V/Q Basics - The Lung's Balancing Act
- Ventilation/Perfusion ($V/Q$) Ratio: A measure of gas exchange efficiency. The ideal system-wide value is ~0.8.
- Gravity's Effect: In an upright person, gravity pulls both air (V) and blood (Q) towards the lung base.
- Apex (Top): Less perfusion and less ventilation. Perfusion is very low, leading to a high $V/Q$ ratio (physiologic dead space).
- Base (Bottom): More perfusion and more ventilation. Perfusion is very high, resulting in a low $V/Q$ ratio (physiologic shunt).

⭐ Both ventilation and perfusion are highest at the lung base. However, the increase in perfusion is far greater than the increase in ventilation, which is why the $V/Q$ ratio is lowest at the base.
Gravity & Perfusion - Blood's Downhill Ride
- Gravity pulls blood towards the lung base (dependent parts).
- This creates a gradient of blood flow (perfusion), which is lowest at the apex and highest at the base.
- This is described by the three West Zones, based on the relationship between alveolar ($P_A$), arterial ($P_a$), and venous ($P_v$) pressures.
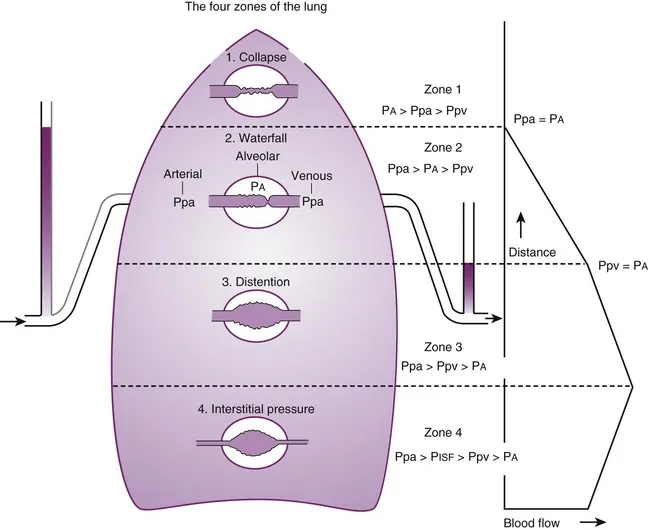
| Zone | Pressure Relationship | Blood Flow |
|---|---|---|
| 1 (Apex) | $P_A > P_a > P_v$ | ↓ Lowest |
| 2 (Middle) | $P_a > P_A > P_v$ | Intermittent |
| 3 (Base) | $P_a > P_v > P_A$ | ↑ Highest |
Gravity & Ventilation - Air's Uphill Battle
- Gravity pulls the lungs down, making intrapleural pressure more negative at the apex than the base.
- Apex Alveoli:
- Higher transpulmonary pressure at rest → more inflated.
- Operate on the flatter, less compliant part of the pressure-volume curve.
- Result: ↓ ventilation during tidal breathing.
- Base Alveoli:
- Lower transpulmonary pressure at rest → less inflated (more compressed).
- Operate on the steep, highly compliant part of the P-V curve.
- Result: ↑ ventilation during tidal breathing.
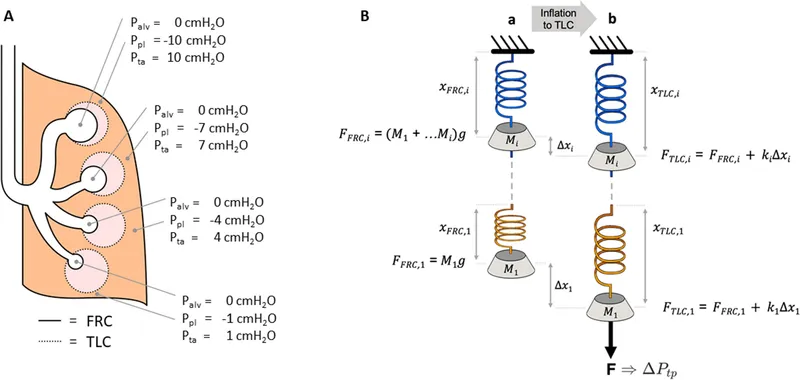
⭐ Despite being more distended at rest, the apex is less ventilated than the base during normal breathing because the basal alveoli are more compliant.
V/Q Gradient - Apex-to-Base Summary
In an upright individual, gravity dictates that both ventilation (V) and perfusion (Q) are lowest at the apex and highest at the base. However, the gradient for perfusion is much steeper than for ventilation.

-
Apex (Zone 1):
- Alveoli are stretched open, but perfusion is minimal due to gravity.
- ↓ Ventilation, ↓↓↓ Perfusion.
- High V/Q Ratio (~3.0): Wasted ventilation, creating physiologic dead space.
- Gas pressures approach inspired air: ↑ $P_{A}O_2$ (
130 mmHg), ↓ $P_{A}CO_2$ (28 mmHg).
-
Base (Zone 3):
- Alveoli are less expanded but receive the bulk of cardiac output.
- ↑ Ventilation, ↑↑↑ Perfusion.
- Low V/Q Ratio (~0.6): Wasted perfusion, creating a physiologic shunt.
- Gas pressures approach mixed venous blood: ↓ $P_{A}O_2$ (
90 mmHg), ↑ $P_{A}CO_2$ (42 mmHg).
⭐ The high $P_{A}O_2$ at the lung apex creates a favorable, oxygen-rich environment for aerobic pathogens like Mycobacterium tuberculosis, explaining the classic location of reactivation disease.
High‑Yield Points - ⚡ Biggest Takeaways
- In an upright lung, gravity pulls blood down, making perfusion (Q) greatest at the base.
- Ventilation (V) is also greater at the base, but the gradient is less steep than for perfusion.
- This results in the V/Q ratio being lowest at the base (<1) and highest at the apex (>1).
- The apex acts as physiologic dead space (wasted ventilation).
- The base acts as a physiologic shunt (wasted perfusion).
- Tuberculosis reactivation favors the high O₂ environment of the apex.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

