Follicular Phase - Prepping the Palace
- Initiation: Pulsatile GnRH from the hypothalamus stimulates the anterior pituitary to release FSH & LH.
- Follicle Growth: FSH stimulates a cohort of primordial follicles to develop. One becomes the dominant Graafian follicle.
- Estrogen Production: LH stimulates theca cells to produce androgens; FSH stimulates granulosa cells to convert these to estrogen.
- Endometrial Effect: Rising estrogen levels induce the proliferative endometrium.
⭐ In the late follicular phase, sustained high estrogen levels switch from negative to positive feedback on the pituitary, causing the LH surge that triggers ovulation.
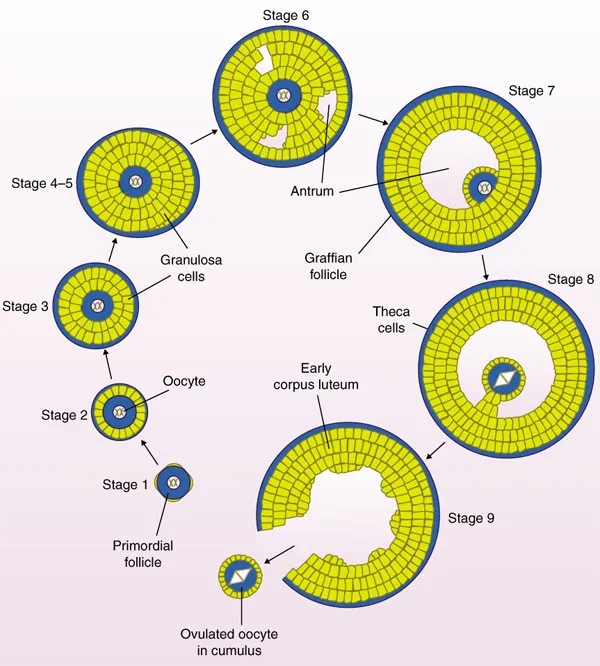
Ovulation - The Great Escape
- Trigger: A massive Luteinizing Hormone (LH) surge, which is induced by a sustained peak in estrogen from the mature Graafian follicle.
- Mechanism: Positive feedback loop.
- When estrogen levels are sustained >200 pg/mL for ~48 hours, the feedback on the hypothalamus (GnRH) and pituitary switches from negative to positive.
- This results in a dramatic ↑ LH release.
- Event: Occurs ~10-12 hours after the LH peak, typically on day 14.
- The primary oocyte completes meiosis I.
- The follicle ruptures, releasing the secondary oocyte.
- Clinical: May be associated with mittelschmerz (mid-cycle pain).
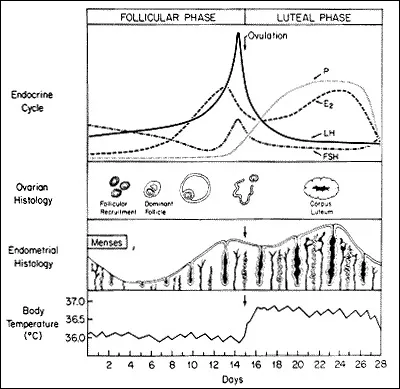
⭐ The LH surge is the critical trigger that allows the primary oocyte (arrested in prophase I) to resume meiosis and become a secondary oocyte (arrested in metaphase II).
Luteal Phase - The Waiting Game
- Duration: Fixed at 14 days, post-ovulation.
- Key Player: The corpus luteum (CL), formed from the ruptured follicle.
- Hormone: The CL primarily secretes progesterone.
- 📌 Progesterone = Promotes Gestation.
- Transforms the endometrium into a thick, vascular secretory endometrium, ideal for implantation.
- Two Fates:
- No Pregnancy: Without hCG, the CL degenerates into a scar (corpus albicans). ↓Progesterone triggers menstruation.
- Pregnancy: Embryonic hCG "rescues" the CL, maintaining progesterone until the placenta develops.
⭐ The luteal phase's fixed 14-day length is the most constant part of the menstrual cycle. Variability in total cycle length usually comes from the follicular phase.
