ID Diagnosis - Brains & Behavior
- Core Criteria: Deficits in both intellectual & adaptive functioning, onset during developmental period.
- Intellectual Functioning: Assessed by IQ testing.
- Mild: 50-70
- Moderate: 35-49
- Severe: 20-34
- Profound: <20
- Adaptive Functioning: Failure to meet sociocultural standards for independence. 3 domains:
- Conceptual (e.g., language, memory)
- Social (e.g., empathy, social judgment)
- Practical (e.g., personal care, job skills)

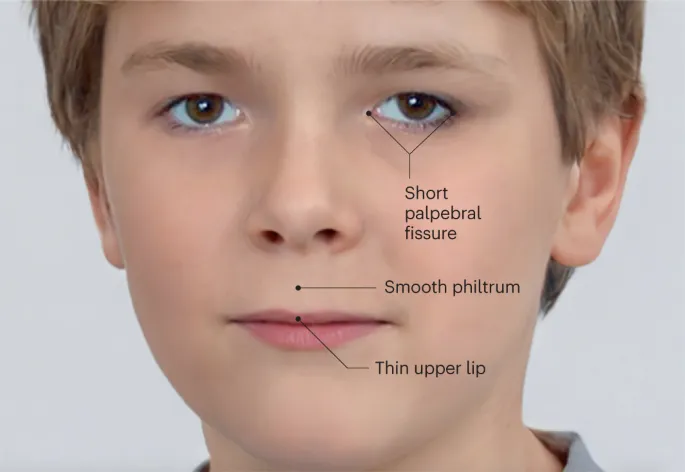
⭐ Etiology: Fetal alcohol syndrome is the leading preventable cause of intellectual disability in the United States.
The Severity Spectrum - More Than a Number
-
DSM-5 shifted the primary basis for severity classification from fixed IQ scores to adaptive functioning.
-
Severity is determined by the level of support required across three key domains.
-
📌 "Can Sam Play?" recalls the domains: Conceptual, Social, Practical.
-
Mild (IQ ~50-70)
-
- Conceptual: Academic skills up to approximately 6th-grade level. Abstract thinking is impaired.
-
- Social: Immature in social interactions; difficulty regulating emotion and behavior.
-
- Practical: Can achieve independence in personal care (ADLs); needs support with complex tasks like legal decisions or healthcare management.
-
-
Moderate (IQ ~35-50)
-
- Conceptual: Skills develop slowly, remaining at an elementary level in adulthood.
-
- Social: Marked differences from peers in social behavior; requires significant support for relationships.
-
- Practical: Can manage personal needs with extensive teaching; requires considerable support for household tasks and employment.
-
-
Severe (IQ ~20-35)
-
- Conceptual: Limited attainment of conceptual skills; little understanding of written language or concepts involving numbers.
-
- Social: Spoken language is limited to single words or phrases.
-
- Practical: Requires support for all ADLs, including meals, dressing, and bathing; constant supervision is essential.
-
-
Profound (IQ <20)
-
- Conceptual: Generally involves the physical world rather than symbolic processes.
-
- Practical: Dependent on others for all aspects of daily physical care, health, and safety.
-
⭐ Mild intellectual disability is the most common form, accounting for approximately 85% of all cases. These individuals can often live independently with minimal support.
ID Origins - Roots & Roommates
- Etiologies (often multifactorial):
- Prenatal (~35%): Genetic syndromes (e.g., Down, Fragile X), inborn errors of metabolism, maternal infections (📌 TORCH), toxins (Fetal Alcohol Syndrome).
- Perinatal (~10%): Hypoxic-ischemic encephalopathy, extreme prematurity, birth trauma.
- Postnatal (~20%): Traumatic brain injury, meningitis/encephalitis, severe malnutrition, lead poisoning.
- Common Comorbidities ("Roommates"):
- ADHD, Autism Spectrum Disorder (ASD), Cerebral Palsy, Epilepsy.
⭐ Fragile X Syndrome is the most common inherited cause of intellectual disability.
High-Yield Points - ⚡ Biggest Takeaways
- Intellectual disability requires deficits in both intellectual and adaptive functioning with onset during the developmental period.
- Adaptive functioning has three domains: conceptual, social, and practical.
- Severity (mild, moderate, severe, profound) is determined by adaptive functioning, not just the IQ score.
- Mild ID (IQ ~50-70): Can achieve 6th-grade academic skills; capable of independent living with support.
- Moderate ID (IQ ~35-50): Can achieve 2nd-grade skills; requires supervised living arrangements.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

