Pathophysiology & Presentation - The Angry Worm
- Pathogenesis: Luminal obstruction (fecalith, lymphoid hyperplasia) → mucus buildup → ↑ intraluminal pressure → bacterial overgrowth (E. coli, Bacteroides).
- Progression: Inflammation → venous congestion → ischemia → necrosis → perforation (< 24-48 hrs).
- Classic Symptoms:
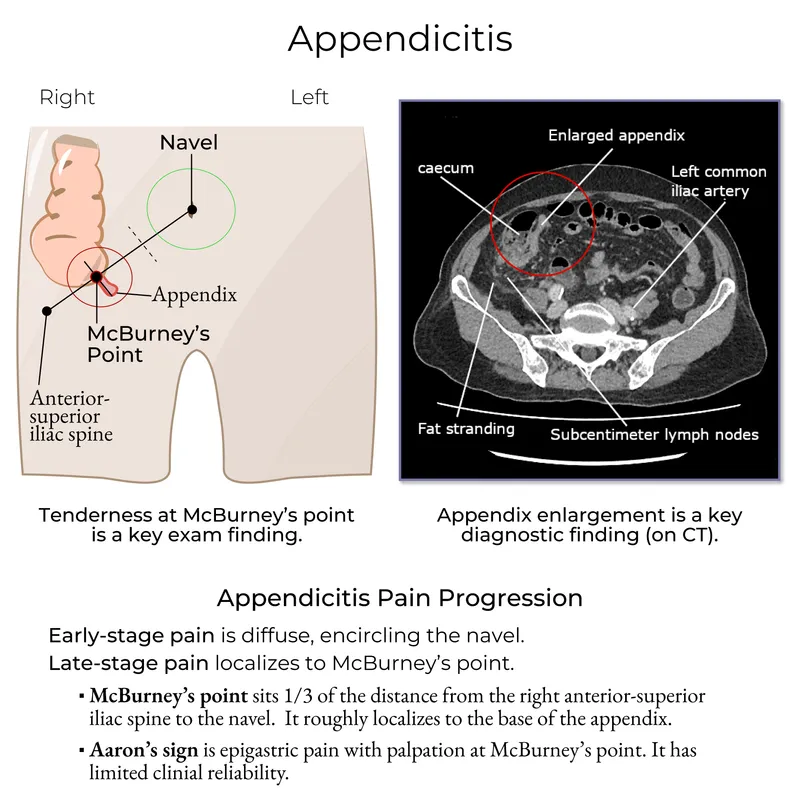
- Early: Vague, dull periumbilical pain (visceral).
- Followed by: Anorexia (the "hamburger sign"), nausea, and vomiting.
- Late: Pain migrates to the Right Lower Quadrant (RLQ), becoming sharp and localized (somatic).
- Key Signs:
- Tenderness at McBurney's point.
- Low-grade fever (~38°C / 100.4°F).
- Peritoneal signs: Rovsing's, Psoas, Obturator.
⭐ Exam Tip: The migration of pain from the periumbilical area to the RLQ is the most reliable clinical feature.
Diagnosis & Scoring - The Scorecard
-
Alvarado Score: A 10-point clinical scale to stratify risk and guide management.
- 📌 Mnemonic: MANTRELS
- Migratory RLQ pain (1)
- Anorexia (1)
- Nausea/Vomiting (1)
- Tenderness in RLQ (2)
- Rebound tenderness (1)
- Elevated temp >37.3°C (1)
- Leukocytosis >10,000/mm³ (2)
- Shift to left-bandemia (1)
-
Score-Based Triage Pathway:
- Imaging Confirmation:
- CT scan (IV contrast): Gold standard in adults. Shows dilated appendix (>6mm), wall enhancement, periappendiceal fat stranding.
- Ultrasound: Preferred for children and pregnant patients to avoid radiation.
⭐ A normal white blood cell count does not exclude appendicitis. Up to 20% of patients with surgically confirmed appendicitis present with a WBC within the normal range.
Imaging & Differentials - Picture Perfect?
- Imaging Modalities:
- CT Scan (A/P with IV contrast): Preferred for most adults.
- Key signs: Appendix >6 mm diameter, wall thickening, periappendiceal fat stranding, appendicolith.
