Diagnosis & Core Features - Spotting the Shadows
- Foundation: Patient must meet full DSM-5 criteria for a Major Depressive Episode (MDE).
- ≥5 of 9 SIGECAPS symptoms for ≥2 consecutive weeks.
- Must include either depressed mood or anhedonia (loss of interest/pleasure).
- Psychosis Overlay: Presence of delusions (fixed, false beliefs) and/or hallucinations (sensory perceptions without external stimuli).
- Mood-Congruent: Content aligns with depressive themes (e.g., guilt, disease, death, nihilism, deserved punishment).
- Mood-Incongruent: Content does not involve typical depressive themes.
- Critical Timing: Psychotic symptoms occur exclusively during major depressive episodes.
⭐ If psychosis occurs for ≥2 weeks in the absence of a major mood episode, the diagnosis is more likely Schizoaffective Disorder.
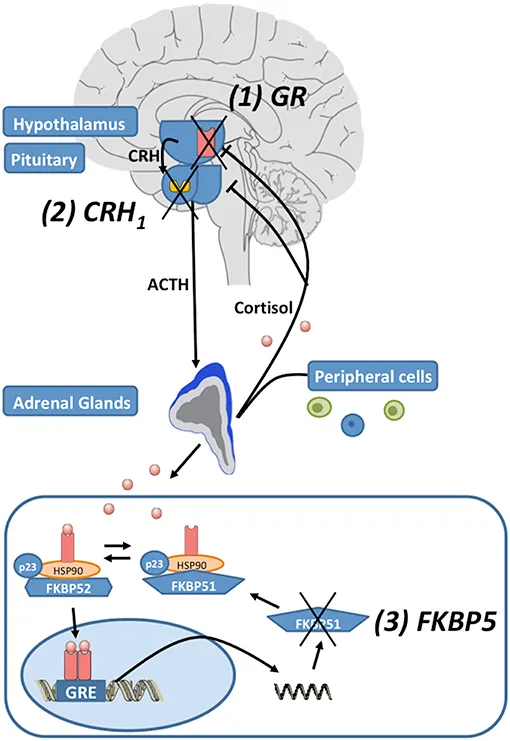
Pathophysiology & Neurobiology - Brain Under Siege
- HPA Axis Hyperactivity: ↑ Cortisol from chronic stress.
- Causes glucocorticoid receptor resistance, leading to hippocampal atrophy.
- Dopamine (DA) Dysregulation:
- ↑ Mesolimbic DA → positive psychotic symptoms.
- ↓ Mesocortical DA → negative symptoms & cognitive deficits.
- Monoamine & Glutamate Imbalance:
- ↓ Serotonin (5-HT) & Norepinephrine (NE) → depressed mood.
- ↑ Glutamate → excitotoxicity.
- Neuroinflammation: ↑ Pro-inflammatory cytokines (e.g., IL-6, TNF-α).
⭐ Failure to suppress cortisol with dexamethasone is strongly associated with psychotic depression, indicating severe HPA axis dysfunction.
Clinical Workup & Differentials - Ruling Out Mimics
- Initial Labs: Rule out organic causes with CBC, CMP, TSH, Vitamin B12/folate, and urine toxicology.
- Neuroimaging (CT/MRI): Consider for late-onset psychosis or if neurological signs are present.
- Primary Goal: Differentiate from other primary psychotic disorders based on symptom timing.
⭐ In psychotic depression, psychotic features resolve with the resolution of the mood episode. In contrast, schizoaffective disorder requires at least 2 weeks of psychosis without mood symptoms.
Treatment & Management - Restoring the Light
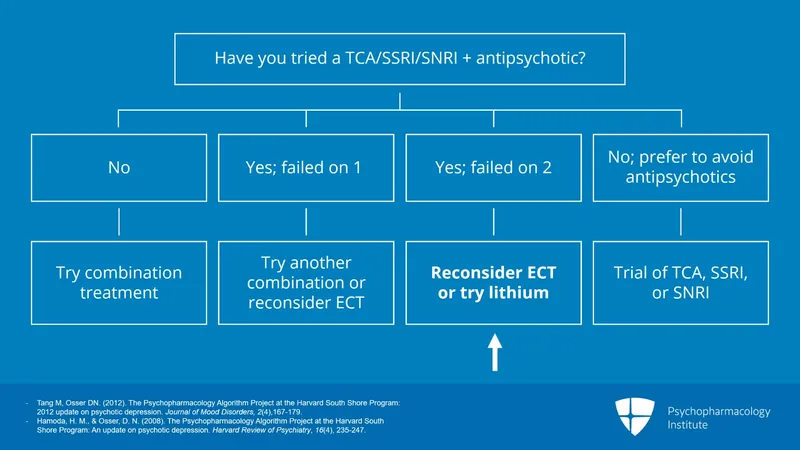
- First-Line: Combination therapy is key. Monotherapy with an antidepressant is ineffective.
- Antidepressant (SSRI/SNRI) + Antipsychotic (SGA).
- Example: Sertraline + Olanzapine.
- ECT (Electroconvulsive Therapy): Most effective & rapid treatment.
- Consider for severe suicidality, catatonia, malnutrition, or treatment resistance.
⭐ High-Yield: Antidepressant monotherapy can worsen psychosis in these patients and is considered malpractice.
High‑Yield Points - ⚡ Biggest Takeaways
- A subtype of Major Depressive Disorder (MDD) where patients experience hallucinations or delusions.
- Psychotic features are typically mood-congruent, involving themes of guilt, deserved punishment, or nihilism.
- Differentiate from schizoaffective disorder: psychosis occurs only during depressive episodes.
- First-line treatment is combination therapy with an antidepressant PLUS an antipsychotic.
- Electroconvulsive therapy (ECT) is a highly effective primary treatment, especially for severe or urgent cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

