Preload - The Big Stretch
- Definition: The stretch on ventricular muscle fibers at the end of diastole (EDV). Essentially, the volume the ventricle has to pump out.
- Frank-Starling Mechanism: ↑ Preload → ↑ stretch → ↑ force of contraction → ↑ stroke volume (up to a point).
- Think of a rubber band: more stretch, more snap-back.
- Factors Increasing Preload:
- ↑ Venous return (e.g., IV fluids, exercise)
- Slower heart rate (more filling time)
- Factors Decreasing Preload:
- ↓ Venous return (e.g., diuretics, venodilators like Nitroglycerin)
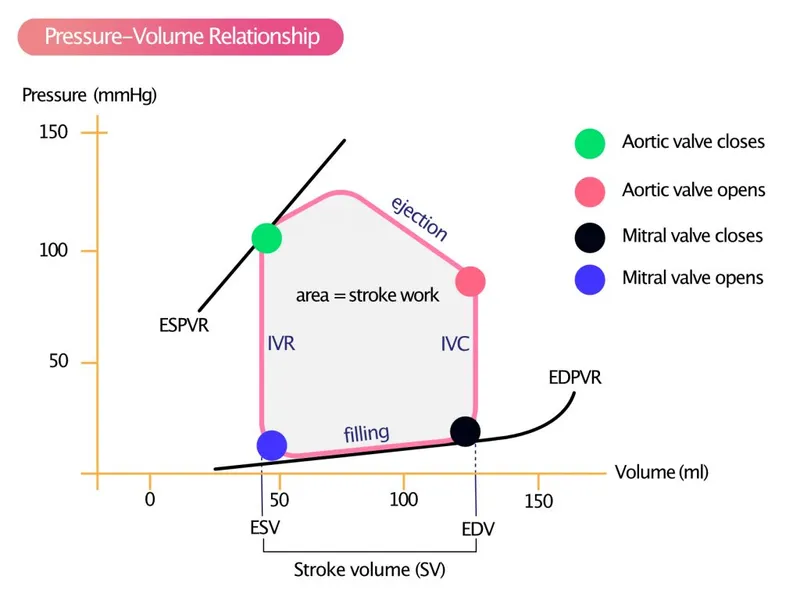
⭐ In heart failure, excessive preload leads to pulmonary/systemic congestion. Reducing preload with diuretics is a cornerstone of symptomatic therapy.
Afterload - The Squeeze Against
- Definition: The force or resistance the left ventricle must overcome to circulate blood. Essentially, it's the pressure the chamber has to generate to open the aortic valve.
- Primary Determinants:
- Systemic Vascular Resistance (SVR)
- Aortic pressure
- Wall tension (Laplace's Law: $Stress = (P \times r) / (2h)$)
- Factors Increasing Afterload:
- Systemic Hypertension
- Aortic Stenosis
- Vasoconstriction (e.g., sympathomimetics)
- Factors Decreasing Afterload:
- Vasodilators (e.g., ACE inhibitors, hydralazine)
- Septic shock
⭐ Chronically elevated afterload (like in untreated hypertension or aortic stenosis) leads to concentric left ventricular hypertrophy as the myocardium thickens to generate more force.

Clinical Correlations - When Loads Go Wrong

-
Preload Imbalances (Volume):
- ↑ Preload: Seen in heart failure, fluid overload, and valve regurgitation. Causes ventricular dilation and can lead to systolic dysfunction.
- ↓ Preload: Results from hemorrhage, dehydration, or sepsis. Leads to reduced stroke volume (SV) and cardiac output (CO) per Frank-Starling.
-
Afterload Imbalances (Pressure):
- ↑ Afterload: Caused by hypertension or aortic stenosis. The ventricle hypertrophies (LVH) to generate more pressure, leading to diastolic dysfunction.
- ↓ Afterload: Occurs in septic shock or with vasodilator use.
-
Pharmacological Intervention:
- Preload Reducers: Nitrates (venodilators), Diuretics.
- Afterload Reducers: ACE inhibitors, ARBs, Hydralazine.
⭐ An S3 heart sound is a classic sign of increased preload (volume overload), often heard in decompensated heart failure. An S4 sound suggests a stiff ventricle from chronic ↑ afterload (pressure overload), like in long-standing hypertension.
High‑Yield Points - ⚡ Biggest Takeaways
- Preload is the end-diastolic ventricular stretch, primarily determined by venous return.
- Afterload is the resistance the ventricle must overcome to eject blood, approximated by arterial pressure.
- The Frank-Starling mechanism dictates that ↑ preload leads to an ↑ stroke volume, up to a point.
- Contractility is the intrinsic strength of cardiac muscle, independent of loading conditions.
- Reducing preload (diuretics) and afterload (vasodilators) is a key strategy in heart failure management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

