Juxtaglomerular Apparatus - The Kidney's Sensor
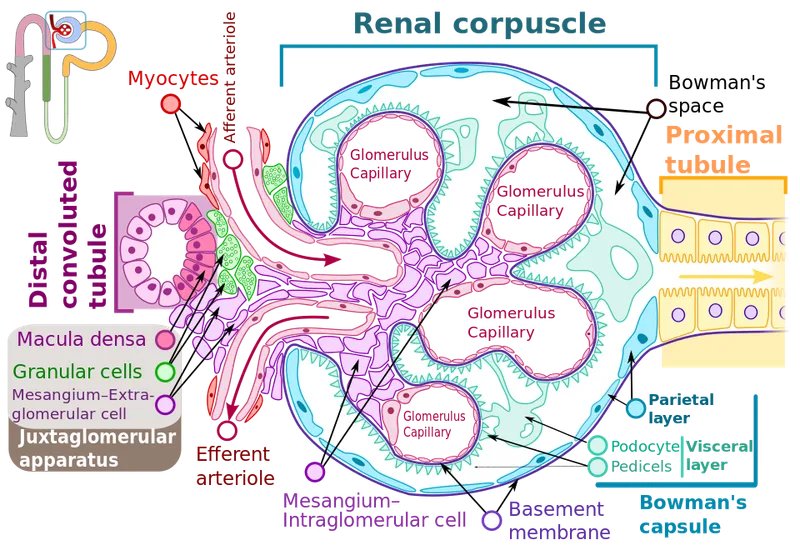
- Location: A specialized structure at the vascular pole of the glomerulus, where the Distal Convoluted Tubule (DCT) contacts the afferent arteriole.
- Components:
- Macula Densa: Modified DCT epithelial cells. They are chemoreceptors sensing tubular fluid [NaCl].
- Juxtaglomerular (JG) Cells: Modified smooth muscle cells in the afferent arteriole wall. They are mechanoreceptors that synthesize, store, and secrete renin.
- Extraglomerular Mesangial Cells (Lacis cells): Transmit signals between the macula densa and JG cells.
⭐ High-Yield: Adenosine is the primary paracrine signal released by the macula densa in response to ↑ NaCl. It causes vasoconstriction of the afferent arteriole, reducing GFR.
TGF Mechanism - The Feedback Loop
- Trigger: An increase in Glomerular Filtration Rate (GFR) leads to ↑ delivery of NaCl to the distal tubule.
- Sensor: The macula densa cells in the Juxtaglomerular Apparatus (JGA) detect this ↑ tubular [NaCl].
- Signal: In response, macula densa cells release vasoactive substances, primarily ATP and adenosine.
- Effector: These paracrine signals cause vasoconstriction of the adjacent afferent arteriole.
- Result: Afferent constriction ↑ resistance, which ↓ renal blood flow and ↓ glomerular hydrostatic pressure, returning GFR to normal.
⭐ High-Yield: Adenosine is the key mediator causing afferent vasoconstriction in TGF. This is why caffeine, an adenosine antagonist, can interfere with this regulatory process, leading to a temporary increase in GFR.
TGF Modulators - Turning the Dial
-
↑ TGF Sensitivity (↓ GFR): Macula densa is more sensitive to NaCl, enhancing afferent vasoconstriction.
- Adenosine
- Angiotensin II
- Thromboxane A2
- Volume depletion
-
↓ TGF Sensitivity (↑ GFR): Macula densa is less sensitive to NaCl, blunting afferent vasoconstriction.
- Nitric Oxide (NO)
- Atrial Natriuretic Peptide (ANP)
- Loop diuretics (furosemide)
- High dietary protein
⭐ Exam Favorite: NSAIDs inhibit prostaglandins (which normally blunt TGF). This leads to unopposed afferent arteriole vasoconstriction, ↑ TGF sensitivity, and a ↓ GFR. This effect is most pronounced in patients with underlying renal hypoperfusion (e.g., heart failure, cirrhosis).
High‑Yield Points - ⚡ Biggest Takeaways
- Tubuloglomerular feedback (TGF) is a primary mechanism for GFR autoregulation.
- The macula densa in the distal tubule senses NaCl concentration as a proxy for GFR.
- High NaCl (high GFR) causes macula densa cells to release ATP and adenosine.
- These paracrine factors cause vasoconstriction of the afferent arteriole.
- This reduces renal blood flow and returns GFR to normal.
- Low NaCl (low GFR) has the opposite effect, causing vasodilation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

