Hemodynamic Principles - Pressure, Flow, & Pipes
- Ohm's Law for Fluids: Blood flow (Q) is driven by the pressure gradient (ΔP) and opposed by resistance (R).
- Formula: $Q = ΔP / R$
- Resistance (Poiseuille's Law): Primarily determined by vessel radius (r), length (L), and blood viscosity (η).
- $R hickapprox Lη / r^4$
- 📌 Halving the radius increases resistance 16-fold.
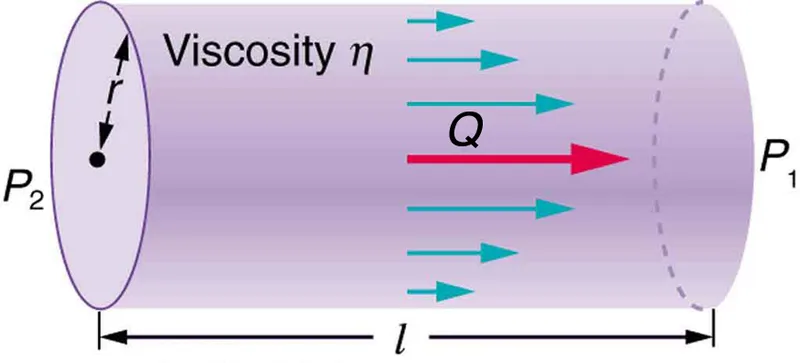
⭐ Arterioles are the principal sites of systemic vascular resistance (SVR) due to their ability to change radius, significantly impacting blood pressure regulation.
Invasive Monitoring - Lines, Waves & Pressures
- Arterial Line: For continuous BP monitoring & frequent arterial blood gas (ABG) sampling.
- Waveform: Systolic upstroke, peak pressure, dicrotic notch (aortic valve closure), diastolic runoff.
- Mean Arterial Pressure (MAP) = $⅓(SBP) + ⅔(DBP)$. Target > 65 mmHg.
- Central Venous Pressure (CVP): Measures right atrial pressure; a proxy for RV preload.
- Normal: 2-8 mmHg.
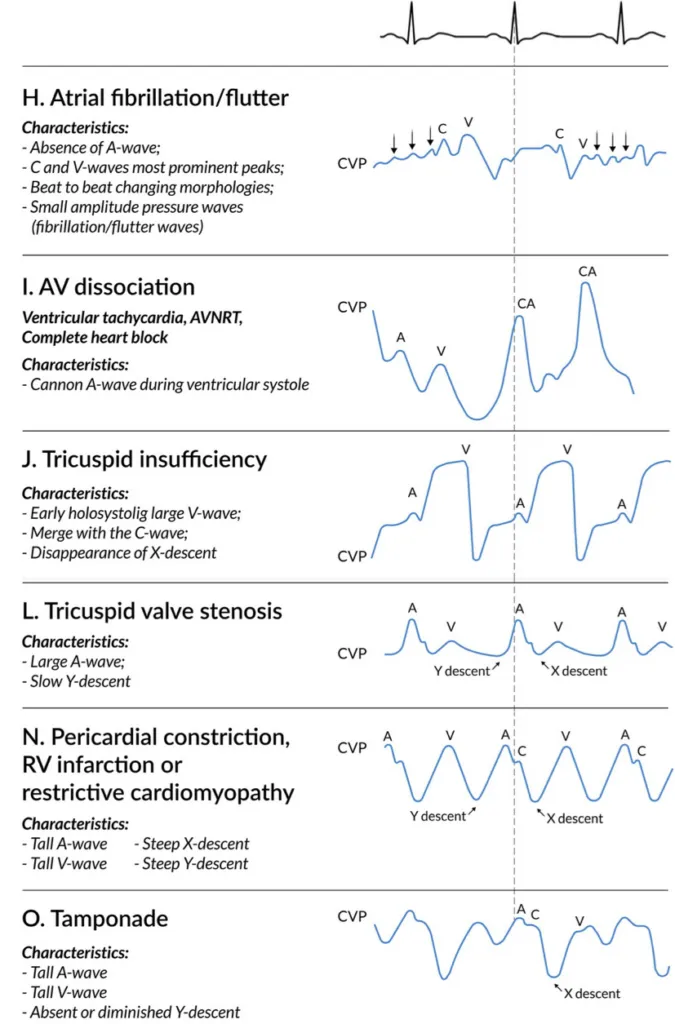
- Waveform: a (atrial contraction), c (ventricular contraction/tricuspid bulge), x (atrial relaxation), v (venous filling), y (atrial emptying).
