RAAS - The Pressure Player
Triggered by ↓ renal blood pressure or ↓ Na⁺ delivery to the macula densa. The juxtaglomerular (JG) cells release renin, initiating a cascade to restore blood pressure and GFR.
- Angiotensin II (AT-II) Actions:
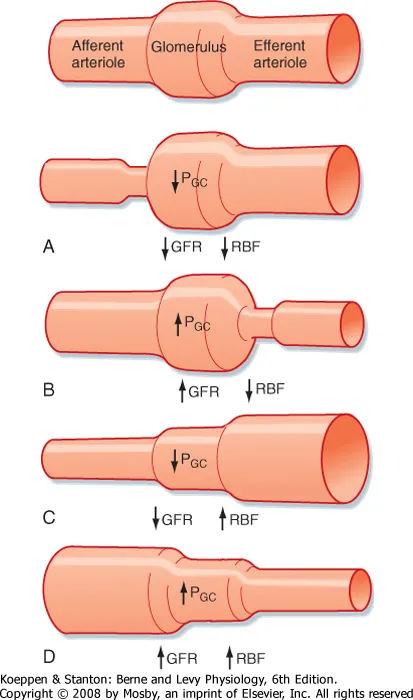
- Potent systemic vasoconstrictor → ↑ Mean Arterial Pressure.
- Preferentially constricts the efferent arteriole > afferent arteriole.
- Increases glomerular hydrostatic pressure ($P_{GC}$) → ↑ GFR.
- Increases filtration fraction (FF = GFR/RPF).
- Stimulates aldosterone release from the adrenal cortex → ↑ Na⁺ and H₂O reabsorption.
- Promotes ADH secretion and thirst.
⭐ In bilateral renal artery stenosis, giving an ACE inhibitor (e.g., lisinopril) can cause acute kidney injury. It blocks the vital efferent arteriole constriction needed to maintain GFR, leading to a precipitous drop.
ANP & BNP - The Volume Relievers
- Source: Released from atrial (ANP) & ventricular (BNP) myocytes in response to ↑ stretch (volume expansion).
- Primary Action: Counteract volume overload by promoting natriuresis and diuresis.
- Renal Effects on GFR:
- Dilates afferent arteriole → ↑ Renal Blood Flow.
- Constricts efferent arteriole.
- Both actions synergistically ↑ Glomerular Hydrostatic Pressure → ↑ GFR.
- Other Renal Actions:
- Inhibits renin secretion.
- Reduces Na⁺ reabsorption in the collecting duct.
⭐ Clinically, BNP levels are a crucial biomarker in diagnosing and assessing the severity of heart failure; a level > 100 pg/mL is a key threshold.
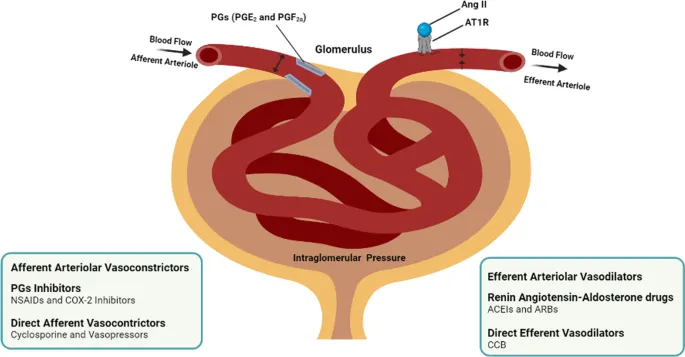
Prostaglandins - The Local Protectors
- Source: Synthesized locally within the kidneys, primarily Prostaglandins E₂ (PGE₂) and I₂ (PGI₂).
- Primary Action: Vasodilation of the afferent arteriole.
- This action ↑ Renal Blood Flow (RBF) and helps maintain the Glomerular Filtration Rate (GFR).
- Crucially counteracts potent vasoconstrictors (e.g., Angiotensin II, norepinephrine), especially during periods of systemic hypotension or volume depletion.
- Clinical Significance:
- Non-steroidal anti-inflammatory drugs (NSAIDs) inhibit prostaglandin synthesis.
- This inhibition removes the protective vasodilation, leading to unopposed afferent arteriole constriction, ↓ RBF, and ↓ GFR.
⭐ In patients with reduced effective renal perfusion (e.g., heart failure, dehydration), NSAID use can precipitate acute kidney injury by blocking this essential compensatory mechanism.
High‑Yield Points - ⚡ Biggest Takeaways
- Angiotensin II preferentially constricts the efferent arteriole, preserving GFR; high levels constrict both, ↓ GFR.
- ANP and BNP dilate the afferent arteriole while constricting the efferent, leading to an ↑ in GFR.
- Prostaglandins maintain GFR by dilating the afferent arteriole; NSAIDs block this protective vasodilation.
- Sympathetic stimulation strongly constricts the afferent arteriole, causing a significant ↓ in both GFR and RBF.
- Endothelin is a potent vasoconstrictor of both arterioles, which ↓ GFR.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

