Indications & Contraindications - Why Stress & When to Stop
-
Indications for Testing:
- Diagnosis of obstructive CAD in symptomatic patients.
- Prognostic assessment in known CAD.
- Evaluation of exercise capacity & response to therapy.
- Pre-operative risk assessment.
-
Absolute Contraindications (Do NOT test):
- Acute MI (within 2 days).
- High-risk unstable angina.
- Uncontrolled, symptomatic arrhythmias.
- Severe, symptomatic aortic stenosis.
- Acute pulmonary embolism, myocarditis, or aortic dissection.
-
Absolute Termination Criteria (STOP test):
- ST elevation ≥1.0 mm.
- Sustained V-tach.
- Systolic BP drop >10 mmHg with other ischemic signs.
- CNS symptoms (e.g., ataxia, near-syncope).
⭐ The Duke Treadmill Score (DTS) is a key prognostic tool combining exercise time, ST deviation, and angina index. A score ≥5 indicates low risk, while ≤-11 indicates high risk.
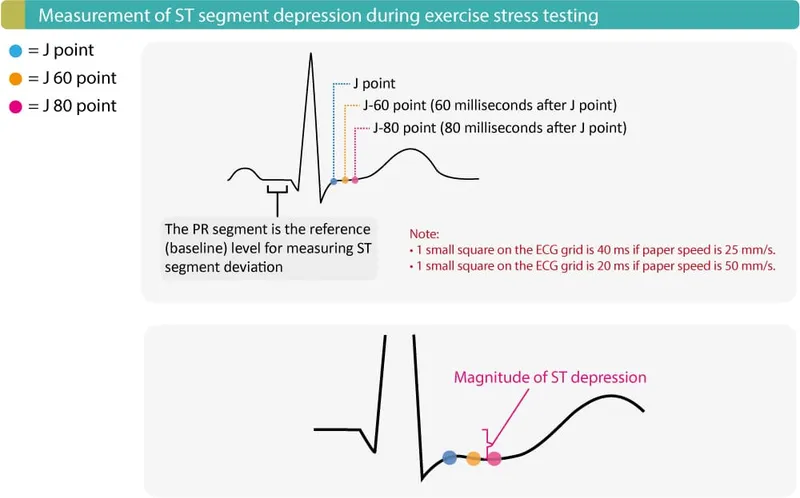
Physiologic Response - The Body Under Pressure
- Cardiovascular:
- CO: ↑ significantly ($CO = HR \times SV$).
- HR: ↑ linearly with workload (Max HR ≈ $220 - \text{age}$).
- SV: ↑, then plateaus at 40-60% $VO_2$ max.
- BP: Systolic ↑; Diastolic stable/↓. Widened pulse pressure.
- TPR: ↓ due to muscle vasodilation.
- Respiratory:
- Minute Ventilation ($V_E$): ↑ dramatically.
- V/Q Matching: Improves for efficient gas exchange.
- Arterial Gases: $PaO_2$ & $PaCO_2$ stable until anaerobic threshold.
- Metabolic:
- $VO_2$ (Oxygen Consumption): ↑ linearly until $VO_2$ max.
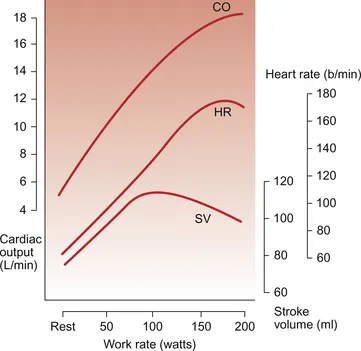
⭐ A key indicator of cardiac stress limitation is an abnormal BP response: a drop in systolic BP or failure to rise >10 mmHg with increasing workload suggests potential myocardial ischemia or LV dysfunction.
Protocols & Interpretation - Reading the Stress Signals
- Protocols: Bruce (standard) & Modified Bruce (for deconditioned/elderly patients). Both incrementally increase speed and grade every 3 minutes.
- Key Monitored Parameters: Heart Rate (HR), Blood Pressure (BP), continuous ECG, and Rate of Perceived Exertion (RPE).
- Termination Criteria (Absolute):
- SBP drop >10 mmHg with other evidence of ischemia.
- Moderate-to-severe angina.
- CNS symptoms (e.g., ataxia, dizziness).
- Sustained V-tach or ST-elevation (≥1.0 mm).
- Interpretation:
- HR: Failure to reach >85% of age-predicted max ($220 - \text{age}$) indicates chronotropic incompetence.
- ECG: Horizontal or downsloping ST depression ≥1 mm suggests ischemia.
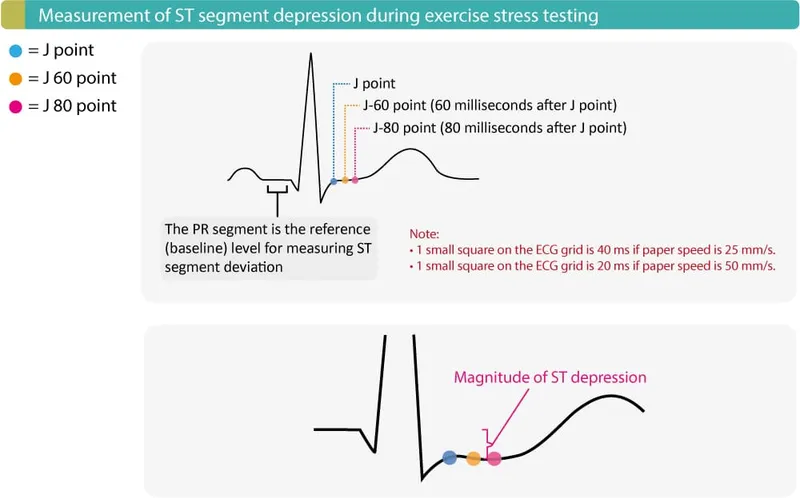
⭐ The workload (in METs) at which ST depression occurs is a key prognostic marker. Ischemia at a low workload (<5 METs) indicates a higher risk of severe coronary artery disease.
Prognostic Scores - The Duke Score
- Integrates exercise time, ST-segment deviation, and angina symptoms to estimate 5-year mortality risk.
- Formula: $DTS = \text{Exercise Time (mins)} - (5 \times \text{ST deviation (mm)}) - (4 \times \text{Angina Index})$
- Angina Index: 0 (none), 1 (non-limiting), 2 (exercise-limiting).
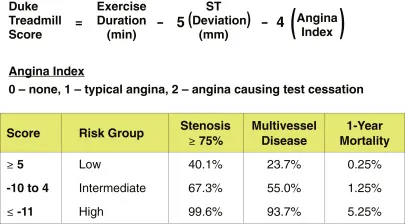
⭐ A high-risk score of ≤ -11 is a strong indication for considering coronary angiography to assess for significant coronary artery disease.
High‑Yield Points - ⚡ Biggest Takeaways
- Maximal heart rate is estimated as 220 − age; achieving >85% is a key goal for a valid stress test.
- VO₂ max is the gold standard for cardiorespiratory fitness, representing maximal oxygen uptake.
- Metabolic Equivalent (MET) is a key unit; 1 MET ≈ 3.5 mL O₂/kg/min (resting oxygen consumption).
- Key reasons to terminate a stress test include a drop in systolic BP, significant ST-segment changes, or severe angina.
- Normally, systolic BP increases with exercise, while diastolic BP remains stable or slightly decreases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

