Starling Forces - The Pressure Players
📌 Mnemonic: PUSH forces (hydrostatic) vs. PULL forces (oncotic). Filtration happens when PUSH out > PUSH in + PULL in.
| Forces Favoring Filtration | Forces Opposing Filtration |
|---|---|
| * Glomerular Hydrostatic Pressure ($P_{GC}$): Blood pressure in glomerular capillaries. Pushes fluid OUT of capillaries. Value: ≈ 60 mmHg | * Bowman’s Capsule Hydrostatic Pressure ($P_{BS}$): Fluid pressure in Bowman’s space. Pushes fluid back INTO capillaries. Value: ≈ 18 mmHg * Glomerular Oncotic Pressure ($\pi_{GC}$): Protein pressure in glomerular blood. PULLS fluid back INTO capillaries. Value: ≈ 32 mmHg |
⭐ Under normal conditions, the filtrate is essentially protein-free, making the oncotic pressure in Bowman's space (π_BS) effectively zero.
The Filtration Equation - Summing It All Up
-
Net Filtration Pressure (NFP) is the net pressure driving filtration, determined by the sum of Starling forces.
- Equation: $NFP = (P_{GC} - P_{BS}) - (π_{GC} - π_{BS})$
- $P_{GC}$ & $π_{BS}$ favor filtration.
- $P_{BS}$ & $π_{GC}$ oppose filtration ($π_{BS}$ is normally negligible).
-
Glomerular Filtration Rate (GFR) is the total volume of fluid filtered from the glomeruli into Bowman's space per unit time.
- Equation: $GFR = K_f \times NFP$
- Kf: The filtration coefficient, reflecting capillary permeability and surface area.
⭐ The filtration coefficient (Kf) is not static; it decreases in glomerular diseases (e.g., glomerulonephritis, diabetic nephropathy) that reduce the surface area available for filtration.
Arteriolar Tone - Dialing the Pressure
By adjusting the resistance of the afferent and efferent arterioles, the kidney tightly controls glomerular capillary pressure ($P_{GC}$) and renal plasma flow (RPF), thereby regulating GFR. The relationship is captured by the Filtration Fraction: $FF = GFR / RPF$.
| Arteriolar Action | Effect on RPF | Effect on $P_{GC}$ | Effect on GFR |
|---|---|---|---|
| Afferent Constriction | ↓↓ | ↓ | ↓ |
| Afferent Dilation | ↑↑ | ↑ | ↑ |
| Efferent Constriction | ↓ | ↑↑ | ↑ |
| Efferent Dilation | ↑ | ↓↓ | ↓ |
⭐ Angiotensin II preferentially constricts the efferent arteriole, a key mechanism to preserve GFR when renal perfusion is low.
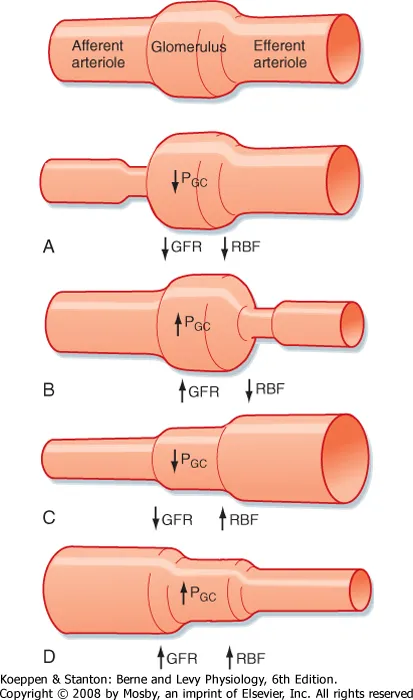
- Net filtration pressure (NFP) is the sum of Starling forces and dictates the glomerular filtration rate (GFR).
- Glomerular hydrostatic pressure (PGC) is the primary force favoring filtration.
- Glomerular oncotic pressure (πGC) is the primary force opposing filtration.
- Afferent arteriole constriction (e.g., NSAIDs) ↓ PGC and ↓ GFR.
- Efferent arteriole constriction (e.g., Angiotensin II) ↑ PGC and initially ↑ GFR.
- Ureteral obstruction ↑ Bowman's capsule hydrostatic pressure (PBS), which ↓ GFR.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

