Pathophysiology - Gut Pouch Punch-Up
- False diverticula: Mucosa and submucosa herniate through the muscularis propria.
- Occur at weak points in the colonic wall where vasa recta penetrate.
- 📌 Sigmoid Is The Site: Highest pressure area.
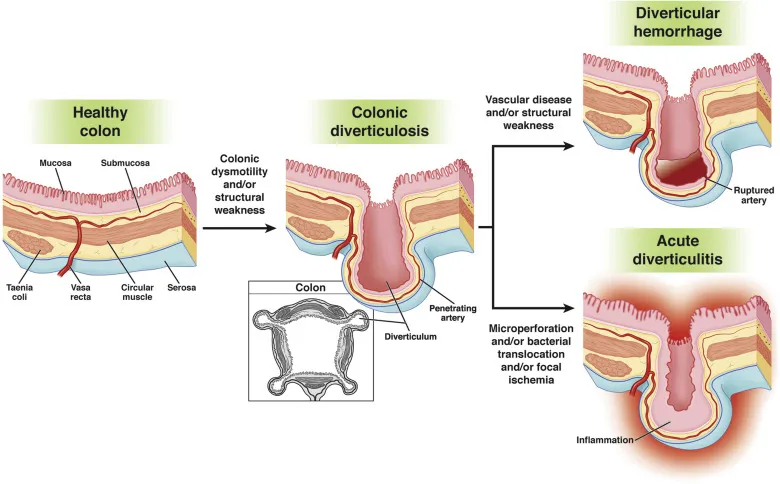
⭐ The sigmoid colon is the most common site for diverticula (>90% of cases) because it's the narrowest colonic segment, generating the highest pressures via the Law of Laplace.
Presentation & Diagnosis - Bellyache Breakdown
-
Classic Presentation: Steady, deep LLQ pain, fever, and altered bowel habits (constipation > diarrhea). Nausea and anorexia are common.
- Physical Exam: Localized tenderness, palpable mass (phlegmon/abscess), guarding.
- 📌 Note: Right-sided diverticula (common in Asian populations) can mimic appendicitis.
-
Diagnostic Workup:
- Labs: Leukocytosis (↑ WBC) is typical.
- Imaging: Abdominal/Pelvic CT with contrast is the gold standard.
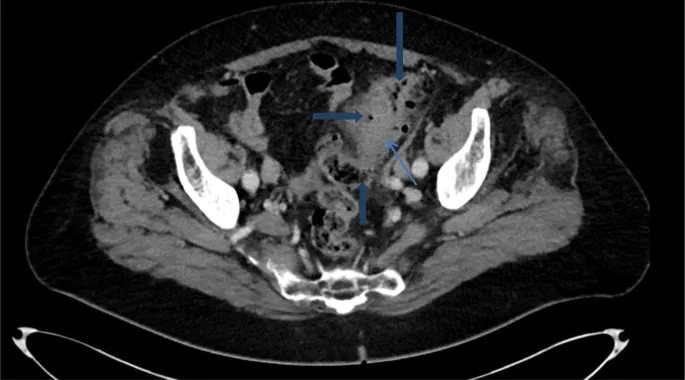
- Key CT Findings: Sigmoid wall thickening (>4 mm), pericolic fat stranding, abscess, fistula.
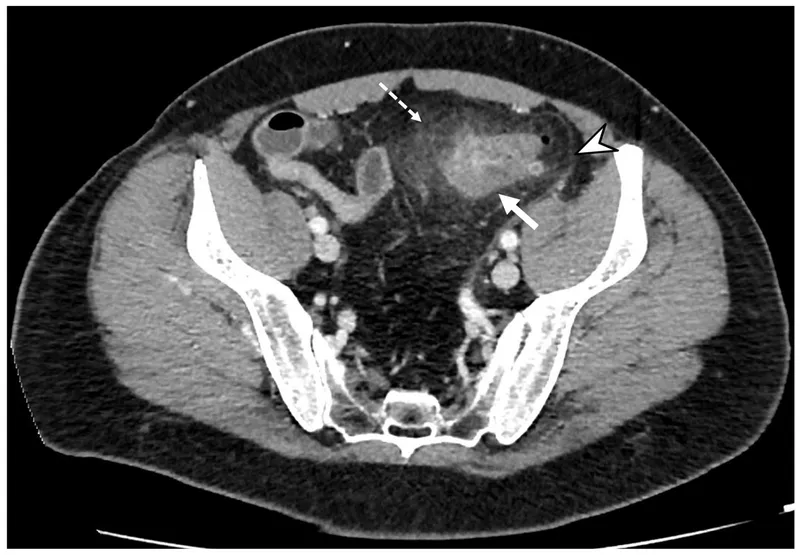
⭐ High-Yield: Never perform a colonoscopy or barium enema during an acute attack. It dramatically increases perforation risk. A colonoscopy should be done 6-8 weeks post-recovery to exclude underlying malignancy.
Staging & Management - Calming the Chaos
- Hinchey Classification (Modified) for Complicated Diverticulitis:
- Stage 1a: Pericolic inflammation/phlegmon
- Stage 1b: Pericolic or mesocolic abscess (<5 cm)
- Stage 2: Pelvic, distant intra-abdominal, or retroperitoneal abscess (≥5 cm)
- Stage 3: Purulent peritonitis
- Stage 4: Feculent peritonitis
⭐ Elective Sigmoidectomy: Consider after recovery in patients who are young, immunosuppressed, or after a complicated episode to prevent recurrence. The old "two-strikes" rule is no longer absolute; decisions are individualized.
Complications - When Guts Go Rogue
- Abscess: Most common complication. Look for persistent fever despite antibiotics. Percutaneous drainage often required if > 4-5 cm.
- Fistula: Abnormal connection to adjacent organs.
- Colovesical: Most common; presents with pneumaturia, fecaluria.
- Colovaginal: Passage of flatus/stool from vagina.
- Obstruction: Partial or complete blockage from stricture formation due to chronic inflammation.
- Perforation: Free perforation leads to purulent or feculent peritonitis (Hinchey stages III/IV).
⭐ High-Yield: The most common fistula type is colovesical, classically presenting with air in the urine (pneumaturia).
High‑Yield Points - ⚡ Biggest Takeaways
- Classic triad: LLQ pain, fever, leukocytosis. Sigmoid colon is the most common site.
- CT scan with contrast is the best diagnostic test.
- Complications include abscess, fistula (colovesical is classic), obstruction, and perforation.
- Uncomplicated cases: treat with bowel rest and oral antibiotics.
- Complicated cases: require IV antibiotics. Abscesses >4 cm need percutaneous drainage.
- Peritonitis or perforation mandates emergency surgery (e.g., Hartmann procedure).
- Prevent recurrence with a high-fiber diet after resolution.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

