🗺️ Anatomy - The Back Passage Basics
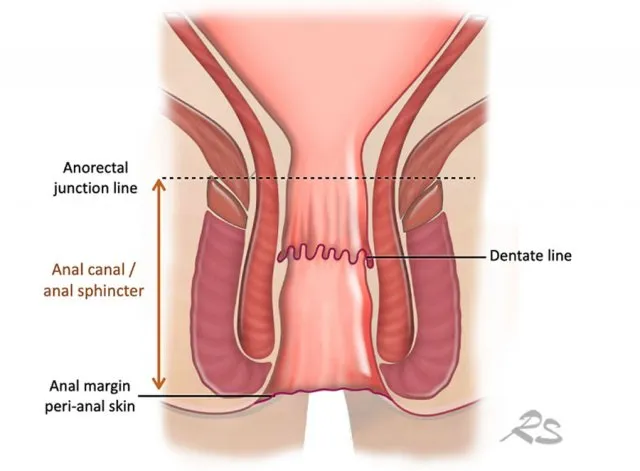
- Anal Canal: ~4 cm long, from anorectal ring to anal verge.
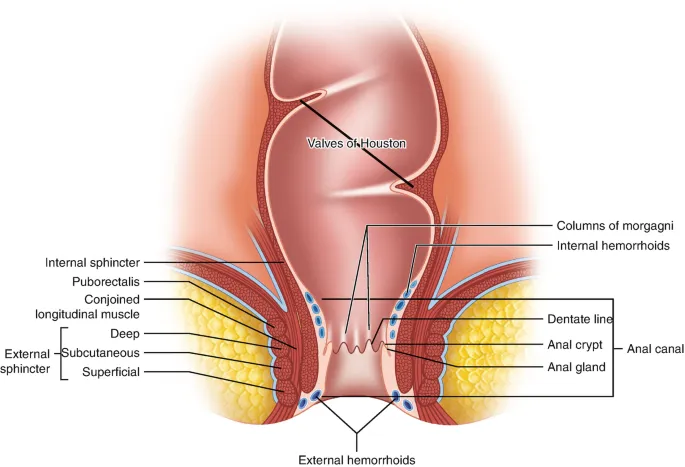
- Sphincters:
- Internal (IAS): Involuntary, smooth muscle (autonomic).
- External (EAS): Voluntary, striated muscle (Pudendal n. S2-S4). 📌 S2,3,4 keeps the poop off the floor.
- Dentate (Pectinate) Line: Critical anatomical landmark.
- Above: Columnar epithelium, visceral innervation (painless), superior rectal a./v. (portal drainage), internal iliac nodes.
- Below: Squamous epithelium, somatic innervation (painful), inferior rectal a./v. (caval drainage), superficial inguinal nodes.
⭐ The dentate line dictates symptoms and metastatic spread. Lesions above are typically painless with drainage to internal iliac nodes; lesions below are painful and drain to superficial inguinal nodes.
🩺 Pathology - Common Anal Woes
-
Hemorrhoids: Dilated submucosal vessels. Risks: straining, constipation, pregnancy.
Type Location Innervation Symptoms Internal Above dentate line Visceral (ANS) Painless, bright red bleeding, prolapse External Below dentate line Somatic Painful, pruritus; severe pain if thrombosed -
Anal Fissure: Longitudinal tear in anoderm, distal to dentate line.
- 90% at posterior midline (↓ blood flow).
- Severe, tearing pain with defecation; blood on tissue.
- Chronic triad: fissure, sentinel pile (skin tag), hypertrophied anal papilla.
⭐ An anal fissure located off the midline (e.g., lateral) is a red flag for underlying pathology like Crohn's disease, HIV, TB, or malignancy.
-
Anorectal Abscess & Fistula:
- 📌 Goodsall's Rule: Anterior-opening fistulas track straight; posterior-opening fistulas track in a curved path to the posterior midline.
✂️ Clinical - Snips, Bands, and Drains
-
Hemorrhoids (Bands): Rubber Band Ligation (RBL)
- Indication: Symptomatic internal hemorrhoids (Grades I-III).
- Procedure: An elastic band is placed at the base of the hemorrhoid (above the dentate line) → ischemic necrosis → sloughing in 7-10 days.
- Complications: Pain (if placed too low), bleeding, thrombosis, pelvic sepsis (rare).
-
Anal Fissure (Snips): Lateral Internal Sphincterotomy (LIS)
- Indication: Chronic anal fissure refractory to medical management (e.g., nifedipine, diltiazem).
- Procedure: Controlled division of the internal anal sphincter to ↓ resting pressure and ↑ blood flow, promoting healing.
- Complication: Minor fecal incontinence (flatus > stool) in up to 5% of patients.
-
Anorectal Abscess (Drains): Incision & Drainage (I&D)
- Indication: Acutely painful, fluctuant perianal/ischiorectal mass.
- Procedure: Urgent drainage, often with a cruciate incision.
- Sequela: High rate (~50%) of subsequent fistula-in-ano formation.
⭐ Post-hemorrhoidectomy urinary retention is the most common immediate complication. Severe, deep-seated pain days later suggests an evolving abscess or pelvic sepsis.
Hemorrhoid Management Algorithm
⚡ Biggest Takeaways
- Anal fissures failing medical therapy need lateral internal sphincterotomy (risk: incontinence).
- Excise thrombosed external hemorrhoids if <72 hours; use rubber band ligation for internal hemorrhoids.
- Anorectal abscesses require prompt incision and drainage; they often precede a fistula-in-ano.
- Treat simple fistulas with fistulotomy; use a Seton for complex cases (Crohn's, high) to preserve sphincter function.
- Full-thickness rectal prolapse (concentric rings) requires surgical rectopexy.
- Pilonidal abscess needs I&D; chronic disease requires excision of sinus tracts.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

