Filtration Fraction - The Kidney's Quota
- The proportion of renal plasma flow (RPF) that is filtered across the glomerulus to form glomerular filtrate (GFR).
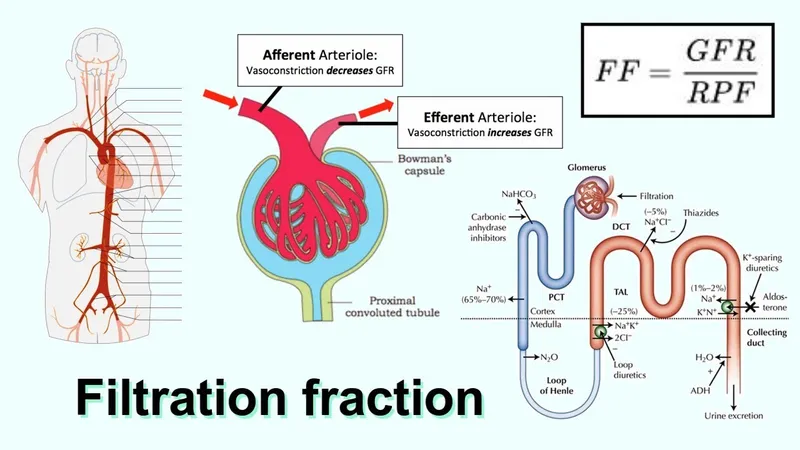
- Formula: $FF = GFR / RPF$.
- Normal FF is ~20%.
- Factors increasing FF:
- Efferent arteriole constriction (e.g., Angiotensin II) → ↓ RPF > ↓ GFR → ↑ FF.
- Factors decreasing FF:
- Efferent arteriole dilation (e.g., ACE inhibitors) → ↑ RPF & ↓ GFR → ↓ FF.
⭐ With significant renal artery stenosis, RPF is low. The kidney compensates by ↑ Angiotensin II, causing efferent constriction to ↑ FF and preserve GFR.
FF Regulation - Arteriole Tug-of-War
Filtration Fraction (FF) is the proportion of renal plasma flow (RPF) that becomes glomerular filtrate (GFR). It's a dynamic balance, primarily adjusted by arteriolar tone.
$FF = GFR / RPF$
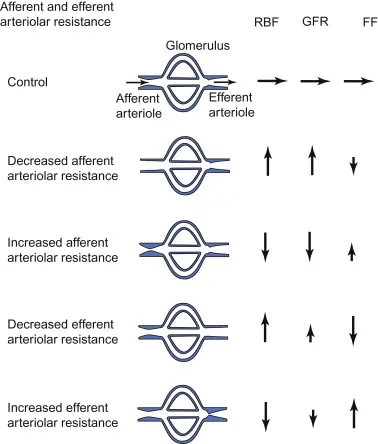
- Afferent Arteriole (Inflow Control):
- Constriction (e.g., NSAIDs): ↓ RPF, ↓ GFR → FF is variable.
- Dilation (e.g., Prostaglandins): ↑ RPF, ↑ GFR → FF is variable.
- Efferent Arteriole (Outflow Control):
- Constriction (e.g., Angiotensin II): ↓ RPF, ↑ GFR → ↑↑ FF.
- Dilation (e.g., ACE inhibitors): ↑ RPF, ↓ GFR → ↓↓ FF.
⭐ ACE inhibitors (e.g., lisinopril) cause efferent arteriole dilation, reducing GFR. This is protective in diabetic nephropathy by decreasing intraglomerular pressure, but can cause acute kidney injury in bilateral renal artery stenosis.
Clinical Correlations - FF in Flux
-
Filtration Fraction (FF) represents the proportion of renal plasma flow (RPF) that is filtered to become glomerular filtrate (GFR).
-
The standard formula is $FF = GFR / RPF$. Normal FF is approximately 20%.
-
Factors Increasing FF (↑ FF):
- Typically result from a decrease in RPF without a proportional drop in GFR.
- Efferent Arteriole Constriction:
- Angiotensin II: Constricts the efferent arteriole more than the afferent, leading to ↓ RPF and a slight ↑ GFR, thus significantly ↑ FF.
- Reduced Renal Perfusion:
- Conditions like renal artery stenosis or severe dehydration decrease RPF. The body compensates via RAAS, constricting the efferent arteriole to preserve GFR, thereby ↑ FF.
-
Factors Decreasing FF (↓ FF):
- Occur with efferent arteriole dilation or when RPF increases more than GFR.
- Efferent Arteriole Dilation:
- ACE inhibitors & ARBs: By blocking angiotensin II, these drugs dilate the efferent arteriole. This causes ↓ GFR and ↑ RPF, leading to a ↓↓ FF.
- Volume Expansion / IV Fluids:
- Dilutes plasma proteins, ↓ oncotic pressure, and ↑ RPF, resulting in a ↓ FF.
⭐ In bilateral renal artery stenosis, ACE inhibitors can precipitate acute renal failure. They eliminate the compensatory Angiotensin II-mediated efferent vasoconstriction, causing a sharp, dangerous drop in GFR.
High‑Yield Points - ⚡ Biggest Takeaways
- Filtration Fraction (FF) is the ratio of GFR to RPF (FF = GFR/RPF), with a normal value of ~20%.
- Represents the proportion of renal plasma flow that gets filtered across the glomerular capillaries.
- Angiotensin II preferentially constricts the efferent arteriole, which significantly increases FF.
- ACE inhibitors and ARBs dilate the efferent arteriole, leading to a decrease in FF.
- FF is increased in states of low renal blood flow, like severe dehydration, to help preserve GFR.
- A high FF raises oncotic pressure in peritubular capillaries, promoting tubular reabsorption.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

