Sexual Response Cycle - The Pleasure Pathway
- Phases: Governed by autonomic nervous system changes leading to vasocongestion and myotonia. 📌 Mnemonic: Excite Plateau Orgasm Resolution.
- Excitement: Parasympathetic control.
- Clitoral erection & vaginal lubrication (transudate).
- Uterus elevates, pulling the cervix up ("tenting effect").
- Plateau: Intensification of excitement.
- Formation of the "orgasmic platform" (vasocongestion of the outer third of the vagina).
- Orgasm: Sympathetic & somatic control.
- Rhythmic contractions of the pelvic floor & orgasmic platform at ~0.8 sec intervals.
- Resolution: Return to baseline. Females do not have a refractory period.
⭐ The pudendal nerve provides key somatic innervation for genital sensation (clitoris, labia) and the voluntary muscular contractions of orgasm.

Neuro-hormonal Drivers - Love's Potion Commotion

-
Central Drivers: Orchestrated by the hypothalamus.
- Dopamine: Fuels libido and motivation; key to the brain's reward circuit (mesolimbic pathway).
- Norepinephrine: Drives arousal and excitement via sympathetic activation.
- Melanocortins: α-MSH acts on melanocortin receptors to ↑ sexual desire.
-
Peripheral & Central Modulators:
- Oxytocin: "Cuddle hormone"; promotes bonding and smooth muscle/uterine contractions during orgasm.
- Prolactin: Released post-orgasm; induces satiety and inhibits dopamine.
- Serotonin (5-HT): Generally exerts an inhibitory effect on sexual function.
⭐ High-Yield Fact: Selective serotonin reuptake inhibitors (SSRIs) frequently cause sexual dysfunction (e.g., anorgasmia, ↓ libido) by enhancing serotonin's inhibitory effects.
Anatomy of Arousal - The Hot Spots
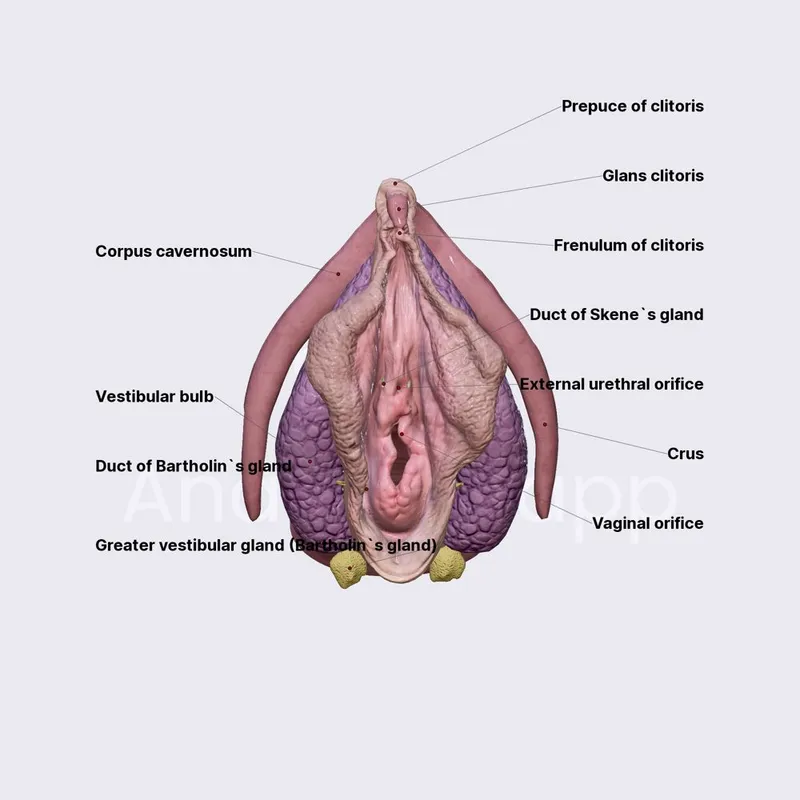
- Clitoris: Primary erogenous center, homologous to the glans penis.
- Composed of erectile tissue (corpora cavernosa) that engorges with blood.
- Glans is densely packed with nerve endings.
- Vestibular Glands: Provide lubrication during arousal.
- Bartholin's Glands: Located posterolaterally to the vaginal orifice; secrete mucus to lubricate the vestibule. Homologous to male bulbourethral glands.
- Skene's Glands: Located on the anterior vaginal wall, near the urethra; secrete fluid. Homologous to the male prostate.
- Vaginal Wall: Lubrication occurs via vasocongestion and plasma transudation through the epithelial lining.
⭐ The primary sensory innervation to the clitoris is via the dorsal nerve of the clitoris, a terminal branch of the pudendal nerve (S2-S4).
Sexual Dysfunction - When Sparks Don't Fly
- Definition: Persistent, recurrent problems with sexual response, desire, orgasm, or pain that cause personal distress.
- Etiology is Multifactorial:
- Psychological: Stress, anxiety, depression, relationship issues.
- Medical: Endometriosis, diabetes, thyroid disorders, pelvic floor dysfunction.
- Medications: Antidepressants (SSRIs), antihypertensives.
- Substance Use: Alcohol, opioids.
- Key Types:
- Hypoactive Sexual Desire Disorder: Low libido.
- Anorgasmia: Difficulty/inability to reach orgasm.
- Genito-Pelvic Pain/Penetration Disorder: Dyspareunia/vaginismus.
⭐ Selective serotonin reuptake inhibitors (SSRIs) are a notorious cause of anorgasmia in females.
- Arousal is parasympathetic (S2-S4), mediated by nitric oxide (NO), causing clitoral erection and vaginal lubrication.
- Orgasm is a sympathetic nervous system response, resulting in rhythmic pelvic muscle contractions.
- The clitoris, homologous to the male penis, is the primary erectile tissue responsible for pleasure.
- Bartholin's glands, homologous to male bulbourethral glands, secrete mucus for lubrication.
- Estrogen is key for maintaining vaginal blood flow, lubrication, and epithelial integrity.
- The pudendal nerve provides the primary sensory and motor innervation for the sexual response.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

