Central Chemoreceptors - The Brain's CO₂ Cops
- Location: Ventral surface of the medulla.
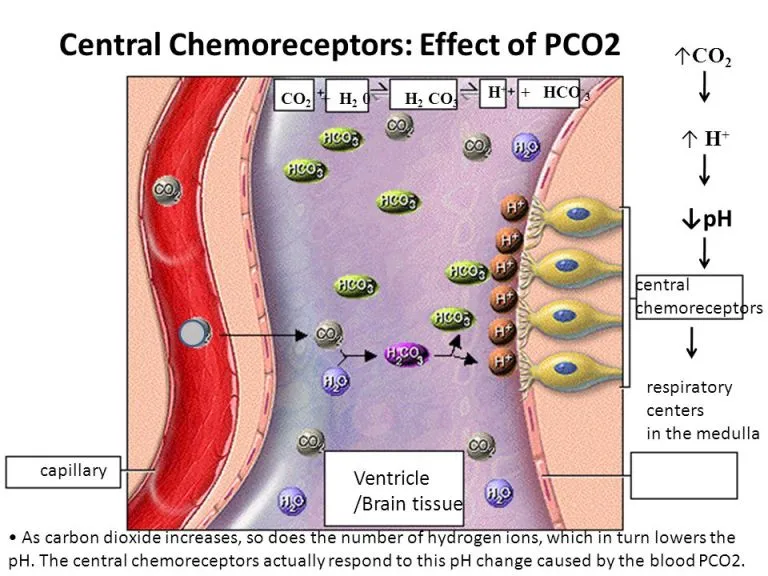
- Primary Stimulus: Changes in arterial $PCO_2$, not arterial pH or $PO_2$.
- Mechanism: Sensitive to the pH of the cerebrospinal fluid (CSF).
- $CO_2$ freely diffuses from blood, across the blood-brain barrier (BBB), into the CSF.
- In CSF: $CO_2 + H_2O \rightarrow H_2CO_3 \rightarrow H^+ + HCO_3^-$.
- The resulting ↑ $[H^+]$ (↓ pH) in the CSF directly stimulates the receptors.
- This triggers an ↑ in ventilation to "blow off" excess $CO_2$.
⭐ In chronic hypercapnia (e.g., COPD), the kidneys compensate by ↑ serum $HCO_3^-$. This bicarbonate slowly enters the CSF, buffering the $H^+$ and blunting the central response. Respiration then becomes dependent on the hypoxic drive via peripheral chemoreceptors.
Peripheral Chemoreceptors - The Hypoxia Watchdogs
- Locations & Innervation:
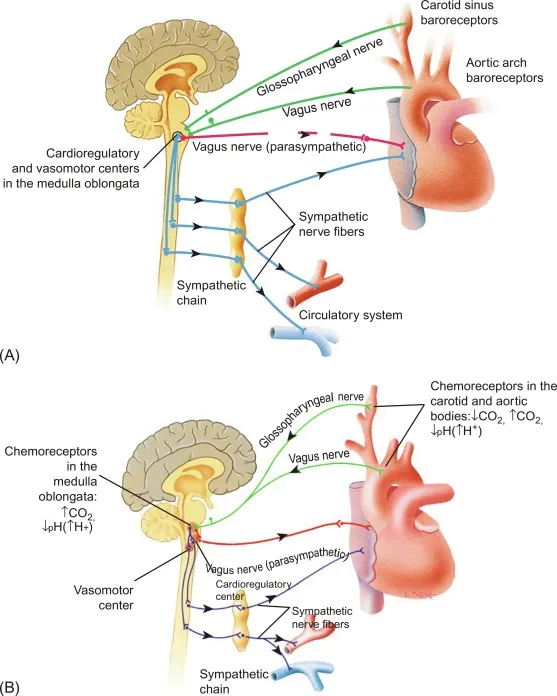
- Carotid Bodies: Located at the bifurcation of the common carotid arteries. Innervated by the glossopharyngeal nerve (CN IX).
- Aortic Bodies: Located on the aortic arch. Innervated by the vagus nerve (CN X).
- Primary Stimulus: Hypoxemia ($PaO_2$ < 60 mmHg). This is the most potent activator.
- Other Stimuli:
- ↑ Arterial $PCO_2$ (Hypercapnia)
- ↓ Arterial pH (Acidosis)
- Mechanism:
- Low $O_2$ inhibits K+ channels in glomus (Type I) cells, causing depolarization.
- Voltage-gated $Ca^{2+}$ channels open, leading to neurotransmitter release (e.g., Dopamine, ACh).
- Signal travels up afferent nerves to the medullary respiratory center, stimulating breathing.
⭐ The ventilatory response to hypoxemia is driven almost exclusively by the peripheral chemoreceptors, particularly the carotid bodies. Central chemoreceptors do not directly sense $O_2$ levels.
- Net Effect: Rapid increase in ventilation (rate and depth) to restore normal blood gas levels.
Integrated Response - Clinical Correlations
-
Chronic Obstructive Pulmonary Disease (COPD)
- Chronic hypercapnia ($↑P_{a}CO_2$) desensitizes central chemoreceptors.
- Ventilatory drive becomes dependent on peripheral chemoreceptor response to hypoxemia ($↓P_{a}O_2$).
- ⚠️ High-flow O₂ can suppress this "hypoxic drive," leading to respiratory arrest.
-
Congenital Central Hypoventilation Syndrome (CCHS)
- "Ondine's Curse": Impaired central response to hypercapnia, especially during sleep.
- Caused by mutations in the PHOX2B gene.
- Patients require ventilatory support during sleep.
⭐ In CCHS, the ventilatory response to hypoxia remains intact, but the response to hypercapnia is severely blunted or absent.
- Central chemoreceptors in the medulla are the primary drivers of respiration, stimulated by ↑ PaCO2 (via CSF [H+]).
- Peripheral chemoreceptors in the carotid and aortic bodies respond mainly to hypoxemia (PaO2 < 60 mmHg), but also to acidosis and ↑ PaCO2.
- In chronic COPD, the central response to CO2 is blunted, making hypoxic drive the main stimulus for breathing.
- Peripheral receptors sense dissolved O2 (PaO2), not O2-hemoglobin saturation (SaO2), thus are not stimulated in CO poisoning.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