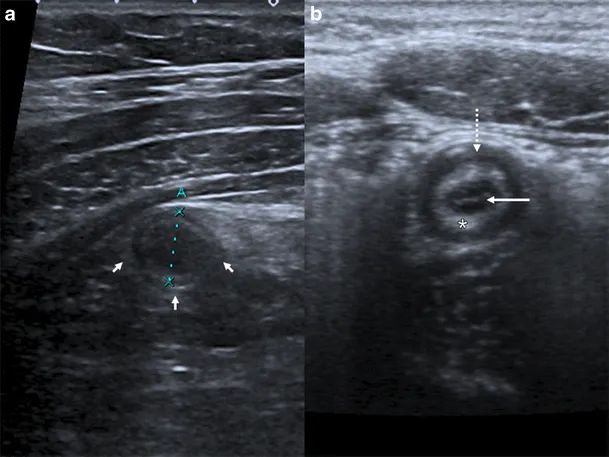
- Ultrasound: Initial choice for children and pregnant women.
- Key signs: Non-compressible, blind-ended tube >6 mm; "target sign" on transverse view.
- MRI: Alternative in pregnancy if ultrasound is equivocal.
- CT Scan (A/P with IV contrast): Preferred for most adults.
- Common Differentials:
- GI: Meckel's diverticulitis, Crohn's ileitis, mesenteric adenitis.
- Gyn (📌 METRO): Meckel's, Ectopic pregnancy, Tubo-ovarian abscess, Ruptured cyst, Ovarian torsion.
- GU: Ureteral colic, pyelonephritis.
⭐ CT scanning has dramatically reduced the negative appendectomy rate (perforating a normal appendix) from ~20% to <5%.
Management & Complications - Snip, Snip, Troubles
- Pre-operative Care: NPO, IV fluids, and broad-spectrum IV antibiotics (e.g., Cefoxitin, Piperacillin-tazobactam) to cover gram-negatives and anaerobes.
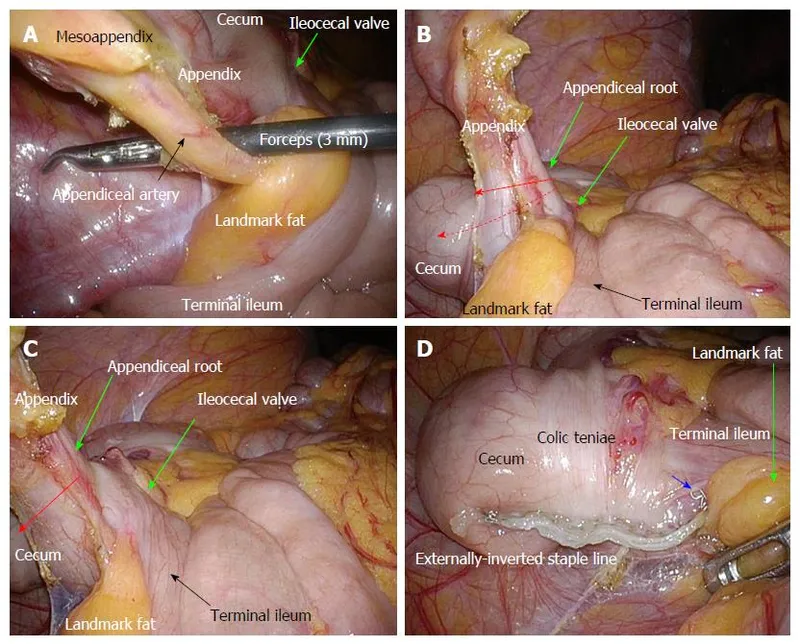
- Definitive Treatment: Laparoscopic appendectomy is the gold standard.
- Complications:
- Perforation: Most common complication, leading to peritonitis.
- Appendiceal Abscess: Contained infection; requires drainage.
- Phlegmon: Inflammatory mass without a drainable pus collection.
- Surgical Site Infection (SSI).
⭐ Appendiceal Mass (Phlegmon/Abscess): If a patient presents late with a contained perforation forming a palpable mass, the initial management is conservative with IV antibiotics and possibly percutaneous drainage. An interval appendectomy is performed 6-8 weeks later.
High‑Yield Points - ⚡ Biggest Takeaways
- Classic presentation is periumbilical pain migrating to the RLQ (McBurney's point).
- Key physical exam findings include Rovsing's, psoas, and obturator signs.
- Caused by luminal obstruction, most commonly by a fecalith.
- Diagnosis is clinical; CT scan is the most accurate imaging in adults.
- Ultrasound is the preferred initial imaging for children and pregnant patients.
- Definitive treatment is surgical appendectomy.
- The most feared complication is perforation, leading to peritonitis or abscess.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

