🔬 Keyhole Endocrine Intro
- Principle: Accessing endocrine glands (thyroid, parathyroid, adrenal) via small, remote incisions, avoiding large neck or abdominal wounds.
- Core Advantages: ↓ post-op pain, ↓ blood loss, shorter hospital stay, and superior cosmesis compared to traditional open surgery.
- Common Procedures:
- Minimally Invasive Parathyroidectomy (MIP)
- Endoscopic Thyroidectomy (transoral, axillary approaches)
- Laparoscopic/Robotic Adrenalectomy
- Tools: Endoscopes, specialized long instruments, and robotic platforms (e.g., da Vinci).
⭐ Precise preoperative localization (e.g., Sestamibi scan, 4D-CT, ultrasound) is paramount for the success of minimally invasive approaches, especially for parathyroid adenomas.
🔪 Management - Thyroid's Tiny Tuck
-
Minimally Invasive Thyroidectomy (MIT): Techniques using small or hidden incisions for improved cosmesis and potentially faster recovery compared to conventional open surgery.
-
Key Selection Criteria:
- Benign nodules or low-risk differentiated thyroid cancer
- Maximum nodule diameter < 3-4 cm
- Thyroid lobe volume < 30-40 mL
- No prior neck surgery or radiation
- No extrathyroidal extension or lymph node metastases
-
Common Approaches:
- MIVAT: Minimally invasive video-assisted; small central neck incision.
- TOETVA: Transoral endoscopic; no visible neck scar.
- Transaxillary: Through an armpit incision.
⭐ TOETVA (Transoral Endoscopic Thyroidectomy Vestibular Approach) is a truly "scarless" neck surgery, accessing the thyroid via incisions inside the lower lip.
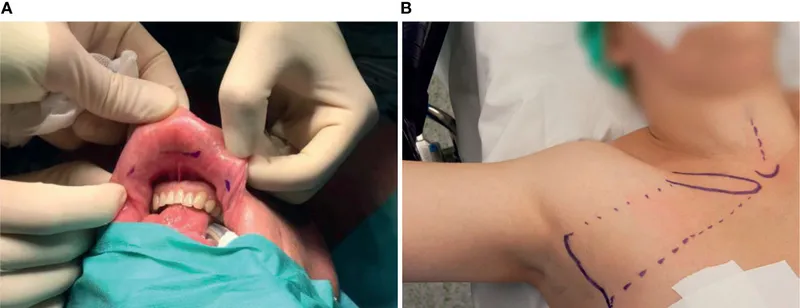
🎯 Management - Parathyroid Pinpointing
Preoperative localization is key for minimally invasive parathyroidectomy (MIP), targeting a single adenoma (~85% of cases).
-
Primary Localization Studies:
- Neck Ultrasound (US): High sensitivity for cervical glands; operator-dependent.
- Sestamibi Scan (⁹⁹ᵐTc): Functional scan; detects hyperfunctioning tissue, including ectopic glands. Often fused with SPECT/CT.
-
Localization Algorithm:
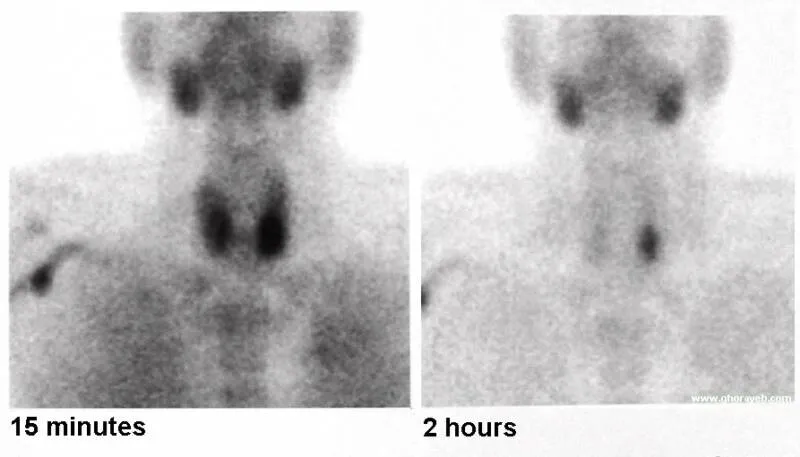
⭐ Intraoperative PTH (ioPTH) Monitoring: Confirms successful resection. A >50% drop from baseline 10 minutes post-excision indicates cure (Miami criterion).
🥷 Adrenal's Stealth Removal
- Laparoscopic Adrenalectomy (LA): Gold standard for most benign, functioning adrenal tumors (Conn's, Cushing's) and pheochromocytomas, typically < 6-8 cm.
- Approaches:
- Transperitoneal (TLA): Standard anterior approach; excellent visualization.
- Posterior Retroperitoneoscopic (PRA): Direct posterior access. 💡 Advantageous for bilateral tumors, morbid obesity, and patients with prior extensive abdominal surgery.
⭐ Pheochromocytoma Prep: Crucial pre-op alpha-blockade (e.g., phenoxybenzamine) followed by beta-blockade is mandatory to prevent intraoperative catecholamine surge and hypertensive crisis.
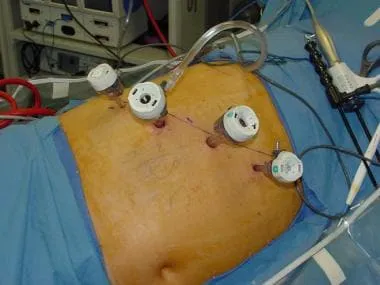
⚠️ Complications - Tiny Access Troubles
- Gas-Related (CO₂ Insufflation):
- Subcutaneous emphysema: Common, benign crepitus.
- Hypercarbia/Acidosis: Monitor end-tidal CO₂.
- Gas embolism: Rare but lethal. Sudden ↓ETCO₂, hypotension.
- Procedure-Specific Nerve Injury:
- Thyroid/Parathyroid: RLN (hoarseness), SLN (voice pitch change).
- Other:
- Port-site issues (hernia, bleeding), visceral/vascular injury (adrenalectomy).
⭐ A sudden, sharp drop in end-tidal CO₂ (ETCO₂) during insufflation is a classic sign of a CO₂ gas embolism.
⚡ Biggest Takeaways
- Minimally Invasive Parathyroidectomy (MIP) is standard for localized adenomas; success is confirmed by a >50% drop in intraoperative PTH.
- Laparoscopic adrenalectomy is the gold standard for most benign tumors (pheo, Conn's); avoid for large (>6 cm) or suspected adrenocortical carcinomas.
- Minimally Invasive Thyroidectomy is for small (<3-4 cm), low-risk nodules; recurrent laryngeal nerve injury risk is similar to open surgery.
- Preoperative localization (sestamibi, US, CT) is critical for patient selection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

