V/Q Mismatch - Lungs Out of Sync
-
V/Q Ratio ($V_A/Q_c$): The ratio of alveolar ventilation ($V_A$) to pulmonary blood flow ($Q_c$), which measures gas exchange efficiency. An ideal match is a V/Q ratio of ~0.8.
-
Mismatch Spectrum:
- Dead Space (V/Q → ∞): Ventilation without perfusion. Occurs with obstruction of blood flow, like in a pulmonary embolism.
- Shunt (V/Q → 0): Perfusion without ventilation. Seen in airway obstruction or fluid-filled alveoli (e.g., pneumonia, ARDS).
-
Physiological Gradient (Upright Lung):
- Apex: ↑ V/Q. Less perfusion relative to ventilation.
- Base: ↓ V/Q. More perfusion relative to ventilation.
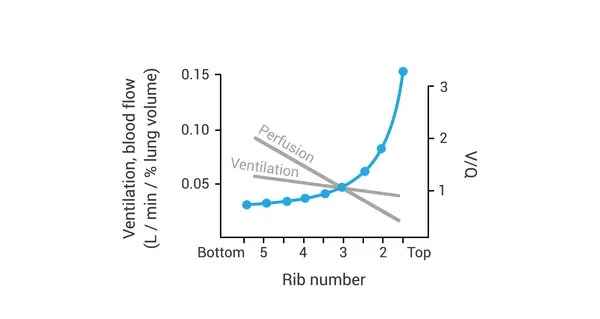
⭐ Both ventilation and perfusion are greatest at the lung base. However, blood flow increases more dramatically from apex to base than ventilation does, causing the V/Q ratio to be lower at the base.
Hypoxic Pulmonary Vasoconstriction - The Lung's Smart Squeeze
A unique, protective mechanism where pulmonary arteries constrict in response to low alveolar oxygen levels ($P_{A}O_2$). This shunts blood from poorly ventilated lung regions to areas with better ventilation, optimizing V/Q matching and systemic oxygenation.
- Trigger: Low alveolar pO₂ ($P_{A}O_2$).
- Action: Smooth muscle constriction in pulmonary arterioles.
- Result: ↑ Pulmonary vascular resistance in hypoxic areas, diverting blood flow to normoxic regions.

⭐ Systemic Contrast: This is the opposite of systemic circulation, where hypoxia triggers vasodilation to increase blood flow and oxygen delivery to tissues.
Pathophysiology - When The Squeeze Goes Global
When hypoxia is widespread (e.g., high altitude, COPD), HPV occurs globally, causing diffuse vasoconstriction instead of shunting blood to better-ventilated areas.
-
This leads to a massive ↑ in Pulmonary Vascular Resistance (PVR).
-
The result is Pulmonary Hypertension.
-
Chronic pressure overload forces the right ventricle to work harder, leading to Right Ventricular Hypertrophy and eventually Cor Pulmonale (right-sided heart failure).
-
Factors that inhibit HPV:
- Certain anesthetics (e.g., halothane)
- Sepsis
- Calcium channel blockers
- Metabolic acidosis or alkalosis
⭐ At high altitude, the A-a gradient is normal. Both alveolar ($P_AO_2$) and arterial ($P_aO_2$) oxygen levels are low due to decreased inspired oxygen, but the gradient itself does not increase.
Clinical Correlations - V/Q Villains
- V/Q Mismatch: Most common cause of hypoxemia. Responds to 100% O₂ because oxygen can still reach underventilated alveoli.
- True Shunt: Blood bypasses ventilation; hypoxemia is refractory to 100% O₂.
| Condition | Pathophysiology | V/Q Ratio |
|---|---|---|
| Pulmonary Embolism | Ventilation without perfusion | $V/Q \rightarrow \infty$ (↑ Dead Space) |
| Pneumonia, Asthma | Perfusion without ventilation | $V/Q \rightarrow 0$ (↑ Shunt) |
| HAPE | Global HPV, ↑ capillary pressure | Low V/Q globally |
High‑Yield Points - ⚡ Biggest Takeaways
- Hypoxic Pulmonary Vasoconstriction (HPV) is a response to alveolar hypoxia (↓ PAO₂), not systemic hypoxemia.
- It diverts blood from poorly ventilated areas to well-ventilated areas, thus optimizing V/Q matching.
- This is the opposite of systemic circulation, where hypoxia causes vasodilation.
- The mechanism involves inhibition of voltage-gated K+ channels in pulmonary artery smooth muscle.
- Chronic, diffuse hypoxia (e.g., COPD, high altitude) can lead to pulmonary hypertension.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

