Respiratory Centers - The Brain's Breathing Bosses
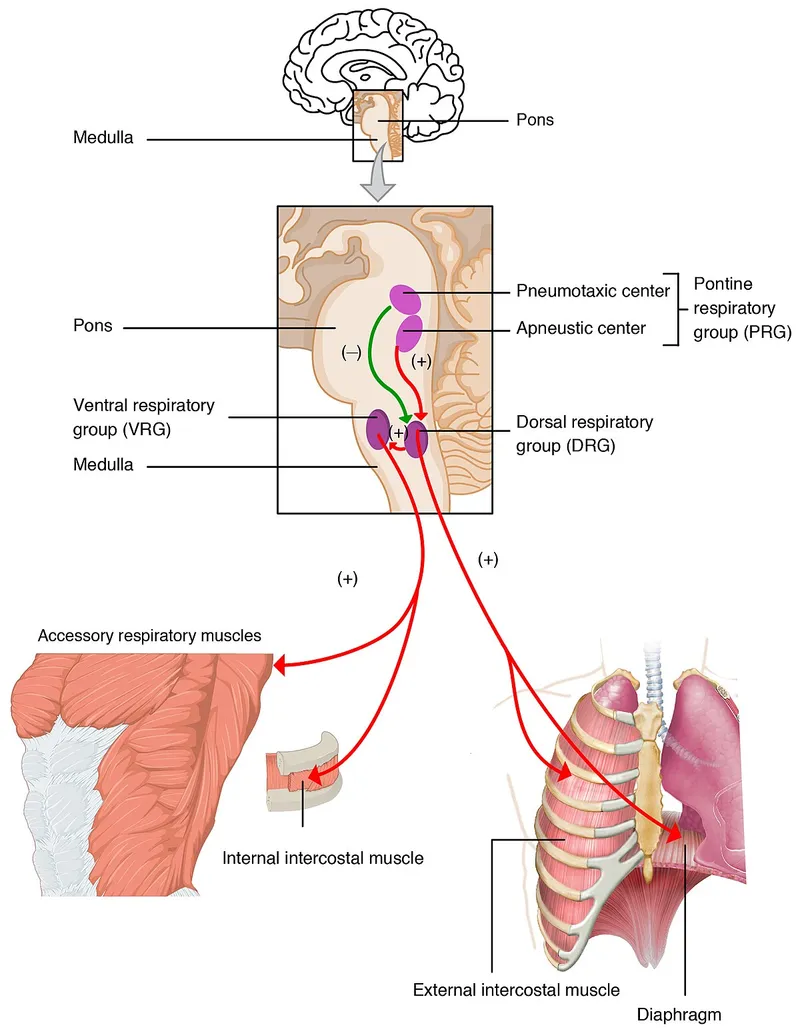
Located in the medulla oblongata and pons, these nuclei orchestrate automatic breathing.
- Medullary Centers: Primary drivers.
- Dorsal Respiratory Group (DRG): Main inspiratory center; gets sensory input.
- Ventral Respiratory Group (VRG): Forced inspiration and active expiration.
- Pontine Centers: Modulate the medulla.
- Pneumotaxic Center: Limits inspiration ('off-switch'), fine-tunes rate.
- Apneustic Center: Stimulates inspiration; overridden by pneumotaxic signals.
⭐ Opioids cause respiratory depression by inhibiting these medullary centers.
Medullary Centers - Medulla's Mighty Meters
-
Dorsal Respiratory Group (DRG): The primary driver for quiet breathing.
- Controls inspiration by activating the diaphragm (via phrenic nerve) and external intercostals.
- Receives sensory input from peripheral chemoreceptors and mechanoreceptors (CN IX, X).
- 📌 DRG → Diaphragm.
-
Ventral Respiratory Group (VRG): Active during forced or active breathing.
- Contains both inspiratory and expiratory neurons.
- Controls accessory muscles for forced inspiration and expiration.
- 📌 VRG → Vigorous Ventilation.
⭐ Pre-Bötzinger complex: Located within the VRG, this is the essential pacemaker that generates the basic respiratory rhythm.
