Overview - The Filtration Fraction

-
Calcium (Ca²⁺): Only the unbound, ionized fraction is filtered by the glomerulus.
- ~60% of plasma Ca²⁺ is filterable (ionized and complexed).
- ~40% is bound to albumin and other proteins; not filtered.
-
Phosphate (PO₄³⁻): Most plasma phosphate is filterable.
- ~85-90% is freely filtered (ionized or complexed with Na⁺, Ca²⁺, Mg²⁺).
- ~10-15% is protein-bound; not filtered.
⭐ Acidosis ↓ albumin binding → ↑ ionized Ca²⁺.
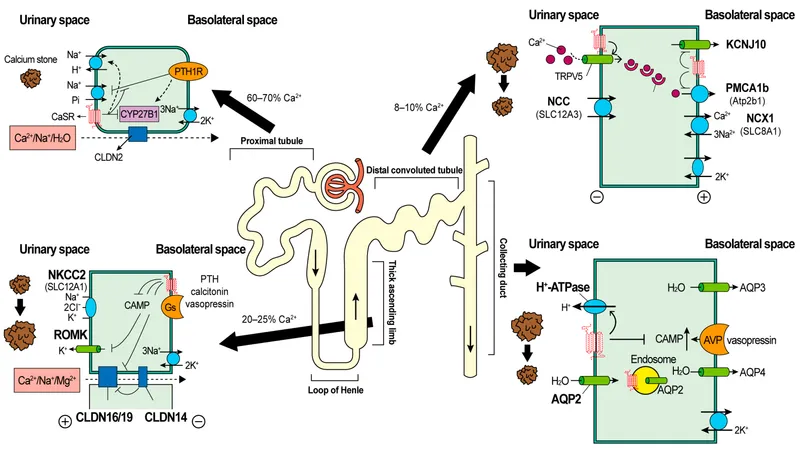
Proximal Tubule - The Bulk Reabsorber
- Calcium ($Ca^{2+}$) Reabsorption (~65-70%):
- Paracellular (~80%): The primary route, driven by the lumen-positive electrochemical gradient and solvent drag.
- Transcellular (~20%): A minor, active component.
- Phosphate ($PO_4^{3-}$) Reabsorption (~85%):
- Mediated by apical Na⁺/PO₄³⁻ cotransporters (NPT2a, NPT2c).
- PTH Regulation: PTH inhibits NPT2a/c activity, promoting their removal from the apical membrane. This action decreases phosphate reabsorption, leading to phosphaturia.
⭐ In humoral hypercalcemia of malignancy, PTH-related peptide (PTHrP) also inhibits NPT2a/c, causing significant renal phosphate wasting and hypophosphatemia.
TAL & DCT - Hormonal Fine‑Tuning
-
Thick Ascending Limb (TAL):
- Reabsorbs ~25% of filtered $Ca^{2+}$.
- Mechanism: Passive, paracellular, driven by the lumen-positive potential generated by the NKCC2 transporter.
- PTH indirectly enhances reabsorption here.
-
Distal Convoluted Tubule (DCT):
- Reabsorbs ~8% of filtered $Ca^{2+}$.
- Mechanism: Active, transcellular; the key site for fine-tuning.
- PTH Action:
- Binds to basolateral receptors.
- Upregulates and opens apical TRPV5 $Ca^{2+}$ channels.
- $Ca^{2+}$ binds to calbindin for transport to the basolateral membrane.
- Extruded into blood via Na⁺/$Ca^{2+}$ exchanger (NCX) and $Ca^{2+}$-ATPase (PMCA).