- Pulmonary Artery (PA) Catheter:
- Measures PCWP (wedge pressure), a proxy for left atrial pressure.
- Normal PCWP: 6-12 mmHg.
⭐ Cannon a waves on CVP tracing are seen in conditions where the right atrium contracts against a closed tricuspid valve (e.g., complete heart block, ventricular tachycardia).
The Swan-Ganz - A Float Through The Heart
-
A pulmonary artery catheter (PAC) providing a continuous, real-time assessment of cardiac function and volume status by measuring pressures as it floats through the right heart.
-
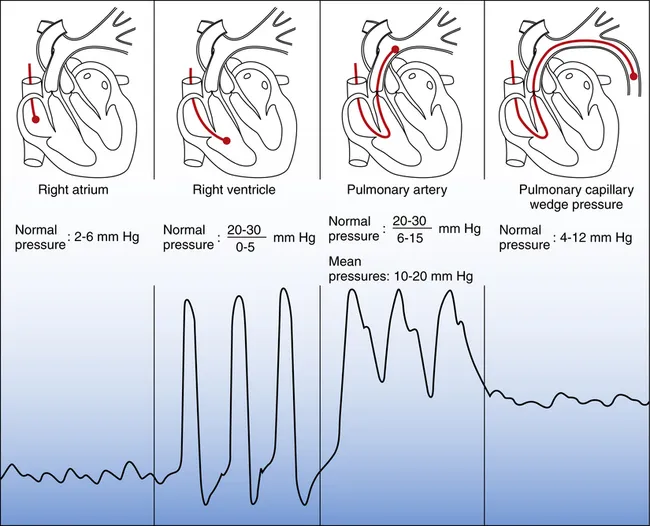
Catheter Path & Typical Pressures (mmHg):
- Right Atrium (RA): Measures central venous pressure (CVP). Normal: 2-8.
- Right Ventricle (RV): Sharp, pulsatile waveform. Normal: 25/5.
- Pulmonary Artery (PA): Dicrotic notch appears. Normal: 25/10.
- Wedge (PCWP): Balloon inflation occludes a PA branch. Normal: <12.
⭐ PCWP provides an indirect estimate of Left Atrial Pressure (LAP), a key indicator of left ventricular preload and mitral valve function.
Shock Profiles - Decoding The Disaster
| Shock Type | CVP/PCWP | CO | SVR |
|---|---|---|---|
| Hypovolemic | ↓ | ↓ | ↑ |
| Cardiogenic | ↑ | ↓ | ↑ |
| Distributive | ↓ | ↑ (early) | ↓ |
| Obstructive | ↑ | ↓ | ↑ |
- CO: Cardiac Output
- SVR: Afterload
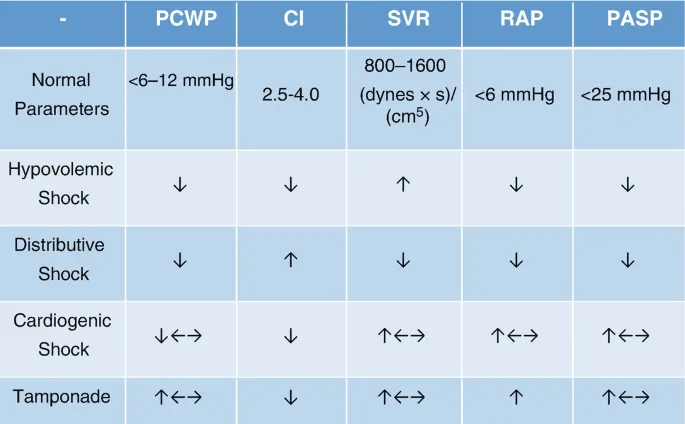
⭐ In early septic shock (distributive), cardiac output is uniquely high while SVR plummets. Mixed venous oxygen saturation (SvO2) is often >70% due to impaired cellular O₂ extraction.
High‑Yield Points - ⚡ Biggest Takeaways
- Pulmonary Artery Catheter (PAC) directly measures CVP, PAP, and PCWP, and allows for CO calculation.
- PCWP is a reliable estimate of left atrial pressure and left ventricular end-diastolic pressure (LVEDP) in the absence of mitral stenosis.
- Cardiac Output (CO) is most commonly determined via thermodilution.
- Systemic Vascular Resistance (SVR) is a calculated variable representing afterload, not directly measured.
- Mixed venous oxygen saturation (SvO2) reflects the balance of oxygen delivery and consumption.
- Differentiating shock states relies on interpreting patterns: cardiogenic shock shows ↑PCWP, ↓CO; septic shock (early) shows ↓SVR, ↑CO.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