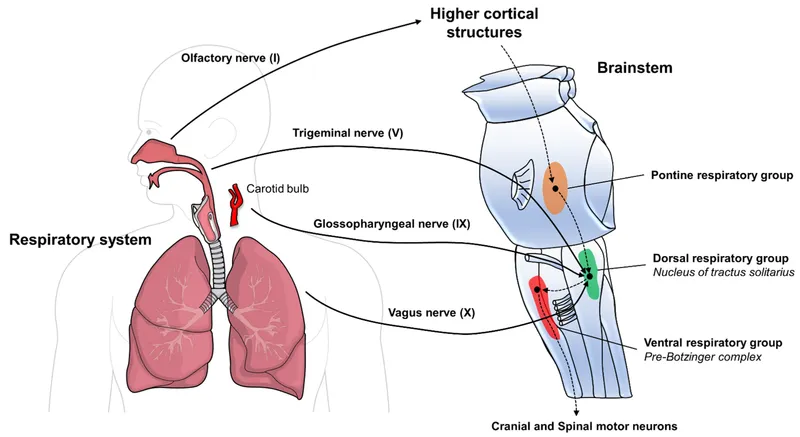
Pontine Centers - Pons' Pacing Partners
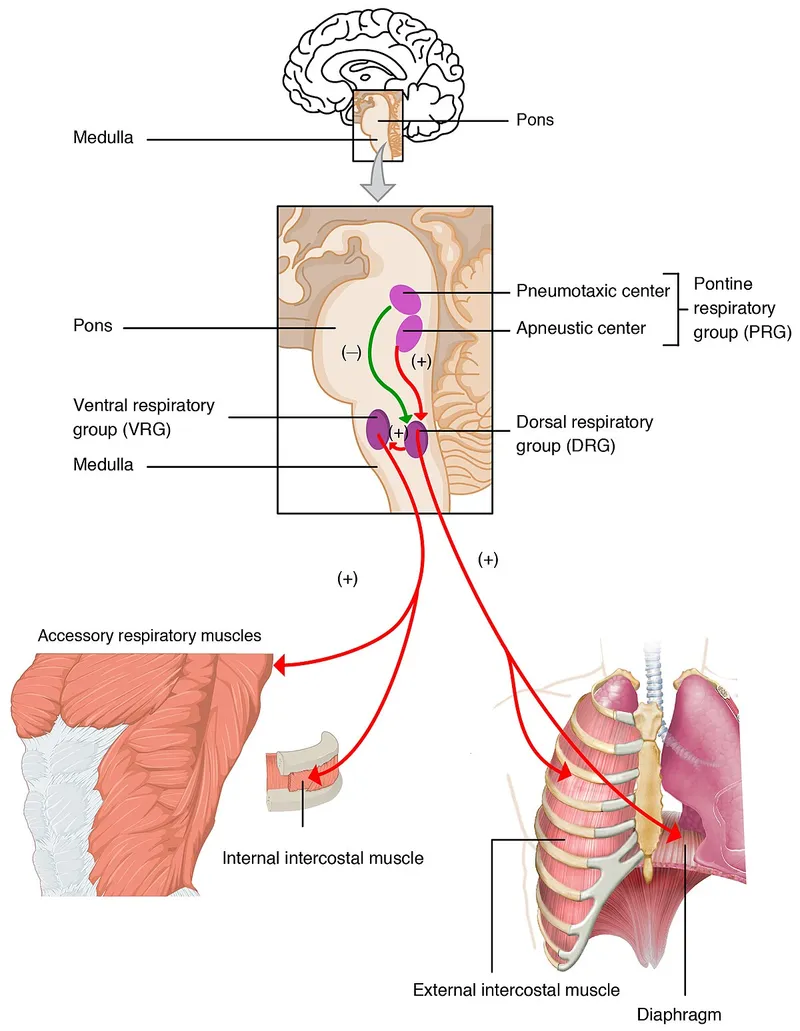
-
Pneumotaxic Center (Upper Pons)
- Fine-tunes the respiratory rhythm by inhibiting inspiration.
- Limits the duration of the inspiratory ramp signal from the medulla.
- Primary effect: controls tidal volume and increases the respiratory rate.
- 📌 Mnemonic: Pneumotaxic Prevents Prolonged inspiration.
-
Apneustic Center (Lower Pons)
- Provides a stimulatory signal to the medullary inspiratory neurons.
- Promotes deep, prolonged inspirations (apneusis).
- Its activity is overridden by inhibitory signals from the pneumotaxic center and vagal afferents.
⭐ Exam Favorite: Lesioning the pneumotaxic center alone only slightly alters breathing. However, if combined with vagotomy (cutting vagus nerve input), it causes apneusis-prolonged inspiratory gasps with brief exhalation-revealing the apneustic center's unopposed activity.
Control of Respiration - Chemical & Neural Command
- Primary Respiratory Centers (Medulla)
- Dorsal Respiratory Group (DRG): Inspiratory pacemaker. Stimulates phrenic nerve → diaphragm contraction.
- Ventral Respiratory Group (VRG): Forced expiration (active). Innervates accessory muscles.
- Pontine Centers (Fine-tuning)
- Pneumotaxic Center: Inhibits DRG, limits inspiration size. Sets respiratory rate.
- Apneustic Center: Stimulates DRG, prolongs inspiration. Overridden by pneumotaxic signals.
⭐ The most powerful stimulus for respiration in a healthy person is arterial $P_{CO_2}$. The hypoxic drive (via peripheral chemoreceptors) only becomes significant when arterial $P_{O_2}$ drops below 60 mmHg.
Clinical Correlates - When Breathing Goes Rogue
- Cheyne-Stokes Breathing: A crescendo-decrescendo pattern of breathing followed by apnea. Often seen in heart failure (CHF) or strokes.
- Apneustic Breathing: Indicates damage to the pons. Presents as prolonged inspiratory gasps with a pause at full inspiration.
- Ataxic (Biot's) Breathing: Highly irregular, unpredictable pattern with random deep and shallow breaths. Signifies severe damage to the medulla.
- Opioid-Induced Respiratory Depression: Suppresses medullary centers, leading to ↓ respiratory rate and tidal volume.
⭐ Cheyne-Stokes breathing in patients with advanced heart failure is a form of central sleep apnea and is associated with a poor prognosis.
High‑Yield Points - ⚡ Biggest Takeaways
- The medulla contains the Dorsal Respiratory Group (DRG) for inspiration and Ventral Respiratory Group (VRG) for forced expiration.
- The DRG is the primary pacemaker for quiet breathing; the VRG is recruited during exertion.
- The pons modulates the medulla: the apneustic center stimulates inspiration, the pneumotaxic center inhibits it.
- Central chemoreceptors in the medulla are most sensitive to arterial PCO2 (via CSF pH).
- Peripheral chemoreceptors are primarily driven by hypoxemia (PaO2 < 60 mmHg).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