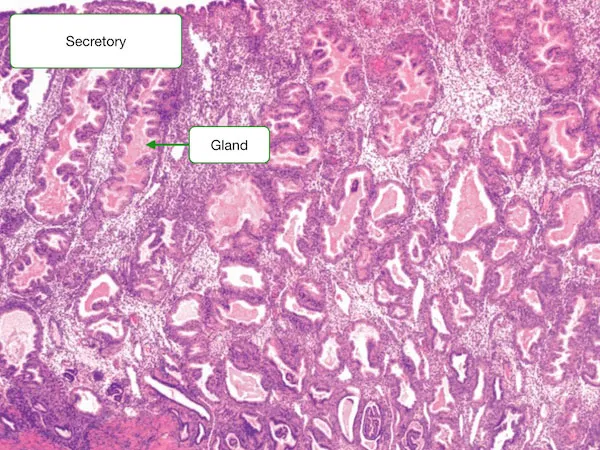
Hormonal Axis - The Conductors
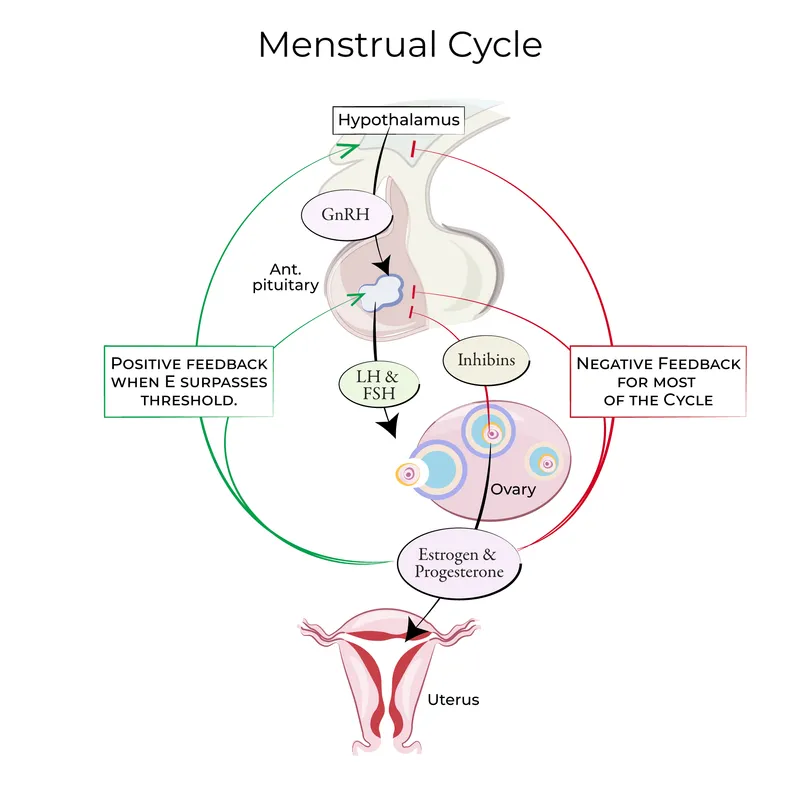
- The Hypothalamic-Pituitary-Ovarian (HPO) axis orchestrates the cycle via a hormonal cascade.
- Hypothalamus: Releases Gonadotropin-Releasing Hormone (GnRH) in pulses.
- Anterior Pituitary: GnRH stimulates Follicle-Stimulating Hormone (FSH) and Luteinizing Hormone (LH) release.
- Ovaries: Respond to FSH & LH, producing estrogen, progesterone, and inhibin.
- Feedback: Generally, estrogen/progesterone provide negative feedback. Inhibin specifically suppresses FSH.
⭐ Sustained high estrogen from a mature follicle switches feedback from negative to positive, causing the LH surge that triggers ovulation approximately 24-36 hours later.
High‑Yield Points - ⚡ Biggest Takeaways
- The follicular phase is estrogen-dominant and driven by FSH, leading to endometrial proliferation.
- A massive LH surge is the direct and essential trigger for ovulation.
- The luteal phase is progesterone-dominant, maintained by the corpus luteum.
- Menstruation is triggered by the withdrawal of progesterone and estrogen.
- If pregnancy occurs, hCG "rescues" the corpus luteum to continue progesterone production.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

