Immediate Response - Thin Air, Fast Breaths
- Primary Insult: ↓ Barometric pressure (P_B) at altitude → ↓ Partial pressure of inspired O₂ ($P_iO_₂$).
- Resulting State: Arterial hypoxemia (↓ PaO₂).
- Key Driver: Hypoxemia is sensed by peripheral chemoreceptors, driving the immediate ↑ in ventilation.
- Gas Exchange: Hyperventilation increases alveolar ventilation, partially correcting $PAO_₂$ but causing hypocapnia (↓ PaCO₂).
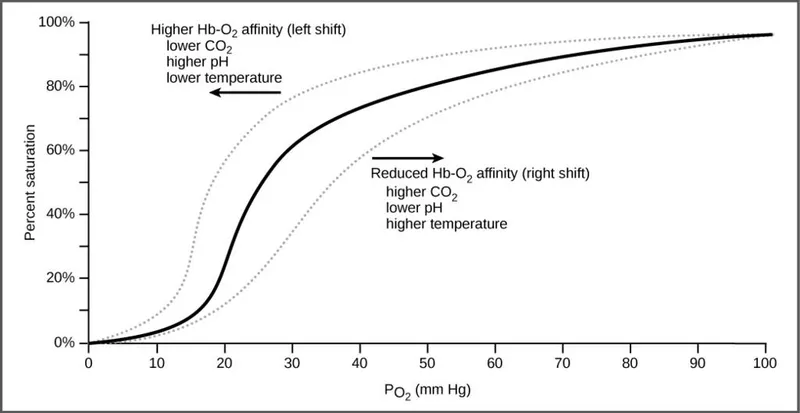
- Acid-Base: Acute respiratory alkalosis (↑ pH) develops, causing a left-shift in the O₂-hemoglobin curve.
⭐ The ventilatory response to high altitude is driven exclusively by peripheral chemoreceptors sensing ↓ PaO₂. Central chemoreceptors are initially inhibited by the resulting hypocapnia and CSF alkalosis.
Acclimatization - The Body's Comeback
- Immediate (Hours to Days):
- Hyperventilation: ↓ PaO₂ stimulates peripheral chemoreceptors, driving ↑ ventilation.
- Respiratory Alkalosis: Resulting from blowing off CO₂, leading to ↑ blood pH.
- Renal Compensation (2-3 days):
- Kidneys increase excretion of bicarbonate ($HCO_3^−$) to help normalize pH.
- Hematologic & Cellular (Days to Weeks):
- ↑ Erythropoietin (EPO): Kidney releases EPO → ↑ RBC production (erythropoiesis) → ↑ hematocrit and hemoglobin.
- ↑ 2,3-BPG: Binds to hemoglobin, causing a rightward shift of the oxygen-hemoglobin dissociation curve, which facilitates O₂ unloading to tissues.
- Cellular Changes: ↑ mitochondria, myoglobin, and angiogenesis.

⭐ A rightward shift in the oxygen-hemoglobin curve, mediated by increased 2,3-BPG, is a critical adaptation that improves peripheral oxygen delivery despite lower arterial oxygen saturation.
📌 Mnemonic for factors that shift the curve to the right: "CADET, face Right!" (↑ CO₂, Acid, 2,3-DPG, Exercise, Temperature).
Pathophysiology - Mountain Maladies
- Acute Mountain Sickness (AMS): Headache plus fatigue, dizziness, or GI upset. Develops 6-12 hrs after ascent. Caused by cerebral vasodilation & mild vasogenic edema from hypoxia.
- High-Altitude Cerebral Edema (HACE): Severe AMS progression. Key signs are ataxia & altered consciousness. Can be fatal within 24 hrs.
- High-Altitude Pulmonary Edema (HAPE): Most lethal. Non-cardiogenic edema from uneven hypoxic pulmonary vasoconstriction → pressure overload & capillary leak.
⭐ Ataxia is the most reliable clinical sign for HACE, distinguishing it from severe AMS. It indicates an emergency requiring immediate descent.

- Hypoxic ventilation response (HVR) triggers immediate hyperventilation, causing respiratory alkalosis.
- Renal compensation follows, with increased bicarbonate (HCO₃⁻) excretion to normalize blood pH.
- Erythropoietin (EPO) levels rise within hours, stimulating erythropoiesis and leading to polycythemia.
- Increased 2,3-BPG shifts the O₂-hemoglobin curve to the right, enhancing O₂ unloading to tissues.
- Chronic hypoxia induces pulmonary vasoconstriction, risking pulmonary hypertension and right heart strain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

