refractory to endoscopic or angiographic intervention.
⭐ Crohn's Disease: Surgery is for complications (stricture, fistula, abscess), not a cure. Resect with minimal margins to preserve bowel length.
🩺 Pre-operative Evaluation - Sizing Up The Job
- Clinical Assessment: H&P for peritonitis (rebound, guarding), dehydration, and history of prior abdominal surgeries (adhesions).
- Laboratory Studies:
- CBC (leukocytosis), CMP (electrolyte abnormalities, renal function).
- ⚠️ Lactate: Crucial marker for bowel ischemia.
- Imaging:
- CT A/P with IV/PO contrast is the gold standard.
- Identifies transition point, etiology, and complications (e.g., ischemia, perforation).
- Patient Optimization: IV fluid resuscitation, NGT decompression, electrolyte correction, and pre-operative antibiotics.
⭐ A rising lactate or new metabolic acidosis in a patient with a small bowel obstruction strongly suggests bowel ischemia, warranting urgent surgical exploration.
✂️ Surgical Technique - The Snip & Stitch
- Core Principles: Create a tension-free, well-vascularized, and watertight connection.
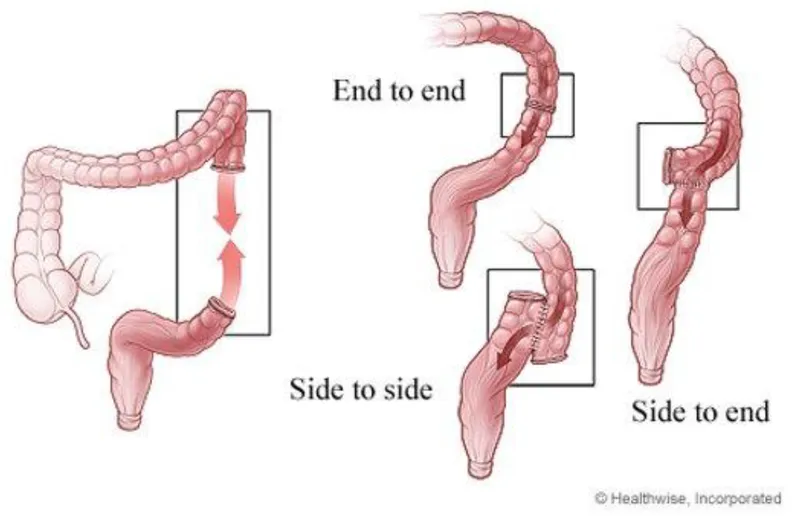
- Anastomosis Types:
- End-to-End: Most common; joins two open ends.
- Side-to-Side: Creates a large opening; often used in bypass (e.g., ileocolic).
- End-to-Side: Connects the end of one segment to the side of another.
- Methods:
- Hand-sewn: Single or double-layer closure.
- Stapled: Faster, uses linear or circular staplers.
⭐ High-Yield: The single most critical factor for a successful, leak-free anastomosis is adequate blood supply to both bowel ends. Ischemia is the enemy.
⚠️ Always close the mesenteric defect to prevent future internal hernias.
💥 Complications - When Seams Split
- Anastomotic Leak: Most feared complication.
- Timing: Peaks post-op day 5-7.
- Presentation: Fever, tachycardia, abdominal pain, prolonged ileus, ↑WBC. Can progress to peritonitis and sepsis.
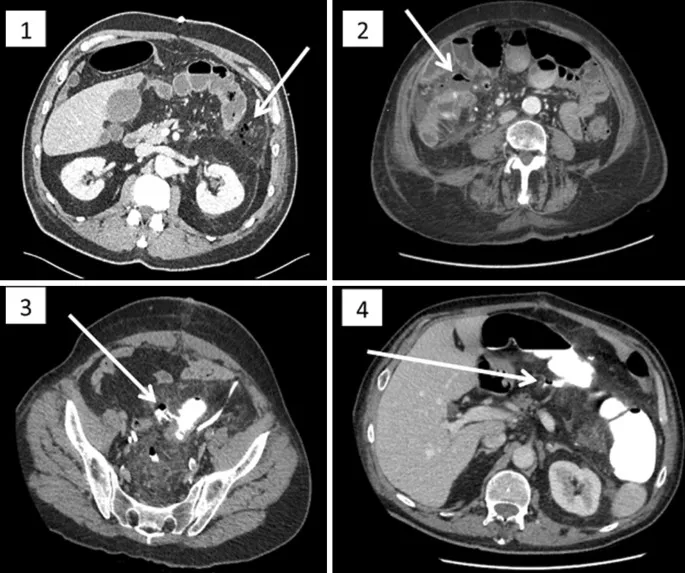
- Diagnosis: Abdominal CT with oral/IV contrast is the gold standard. Look for extraluminal air or contrast extravasation.
- Management: Guided by patient stability.
⭐ Anastomotic leak classically presents on post-op days 5-7, coinciding with the phase of maximal collagenolysis and minimal tensile strength at the suture line.
- Other Complications:
- Bleeding: Early complication from the staple/suture line.
- Stricture: Late complication due to fibrosis, causing obstructive symptoms.
🛣️ Post-operative Care - The Recovery Road
- Initial Management: NPO, IV fluids, pain control (e.g., PCA), DVT prophylaxis (LMWH, SCDs).
- Key Goal: Promote return of bowel function. Early ambulation is crucial.
- Diet Advancement: Guided by clinical signs (flatus, bowel sounds).
⭐ Physiologic Ileus: Expected for 2-3 days. Characterized by absent flatus/stool but minimal pain/distention. Prolonged ileus (>3-5 days) or signs of SBO (e.g., bilious emesis) requires imaging.

⚡ Biggest Takeaways
- Primary indications include ischemia, complicated Crohn's disease, SBO with strangulation, and malignancy.
- Anastomotic leak is the most feared complication, typically presenting on post-op day 5-7 with fever, tachycardia, and pain.
- Prolonged post-op ileus (>5 days) warrants imaging to rule out mechanical obstruction.
- Short bowel syndrome (<200 cm remaining bowel) causes severe malabsorption, often requiring TPN.
- Terminal ileum resection specifically causes vitamin B12 deficiency and impaired bile salt reabsorption.
- A tension-free, well-perfused anastomosis is critical to prevent ischemia and leaks.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

