Baroreceptors & Chemoreceptors - The Body's BP Spies
-
Baroreceptors (Stretch): Rapid, moment-to-moment BP control.
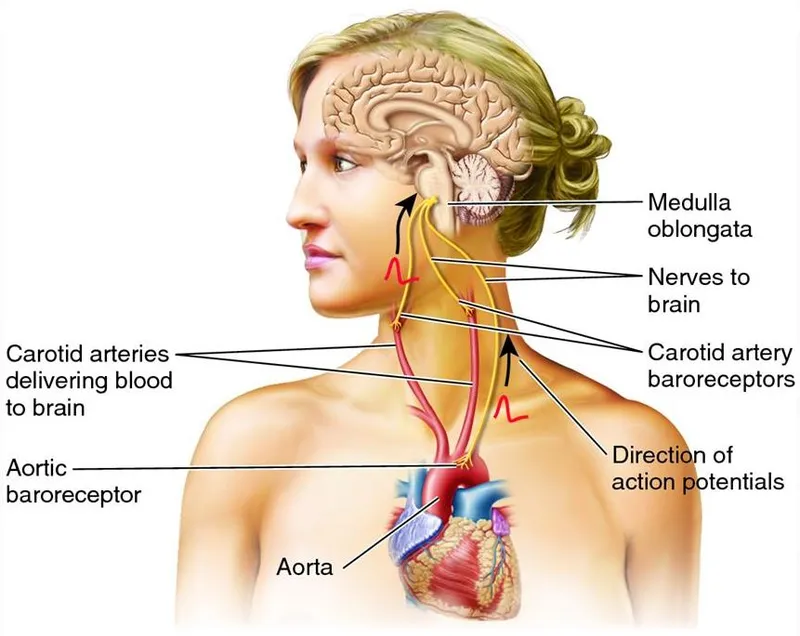
- Locations: Carotid Sinus (glossopharyngeal n. - CN IX), Aortic Arch (vagus n. - CN X).
- Mechanism: ↑ Arterial stretch → ↑ firing → inhibits sympathetic & stimulates parasympathetic output → ↓ HR, ↓ contractility, vasodilation → ↓ BP.
-
Chemoreceptors (Chemical): Respond primarily to hypoxia.
- Locations: Carotid & Aortic bodies.
- Mechanism: Sense ↓ PaO₂, ↑ PaCO₂, or ↓ pH → ↑ sympathetic firing → vasoconstriction & ↑ HR → ↑ BP.
⭐ Cushing Reflex: Increased intracranial pressure compresses cerebral arterioles, causing ischemia. The CNS triggers a powerful sympathetic response (hypertension) to restore perfusion, which in turn stretches peripheral baroreceptors, causing a reflex bradycardia.
RAAS - The Salt & Squeeze System

Activated by ↓ renal perfusion to increase blood pressure.
- Angiotensin II (The “Squeeze”):
- Potent vasoconstrictor → ↑ SVR.
- Stimulates aldosterone & ADH release.
- Aldosterone (The “Salt”):
- Acts on collecting tubule.
- ↑ Na+ reabsorption (water follows).
- ↑ K+ & H+ excretion.
⭐ ACE is abundant in the lungs; ACE inhibitors can cause a dry cough due to ↑ bradykinin.
ADH & ANP - The Fluid Balance Crew
-
Antidiuretic Hormone (ADH): Secreted from posterior pituitary.
- Trigger: ↑ Plasma osmolality, ↓ blood volume.
- Action: Inserts aquaporin-2 in collecting ducts → ↑ H₂O reabsorption.
- Result: ↑ Blood volume, ↑ blood pressure; concentrated urine.
-
Atrial Natriuretic Peptide (ANP): Released from atria.
- Trigger: Atrial stretch due to ↑ blood volume.
- Action: Vasodilation & inhibits renin-angiotensin-aldosterone system.
- Result: ↑ Na⁺ and water excretion → ↓ blood volume & pressure.
⭐ B-type Natriuretic Peptide (BNP) is released from ventricles due to stretch and is a key diagnostic marker for heart failure.
Local Vaso-Regulators - The Micro-Managers
- Metabolic (Active Hyperemia): Blood flow matched to local metabolic demand.
- Vasodilators: ↓$O_2$, ↑$CO_2$, ↑H⁺, ↑K⁺, Adenosine, Nitric Oxide (NO).
- Vasoconstrictors: Endothelin-1 (potent).
- Myogenic (Autoregulation): Intrinsic smooth muscle response to pressure changes.
- ↑Pressure → Stretch → Vasoconstriction.
- ↓Pressure → ↓Stretch → Vasodilation.
⭐ Local metabolic control is the primary mechanism in vital organs like the heart and brain, overriding systemic sympathetic input to ensure constant perfusion.
Integrated Control - The BP Grand Finale
- Overall Goal: Maintain tissue perfusion without damaging vessels.
- Key Equation: Mean Arterial Pressure (MAP) is the product of Cardiac Output (CO) and Total Peripheral Resistance (TPR), expressed as $MAP = CO \times TPR$.
⭐ The Cushing reflex-hypertension, bradycardia, and irregular respirations-is a critical sign of increased intracranial pressure, representing a last-ditch effort to maintain cerebral perfusion.
High‑Yield Points - ⚡ Biggest Takeaways
- Baroreceptors (carotid/aortic) are the fastest mechanism, responding to stretch to modulate autonomic tone.
- RAAS is the key long-term regulator; Angiotensin II is a potent vasoconstrictor, and aldosterone increases volume.
- ANP/BNP are released from stretched cardiac chambers, causing vasodilation and natriuresis to lower BP.
- ADH (vasopressin) increases free water reabsorption and causes vasoconstriction at high concentrations.
- The Cushing reflex-hypertension and bradycardia-is a response to increased intracranial pressure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

