🥊 Drug class/MOA - The Knockout Crew
📌 PEK for IV Anesthetics: Propofol, Etomidate, Ketamine.
| Drug | MOA | Key Clinical Points |
|---|---|---|
| Propofol | Potentiates GABA-A | Rapid onset/offset. Hypotension, apnea, antiemetic. |
| Etomidate | Potentiates GABA-A | Hemodynamically stable (cardio-stable). ⚠️ Adrenal suppression. |
| Ketamine | NMDA Antagonist | Dissociative anesthesia. Sympathomimetic (↑HR, ↑BP), bronchodilation. |
| Barbiturates | Potentiates GABA-A | ↓ICP, neuroprotective. Risk of laryngospasm. |
💨 PK/PD - In, Out, How Fast?
- Inhaled Anesthetics (Uptake/Elimination):
- Blood:Gas Partition Coefficient: Determines speed.
- Low solubility (N₂O, Desflurane) = Fast onset/offset.
- High solubility (Halothane) = Slow onset/offset.
- Induction is faster with: ↑ ventilation, ↓ cardiac output.
- Blood:Gas Partition Coefficient: Determines speed.
- IV Anesthetics (e.g., Propofol):
- Onset: Rapid distribution to vessel-rich groups (brain).
- Termination: Redistribution to muscle/fat, not metabolism.
- Potency - MAC (Minimum Alveolar Concentration):
- Concentration preventing movement in 50% of patients to stimulus.
- ↓ MAC = ↑ Potency.
- Factors ↓ MAC: ↑ Age, hypothermia, opioids.
⭐ In shock (↓ CO), inhaled anesthetic induction is faster. Less blood flow removes less agent from the lungs, causing a rapid rise in alveolar partial pressure.
😴 Staging the Sleep: General Anesthesia
General anesthesia depth is classically described in four stages (Guedel's Classification). The goal is to rapidly achieve and maintain Stage III for surgery.
- Stage I (Analgesia): Drowsy, conscious, reduced pain sensation.
- Stage II (Excitement): Delirium, irregular breathing, risk of laryngospasm.
⭐ This stage is dangerous and is bypassed quickly with modern agents (e.g., propofol). Uninhibited reflexes can cause vomiting, aspiration, and injury.
- Stage III (Surgical Anesthesia): Unconscious, regular breathing, loss of reflexes. Ideal for surgery.
- Stage IV (Overdose): Medullary paralysis, apnea, circulatory collapse. ⚠️ Lethal.
😱 The Unwanted Wake-up (Intraoperative Awareness)
- Definition: Explicit recall of sensory perceptions (auditory, tactile, pain) during general anesthesia. A devastating complication, can cause PTSD.
- High-Risk Scenarios:
- Cardiac surgery, trauma, C-sections
- Hemodynamic instability requiring ↓ anesthetic
- History of awareness, substance use
- Prevention & Monitoring:
- Vigilant monitoring of vitals & end-tidal anesthetic concentration (ETAC).
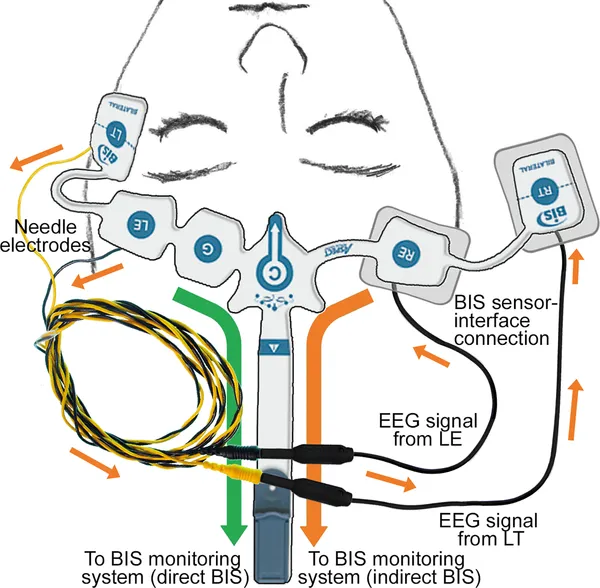
- Processed EEG (e.g., Bispectral Index - BIS) helps titrate anesthetic depth. Target BIS: 40-60.
⭐ Warning: The greatest risk is paralysis without amnesia. Always ensure adequate sedation and amnesia (e.g., benzodiazepines, volatile anesthetics) before administering neuromuscular blockers.
⚡ Biggest Takeaways
- MAC (Minimum Alveolar Concentration) is inversely proportional to potency; it's decreased by age, hypothermia, and other CNS depressants.
- Low blood:gas solubility (e.g., N₂O, Desflurane) means rapid induction and recovery; high solubility means slow onset.
- Propofol is common for induction/maintenance; Etomidate is hemodynamically stable but causes adrenal suppression.
- Ketamine causes dissociative anesthesia and is a sympathomimetic (bronchodilation, ↑HR/BP).
- Malignant hyperthermia is triggered by succinylcholine/volatile anesthetics; treat with dantrolene.
- Succinylcholine can cause life-threatening hyperkalemia, especially in burn/crush injury patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

