P Wave Anatomy - The Atrial Kickstart
- Represents the depolarization of both atria, initiated by the Sinoatrial (SA) node.
- Normal Duration: < 0.12 seconds (3 small squares).
- Normal Amplitude: < 2.5 mm in limb leads.
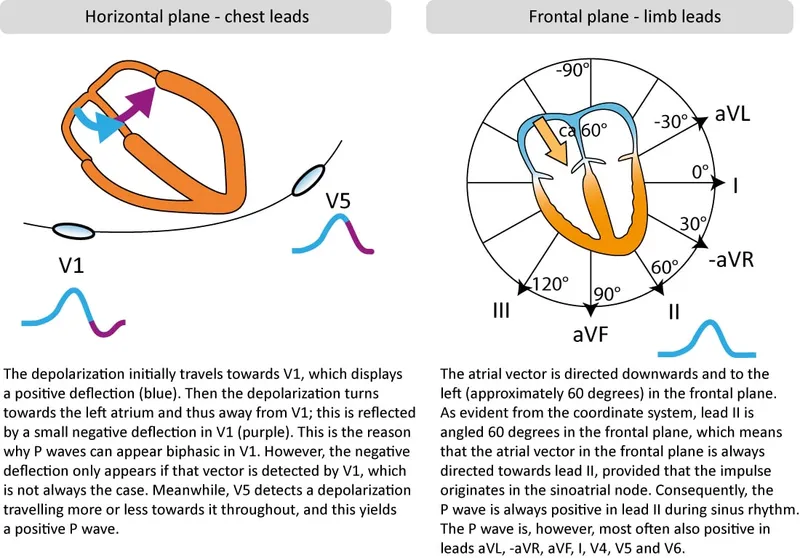
- Sequence of Depolarization:
- First half of P wave: Right Atrium (RA) depolarization.
- Second half of P wave: Left Atrium (LA) depolarization.
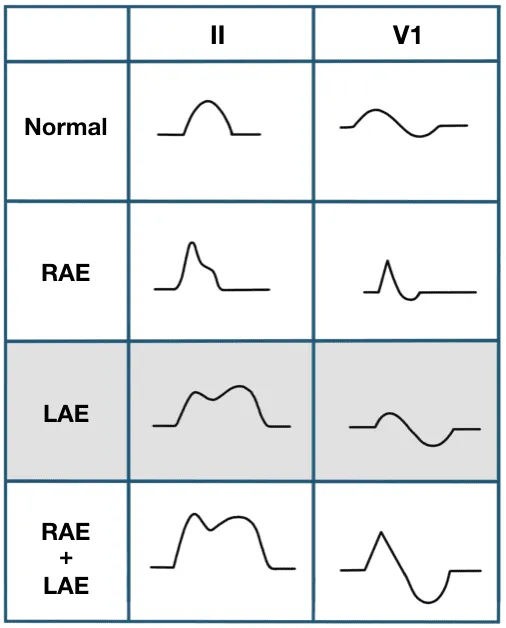
⭐ In Lead II, Right Atrial Enlargement (RAE) causes tall, peaked P waves (P pulmonale, >2.5mm). Left Atrial Enlargement (LAE) causes a wide, notched P wave (P mitrale, >0.12s).
Right Atrial Enlargement - The 'P' in Pulmonale
- Also known as "P pulmonale," reflecting its common origin from pulmonary disease, which increases right atrial pressure.
- ECG Hallmark: A tall, peaked P wave, best visualized in the inferior leads (II, III, and aVF).
- Diagnostic Criteria:
- P wave amplitude >2.5 mm in lead II.
- P wave duration remains normal (<0.12 s).
- 📌 The 'P' in Pulmonale reminds you of the Peaked P wave.
- Primary Causes: Conditions leading to right ventricular overload, such as COPD, pulmonary hypertension, and tricuspid valve disease.
⭐ The classic cause is cor pulmonale (right-sided heart failure from lung disease), making a patient's respiratory history crucial for interpretation.
Left Atrial Enlargement - The 'M' in Mitrale
- Pathophysiology: Increased left atrial pressure or volume overload causes delayed depolarization of the enlarged left atrium.