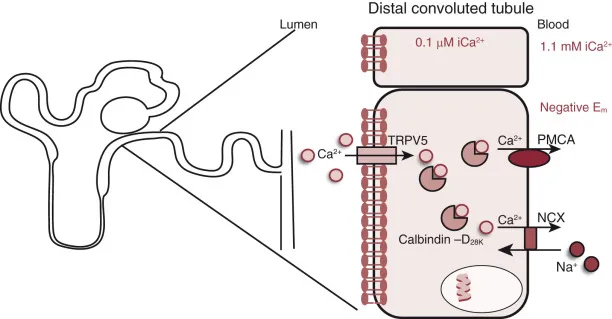
⭐ Thiazide diuretics block the Na⁺-Cl⁻ cotransporter (NCC) in the DCT. This reduces intracellular $Na^{+}$, which enhances the activity of the basolateral Na⁺/$Ca^{2+}$ exchanger, leading to increased $Ca^{2+}$ reabsorption and potential hypercalcemia.
Key Regulators - The Hormone Squad
| Hormone | Effect on Serum Ca²⁺ | Effect on Serum PO₄³⁻ | Renal Action (Ca²⁺ & PO₄³⁻) |
|---|---|---|---|
| PTH | ↑ | ↓ | ↑ Ca²⁺ reabsorption (DCT) ↓ PO₄³⁻ reabsorption (PCT) 📌 Phosphate Trashing Hormone |
| Calcitriol | ↑ | ↑ | ↑ Ca²⁺ & ↑ PO₄³⁻ reabsorption |
| FGF23 | ↔ | ↓ | ↓ PO₄³⁻ reabsorption ↓ Calcitriol synthesis |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | |||
| flowchart TD |
LowCa["<b>🩸 Low Serum Ca2+</b><br><span style='display:block; text-align:left; color:#555'>• Hypocalcemia state</span><span style='display:block; text-align:left; color:#555'>• Initial stimulus</span>"]
HighPTH["<b>⬆️ PTH Level</b><br><span style='display:block; text-align:left; color:#555'>• Parathyroid gland</span><span style='display:block; text-align:left; color:#555'>• Hormonal response</span>"]
subgraph Kidney["<b>🧬 Kidney Response</b>"]
CaRe["<b>⬆️ Ca2+ Reabsorp</b><br><span style='display:block; text-align:left; color:#555'>• Distal tubule</span><span style='display:block; text-align:left; color:#555'>• Conserve Calcium</span>"]
PORe["<b>⬇️ PO4 3- Reabsorp</b><br><span style='display:block; text-align:left; color:#555'>• Proximal tubule</span><span style='display:block; text-align:left; color:#555'>• High Phosphate loss</span>"]
Calc["<b>⬆️ Calcitriol</b><br><span style='display:block; text-align:left; color:#555'>• 1-alpha activation</span><span style='display:block; text-align:left; color:#555'>• Vitamin D3 increase</span>"]
end
LowCa --> HighPTH
HighPTH --> Kidney
style LowCa fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C
style HighPTH fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8
style CaRe fill:#EEFAFF, stroke:#DAF3FF, stroke-width:1.5px, rx:12, ry:12, color:#0369A1
style PORe fill:#EEFAFF, stroke:#DAF3FF, stroke-width:1.5px, rx:12, ry:12, color:#0369A1
style Calc fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
style Kidney fill:#F6F5F5, stroke:#E7E6E6, stroke-width:1.5px, color:#525252
> ⭐ FGF23 is the primary phosphaturic hormone. In chronic kidney disease (CKD), FGF23 levels rise early to maintain normal phosphate levels, but this contributes to suppressing Vitamin D activation.
## High‑Yield Points - ⚡ Biggest Takeaways
> * **Parathyroid hormone (PTH)** **increases serum Ca²⁺** while **decreasing serum PO₄³⁻**.
> * PTH **inhibits Na/PO₄ cotransport** in the **proximal tubule** and **stimulates Ca²⁺ reabsorption** in the **distal tubule**.
> * **Active Vitamin D (Calcitriol)** **increases absorption of both Ca²⁺ and PO₄³⁻** from the gut and kidney.
> * **FGF23** acts to **decrease serum phosphate** by promoting its excretion in the urine.
> * The **distal convoluted tubule (DCT)** is the primary site for **hormonally-regulated Ca²⁺ fine-tuning**.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