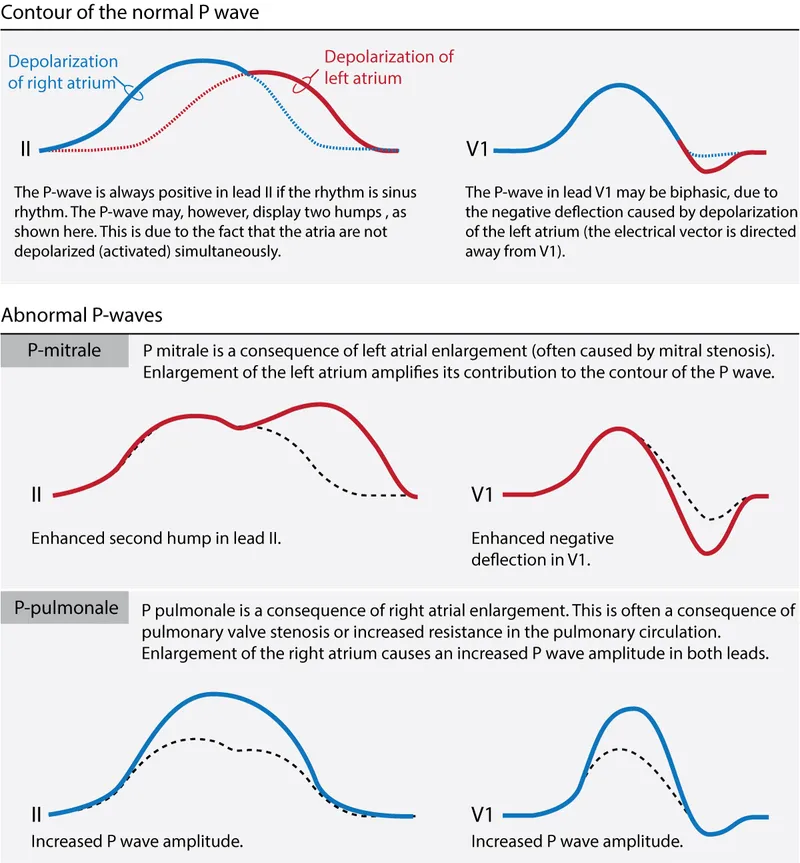
- ECG Findings ("P mitrale"):
- Lead II: Notched, 'M'-shaped P wave with duration > 0.12s. The interval between the two peaks is > 0.04s.
- Lead V1: Biphasic P wave where the terminal negative portion is > 1 mm deep and > 0.04s in duration.
- 📌 Mnemonic: The M-shape in lead II suggests Mitral valve disease causing LAE.
⭐ Left atrial enlargement on an ECG is an independent predictor of developing atrial fibrillation, stroke, and cardiovascular mortality.
Ectopic Rhythms - Rogue Pacemakers
- Premature Atrial Contraction (PAC): An early, ectopic P wave with abnormal morphology, followed by a QRS. Often feels like a "skipped beat."
- Wandering Atrial Pacemaker (WAP):
- Heart rate <100 bpm.
- ≥3 distinct P wave morphologies.
- Irregular rhythm.
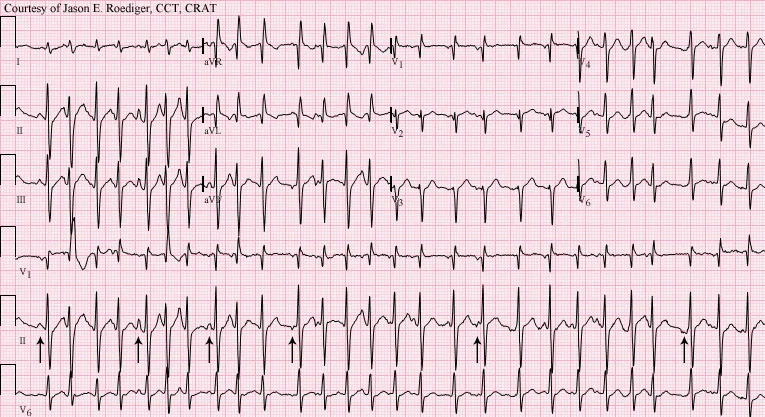
⭐ Multifocal Atrial Tachycardia (MAT) is strongly associated with severe pulmonary disease, like a COPD exacerbation. Management focuses on the underlying lung condition, not just rate control.
High‑Yield Points - ⚡ Biggest Takeaways
- The P wave represents the sequential depolarization of the atria, initiated by the SA node.
- Normal morphology is upright in leads I, II, and aVF, and often biphasic in lead V1.
- Normal duration is <0.12 seconds (<3 small squares); amplitude is <2.5 mm.
- Tall, peaked P waves (P pulmonale) are a sign of Right Atrial Enlargement (RAE).
- Notched, wide P waves (P mitrale) suggest Left Atrial Enlargement (LAE).
- Absent P waves are a hallmark of atrial fibrillation and junctional rhythms.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

